Epidemiology of Spinal Cord Injury
Original Editor - Naomi O'Reilly
Top Contributors - Naomi O'Reilly, Kim Jackson, Tarina van der Stockt, Rucha Gadgil and Jess Bell
Introduction[edit | edit source]
Spinal cord injury impacts an individual’s physical, psychological, and social well-being and places a substantial financial burden on health care systems worldwide. While historically spinal cord injury has been associated with very high mortality rates, the work of the American Neurosurgeon Dr Donald Munro at Boston City Hospital in the 1930s, emulated by Sir Ludwig Guttmann at Stoke Mandeville Hospital in the United Kingdom in 1944, saw the beginning of effective treatment and management of spinal cord injury. As a result of 2-hourly turning and skincare, together with better bladder management, the prevailing 80% mortality rate for spinal cord injury began to decline, and improved functional outcomes were achieved with physical and occupational therapy, and more holistic care. [1]
Today spinal cord injury is preventable; spinal cord injury is survivable; spinal cord injury need not prevent a good quality of life and full contribution to society. [1] While this change reflects better medical provision in higher-income countries, which means that people are able to survive, live and flourish after injury, in many low-income countries the situation is very different and spinal cord injury still too often remains a terminal condition. Yet the fact that such dramatic progress in survival and participation has been seen in high-income countries over a relatively short period of time should be a reason to be optimistic for other parts of the world. [2][3]
Being able to quantify both the incidence and prevalence of spinal cord injury allows us to better understand the rates of occurrence and delineate ways of prevention, which enables health care providers to estimate both the cost and psychosocial burden of this disease and the resources required leading to improvements in spinal cord injury management. With the right policy responses, it should be possible to live, thrive and contribute with SCI anywhere in the world. Here we will review some findings from the literature with regards to the incidence and prevalence of spinal cord injury worldwide, age and gender distribution, and risk factors associated with spinal cord injury. [2][3]
Etiology[edit | edit source]
Spinal Cord Injury can occur as a result of non-traumatic causes (16%) and traumatic causes (84%), although recent studies indicate a slight trend in recent years towards an increase in the share of non-traumatic spinal cord injury.
Non-traumatic spinal cord injuries occur as a result of disease, infection and congenital defects with the leading causes being neoplastic tumours and degenerative conditions of the spinal column, followed by vascular and autoimmune disorders.
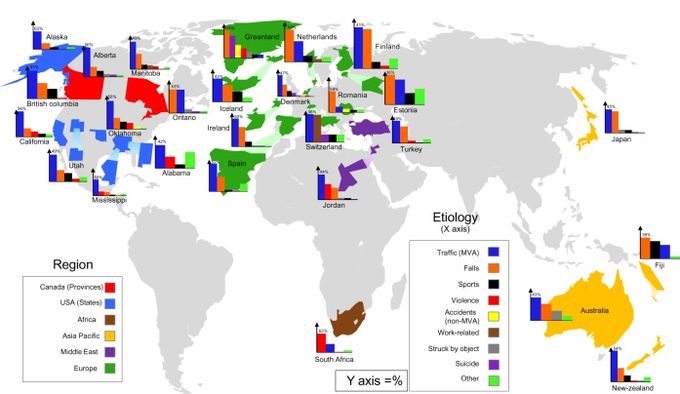
Traumatic spinal cord injuries most commonly occur as a result of motor vehicle and motor-bike accidents, followed by falls. Sport, in particular, water-based activities and work-related injuries are also common, with a further small but increasing contribution from a gun, knife or war-related injury.[2][3][5][6]
| Cause | Conditions | |
|---|---|---|
| Traumatic | Motor Vehicle Accidents (36 - 48%); Falls (17 - 21%), Sport Injuries; Violence (5 - 29%); Self-harm; Work-related Accidents | |
| Non-Traumatic | Congenital & Developmental | Spinal Dysraphism; Skeletal Malformations; Arnold Chiari Malformations; Diastematomyelia; Spina Bifida |
| Degenerative CNS Disorders | Amyotrophic Lateral Sclerosis; Friedreich’s Ataxia; Hereditary Spastic Paraparesis; Infantile Neuroaxonal Dystrophy; Pelizaeus-Merzbacher Disease; Canavan’s Disease; Spinal Muscular Atrophy | |
| Genetic & Metabolic | Glutathione; Methylcrotonylglycinuria; Gangliosidosis; Myelin Protein Zero; Adrenomyeloneuropathy; Abetalipoproteinaemia; Vitamin B12 Deficiency | |
| Inflammatory | Multiple Sclerosis; Transverse Myelitis | |
| Ischemic | Arterial vs Venous
Aortic Dissection; Cardiac Arrest; Systemic Hypotension; Atherosclerosis; Thrombosis; Embolism; Iiatrogenic (Aortic Repair); Arteriovenous Malformations | |
| Rheumatological | Spondylolysis; Stenosis; Disc Disease; Paget’s Disease; Rheumatoid Arthritis; Posterior Longitudinal Ligament Ossification | |
| Toxic | Methotrexate; Cytosine Arabinoside; Radiation | |
| Tumors | Primary or Metastatic
Intramedullary or Extramedullary | |
| Infectious | Viral: Herpes Simplex; Varicella-Zoster; Cytomegalo; Human T Cell Leukaemia; HIV, Polio | |
| Bacterial: Pott’s Disease, Mycobacterium App | ||
| Fungal: Cryptococcus Spp | ||
| Parasitic: Toxoplasma Gondii; Schistosoma Mansoni | ||
Prevalence[edit | edit source]
Prevalence is the proportion of a population living with a disease at a particular time and is key information required to estimate the demand for both health and social care support, and for assessing the impact of secondary prevention measures. Data on the prevalence of spinal cord injury is sparse, with limited reliable global or regional estimates of all-cause spinal cord injury prevalence. [1]
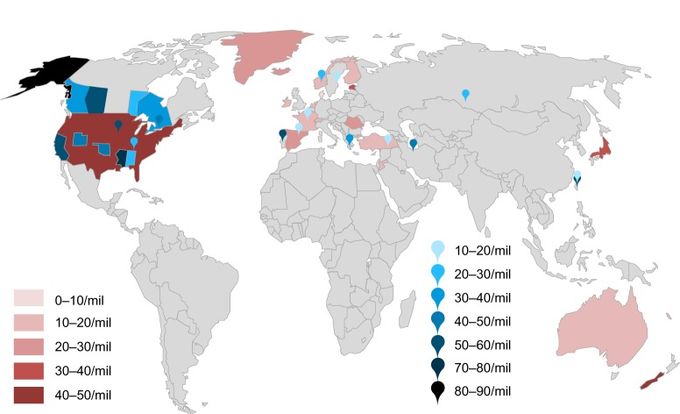
