Leprosy
Top Contributors - Manisha Shrestha, Kim Jackson, Nikhil Benhur Abburi and Nupur Smit Shah
Introduction[edit | edit source]
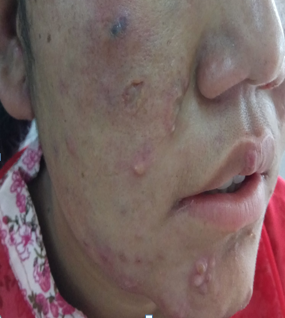
Leprosy is a chronic infectious bacterial disease affecting the nerves, skin, eyes, and muscosa of upper respiratory tract. Leprosy was renamed Hansen’s disease after Norwegian scientist Gerhard Henrik Armauer Hansen, who in 1873 discovered the slow-growing bacterium now known as Mycobacterium leprae as the cause of the illness.[1]
Leprosy is curable and treatment in the early stages can prevent disability. It can be cured with multidrug treatment regime, if early diagnosis is made.
Leprosy is a polymorphic infectious disease, the manifestation of which is determined by the immune system of the host.[2]
World Leprosy Day is observed on the last Sunday of January each year. Established in 1954 by French philanthropist Raoul Follereau, it aims to raise awareness about leprosy (now called Hansen’s disease) and teach people about this ancient disease that is easily curable today.
Epidemiology[edit | edit source]
Around the world:
- The number of new cases reported globally to World Health Organization (WHO) external icon in 2019 was more than 200,000 and 127558 new leprosy cases detected globally in 2020 which includes 8 629 children below 15 years. .[3][4]
- Among the new cases 7 198 new cases were detected with grade2 disabilities (G2D) and the new G2D rate was recorded at 0.9 per million population.[3]
- An estimated 2 to 3 million people are living with Hansen’s disease-related disabilities globally.[5]
- In 2019, the countries with the highest number of new diagnoses were India, Brazil, and Indonesia.[5]
- Over half of all new cases of Hansen’s disease are diagnosed in India, which remains home to a third of the world’s poor, a group disproportionately affected by the disease. [5]
- The COVID 19 pandemic has disrupted programme implementation and a reduction in new case detection by 37% in 2020 compared with 2019.[4]
Mycobacterium Leprae[edit | edit source]
Mycobacterium leprae is:
- an intracellular, pleomorphic, acid-fast, pathogenic bacterium
- an aerobic bacillus (rod-shaped bacterium)
- in size and shape, it closely resembles Mycobacterium tuberculosis
- The difficulty in culturing the organism appears to be because it is an obligate intracellular parasite that lacks many necessary genes for independent survival.
- grown in mouse foot pads and more recently in nine-banded armadillos
- It multiplies slowly. On average, the disease incubation period is 5 years but symptoms may occur within 1 year. It can also take as long as 20 years or even more to occur.
- They can be grown in the laboratory by injection into the footpads of mice.
Mode of Transmission[edit | edit source]
- Two exit routes of M. leprae from the human body often described are the skin and the nasal mucosa.
- The entry route of M. leprae into the human body is also not definitively known. The skin and the upper respiratory tract are most likely; however, recent research increasingly favours the respiratory route.[6]
- The bacillus is likely transmitted via droplets, from the nose and mouth, during close and frequent contact with untreated cases.[1]
Risk Factors for Leprosy[edit | edit source]
- Close contact with patients of leprosy
- People living in endemic areas
- Immunocompromised individuals
- Armadillo exposure
- Genetic influences
- Overcrowding
- Low socio economic status[6]
Clinically Relevant Anatomy[edit | edit source]
Pheripheral nerve and adjacent cells( schwann cell)
Eye
Mechanism of Injury / Pathological Process[edit | edit source]
Lepra bacilli enters into the body through respiratory route. Then those bacilli migrates towards the neural tissues and binds to schwann cells ( which is the major target of the bacilli). Afterward, it invades schwann cells by specific laminin binding protein and phenolic glycolipid-1(PGL-1). Binding of M. leprae to SCs induces demyelination and loss of axonal conductance. Bacteria are also found in macrophages, muscle cells and endothelial cells of blood vessels. Bacilli start multiplying slowly within the cells and gets liberated from destroyed cells and then enter unaffected cells. As bacilli multiply ,bacterial load increases in body and thus infection is recognized by body immune system. Specific and effective cell mediated immunity provides protection to a person against leprosy.
