Managing Disorders of the Canine Front Limb
Introduction[edit | edit source]
Forelimb lameness in dogs is very common, but it can be difficult to determine its exact cause.[1] This page discusses some of the more common types of forelimb lameness in the canine patient.
Shoulder[edit | edit source]
The shoulder joint is the most mobile of all canine limb joints. Motion at the shoulder includes abduction, adduction, internal rotation, external rotation, but the primary movement is in the sagittal plane. The stability of the canine shoulder is maintained by the joint capsule, the medial and lateral glenohumeral ligaments, as well as large tendons located inside or just outside the joint.[2]
Osteochondrosis[edit | edit source]
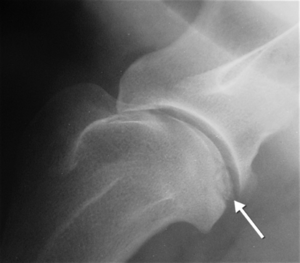
The most common cause of shoulder lameness is osteochondrosis (OCD).[3] OCD occurs when cartilage grows at a faster rate than the underlying bone, which causes areas of cartilage thickening. The thickened cartilage becomes prone to shearing forces and may detach from the subchondral bone. Once there is detachment, the synovial fluid comes into direct contact with the subchondral bone, which causes inflammation. At this stage in the disease process, the syndrome becomes known as osteochondrosis dissecans and has an inflammatory component.[4]
Early diagnosis is important as it can influence recovery rate and may prevent degenerative changes from occurring.[5]
OCD is present bilaterally in around one-third of dogs. Although it can occur in other joints, the shoulder is most often affected by OCD. It can also occur in multiple joints in the same animal. A dog with OCD usually presents with intermittent lameness at around six months of age. There is usually some atrophy of the shoulder musculature and pain will be elicited on passive shoulder extension. There will also be some pain on digital pressure over the humeral head.
Ideally, OCD lesions will be surgically removed. Once the cartilage flap is removed, the defect fills with connective tissue. If the lesion is not removed, it will remain a source of joint irritation causing long-term deficits and degeneration of the joint cartilage - i.e. osteoarthritis.
If the cartilage flap completely detaches, it forms a "joint mouse" - i.e. a small piece of floating cartilage in the joint - this becomes a source of continuous irritation and can also impinge on the bicipital tendon, which runs through the shoulder joint.
Key features[4][edit | edit source]
- Dogs are aged between 6 and 9 months of age (although it can present up until 12 months of age)
- Affects medium to large-breed dogs more than small-breed dogs[6]
- Around one-third of dogs are affected bilaterally
- The shoulder joint is most often affected, but it can occur in other joints and multiple joints can be affected
- There will usually be a history of intermittent lameness
- There will usually be some shoulder muscle atrophy
- Pain is provoked with passive shoulder extension and flexion,[7] as well as with digital pressure over the humeral head
- It can be imaged with x-ray, ultrasound, CT and MRI[8]
- If the cartilage flap becomes completely detached, it becomes what is referred to as a "joint mouse", which becomes a source of continuous irritation[4]
Management[edit | edit source]
Surgical management is usually required. Once the cartilage flap is removed, the area will fill with connective tissue (fibrocartilige). If this flap is not removed, there will be ongoing joint irritation, which will cause long-term deficits and degeneration of the joint cartilage (i.e. there is a high risk of osteoarthritis).[4] Young dogs aged between 6 and 10 months have the best outcomes following surgical interventions.[5]At this stage, little joint damage will have occurred.
