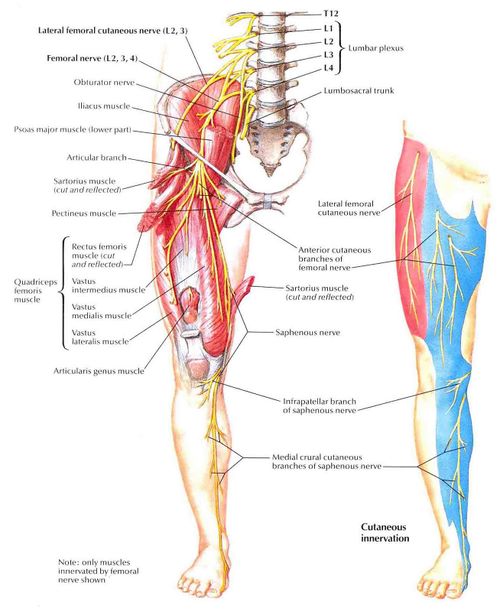
Gonalgia paresthetica
Introduction[edit | edit source]
Saphenous neuritis as it is commonly known as (also Gonalgia Paresthetica ) is a chronic irritation of the saphenous nerve.
This pathology is caused by a compression or irritation of the saphenous nerve which develops pain in many cases on the anterior side of the knee or on the medial side of the knee.
- Symptoms of saphenous nerve entrapment may include a deep thigh ache, knee pain, and paresthesias in the nerve’s cutaneous distribution in the leg and foot.
- The infrapatellar branch may become entrapped on its own because it passes through a separate foramen in the sartorius tendon.
- It may also be exposed to trauma where it runs horizontally across the prominence of the medial femoral epicondyle.
- Patients report paresthesias and numbness in the infrapatellar region that worsen with knee flexion or compression by garments or braces.
Saphenous nerve entrapment is a frequently overlooked cause of persistent medial knee pain in patients who experience trauma or direct blows to the medial aspect of the knee. Because the saphenous nerve is purely sensory, an isolated injury to this nerve should not result in weakness.[1]
Clinically Relevant Anatomy[edit | edit source]
The saphenous nerve is the largest cutaneous branch of the femoral nerve. This nerve travels with the superficial femoral artery and vein, and passes through the adductor canal. From the adductor canal it continues toward the skin of the medial lower leg and foot. The floor of the saphenous nerve is composed of the adductor longus and magnus, and this nerve borders anterolateral to the Vastus Medialis. The saphenous nerve innervates the sartorius and the vastus medialis.
Characteristics/Clinical Presentation
Saphenous neuritis occurs mainly to adults after a physical activity or after other strenuous activities such as a walk or after a long day at work.
- The pain is especially felt in response to limb movements that cause nerve stretch.
- Pain characterized by saphenous neuritis is mostly activity-related pain, but it can also be characterized as rest-pain.
- Clinical research shows elective pressure pain in the canal of Hunter (Adductor Canal) at the height of the medial thigh.
- It can also find diffuse tenderness at the medial structures and at the pes anserinus.
- This pathology can appear beside other common problems, such as osteoarthritis or patellofemoral pain syndrome.
- The clinical appearance of saphenous neuritis is characterized by allodynia along the nerve.
- Many studies concluded that it is very important to know the anatomy of this nerve to evaluate and treat saphenous neuritis correctly. There are different causes of saphenous neuritis.
- The most frequent cause is the compression of the nerve, along its anatomic course, the Adductor Canal.
- The pain is most sensible at the joint line associated with hyperaesthesia or hypoaesthesia on the medial side of the lower leg (knee) when it’s caused by compression. [2]
A few causes which may produce saphenous neuritis, on a direct and indirect manner.
- DIRECT: Trauma (for example: rotation injury) Direct contact: compression (for example: Dashboard injury) Cut-incision Scar-synovial Resection Stretch PLRI (Posterolateral Rotator Instability)
- INDIRECT Reflex Sympathetic dystrophy, Fibromyalgia, Lumbar Disc Disease, Degenerative joint disease of the knee, Meniscal tear, Surgery (see below)
Neuropathic knee pain (particularly of the infrapatellar branch of the Ramus Infrapattelaris), is an important complication of knee replacement surgery, with an incidence as high as 70%. The increasing number of elderly patients requiring knee surgery, including total knee arthroplasty (TKA), has contributed to an increase in the number of patients with this pathology. Treatment includes neurectomy, infiltration therapy, and cryodenervation. Percutaneous cryodenervation of the infrapatellar branch is a promising option.[3]
Diagnostic Procedures[edit | edit source]
- Medial pain at the knee is often a primary indication of saphenous neuritis, but sometimes the pain develops a few days after the initial injury.
