Introduction to Affirming Care for Gender and Sexual Minorities
Original Editor - Ewa Jaraczewska based on the course by Brianna Durand
Top Contributors - Ewa Jaraczewska, Kim Jackson, Jess Bell and Tarina van der Stockt
Introduction[edit | edit source]
In the healthcare environment, LGBTQ+ adolescents and adults experience marginalisation, stigma and normative pressure resulting in poor health and social outcomes.[1][2] This may be due to healthcare providers' lack of training and sensitivity to the health needs of LGBTQ+ people.[1] Healthcare workers report being uncomfortable communicating with sexual and gender minorities (SGMs) patients.[3] Additionally, chronic stress related to marginalisation and discrimination contributes to healthcare disparities among the SGMs group.[4] They not only experience poorer health, but also worse healthcare experiences.[2] Yet, their healthcare needs are well documented, as various reports indicate high rates of substance abuse, depression, suicide, and cardiovascular disease.[2]
Gender and sexual minorities live in every part of the world and comprise all races and/or ethnicities, religions, and social classes. They require access to healthcare to meet their medical needs. At the same time, healthcare organisations must ensure that their environment is inclusive for LGBTQ+ patients by educating staff on cultural awareness and nondiscrimination policies.[5]
Gender-Neutral Language[edit | edit source]
A worldwide movement to develop a language representing gender identity and sexual orientation is currently underway. LGBTQ+ activists and linguists are working on creating entirely new non-binary terms and changing already existing words and grammar constructions.[6] The following are examples of gender-neutral language changes that were introduced to English and other languages:
- English: there is no distinction between genders except for singular pronouns, which can be masculine or feminine. In 2019, “they” was added to the Merriam-Webster dictionary as the pronoun to use for a “single person whose gender identity is non-binary.”[6]
- Spanish: all nouns have feminine and masculine cases. In daily conversation, the masculine “o” or the feminine “a” is now replaced with the gender-neutral “e” in certain words.[6]
- Arabic: each verb, noun and adjective is always assigned either a male or female case. General awareness and tolerance of gender-neutral language remains extremely low in Arabic-speaking countries.[6]
- Hebrew: gender is assigned to verbs, nouns, and adjectives based on the noun. In gender-neutral language, there is a default to a feminine plural or a “mixed” gender, sometimes male and sometimes female for the same person.[6]
- German: includes male, female and neutral grammatical genders, signified by the suffixes “r” or “rn” for men, and “in” or “innen” for women. In gender-neutral language, the uppercase "I" in compound nouns is used to address both males and females at once. A "gender star" in the form of an asterisk has also been added to include persons who do not consider themselves either."[6]
- French uses male or female gender in all nouns referring to an individual. The first step in gender-neutral language was to use asterisks to combine case endings to create gender-neutral plurals, for example, “ami•e•s” for friends.[6]
- Swedish: the word “hen” was added to the official dictionary, which indicates a gender-neutral pronoun as an alternative to the male pronoun “han” and female “hon".[6]
Learn more about gender-neutral language here.
Gender and Sexual Minorities[edit | edit source]
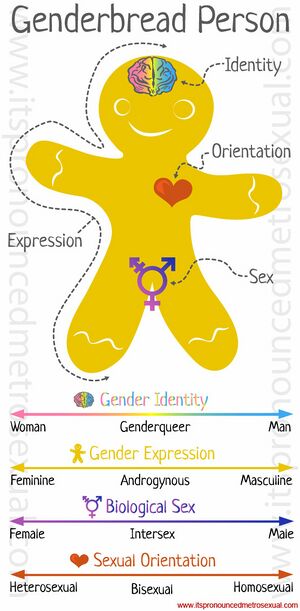
Gender identity and sexual orientation are not the same things. Gender is a spectrum. Sexual orientation defines attraction and biological sex. Binary sex refers to maleness or femaleness. Intersex can define individuals who move from one sex to the other across their lifetime or who are born with a different degree of maleness or femaleness.[7]
LGBTQQIIP2SAA+ stands for lesbian, gay, bisexual, transgender, questioning, queer, intersex, intersectional, pansexual, two-spirit (2S), androgynous and asexual. This is the most complete acronym to date for gender and sexual minorities.[8]
- Lesbian: women who are romantically and/or sexually attracted to women.[7]
- Gay: usually identifies men with romantic and/or sexual attraction to men.[7]
- Bisexual: an individual who is sexually, romantically, physically, and/or spiritually attracted to more than one gender.[9] Someone who is attracted to the same gender as their own and another gender.[8]
- Transgender: people whose gender identity does not correspond to the sex they were assigned at birth.[7]
- Questioning: person searching for their gender identity and/or sexual orientation.[9]
- Queer: a person who does not conform to cultural norms regarding gender or sexuality and who is attracted to people of many genders.[9] A term that includes anybody who is not cisgender and heterosexual, and is also used as a sexual orientation for those who don't really have a label.[8]
- Intersex: individuals who are born with components of traditionally male and female anatomy.[8]
- Intersectionality: “the network of connections between social categories such as race, class and gender, especially when this may result in additional disadvantage or discrimination”.[11]
- Pansexual: an individual who is sexually, romantically, physically, and/or spiritually attracted to members of all gender identities.[7]
- Two-spirit: a person whose gender identity has two spirits: masculine and feminine.