Rehabilitation[edit | edit source]
There are few evidence-based recommendations for rehabilitation following the surgical removal of an OCD lesion. Some studies recommend between 4 and 12 weeks of complete non-weight-bearing, which usually means 4-12 weeks of cage rest.[4]
Physiotherapy in the initial phase aims to:[4]
- Restore full passive range of motion (ROM)
- Reduce joint swelling
- Introduce static strengthening exercises
- Gradually introduce non-weight bearing exercises through range (e.g. swimming)
In order to progress to weight-bearing exercises, the dog needs to have:[4]
- No pain or swelling in the joint
- Full passive ROM
- Radiographic evidence that the OCD lesion is healing / filling
After 4 to 6 months, the dog may be allowed to start with progressive cardiovascular exercises - i.e. longer walks, straight-line running. They must be on their leash so that they do not twist / turn and strain the joint surface. Dogs can only start more strenuous activities (i.e. sudden turning, sudden stops, acceleration etc) 6 months after surgery if they have no recurrence of pain or joint effusion.[4]
Supraspinatus Tendinopathy[edit | edit source]
Supraspinatus tendinopathy usually occurs in working / performance dogs. There is no specific age, sex, or breed predisposition to developing this condition.[10] It is believed that supraspinatus tendinopathy is caused by overuse (i.e. chronic, repetitive activities). Inflammation may be present in the early stages, but it is not typically involved in the later stages of the disease process.[10]
Key Features[10][edit | edit source]
- Canine patients with this condition usually present with varying degrees of lameness
- Weight-bearing lameness is often worse with activity
- There may be atrophy of the supraspinatus muscle
- There is usually pain on direct palpation of the supraspinatus tendon and with shoulder flexion
- There is often concurrent elbow dysplasia and or other pathological changes in the shoulder
- After function returns, dogs remain susceptible to re-injury[11]
Management[edit | edit source]
The medical management usually involves non-steroidal anti-inflammatories (NSAIDs) and controlled activity for a period of time alongside physiotherapy management.[4] Other treatments may include: acupuncture, deep cross-friction massage, heat, ultrasound, range of motion exercises / stretching, therapeutic laser extracorporeal shockwave therapy,[12] regenerative medicine therapy and ultrasound-guided injections of platelet-rich plasma.[10][11]
Canapp and colleagues found that 74.6 percent of canine patients do not respond well to NSAID therapy and 40.8 percent do not respond to rehabilitation therapy.[10] However, surgical options tend to have low efficacy and lameness often persists.[4]
Physiotherapy Management[edit | edit source]
In 2009, Cook and Purdam proposed the continuum model for tendinopathies. They divide tendinopathy into three phases:[13]
- Reactive tendinopathy
- Tendon disrepair
- Degenerative tendinopathy
In the reactive stage, there is diffuse increased cellularity and ground substance. This is followed, in the second phase, by the emergence of areas of collagen disorganisation and neurovascular ingrowth. Finally, this progresses to degenerative tendinopathy.[14] However, as Cook and colleagues note in a later study, the relationship between structure, pain and function in tendons is not yet fully understood and this contributes in part to the complexities surrounding the management of tendinopathy.[15]
Phase One[edit | edit source]
As in human patients, the first phase of rehabilitation in canine patients focuses on:[4][14]
- Reducing pain
- Avoiding activities that cause compression of the tendon (for supraspinatus this means avoiding activities that occur in full shoulder flexion)
- Avoiding the stretch-shortening cycle. Swimming and down to stand exercises are NOT appropriate choices for this reason[4]
- Introducing isometric exercises in a mid-range position to avoid excessive strain on the tendon[16][17][18] - this might include static stabilisation exercises in standing. In highly irritable tendons, bilateral exercises with shorter holding times and fewer repetitions may be indicated
- Other modalities that may be useful include cryotherapy, TENS and LASER.[19][20]
Once the dog’s pain is controlled, it has good static stability of its limb, and it can achieve an isometric static contraction without an increase in symptoms, it is possible to move into phase two of tendon rehabilitation.[4]
Phase Two[edit | edit source]
Phase two focuses on strengthening. The aim is to gradually increase the tendon’s ability to produce force and manage load.[4]
- Repetitive loading such as running / walking are unlikely to stimulate significant adaptive changes
- The focus is rather on heavier loads that can promote change in muscle and tendon and improve their load capacity
- It remains important to continue to achieve strength changes in the mid-range position and to avoid tendon compression and rapid cycling of the tendon
Exercise prescription must be tailored to the patient in terms of:[4]
- Pain level
- Specific weakness
- Patient goals
- Requirements of sport / work
Tendinopathy loading programmes generally fall into three categories:[21]
- Eccentric loading
- Heavy slow resistance training
- Combined approach
Eccentric exercises have been the mainstay of tendinopathy treatment for many years.[18] More recently, however, research has highlighted the benefit of also focusing on the concentric phase of exercises with heavy slow resistance training.[21]
NB:
- Tendon rehabilitation tends to take time
- For the first 24 to 36 hours after loading, there is a net loss of collagen production[22] - this means there must be adequate time for recovery to allow any strain to the tendon to recover. A fatigued tendon will be at greater risk of regressing.