- The pain of saphenous neuritis only appears with exercise or play activity.
- It can be devastating, but may also come and go.
- The pain can be characterized by sharp pain or constant pain.
- When the patient has pain on the anterior or/and medial side of the knee, especially on the joint line during palpation 7.3 cm proximal and 9.8 cm medial to the superior pole of the patella, it is an important indication of saphenous neuritis.
- For a physiotherapist, the most efficient hallmark of saphenous neuritis is tenderness to light palpation along the nervus saphenous’ course.
- The tenderness may mainly apparent at the nerve’s exit from the adductor canal, near the medial joint line or along the nerve in the proximal third of the leg. Starting from the adductor canal, it is possible to elicit the exact course of the irritated saphenous nerve.
- In some cases, an electromyography (EMG), which tests the activity of the muscles and the sensory guidance, can show a delayed conduction of the saphenous nerve. This feature is mostly related to neuritis of this nerve.[4][5][6][7]
Examination[edit | edit source]
It is important for a physiotherapist to recognize saphenous neuritis immediately during the diagnosis of a knee-injury. Otherwise it can confuse the patient’s clinical picture, complicate treatment and compromise results. It should be part of every routine while examining the knee.
Treatment[edit | edit source]
When saphenous neuritis is diagnostically confirmed with palpation, the best option consists is nonsurgical care. The video below shows how to floss the nerve and home exercises
- This may include activity modification and/or oral analgesics (including narcotics and nonsteroidal anti-inflammatory medication, protective padding, topical analgesic cream, etc.).
- Treatment may be directed at release of the saphenous nerve from the entrapment site via transverse friction technique, functional biomechanical faults corrected, flossing of the nerve and TENS may be utilized to control pain associated with the entrapment syndrome.
- Symptoms of saphenous neuritis may subside with time.
If it is not the case, injection of local anesthetic, without corticosteroid, can be initiated.
When this does not solve the neuritis, surgical intervention is recommended by decompression, or neuroma excision may follow.[2]
References
- ↑ Medscape Logo, Sunday, March 1, 2020 What are the signs and symptoms of saphenous nerve entrapment? Available from:https://www.medscape.com/answers/2225774-32346/what-are-the-signs-and-symptoms-of-saphenous-nerve-entrapment (last accessed 2.3.2020)
- ↑ 2.0 2.1 Morganti CM, McFarland EG, Cosgarea AJ. Saphenous neuritis: a poorly understood cause of medial knee pain. JAAOS-Journal of the American Academy of Orthopaedic Surgeons. 2002 Mar 1;10(2):130-7. Available from:https://www.ncbi.nlm.nih.gov/pubmed/11929207 (last accessed 1.3.2020)
- ↑ Thomas Ackmann MD, Monika Von Düring MD, Wolfram Teske MD, Ole Ackermann MD, Peter Müller MD, Christoph Von Schulze Pellengahr MD. Anatomy of the infrapatellar branch in relation to skin incisions and as the basis to treat neuropathic pain by percutaneous cryodenervation. Pain Physician. 2014 May;17:E339-48. Available from:https://www.ncbi.nlm.nih.gov/pubmed/24850115 (last accessed 1.3.2020)
- ↑ DUDLEY M.D., FERRARI A., 2008. Reflections and Conclusions about the Problem Knee. Mill City Press.
- ↑ Martinelli, P., Montagna, P. & Coccagna, G. Neuropathy of the infrapatellar branch of the saphenous nerve in the differential diagnosis of knee pain. Ital J Neuro Sci 3, 153–154 (1982). https://doi.org/10.1007/BF02043950 Available from:https://link.springer.com/article/10.1007%2FBF02043950 (last accessed 2.3.2020)
- ↑ Tennent TD, Birch NC, Holmes MJ, Birch R, Goddard NJ. Knee pain and the infrapatellar branch of the saphenous nerve. Journal of the Royal Society of Medicine. 1998 Nov;91(11):573-5. Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1296949/ (last accessed 2.3.2020)
- ↑ HULSE R, WYNICK D, DONALDSON L.F., 2009. Intact cutaneous C fibre afferent properties in mechanical and cold neuropathic allodynia. Elsevier.
- ↑ Brain Abelson Flossing saphenous nerve Available from:https://www.youtube.com/watch?v=l2ywfkqYeWQ&feature=youtu.be (last accessed 2.3.2020)