Management of Your Anterior Cruciate Ligament (ACL) Injury
Read Me First[edit | edit source]
This page is not intended to replace your healthcare professional. Please make sure you seek medical advice if you are experiencing any symptoms from any injury or condition.
Common symptoms of an Anterior Cruciate Ligament (ACL) injury include hearing a “pop” or feeling a popping sensation in your knee, severe pain around the knee, swelling, discomfort when you walk, loss of range of movement and a feeling of instability in the knee.
Disclaimer[edit | edit source]
The content on or accessible through Physiopedia is for informational purposes only. Physiopedia is not a substitute for professional advice or expert medical services.
What is an ACL injury?[edit | edit source]
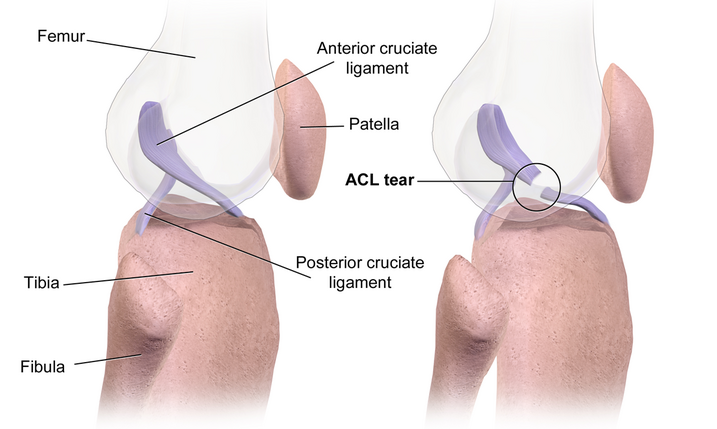
The knee joint is made up of three bones; thigh (femur), shin (tibia), and the kneecap (patella). The kneecap gives the joint some protection at the front of the joint. There are ligaments within the knee joint that connect these bones together and provide the joint with stability. The four major ligaments are the medial collateral ligament, lateral collateral ligament, the anterior cruciate ligament (ACL), and the posterior cruciate ligament. There is also the medial and lateral meniscus which provides additional stability and act as a shock absorber in the knee joint.
The Anterior Cruciate Ligament (ACL) is a strong, flexible band of tissue inside the knee joint connecting the femur (thigh) to the tibia (shin). It forms a cross shape with the posterior cruciate ligament. The ACL is an important structure within the knee joint.
The ACL provides stability to the knee. It is vital in preventing the femur sliding backwards on the tibia and stops the tibia sliding forward under the femur. It also resists rotational loads, which occur when the foot is planted and the leg pivots. When the ACL is injured, the knee becomes unstable or may even give way, especially when trying to stop or turn quickly.
Causes[edit | edit source]
After an assessment, an injury to the ACL is graded at I, II or III. A Grade I injury is when the ligament is still in tact but has stretched. A Grade II injury is a partial tear of the ligament. A Grade III injury is a complete tear or rupture of the ligament.
The cause of the injury can be broken down into two.
Non-contact: occurs when the knee is exposed to sudden decelerating forces combined with rotational forces, e.g., quickly changing direction when pivoting, running or landing from a jump. Hyperextension (too much straightening of the knee) or extreme hyperflexion (too much bending of the knee) can also damage the ACL
Contact: can occur when there is direct trauma or impact to the outside of the knee or lower leg.
- Females are more likely to suffer from an ACL injury. There are slight anatomical differences which increase the risk of injury.
- Previous injury to the ACL.
- Participating in certain sports that require frequent and quick deceleration and changes of direction.
Prevention[edit | edit source]
- Avoid exercising while overly fatigued.
- Strengthening your leg muscles. Weak quadriceps (front of thigh) and especially hamstrings (back of thigh) can increase risk of an ACL injury.
- Work to develop muscle groups evenly.
- Develop a balance between strength and flexibility.
Symptoms[edit | edit source]
When the ACL is injured:
- You may hear a “pop” or feel a popping sensation in your knee.
- You might feel extreme pain and be unable to continue a task or activity.
- There might also be quick onset of swelling .
- Loss of range of motion - you might struggle to bend your knee and straighten your leg.
- Discomfort when walking.
- A feeling of instability in the knee or buckling and “giving way” when weight-bearing.
Diagnosis[edit | edit source]
After a thorough assessment of your knee, your physiotherapist or a doctor may be able to diagnose the injury. To determine the severity of the injury, you may also be referred for an MRI (magnetic resonance imaging) or ultrasound to confirm this. You may also need an x-ray to rule out any bone fractures.