Phase Three[edit | edit source]
It is possible to progress to phase three (i.e. functional rehabilitation) when the patient has good neuromuscular control, relatively even muscle development, no recurrence of pain and swelling or any regression in function. For sporting / working dogs, it is particularly important to include functional rehabilitation.[4] Functional rehabilitation falls into three categories:[14]
- Exercises that are specific to the functional requirements of the affected muscle and tendon
- Improving load capacity of the entire kinetic chain
- Addressing movement dysfunctions that could cause recurrence of the tendinopathy
It is also important to achieve neuroplastic training of the tendon.[23] There are significant neuromotor changes in tendinopathy that affect the descending control of the neuromuscular junction where there is pain and swelling in a tendon. It is, therefore, important to restore optimal communication between the central nervous system and the tendon to ensure it can function under high loads. This can be achieved by the use of an external marker (e.g. treats for dogs).[4]
Biceps Brachii Tendinopathy[edit | edit source]
Canine patients often also present with biceps brachii tendinopathy, particularly of the long head of the biceps. Damage to the tendon either occur from repetitive strain[24] (so it is relatively common in agility dogs who perform repetitive tight turns and repetitive landing on their front legs) or as a result of a single, significant loading event that exceeds the tendon's capacity.[4]
Key Features[edit | edit source]
Biceps brachii tendinopathy is often associated with a supraspinatus tendon lesion. It does not usually occur in isolation.[4] It tends to occur in medium- to large-breed middle-aged or older dogs.[25][26]
Animals present with variable degrees of lameness. Dogs may start to:[4]
- Knock jumps during agility
- Avoid turning tightly
- Avoid performing two-on two-off contact behaviour
Other features include:[4]
- Shortened stride
- Weight bearing lameness that can range from subtle to severe[2]
- Symptoms worsen with activity
- Direct palpation over the biceps origin may elicit a pain response[25]
- Pain and spasm may be noted with a biceps stretch (flexing the shoulder with the elbow in extension)[25]
Management[edit | edit source]
Conservative management is recommended in acute cases. This usually consists of:[4]
- Controlled activity
- Anti-inflammatory medications
- Cryotherapy
- Intra-articular injections of hyaluronic acid, cortisone
- Regenerative therapy approaches such as PRP or STEM cell therapy
Surgical management is recommended when there is an avulsion of the biceps tendon from the scapula, significant tears, or when the injury does not respond to conservative management.[26]
There are two surgical options:
- Tenotomy - where the biceps tendon is transected (cut through)
- Tenodesis
Tenotomy usually has the most favourable long-term clinical results and a high level of owner satisfaction.[26] Even though this results in the loss of function of the long head of the bicep, canine patients usually adapt fairly successfully.[4]
Physiotherapy Management[edit | edit source]
Conservative management is similar to that discussed above for supraspinatus tendinopathy. The position of compression of the bicep tendon is also in shoulder flexion, so this position needs to be avoided in the early phases of rehabilitation.[4]
There is little literature to support specific rehabilitation programmes following tenotomy. It is, therefore, important to remember that if the dog has had a resection of its biceps tendon, there is not a tendon to heal per se. However, the joint capsule is typically quite inflamed, and there will likely be some deconditioning of the shoulder joint. These features will inform treatment options going forwards.[4]
Because the long head of biceps plays a significant role in shoulder stability, both in flexion and neutral, the biceps tendon contributes to cranial and medial stability of the shoulder. Rehabilitation must, therefore, focus on helping the dog to find other effective stabilising strategies. Thus, rehabilitation must include:[4]
- Motor control
- Joint stability
- Strengthening of the synergistic muscles around the shoulder
Throughout rehabilitation, you want to ensure that you achieve and maintain pain-free passive and active range of motion. Like in supraspinatus tendinopathy, heavy, slow resistance-type training will be most effective in terms of enabling the shoulder to cope with heavy high demands during sport and activities.
Medial Shoulder Syndrome[edit | edit source]
Medial shoulder syndrome is a common cause of front limb gait-related issues in dogs.[27] Its aetiology is unknown, but it is usually related to repetitive activity and overuse rather than trauma.[2] Performance / working dogs who do a lot of turning or jumping are prone to this condition (particularly agility dogs). Repetitive strain predisposes the dog to degeneration of the tissues, which reduces tensile strength in the medial shoulder compartment and can cause fraying, disruption, and eventually a complete breakdown of the tissues.[2]
If this syndrome continues to progress, instability and subluxation of the shoulder can occur. Medial shoulder instability is essentially the end stage of a chronic progression of medial shoulder disease. It is, therefore, important to identify this condition and start treatment early on to achieve the best long-term results.[4]
Key Features[edit | edit source]
Signs of medial shoulder syndrome range from performance-related issues (i.e. the dog may not want to do tight turns anymore[2]) to relatively significant weight-bearing lameness:[4]
- Front leg lameness is intermittent,[2] and tends to worsens with exercise / heavy activity
- Does not respond well to rest and anti-inflammatory medications
- Usually unilateral
- Variable presentation from slightly shortened stride to significant weight-bearing lameness
- Some atrophy is usually associated with chronic cases
- Restricted shoulder extension common on passive range of motion testing[2]
- Muscle spasm in the muscles around the shoulder and discomfort on passive glenohumeral abduction of the shoulder is common
Medial shoulder pathology can be seen on ultrasound[27] and it is usually classified as either:
- Mild medial shoulder syndrome - mild pathological changes which could include inflammation, fraying or disruption of the structures of the medial aspect of the shoulder joint, and there might be some laxity of the medial glenohumeral ligament. As the subscapularis tendon attaches to the medial joint capsule, it might also be involved in this pathological picture.[4]
- Moderate medial shoulder instability - this includes more significant subscapularis tendinopathy - there may be a core lesion where the tendon inserts, or there might be some significant fraying or disruption of the tendon. There may be medial glenohumeral ligament lesions, thickening of the craniomedial joint capsule and labral lesions. In some cases, concurrent supraspinatus tendinopathy may cause impingement of the biceps tendon.[4]
Management[edit | edit source]
Conservative management is appropriate if diagnosed early in the disease process. If medial shoulder syndrome is not addressed early on, it causes a cascade of pathological changes, involving a variety of soft tissue structures, and becomes more challenging to manage.