The current available research show variance in the global prevalence of spinal cord injury anywhere from 236 to 1298 per million of population, although all show a recent trend in increasing prevalence over the last decade. A recent systematic review found the prevalence of spinal cord injury to be dependent on the region the studies were conducted in, ranging from the highest prevalence of 906 per million in the USA and the lowest prevalence of 250 per million in Rhone-Alpes, France. [2] While further studies found similar results with prevalence ranging from 1298 per million to 50 per million. [3]
Incidence[edit | edit source]
The incidence of a disease is the number of new cases in a population at risk in a given time period. While a relatively rare condition, spinal cord injury is life-altering and costly, both for health care systems and the individual, with a mortality risk that varies widely by country and depends heavily on the availability of quality and timely clinical care and rehabilitation services.[1]
It is unclear how many people in the world are currently living with a spinal cord injury, as much of the available research report crude incidence, and therefore comparisons between countries, states/provinces, and regions could not be made. Global incidence shows a huge variance from 8 to 246 cases per million of the population in one study, while further research found similar results with 3.3 to 246 per million, so anywhere from 250,000 to 500,000 new spinal cord injuries annually. [2][3]
Annual incidence rates also varied significantly between region, ranging from 246 per million in Taiwan, 49.1 per million in New Zealand to just 10.0 per million in Fiji. Similarly, studies available also show a high male-to-female ratio of 5:1 and peak incidence of spinal cord injury occurring at 42 years old, increased from 29 years old in 1970 with a gradual increase in the proportion of non-traumatic spinal cord injury cases, which have been partly attributable to the world’s ageing population. [1][2][3]
Mortality and Life Expectancy[edit | edit source]
Longer life expectancy with a decreased risk of mortality from secondary conditions is evident for individuals with a spinal cord injury in high-income countries as a result of improvements in recognition, evaluation, pre-hospital management, trauma care services, general clinical care and rehabilitation services for spinal cord injury. Although overall research has indicated that individuals with a spinal cord injury die earlier than those without a spinal cord injury, and are 2 to 5 times more likely to die prematurely. [1]
Mortality risk also depends on the level and severity of the injury with individuals with tetraplegia more likely to die earlier than individuals with paraplegia, with a complete injury nearly doubling the mortality rate of people with paraplegia, and nearly tripling it for those with tetraplegia. Although secondary conditions of spinal cord injury are no longer the main cause of death of people with SCI in high-income countries, in low-income countries, preventable secondary conditions, e.g. urologic complications and pressure sores are still all too commonly a cause of death secondary to absence of adequate medical care. [1]
But overall life expectancy has increased since the 1950s, in particular showing a steady increase in life expectancy for individuals with spinal cord injury in high-income countries, with a 40% decrease in mortality between 1973 and 2004 during the first 2 years post-injury in the United States of America, which reflects improvements in clinical care and rehabilitation medicine for individuals with spinal cord injury. [1]
Summary[edit | edit source]
Incidence and prevalence of Spinal Cord Injury can differ significantly between countries and regions and identifies the need for development of preventative and management strategies that are tailored towards regional trends. There is limited available research that examines the reasons for this variation suggesting the need for further comprehensive and comparative studies, and for international standards and guidelines for reporting on spinal cord injury. Without this reliable information, the priorities for prevention, medical and social care cannot be satisfactorily determined. [2]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 World Health Organization, International Spinal Cord Society. International Perspectives on Spinal Cord Injury. World Health Organization; 2013.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 Singh A, Tetreault L, Kalsi-Ryan S, Nouri A, Fehlings MG. Global Prevalence and Incidence of Traumatic Spinal Cord Injury. Clinical Epidemiology. 2014;6:309.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 Furlan JC, Sakakibara BM, Miller WC, Krassioukov AV. Global Incidence and Prevalence of Traumatic Spinal Cord Injury. Canadian Journal of Neurological Sciences. 2013 Jul;40(4):456-64.
- ↑ Dominic Power. Spinal Cord Injury 1: Epidemiology and Classification of SCI. Available from: https://youtu.be/8lRM-emvn2Y[last accessed 30/10/17]
- ↑ Stack E, Stokes M, editors. Physical Management for Neurological Conditions. Elsevier Churchill Livingstone; 2012.
- ↑ Harvey L. Management of Spinal Cord Injuries: A Guide for Physiotherapists. Elsevier Health Sciences; 2008 Jan 10.
- ↑ Singh A, Tetreault L, Kalsi-Ryan S, Nouri A, Fehlings MG. Global Prevalence and Incidence of Traumatic Spinal Cord Injury. Clin Epidemiol. 2014;6:309-31. Published 2014 Sep 23. doi:10.2147/CLEP.S68889