When cell mediated immunity (CMI) is effective in controlling infection, lesions are healed spontaneously or produce paucibacillary type of leprosy. Person with good CMI may have granuloma formation in cutaneous nerve causing swelling of nerve and hence destroyed. It causes inflammation in epineurium causes compression and destruction of unmyelinated sensory and autonomic fiber. Myelinated motor fibers are the last to get affected causing motor impairments. Good CMI limits disease to schwann cells-pure neural leprosy.
If CMI is deficient, produce multibacilary leprosy with multi system involvement. Bacilli which escapes from nerve to adjacent skin caused classical skin lesions. Bacilli liberated by schwann cells engulfed by histiocytes-wandering macrophages-travel to other tissue through blood and lymph. Phagocytosis of M. leprae by monocyte-derived macrophages can be mediated by complement receptors CR1 (CD35), CR3 (CD11b/CD18), and CR4 (CD11c/CD18) and is regulated by protein kinase.
Immunological Reactions[edit | edit source]
Lepra reaction is the immune-mediated complication associated with up to 50% of patients, can cause rapid nerve damage resulting in anaesthesia and weakness, which in turn increases risk of injury and deformity. They can occur at presentation, during treatment for leprosy with multi-drug therapy (MDT) and occasionally following completion of MDT.
Two types of reactions are recognized:
- Type 1 (T1R, also known as reversal or downgrading)
- Occurs BT, BB, or BL disease
- Caused by an increase in cell-mediated immunity, result in skin or nerve inflammation at sites of Mycobacterium leprae infection.
- Clinical manifestations:
- A red swollen patch in preexisting skin lesion or overlying a major nerve trunk.
- Erythema and induration of pre-existing skin lesion
- Inflammation associated with reactions can lead to severe nerve injury with subsequent paralysis and deformity
- Ulcerated skin lesions
- Pain or tenderness in one or more nerves
- Loss of nerve function with muscle weakness or loss of sensation.
- Observed recovery rate is 60-70% in those who are identified and treated within six months of onset.
- Type 2 reactions (erythema nodosum leprosum, ENL)
- Caused by immune complex-mediated.
- Symptoms are diverse with characteristic painful, erythematous subcutaneous nodules occurring with systemic features including fever, lymphadenitis, arthritis, neuritis, iridocyclitis or orchitis.[8]
Classification[edit | edit source]
Leprosy can be broadly classified via two classification system.
- Ridley and Jopling classification
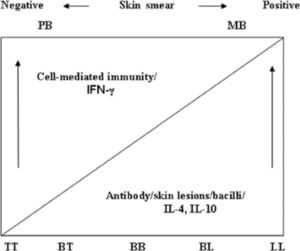
- In the 1960s, Ridley and Jopling proposed a histological classification scheme for leprosy that ranged in severity. Leprosy is classified within two poles of the disease with transition between the clinical forms . Clinical, histopathological, and immunological criteria identify five forms of leprosy:
- Tuberculoid leprosy (TT)
- Borderline tuberculoid (BT)
- Mid borderline (BB)
- Borderline lepromatous (BL)
- Lepromatous leprosy (LL)
- In the 1960s, Ridley and Jopling proposed a histological classification scheme for leprosy that ranged in severity. Leprosy is classified within two poles of the disease with transition between the clinical forms . Clinical, histopathological, and immunological criteria identify five forms of leprosy:
- WHO classification
- Initially, patients were divided into two groups for therapeutic purposes: paucibacillary (TT, BT) and multibacillary (midborderline (BB), BL, LL) . It was recommended later that the classification is to be based on the number of skin lesions, less than or equal to five for paucibacillary (PB) and greater than five for the multibacillary (MB) form. [2]
Clinical Presentation[edit | edit source]
Clinical features of Leprosy