In mild cases, treatment is usually focused on physiotherapy management. A key component of early rehabilitation is the use of shoulder hobbles (i.e. an external brace used to limit abduction during movement and allow for early protected functional rehabilitation). If the dog has moderate or severe medial shoulder syndrome, it will usually require arthroscopic intervention.[4]
Moderate or severe cases usually require intervention by arthroscopy where radiofrequency is used to clean out the medial compartment and remove all the frayed remnants of the structures in the medial compartment of the shoulder. For the first two weeks post-arthroscopy, the mechanical properties of the tissues are reduced. Strength gradually returns after two weeks and it is usually possible to progress dogs to normal activity between six and 12 weeks, depending on the extent of the damage. It is recommended that the patient is placed in hobbles for the first three months after arthroscopy.[4]
Biological therapies such as PRP or STEM cell might also be used in conjunction with arthroscopy depending on how severe the case is. In rare cases, damage to the medial shoulder structures can occur as a result of an acute trauma. In these instances, complete reconstruction of the medial compartment is necessary and the patient will be more significantly immobilised after surgery. The rehabilitation programme is, thus, more complicated and requires close communication with the surgeon.
Guidelines[edit | edit source]
There is little high-level evidence to support / develop post-operative rehabilitation protocols.[30] Recent animal studies suggest that immobilisation after rotator cuff repair of at least two weeks significantly reduces postoperative stiffness.[31][32]
Phase One[edit | edit source]
Goals:[4]
- Protect healing tissue
- Reduce pain
- Minimise the formation of post-operative adhesions
Collagen deposition and growth factor release peaks at around ten days after surgery, with ongoing deposition for one to two months. This plateaus at around 28 to 56 days. The newly formed collagen network needs gentle stress applied to it in order to positively affect fibre orientation. The repair should not, however, be exposed to the excessive forces imposed by active motion.[4]
Passive range of motion (PROM) of the glenohumeral joint should begin as soon as possible to minimise potential joint stiffness. PROM may be safer than more active techniques in the first two weeks. Passive motion continues until symmetrical and pain free motion is achieved when compared to the contralateral shoulder.[4]
During this time, it is important to guide the alignment of tendon deposition to ensure that the scar is functional and that the risk of adhesions is minimised. By about ten days, the animal therapist will start working towards restoring full PROM.
At this stage, exercises that help to maintain mobility of the cervical and thoracic spine, as well as isometric exercises in standing can be introduced. Active movements of the carpus and elbow can be encouraged if dogs have sufficient training to perform these actions.[4]
Phase Two[edit | edit source]
Usually after around two weeks, the patient can progress to phase two. Dogs need to demonstrate that they have:[4]
- Equal muscle strength in static positions between the affected and unaffected sides
- Good weight-bearing
- Equal resistance to external perturbation between the affected and unaffected sides
During phase two, active ROM exercises of the shoulder should be encouraged e.g. “give paw”. If a dog is able to place a paw on the handler's hand, this an open-chain proprioceptive activity. The angle of the handler's hand can be varied slightly to add a slight rotation component to the activity. Check for discomfort and any increase in symptoms after the exercises are performed.[4]
At this stage, slow active ROM exercises underwater (warm water at mid-scapular level, but NOT swimming) can be started to improve glenohumeral ROM as an adjunct to land-based exercises. The hydrostatic pressure and water temperature reduce pain and reactive muscle spasm /guarding, encourages more efficient neuromotor responses in a safe, supported environment and promotes resolution to oedema.[4][33][34]
The aim is to engage in functional exercises like slow walking, rhythmic stabilisations and active ROM exercises such as "give-paw", back-ups and side-stepping in the water.