- Androgynous: a person whose gender expression does not fit into gender norms.[9]
- Asexual: Someone who does not experience a sexual attraction and/or has no interest in pursuing a sexual relationship with others. An individual with a persistent lack of sexual attraction towards any gender.[7]
You can read more about asexuality here.
Other acronyms and descriptions related to gender identity and sexual orientation:
- Folx = folks (people) is used to highlight the inclusion of groups commonly marginalised
- TGNC stands for Transgender and Gender Nonconforming.
- Gender Nonconforming describes someone who does not conform to gender expectations (example: assigned female at birth, identifies as a woman, but has masculine presentation: short hair, wears men's clothes, etc).
- Cisgender: an individual who identifies with the gender assigned at birth.[8]
- Agender: persons who feel that they have no gender.[8]
- Genderfluid or genderqueer: people who feel like their gender fluctuates.[8]
- Monosexual: attracted to one type of gender identity.[8]
- Polysexual: attracted to several types of gender identities.[8]
- Homoromantic: a person interested in having relationships romantically with one person.
- Heteroromantic: a person interested in having a relationship with two different genders.
- Biromantic: person romantically attracted to people of two specific and distinct gender identities.
- AMAB: Assigned male at birth.
- AFAB: assigned female at birth.
Cultural Competence[edit | edit source]
According to Cross and colleagues,[14] cultural competence is “a set of congruent behaviours, attitudes and policies that come together in a system, agency or amongst professionals and enables that system, agency or those professionals to work effectively in cross-cultural situations.”[14] Cultural competence aims to enhance healthcare delivery by providing quality care that is unbiased and culturally sensitive, where diversity is respected and the healthcare outcome is not affected by providers' language, communication styles, attitudes, and behaviours.[15] [16]
"Cultural competence is simply making an effort to reduce any cultural, linguistic, or other barriers that exist between, in this case, patients and medical professionals, such as yourself."[8] Dr Durand
A systematic review of literature on the LGBTQ+ communities demonstrated that their inability to access equitable healthcare may have a profound impact on their overall well-being. They report having to teach providers about their healthcare-related needs, experiencing provider discrimination, receiving inappropriate care recommendations, and even that the care they need is denied.[17]
Cultural competence in healthcare can be achieved through appropriate staff training. Staff should be taught reflective awareness, empathy, and active listening techniques when facing racial and ethnic differences, or when attending to marginalised population.[15]
LGBTQIA+ Demographic[edit | edit source]
In 2021, the global survey on gender identity worldwide was conducted and the responders from 27 countries were asked about their gender identities and sexual orientations. The results were as follows:[18]
- 3% of respondents declared themselves to be homosexual, gay, or lesbian
- The largest group of bisexual respondents were from India (9%)
- 1% of the interviewees declared themselves to be pansexual or omnisexual (attracted to people of all gender identities and sexual orientations)
- 2% identified themselves as transgender, non-binary/non-conforming/gender-fluid, or in another way.
- 3% of responders from Germany and Sweden identified themselves as gender or sexual minority.