| Characteristics | Tuberculoid | Borderline tuberculoid | Midborderline | Borderline lepromatous | Lepromatous leprosy |
|---|---|---|---|---|---|
| Number of lesions | Single or upto 3 | A Few (up to 10) | Several (10–30) | Numerous, asymmetrical (>30) | Innumerable, symmetrical |
| Size | Variable,
usually large |
Variable, some are large | Variable | Small, some
can be large |
Small |
| Surface changes | Hypopigmented | Dry, scaly, look bright, and infiltrated | Dull or slightly shiny | Shiny | Shiny |
| Sensations | Absent | Markedly diminished | Moderately diminished | Slightly diminished | Minimally diminished |
| Hair growth | Nil | Markedly diminished | Moderately diminished | Slightly diminished | Not affected initially |
| Skin smear | Negative | Negative or 1+ | 1–3+ | 3–5+ | Plenty, including globi (6+) |
| Lepromin test | Strongly positive | Weakly positive | Negative | Negative | Negative |
Since it mainly affects skin and nerves, these are some clinical features seen in patient with leprosy:
- Hypopigmented or reddish patch/es on skin
- Diminished sensation within skin patches
- Paresthesias (tingling or numbness in hands or feet)
- Painless wounds or burns on hands or feet
- Tender, enlarged peripheral nerves
If the diseases is left untreated, it become chronic and may lead to various physical deformities. Such as:
- Weakness of hands with claw fingers
- Foot drop
- Facial paralysis
- Lagopthalmos
- Lack of eyebrows and eyelashes
- Collapsed nose
- Perforated nasal septum
- Trophic ulcers
Diagnostic Procedures[edit | edit source]
- Histopathologic examination of skin biopsies
- confirm diagnosis of leprosy
- classification of leprosy.
- Bacteriological Examination
- Skin smears:
- Smears taken from the lesions ,from ear lobules and eyebrows and are stained using modified zeihl-neelsen method.
- Reading of smears:
- Bacteriological index- Indicates density of leprosy bacilli (live & dead) in the smears and ranges from 0 to 6+
- Morphological index- It is the percentage of presumably living bacilli in relation to total number of bacilli in the smear
- Skin smears:
- Lepromin test
- Immunological test indicative of host resistance to lepra bacilli. A sample of inactivated leprosy causing bacteria is injected just under the skin ,usually on the forearm.
- Tuberculoid-immune system recognizes and produces allergic reactions: positive
- Lepromatous-the immune system does not recognizes: negative
- Polymerase chain reaction
- for detection of M. lepra DNA in tissue.
Diagnostic Criteria[edit | edit source]
To diagnosed disease clinically, at least one of the three cardinal signs:
- Definite loss of sensation in hypopigmented or reddish skin patch.
- Thickened peripheral nerves with loss of sensation and/or weakness of the muscle supplied by that nerve.
- Presence of acid fast bacilli in a slit skin smear or biopsy material.[9]
Management / Interventions[edit | edit source]
Medical Management[edit | edit source]
WHO has recommended multi drug therapy for patient with leprosy. The treatment of patient varies based upon the type of leprosy i.e. either paucibacillary or multibacillary.[10]
1998 WHO guideline suggested:
Paucibacillary leprosy (6 months)
- Cap. Rifampicin (600 mg) monthly, supervised
- Tab. Dapsone (100 mg) daily
Multibacillary leprosy (1 year)
- Cap. Rifampicin (600mg) monthly, supervised
- Cap. Clofazimine (300mg) monthly, supervised
- Tab. Dapsone (100mg) daily
- Cap. Clofazimine (50mg) daily
This guideline was revised in 2018 by WHO and thus recommend uniform MDT for both type of disease classification:
- Administration of three drugs (rifampin,dapsone,clofazimine)to all patients regardless of disease classification.
- Reduces the likelihood of undertreating patients with multibacillary disease who may be misclassified as paucibacillary disease.
- However, the treatment regimen is controversial.