Specific aquatic exercises include:[4]
- Figure of eights to introduce rotation
- Active flexion through carpus, elbow, shoulder when a Cavaletti rail is placed in the water
- Step on and off a raised step to achieve concentric and eccentric muscle work, and progressively load the tendon tissue
- Side-stepping - this isolates abduction and adduction, ensuring that all the dynamic components of the kinetic chain can be strengthened and also enhances proprioception
In phase two, the dog can start to progress to:[4]
- Single-leg stability exercises
- Controlled rotation components in exercises
Phase Three[edit | edit source]
It is possible to progress to phase three when the dog’s active ROM is the same on both sides. This usually occurs two or three months post-surgery. It is also possible to increase the load on the medial shoulder structures with more strenuous isotonic-type stability exercises.[4]
- Controlled, progressive swimming exercises or potentially underwater treadmill therapy can be introduced
- Stability exercises can be progressed to single-leg exercises on unstable surfaces
- Dynamic rotation components can be introduced
- Challenge muscles and joints through a full range
Phase Four[edit | edit source]
Advanced strengthening can typically be started by around three months (12-16 weeks). In order to progress to phase four, the patient needs to be:[4]
- Pain-free with activities of daily living and during / after training
- Able to tolerate all phase three exercises
Exercises are progressed by increasing the load, repetitions, challenge of the surface and the degree of movement during the exercise. It is now possible to work through the range with external resistance. It is also possible to introduce plyometrics, but to avoid fatigue, as this increases the risk of regression. There must, therefore, be adequate recovery between training sessions. One day of strenuous training should be followed by two days or rest, relative rest and recovery.[4]
Elbow[edit | edit source]
Elbow Dysplasia[edit | edit source]
. Elbow dysplasia encompasses three distinct syndromes that result from abnormal growth and development:
- ununited anconeal process (UAP),
- fragmented medial coronoid process (FCP), and
- osteochondrosis.
Elbow dysplasia is a common condition that affects large- and giant-breed dogs. The pathogenesis of elbow dysplasia is not completely understood, but it is thought to be due to asynchronous growth of the radius and ulna with genetic and environmental origins, including nutrition.[4][35] Dogs with elbow dysplasia may develop secondary osteoarthritis.[36]
The term dysplasia simply means an abnormality in development[37]. Elbow dysplasia encompasses three distinct syndromes that result from abnormal growth and development that should be considered in the differential diagnosis:[4]
- Ununited anconeal process (UAP)
- Fragmented medial coronoid process (FCP)
- Osteochondrosis
Dogs may present from around four months, and surgical management is recommended to reduce the risk of arthritis.[4]
Post-Operative Physiotherapy Management[edit | edit source]
There are no evidence-based guidelines. The length of cage rest is determined by the surgeon. Physiotherapy focuses on:[4]
- Pain management
- Restoring function as per assessed deficits:
- ROM (active and passive)
- Motor control / stability
- Strength
- Proprioceptive retraining
Physiotherapy Management for Elbow Osteoarthritis[edit | edit source]
The pharmacological management is determined by the veterinarian. Physiotherapy interventions are determined based on specific deficits:[4]
- Pain
- Stiffness
- Weakness
- Loss of motor control
- Proprioceptive deficits
Treatments include:[4]
- Education and self-management
- Exercise and weight loss
- Low impact land- or water-based exercise
- Active ROM
- Weight management
- Thermal modalities
- There is inconclusive evidence for bracing, but it can be used if it improves pain-free function. However, many dogs will not tolerate a brace and chew it off
- Taping may help determine whether a dog will benefit from, and tolerate a brace
Carpus and Digits[edit | edit source]
Carpal Hyperextension[edit | edit source]
Carpal hyperextension injuries can result in damage to the flexor retinaculum and the palmar fibrocartilage. They are often traumatic (i.e. occur after falls, stepping in a hole, or from a twisting motion at the limb), but can also be caused by chronic overloading of the carpi due to pelvic limb impairment such as chronic cranial cruciate ligament injuries.[4]
Key Features[4][edit | edit source]
- Grade 1 sprains are mild and are described as an overstretching of the ligament without disruption or loss of function of the ligament
- Grade 2 sprains are moderate in severity and are described as a partial tear of the ligament. The general continuity of the ligament is intact although the strength of the ligament is significantly reduced