The 2021 Gallup conducted a survey on LGBT Identification in United States (U.S.). The results were as follows: [19]
- 7.1%of U.S. adults self-identified as being lesbian, gay, bisexual, transgender or something other than heterosexual
- 21% of Generation Z Americans identify as LGBT
- 10.5% of Millennials identified themselves LGBT
- 57% of LGBT Americans indicate they are bisexual, which account for 4.0% of all U.S. adults
- 21% of LGBT Americans indicate they are gay, 14% lesbian, 10% transgender and 4% something else
- 6.0% of women say they are bisexual as compared to 2.0% of men
According to the 2019 U.S. Census Bureau, 5.6% of the U.S. population is LGBTQIA+ (18.5 million people).[8]
Please watch this short video highlighting the life of elderly LGBTQIA+ in the US.
Physiotherapy Needs in LGBTQIA+ Community[edit | edit source]
The physiotherapy needs of the LGBTQ+ population are high, but services are often delayed.[21] Patients from this community may avoid early intervention due to fear of stigma, discrimination, and physiotherapists' lack of knowledge about LGBTQ+-specific health issues.[22] These factors may lead to health conditions that are poorly controlled.[21] Ross and Setchell[22] describe challenges LGBTQ+ individuals face when attending physiotherapy, which may include limited skills to treat their pelvic pain, bowel, bladder, or sexual symptoms.[22] In addition, minority stress experienced by LGBTQ+ patients may influence their recovery and outcomes.[23] To optimise the care of gender and sexual minorities, they should be referred to all needed speciality services early in the process to facilitate recovery.[21]
Medical issues commonly present in LGBTQIA+ individuals:
- Urinary tract infections: often related to holding the urine too long due to a lack of gender-neutral restrooms
- Gender dysphoria leading to postural changes: rounded shoulders, forward head, thoracic kyphosis
- Respiratory issues and pelvic floor issues related to inadequate engagement of the diaphragm as a consequence of poor posture
- Urinary tract complications including incontinence, urgency, or frequency
Clinical settings where care for LGBTQ+ individuals is delivered: outpatient orthopaedics, Long Term Care (LTC) facilities, Skilled Nursing Facilities (SNFs), home health, acute care, and paediatric clinics.
Specialities involved in care for LGBTQ+ individuals:
- Orthopaedics: complications related to removal or augmentation of chest tissue, including thoracic spine mobility, upper extremity mobility, scar tissue, pain
- Pelvic Floor Health: medical transition and gender-affirming surgery, physiotherapy for the pelvic floor, dilator training after vaginoplasty
Resources[edit | edit source]
- National Standards for Culturally and Linguistically Appropriate Services in Health Care. Final report. Available from https://minorityhealth.hhs.gov/assets/pdf/checked/finalreport.pdf
- The State of the LGBTQ Community in 2020. A National Public Opinion Study. Available from https://www.americanprogress.org/article/state-lgbtq-community-2020/
- What Does Gender and Inclusion Mean for Clinical Practice?
- The Genderbread Person – https://www.genderbread.org/
References[edit | edit source]
- ↑ 1.0 1.1 Wahlen R, Bize R, Wang J, Merglen A, Ambresin AE. Medical students’ knowledge of and attitudes towards LGBT people and their health care needs: Impact of a lecture on LGBT health. PloS one. 2020 Jul 1;15(7):e0234743.
- ↑ 2.0 2.1 2.2 Elliott MN, Kanouse DE, Burkhart Q, Abel GA, Lyratzopoulos G, Beckett MK, Schuster MA, Roland M. Sexual minorities in England have poorer health and worse health care experiences: a national survey. J Gen Intern Med. 2015 Jan;30(1):9-16.
- ↑ Hinchliff S, Gott M, Galena E. 'I daresay I might find it embarrassing': general practitioners' perspectives on discussing sexual health issues with lesbian and gay patients. Health Soc Care Community. 2005 Jul;13(4):345-53.
- ↑ Hughes TL, Jackman K, Dorsen C, Arslanian-Engoren C, Ghazal L, Christenberry-Deceased T, Coleman C, Mackin M, Moore SE, Mukerjee R, Sherman A, Smith S, Walker R. How can the nursing profession help reduce sexual and gender minority-related health disparities: Recommendations from the national nursing LGBTQ health summit. Nurs Outlook. 2022 Apr 13:S0029-6554(22)00013-6.