Other Treatment Regimen[edit | edit source]
Comprises:
- Rifampin - 600 mg
- Ofloxacin - 400 mg
- Minocycline – 100 mg
Single dose for single lesion leprosy
ROM -6 (Monthly for 6 months) - Paucibacillary
ROM -12 (Monthly for 12 months) – Multibacillary
Newer drugs: ofloxacin, minocycline,clarithromycin
Follow Up After Initiation of Medical Treatment[edit | edit source]
- The first follow up visit-2-4weeks to evaluate side effects of medications
- Then routine follow up –every three months
- After completion of treatment annual follow up for 3 more years for patient with tuberculoid disease and for five more years with lepromatous disease.[10]
Management of Leprosy Reactions[edit | edit source]
| TYPE 1 REACTION | TYPE 2 REACTION | |
| MILD | NSAIDS | NSAIDS |
| MODERATE | NSAIDS
ORAL STEROIDS |
NSAIDS
THALIDOMIDE CHLOROQUINE CLOFAZIMINE |
| SEVERE | NSAIDS
ORAL STEROIDS |
THALIDOMIDE
ORAL STEROIDS |
Prophylaxis Doses[edit | edit source]
• Within the endemic areas, WHO 2018 guidelines recommend single dose of rifampin for adults and children >/= 2yrs.
Rehabilitation[edit | edit source]
The primary goal of rehabilitation is reversing the physical impairments caused by leprosy, while the secondary goal is customizing lifestyle modifications for the individual patients, their families, and their communities. It should start at diagnosis and continue until the patient is able to return to an active normal life.[11]
The physical rehabilitation of the leprosy-affected can be classified into the following categories:
- Identifying nerve function impairment (NFI),
- Monitoring impairments, and
- Preventing further deterioration of impairments.
Identifying Nerve Impairment[edit | edit source]
The superficial nerve trunks are commonly affected in neuritis, as the lower temperature in proximal areas allows sustained growth of the leprosy bacilli. assessment of neuritis should be done before start of anti-leprosy treatment, during anti-leprosy treatment (every month when patient comes in for MDT, while on a steroid course for reversing the impairment (every fourteen days) and at the end of anti-leprosy treatment. Nerves that are routinely palpated during diagnosis and follow up of the disease are the greater auricular, ulnar, median, radial, common peroneal, and posterior tibial nerves.
Examination that are done for the assessment of nerve impairment are
- Palpation of nerve along its course to look for signs of tenderness, thickening, and abscess.
- Sensory testing: In leprosy, sensory loss can include all of the different modalities, including pain, temperature, light touch, and pressure. Testing to determine the presence of sensation is performed on ten points in the hand and ten points in the feet.
- Motor testing: It involve muscle strength testing through MMRC grading
Type of impairment following leprosy
- Primary Impairment: Primary impairments in leprosy occur as a direct result of damage to the nerves.
- Lagophthalmos and corneal anesthesia
- Clawing of fingers
- Ape thumb deformity
- Wrist drop
- Sensory loss over palm
- Foot drop
- Claw toes
- Plantar anesthesia
- Autonomic dysfunction
- Secondary Impairment: It is because of consequences following peripheral nerve damaged by leprosy and can be thus impairment.
- Stiff joints
- Joint contractures
- Ulcers
- Shortening
- Disintegration of the bones
- Exposure keratitis, corneal ulcer, and corneal opacity
Monitoring Impairment[edit | edit source]
Grading Impairment[edit | edit source]
The WHO grading system has separate components for hands, feet, and eyes. Therefore, hands, feet, and eyes are graded separately based on the impairments present. The scale has a maximum score of two and a minimum score of zero.
- WHO- Grading of deformity (1988)
| Grade | Hands and feet | Eyes |
| Grade 0 | No anesthesia
No visible deformity or damage |
No eye problems due to leprosy
No evidence of visual impairment |
| Grade 1 | Anesthesia present
No visible deformity or damage |
Eye problems due to leprosy
Present but vision not severely affected (Vision is 6/60 or better; can count finger at 6 meters) |
| Grade 2 | Visible deformity or damage present | Severe visual impairment
(Vision is worse than 6/60; cannot count fingers at 6 meters) |
The Eye, Hand, and Feet (EHF) scoring system was developed to more readily document the progression of impairments in individual patients. The EHF score calculates the sum of the individual WHO scores for each eye, hand, and foot. For example, the maximum EHF score in a patient with grade 2 disabilities in both eyes, both hands, and both feet would be 12.