- Grade 3 sprains are severe and result from complete disruption or tearing of the ligament, resulting in instability of the joint
- The degree of damage (grade 1, 2, or 3) will dictate the appropriate treatment; however, conservative management of grade 3 carpal hyperextension injuries is rarely successful and surgical fixation is recommended (pancarpal or partial carpal arthrodesis)
- Ligament healing times can be quite lengthy[43]
Physiotherapy Management[edit | edit source]
Grade 1 and 2[edit | edit source]
Physiotherapy treatment aims include:[4]
- Preventing abnormal scar tissue formation, joint stiffness, muscle weakness
- Restoring as normal as possible movement patterns
- Pain relief through joint mobility techniques, soft tissue massage, electrotherapy
- Improving scar tissue quality
- Loosening or strengthening the injured region
- Improving performance when the client returns to sport, work or daily life
- Correcting any biomechanical faults that may be affecting movement, technique or predisposing the client to injury
The amount of rehabilitation and the time needed for full recovery after a sprain or strain depend on the severity of the injury and individual rates of healing (from weeks for a mild sprain to months for a severe sprain). Extra care should be taken to avoid re-injury.[4]
Treatment options:
- POLICE (protection, optimal loading, ice compression, and elevation) - this promotes and guides safe and effective loading in acute soft tissue injury management
- Early (protected) mobilisation
- Functional treatment is superior to immobilisation[44]
- Bracing is important to allow for early safe loading
- Aquatic exercises in the initial phase of rehabilitation may be superior to land-based rehabilitation
If patients require repair or arthrodesis surgery (i.e. for Grade 3 injuries) they will need a post-operative external splint (for 6 – 8 weeks after repair surgery and for 8 weeks after arthrodesis surgery). After this, rehabilitation is as for Grades 1 and 2 sprains.[4]
Toe Injuries[edit | edit source]
Toe injuries are often under-diagnosed as a cause of lameness in dogs. They are most commonly due to tendon sprains or collateral ligament strains. They are usually caused by sudden excessive force on the interphalangeal joints due to uneven / deep / slippery surfaces, getting stuck on a surface, and stubbing toes against an object. These same forces can also result in a fracture.[4]
Patients with digit injuries usually present with severe weight-bearing to non-weight-bearing lameness. With acute injuries, there may be significant swelling, as well as pain and crepitus on manipulation. With chronic injuries, there may be swelling at the site of injury and pain on manipulation.[4]
Differential diagnosis: Exclude fractures of MC or Phalanges or sesamoids – Increased duration of restricted movement (cage rest). Dental x-ray plates often allow for better visualisation of toe/sesamoid fractures.
Managing toe injuries[edit | edit source]
Once fractures of the metacarpal, phalanges or sesamoid bones are excluded, these injuries are mostly managed conservatively (see above recommendations for carpal injuries):[4]
- It is difficult to brace/support toe injuries effectively, but can be done with taping/bandaging to prevent lateral movement of the toes.
- Otherwise use the same principles as with arthritis
- Walking on soft surfaces has been described as a useful exercise for reconditioning toes, but there is no evidence to support this
References[edit | edit source]
- ↑ Canapp SO, Dycus D, Kirkby Shaw K. Disorders of the Canine Thoracic Limb. In: Zink C, Van Dyke JB, editors. Canine Sports Medicine and Rehabilitation, Second Edition. Hoboken: John Wiley & Sons, Inc, 2018. p294-332.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 Marcellin-Little DJ, Levine D, Canapp SO. The Canine Shoulder: Selected Disorders and Their Management with Physical Therapy. Clinical Techniques in Small Animal Practice. 2007;22(4):171-82.
- ↑ Maddox TW, May C, Keeley BJ, McConnell JF. Comparison between shoulder computed tomography and clinical findings in 89 dogs presented for thoracic limb lameness. Vet Radiol Ultrasound. 2013;54(4):358-64.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 4.13 4.14 4.15 4.16 4.17 4.18 4.19 4.20 4.21 4.22 4.23 4.24 4.25 4.26 4.27 4.28 4.29 4.30 4.31 4.32 4.33 4.34 4.35 4.36 4.37 4.38 4.39 4.40 4.41 4.42 4.43 4.44 4.45 4.46 4.47 4.48 4.49 4.50 4.51 4.52 4.53 4.54 4.55 4.56 4.57 Van der Walt A. Managing Disorders of the Canine Front Limb Course. Plus , 2021.
- ↑ 5.0 5.1 Biezyński J, Skrzypczak P, Piatek A, Kościółek N, Drozdzyńska M. Assessment of treatment of Osteochondrosis dissecans (OCD) of shoulder joint in dogs--the results of two years of experience. Pol J Vet Sci. 2012;15(2):285-90.