- ↑ Goldhammer H, Maston ED, Kissock LA, Davis JA, Keuroghlian AS. National findings from an LGBT healthcare organizational needs assessment. LGBT health. 2018 Dec 1;5(8):461-8.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 6.7 A guide to how gender-neutral language is developing around the world. Available from https://www.washingtonpost.com/world/2019/12/15/guide-how-gender-neutral-language-is-developing-around-world/ [last access 6.6.2022]
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 Lesbian, Gay, Bisexual, Transgender, Queer,&Intersex Life. Available from https://www.vanderbilt.edu/lgbtqi/resources/definitions [last accessed 9.6.2022]
- ↑ 8.00 8.01 8.02 8.03 8.04 8.05 8.06 8.07 8.08 8.09 8.10 Durand B. LGBTQ and Transgender Informed Care - Introduction to Affirming Care for Gender and Sexual Minorities. Part 1 &2. Plus Course 2022
- ↑ 9.0 9.1 9.2 9.3 What is LGBTQ? Available from https://gaycenter.org/about/lgbtq/#questioning [last accessed 9.06.2022]
- ↑ Teen Voque: What Was Done To These Intersex People Was Not Okay | Teen Vogue. 2017. Available from: https://www.youtube.com/watch?v=mT4dDO-ZwcQ[last accessed 11/6/2022]
- ↑ Intersectionality.(n.d) In Oxford Learner's Dictionaries. Available from https://www.oxfordlearnersdictionaries.com/definition/english/intersectionality?q=intersectionality [last access 7.06.2022]
- ↑ Kimberlé Crenshaw: What is Intersectionality? 2018. Available from: https://www.youtube.com/watch?v=ViDtnfQ9FHc[last accessed 6/6/2022]
- ↑ TED: The way we think about biological sex is wrong | Emily Quinn 2019. Available from: https://www.youtube.com/watch?v=stUl_OapUso[last accessed 6/6/2022]
- ↑ 14.0 14.1 Cross TL, Bazron BJ, Dennis KW, Isaacs MR. Toward a Culturally Competent System of Care. National Institute of Mental Health, Child and Adolescent Service Program (CASSP) Technical Assistance Center, George-town University Child Development Center; 1989.
- ↑ 15.0 15.1 Improving Cultural Competence to Reduce Health Disparities for Priority Populations. Available from https://effectivehealthcare.ahrq.gov/products/cultural-competence/research-protocol [last accessed 9.06.2022]
- ↑ Saha S, Beach MC, Cooper LA. Patient centeredness, cultural competence and healthcare quality. J Natl Med Assoc. 2008 Nov;100(11):1275-85.
- ↑ Butler M, McCreedy E, Schwer N, Burgess D, Call K, Przedworski J, Rosser S, Larson S, Allen M, Fu S, Kane RL. Improving Cultural Competence to Reduce Health Disparities [Internet]. Rockville (MD): Agency for Healthcare Research and Quality (US); 2016 Mar. Report No.: 16-EHC006-EF.
- ↑ LGBTQ+ worldwide - Statistics & Facts. Available from https://www.statista.com/topics/8579/lgbtq-worldwide/#dossierKeyfigures [last access 11.06.2022]
- ↑ Jones JM.LGBT Identification in U.S. Available from https://news.gallup.com/poll/389792/lgbt-identification-ticks-up.aspx [last access 3.06.2023]
- ↑ Stewart Maddux. Gen Silent, The LGBT Aging Documentary: Official Trailer. 2009. Available from: https://www.youtube.com/watch?v=fV3O8qz6Y5g[last accessed 6/6/2022]
- ↑ 21.0 21.1 21.2 Tollinche LE, Walters CB, Radix A, Long M, Galante L, Goldstein ZG, Kapinos Y, Yeoh C. The perioperative care of the transgender patient. Anaesthesia and analgesia. 2018 Aug;127(2):359.
- ↑ 22.0 22.1 22.2 Ross MH, Jenny Setchell J. People who identify as LGBTIQ+ can experience assumptions, discomfort, some discrimination, and a lack of knowledge while attending physiotherapy: a survey. Journal of Physiotherapy, 2019; 65 (2): 99-105.
- ↑ Torres JL, Gonçalves GP, Pinho AD, Souza MH. The Brazilian LGBT+ Health Survey: methodology and descriptive results. Cadernos de saude publica. 2021 Oct 15;37:e00069521.