Activity Limitation[edit | edit source]
Loss of manual dexterity: The paralysis of hand muscles causes a loss of manual dexterity. Subjective and objective outcome measurement tool scan be used. In leprosy, a tool with 20 questions, the SALSA (Screening of Activity Limitation and Safety Awareness Score), is commonly used to help identify patients’ perceptions of their functional ability to use their hands, feet, and eyes.
Locomotion limitations: The presence of foot deformities causes problems in locomotion. The patient may have gait abnormalities or may not be able to walk. Deformities such as foot drop can cause a high stepping gait, leading to postural abnormalities and imbalance. Foot drop and anesthesia further increase the risk of developing plantar ulcers.
Visual impairments: Visual impairments can lead to an inability to perform self-care, personally groom, or maintain good hygiene, as well as interfere with employment and many daily activities.
Preventing Further Deterioration of Impairments[edit | edit source]
The goal of the rehabilitation team should be to prevent any new impairment or the worsening of a primary impairment to a secondary impairment. These can be done via:
- Exercises: Different type of exercise should be prescribed based upon the muscle strength of the respective muscles.
| MRC Grading | ‘S’ ‘W’ ‘P’ Score | Exercise Prescription |
| 0 | ‘P’ – Paralyzed | Passive Exercise |
| 1 |
| |
| 2 | Active and
Active Assisted | |
| 3 | ||
| 4 | Active | |
| 5 | ‘S’ – Strong | Active Resisted |
- Splinting: Splints are supportive devices that are primarily used to immobilize a part of the body so as to prevent contractures, to relieve pain from neuritis.
- Tendon transfer surgeries: pre- post rehabilitation for respective tendon is required.
- Self care:
- Self-care for eyes
- Think Blink’ is one of the best methods of preventing such complications. The patient is taught to deliberately close the eye at regular intervals. If the patient remembers to blink every few minutes, the risk of corneal damage can be reduced.
- Wear protective eyeglasses to help prevent dust and insects from damaging the eye and to prevent dryness on the surface of the eye.
- Cover the head during sleep with a clean bed sheet or towel, and wear a wide-brimmed hat or cover the eye with any available cloth during the day, to prevent damage to the eye from foreign particles and insects.
- Perform passive eye exercises to maintain muscle tone and prevent atrophy.
- Wash the eye with clean water at least twice a day to flush out dirt and to prevent dryness.
- Inspect the eye in a mirror to help the early detection of redness or injury.
- Avoid rubbing the eye at all costs, as it can compound damage.
- Self- care for hands and feet
- Use thick cloth or gloves for insulation when handling hot objects to protect insensate hands.
- Use tools with wooden or rubber-covered handles to help prevent injury.
- Use grip aids and splints to protect hands.
- Wear appropriate footwear to protect insensate feet.
- Use appropriate footwear to help prevent plantar ulcers.
- Soak a palm or sole with sensory loss for 20 minutes in cool clean water to make the skin supple. Then rub off the hard skin with a scrapper stone, which keeps the skin soft. Oil the wet skin to help retain moisture and prevent dryness.
- Include inspecting as well as soaking, scraping, and oiling in the self-care routine to help the early detection of issues.
- Inspect the anaesthetic area for injuries, or even red spots, swelling, and cracks and take adequate precautions to prevent the wound from becoming bigger.
- Treat simple wounds at home by bandaging with a clean cloth. A wound area on the hand should be rested; one on the foot should be offloaded. Immediately report any signs of infection to the physician for further management.
- Make lifestyle modifications to protect the hands and feet from being injured.