- ↑ Ytrehus B, Carlson CS, Ekman S. Etiology and pathogenesis of osteochondrosis. Vet Pathol. 2007;44(4):429-48.
- ↑ Morris A, Anderson A. Osteochondrosis dissecans of the canine shoulder. Companion Animal. 2013;18(6):264-9.
- ↑ Wall CR, Cook CR, Cook JL. Diagnostic sensitivity of radiography, ultrasonography, and magnetic resonance imaging for detecting shoulder osteochondrosis/osteochondritis dissecans in dogs. Vet Radiol Ultrasound. 2015;56(1):3-11.
- ↑ Greg Martinez DVM. Lameness in Young Dogs :OCD. Available from: https://www.youtube.com/watch?v=w6KovKEiiFY [last accessed 17/2/21]
- ↑ 10.0 10.1 10.2 10.3 10.4 Canapp S, Canapp D, Carr B, Cox C, Barrett J. Supraspinatus Tendinopathy in 327 Dogs: A Retrospective Study. Veterinary Evidence. 2016;1(3).
- ↑ 11.0 11.1 Ho LK, Baltzer WI, Nemanic S, Stieger-Vanegas SM. Single ultrasound-guided platelet-rich plasma injection for the treatment of supraspinatus tendinopathy in dogs. Can Vet J. 2015;56(8):845-9.
- ↑ Leeman JJ, Shaw KK, Mison MB, Perry JA, Carr A, Shultz R. Extracorporeal shockwave therapy and therapeutic exercise for supraspinatus and biceps tendinopathies in 29 dogs. Vet Rec. 2016;179(15):385.
- ↑ Cook JL, Purdam CR. Is tendon pathology a continuum? A pathology model to explain the clinical presentation of load-induced tendinopathy. British Journal of Sports Medicine. 2009;43:409–16.
- ↑ 14.0 14.1 14.2 Goom TS, Malliaras P, Reiman MP, Purdam CR. Proximal Hamstring Tendinopathy: Clinical Aspects of Assessment and Management. J Orthop Sports Phys Ther. 2016;46(6):483-93.
- ↑ Cook JL, Rio E, Purdam CR, et al. Revisiting the continuum model of tendon pathology: what is its merit in clinical practice and research? British Journal of Sports Medicine. 2016;50:1187-91.
- ↑ Rio E, Kidgell D, Purdam C, Gaida J, Moseley GL, Pearce AJ et al. Isometric exercise induces analgesia and reduces inhibition in patellar tendinopathy. Br J Sports Med. 2015;49(19):1277-83.
- ↑ van Ark M, Cook JL, Docking SI, Zwerver J, Gaida JE, van den Akker-Scheek I et al. Do isometric and isotonic exercise programs reduce pain in athletes with patellar tendinopathy in-season? A randomised clinical trial. J Sci Med Sport. 2016;19(9):702-6.
- ↑ 18.0 18.1 Malliaras P, Cook J, Purdam C, Rio E. Patellar Tendinopathy: Clinical Diagnosis, Load Management, and Advice for Challenging Case Presentations. J Orthop Sports Phys Ther. 2015;45(11):887-98.
- ↑ Haslerud S, Magnussen LH, Joensen J, Lopes-Martins RA, Bjordal JM. The efficacy of low-level laser therapy for shoulder tendinopathy: a systematic review and meta-analysis of randomized controlled trials. Physiother Res Int. 2015;20(2):108-25.
- ↑ Tumilty S, Munn J, McDonough S, Hurley DA, Basford JR, Baxter GD. Low -evel laser treatment of tendinopathy: a systematic review with meta-analysis. Photomed Laser Surg. 2010;28(1):3-16.
- ↑ 21.0 21.1 Malliaras P, Barton CJ, Reeves ND, Langberg H. Achilles and patellar tendinopathy loading programmes: a systematic review comparing clinical outcomes and identifying potential mechanisms for effectiveness. Sports Med. 2013;43(4):267-86.
- ↑ Magnusson SP, Langberg H, Kjaer M. The pathogenesis of tendinopathy: balancing the response to loading. Nat Rev Rheumatol. 2010;6(5):262-8.
- ↑ Rio E, Kidgell D, Moseley GL, Gaida J, Docking S, Purdam C et al. Tendon neuroplastic training: changing the way we think about tendon rehabilitation: a narrative review. Br J Sports Med. 2016 Feb;50(4):209-15.
- ↑ Sharma P, Maffulli N. Tendon injury and tendinopathy: healing and repair. J Bone Joint Surg Am. 2005;87(1):187-202.