Management[edit | edit source]
There may be different options available to you following an injury to your ACL. This can all depend on the nature and severity of the injury. It is important that you have a thorough discussion with your doctor or physiotherapist to analyse the pros and cons of the options available. You may also want to include your friends and family to discuss these options.
After an injury to your ACL you may not want or need surgery, this is sometimes called the "conservative" approach, this will mean that there will not be any surgical intervention and you will follow a rehabilitation programme with your physiotherapist. This can depend on a number of circumstances such as occupation, lifestyle, or activity levels. The role of your physiotherapist, is to support and empower you through your rehabilitation. The focus will be on regaining movement and function, as well as getting you back to what you enjoy doing.
You might also be able to opt for the surgical route. Before starting the treatment and rehabilitation program, it is important that you and your physiotherapist discuss your goals and aspirations. This will allow you to adapt and suit the rehabilitation program to meet your needs and expectations. The rehabilitation process post surgery tends to last 9-12 months, but it can sometimes be slightly quicker or slower. It is completely normal to feel some nerves and apprehension about the injury and surgery. Your physiotherapist and doctor will support you through this. If you want to know anything or if you are finding anything difficult, then please don’t hesitate in contacting your physiotherapist or other suitable healthcare professional.
Exercises[edit | edit source]
During the first 0-2 weeks, it is important to bring the swelling under control but also begin early rehabilitation exercises such as normalising walking pattern and some muscle activation. You may also notice some pain and stiffness during this stage.
The following videos should give you an idea of the process for rehabilitation. These are just examples to help you gain a better understanding, your own programme may look slightly different.
Please be aware of swelling around the knee joint - and follow the POLICE (Protect, Optimal Loading, Ice, Compression, Elevation) principle when necessary.
Moving into the period of 2-6 weeks stage you will start working towards full range of movement in the knee. Again, remember to manage any swelling if necessary.
During the 6-12 weeks stage, you would gradually begin to strengthen the muscles in your leg and progress this over time. Avoid pivoting, jumping, hopping and quick changes of direction at this point. From 6 weeks, you may start cycling on a static bike, as long as you have full range of movement. Walking is also a great way to build up some strength and stamina. Remember to listen to your body throughout.
Typically, after 12 weeks you would begin to factor in some sport-specific or functional exercises that will be specific to you and your needs. It will be normal to experience some highs and lows along the way. Remember that rehabilitation is a process. The aim is to get you back to a feeling of wellbeing, full of confidence, and to full function.
Self-Management[edit | edit source]
- It is important to continue a healthy lifestyle during your rehabilitation. You can do this by spending time on yourself, seeing friends and family, or if possible, participating in hobbies that you enjoy. Remember to maintain a good sleeping pattern too.
- Driving is not advised until you can walk unaided and fully weight bear through your operated leg. This can be for around 6 weeks.
- Remember to exercise your non-injured leg too.
- Keep track of your knee’s response to exercise. How did it feel after training? How did it feel in the evening? How did it feel the morning after? How does that compare to the day before?
More Information and Support[edit | edit source]
These links will provide you with some more information and support.
Anterior Cruciate Ligament (ACL)
Anterior Cruciate Ligament (ACL) Rehabilitation
References[edit | edit source]
- ↑ Rehab My Patient. VMO Static quadriceps contraction sitting. Available from: http://www.youtube.com/watch?v=ltZhmKM9KT4 [last accessed 28/2/2022]
- ↑ Rehab My Patient. How to improve knee mobility lying. Available from: http://www.youtube.com/watch?v=skOauZ54MLU [last accessed 28/2/2022]
- ↑ Rehab My Patient. VMO Inner range quadriceps sitting. Available from: http://www.youtube.com/watch?v=ZPt0HPDgNDw [last accessed 3/3/2022]
- ↑ Rehab My Patient. Half squat. Available from: http://www.youtube.com/watch?v=b1JD-Bzw7kQ [last accessed 3/3/2022]
- ↑ Rehab My Patient. How to do a box step front. Available from: http://www.youtube.com/watch?v=EI739iJbGUU [last accessed 3/3/2022]
- ↑ Rehab My Patient. Balance exercise One leg stand. Available from: http://www.youtube.com/watch?v=ZLxyh_PEstI [last accessed 3/3/2022]
- ↑ Rehab My Patient. Sit-down chair squat. Available from: http://www.youtube.com/watch?v=Z20XNb0VdEk [last accessed 3/3/2022]
- ↑ Rehab My Patient. Wobble Cushion Dyna Disc Balance Stand. Available from: http://www.youtube.com/watch?v=YDn4ODy8EkU [last accessed 3/3/2022]
- ↑ Rehab My Patient. Calf raises one leg. Available from: http://www.youtube.com/watch?v=QEILIo9Kzlw [last accessed 3/3/2022]