- Footwear
- Feet that have sensory loss are at a high risk of thermal and repetitive pressure injuries, as well as injuries from sharp objects. Therefore, the care and protection of the foot should be accorded the highest priority. Patients with existing secondary impairments, such as shortening, plantar ulcers, or deformed feet, require specialized footwear.[11]Microcellular Rubber footwear are used to redistribute pressure to cushion the feet and provide adequate protection
- Self-care for eyes
| Foot Assessment | Footwear and Orthoses to be prescribed |
| No deformities | MCR footwear or any appropriate footwear |
| Claw toes and forefoot scarring | MCR footwear with a metatarsal pad |
| Pronated subtalar joint | MCR footwear with a tarsal cradle |
| Hyper pronated subtalar joint | MCR footwear with a hatti pad |
| Supinated subtalar joint | MCR footwear with a heel cup or tarsal platform |
| Ulcer on the metatarsal head on a supinated foot | MCR footwear with a plantar metatarsal pad |
| Ulcer on the metatarsal head on a pronated subtalar joint | MCR footwear with a plantar metatarsal pad and a tarsal cradle |
| Neuro arthropathy | Fixed Ankle Brace |
| Shortened and scarred foot | Patellar Tendon Bearing Brace |
Differential Diagnosis[edit | edit source]
- Vitiligo
- Tinea versicolor
- Pityriasis alba
- Post kalazar dermal leishmaniasis
- Sarcoidosis
Leprosy Prevention and Control[edit | edit source]
Prevention of leprosy
- Early detection through survey and initiation treatment
- Families of patients to be kept under surveillance
- Improvement in socio-economic conditions
- Vaccination with BCG partially protective for leprosy, single dose-50% protective
Control of leprosy
- Clinical management of active cases as well as contact management
- Household contacts to be evaluated annually for evidence of disease for at least five years
Resources[edit | edit source]
Physical Rehabilitation In Leprosy ( International textbook of Leprosy)
References[edit | edit source]
- ↑ 1.0 1.1 World Health Orgaization. Leprosy ( hansen's disease). Available from: https://www.who.int/health-topics/leprosy#tab=tab_1 Lasted accessed: 26th January 2022
- ↑ 2.0 2.1 Parkash O. Classification of leprosy into multibacillary and paucibacillary groups: an analysis. FEMS Immunology & Medical Microbiology. 2009 Jan 1;55(1):1-5.
- ↑ 3.0 3.1 World Health Organization. Leprosy/Hansen Disease: Management of reactions and prevention of disabilities. Available from: https://www.who.int/publications/i/item/9789290227595 Lasted accessed: 29th January 2022
- ↑ 4.0 4.1 World health Organization. Leprosy. Available from: https://www.who.int/news-room/fact-sheets/detail/leprosy last accessed: 26th Jan 2022
- ↑ 5.0 5.1 5.2 CenterS for Disease Control and Prevention. Hansen's Disease (Leprosy). Available from: https://www.cdc.gov/leprosy/world-leprosy-day/index.html#:~:text=Around%20the%20world%3A,Hansen's%20disease%2Drelated%20disabilities%20globally. lasted accessed: 29th January 2022
- ↑ 6.0 6.1 Bhat RM, Prakash C. Leprosy: an overview of pathophysiology. Interdisciplinary perspectives on infectious diseases. 2012 Sep 4;2012.
- ↑ How Does Leprosy Damage the Human Body? Available from: https://www.youtube.com/watch?v=n-TZ0o-O8Ts. Last accessed: 26th Jan 2022
- ↑ Raffe SF, Thapa M, Khadge S, Tamang K, Hagge D. Diagnosis and Treatment of Leprosy Reactions in Integrated Services-The Patients’. Perspective in Nepal’, PLoS Neglected Tropical Diseases. 2013;7(3).
- ↑ Bhat RM, Prakash C. Leprosy: an overview of pathophysiology. Interdisciplinary perspectives on infectious diseases. 2012 Sep 4;2012.
- ↑ 10.0 10.1 Available from: https://apps.who.int/iris/bitstream/handle/10665/274127/9789290226383-eng.pdf
- ↑ 11.0 11.1 The International Textbook of Leprosy (pp.Physical Rehabilitation In Leprosy). Published by American Leprosy Missions. Available at: https://www.researchgate.net/publication/330554640_Physical_Rehabilitation_In_Leprosy
- ↑ Available from:https://www.youtube.com/watch?v=N2hsD2QH6Q8