- ↑ 25.0 25.1 25.2 Bruce WJ, Burbidge HM, Bray JP, Broome CJ. Bicipital tendinitis and tenosynovitis in the dog: a study of 15 cases, New Zealand Veterinary Journal. 2000;48(2):44-52.
- ↑ 26.0 26.1 26.2 Bergenhuyzen AL, Vermote KA, van Bree H, Van Ryssen B. Long-term follow-up after arthroscopic tenotomy for partial rupture of the biceps brachii tendon. Vet Comp Orthop Traumatol. 2010;23(1):51-5.
- ↑ 27.0 27.1 Squire N, Canapp S, Canapp D, Dycus D, Leasure CS. Assessment of Magnetic Resonance Imaging, Musculoskeletal Ultrasound, and Arthroscopy in the Diagnosis of Medial Shoulder Syndrome in Canines. Vet Comp Orthop Traumatol. 2019;32(S 04):A13-A24.
- ↑ Susan Garrett. Canine Medial Shoulder Syndrome: With Drs. Canapp and Susan Garrett. Available from: https://www.youtube.com/watch?v=idi_-8GOqOc [last accessed 17/2/21]
- ↑ TNTBorderCollies. Chill Putting on Hobbles. Available from: https://www.youtube.com/watch?v=cQCbxER9Mgc [last accessed 17/2/21]
- ↑ van der Meijden OA, Westgard P, Chandler Z, Gaskill TR, Kokmeyer D et al. Rehabilitation after arthroscopic rotator cuff repair: current concepts review and evidence-based guidelines. Int J Sports Phys Ther. 2012;7(2):197-218.
- ↑ Gimbel JA, Van Kleunen JP, Williams GR, Thomopoulos S, Soslowsky LJ. Long durations of immobilization in the rat result in enhanced mechanical properties of the healing supraspinatus tendon insertion site. J Biomech Eng. 2007;129(3):400-4.
- ↑ Peltz CD, Dourte LM, Kuntz AF, Sarver JJ, Kim SY, Williams GR, Soslowsky LJ. The effect of postoperative passive motion on rotator cuff healing in a rat model. J Bone Joint Surg Am. 2009;91(10):2421-9.
- ↑ Tomlinson R. Use of canine hydrotherapy as part of a rehabilitation programme. The Veterinary Nurse. 2012;3(10):624-9.
- ↑ De Smedt L. Hydrotherapy as a conservative therapy for canine hip dysplasia [dissertation]. Ghent: Ghent University. 2019.
- ↑ Michelsen J. Canine elbow dysplasia: Aetiopathogenesis and current treatment recommendations. The Veterinary Journal. 2013; 196(1):12-9.
- ↑ Hercock CA, Pinchbeck G, Giejda A, Clegg PD, Innes JF. Validation of a client-based clinical metrology instrument for the evaluation of canine elbow osteoarthritis. J Small Anim Pract. 2009;50(6):266-71.
- ↑ Blood, D.C. & Studdert, V.P. Saunders comprehensive veterinary dictionary. 1999
- ↑ Colorado Canine Orthopedics & Rehab. Canine Elbow Dysplasia by Dr. Michael Bauer Available from: https://www.youtube.com/watch?v=1IgmyNNkkTY [last accessed 17/2/21]
- ↑ MercolaHealthyPets. Elbow Dysplasia in Dogs. Available from: https://www.youtube.com/watch?v=fjITYgIbej0 [last accessed 17/2/21]
- ↑ Brosseau L, Yonge KA, Robinson V, Marchand S, Judd M, Wells G, Tugwell P. Thermotherapy for treatment of osteoarthritis. Cochrane Database Syst Rev. 2003;2003(4):CD004522.
- ↑ Denegar CR, Dougherty DR, Friedman JE, Schimizzi ME, Clark JE, Comstock BA et al. Preferences for heat, cold, or contrast in patients with knee osteoarthritis affect treatment response. Clin Interv Aging. 2010;5:199-206.
- ↑ Exubrion Therapeutics. The Challenges of Canine Elbow Osteoarthritis (OA). Available from: https://www.youtube.com/watch?v=ByCgRdnrlvA [last accessed 17/2/21]
- ↑ Hauser RA, Dolan EE. Ligament Injury and Healing: An Overview of Current Clinical Concepts. Journal of Prolotherapy. 2011;3(4):836-46.
- ↑ Kerkhoffs GM, Rowe BH, Assendelft WJ, Kelly KD, Struijs PA, van Dijk CN. Immobilisation for acute ankle sprain. A systematic review. Arch Orthop Trauma Surg. 2001;121(8):462-71.