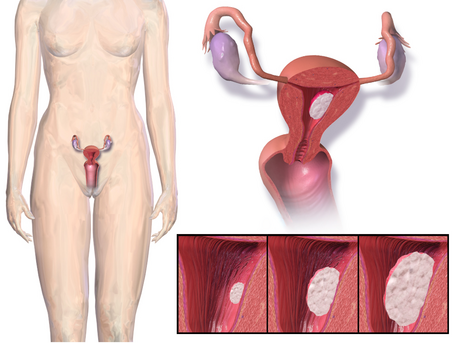
Endometrial Cancer
Definition/Description[edit | edit source]
Endometrial cancer— its a tumour which originates in the endometrium.
Epidemiology[edit | edit source]
Endometrial cancer occurs in up to 29% of women before 40 years of age and at the same time, seventy percent of these patients are nulliparous.[1]Endometrial cancer is the sixth most common cancer in women worldwide.[2] In 2020, approximately 417,367 women suffered from endometrial cancer and 97,370 died from the disease.[2]Moreover, in the United States, endometrial cancer has both increasing incidence (about 1% yearly from 2007 to 2016) and mortality rates (about 2% yearly from 2008 to 2017).[3]
Incidence- Approximately 15,000 women are freshly diagnosed with endometrial cancer in each year, 4% of which are at reproductive age.[4]
It occurs in women predominantly after menopause. The estimated age-standardized incidence rates (ASRs) vary from one to 30 cases per 100 000 women across countries globally, with the highest rates found in countries with a very high Human Development Index, where almost two-thirds of all cases occur. Low rates are observed in several Sub-Saharan African, Middle-Eastern, and South-Central Asian countries[5]
Stages[edit | edit source]
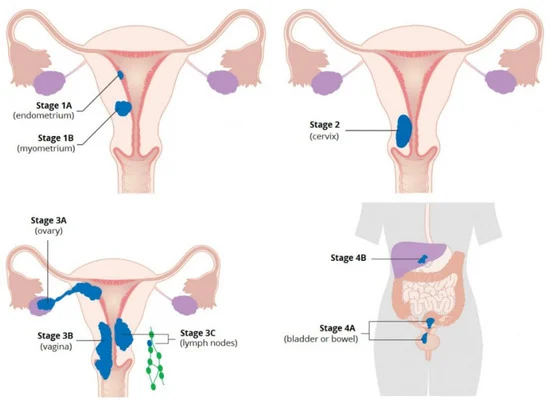
The system used for staging endometrial cancer is the FIGO (International Federation of Gynecology and Obstetrics) system.
| FIGO STAGE | INTERPRETATION |
|---|---|
| I | The tumour is growing inside the uterus and glands around the cervix but not the supporting connective tissue of the cervix. Cancer has not spread to the nearby lymph nodes and distant sites. |
| IA | The tumour is in the endometrium and is halfway to the myometrium. It also has not spread through the nearby lymph nodes and distant sites. |
| IB | The tumour has spread to the myometrium from the endometrium but not beyond the uterus.No signs of spreading into nearby lymph nodes and distant sites. |
| II | Cancer has spread from the body of the uterus to the supportive connective tissue of the cervix but not to the uterus, nearby lymph nodes and distant sites. |
| III | Cancer has escalated outside the uterus but not to the inner lining of the rectum or urinary bladder, lymph nodes or distant sites. |
| IIIA | Cancer has spread to the outer surface of the uterus (called the serosa) and/or to the fallopian tubes or ovaries (the adnexa) but not to lymph nodes or distant sites. |
| IIIB | Cancer has spread to the vagina or to the tissues around the uterus (the parametrium) but not to the lymph nodes or distant sites. |
| IIIC I | Cancer is growing in the body of the uterus. It may have spread to some nearby tissues, but is not growing into the inside of the bladder or rectum and has also spread to pelvic lymph nodes but not to lymph nodes around the aorta or distant sites |
| IIIC II | Cancer is growing in the body of the uterus. It may have spread to some nearby tissues, but is not growing into the inside of the bladder or rectum and has also spread to lymph nodes around the aorta (para-aortic lymph nodes) but not to distant sites. |
| IVA | Cancer has spread to the inner lining of the rectum or urinary bladder.It may or may not have spread to nearby lymph nodes. |
| IVB | Cancer has spread to inguinal (groin) lymph nodes, the upper abdomen, the omentum, or to organs away from the uterus, such as the lungs, liver, or bones. Cancer can be any size and it might or might not have spread to other lymph nodes. |
Risk Factors/Etiology[edit | edit source]
- Accepted risk factors in medical literature for endometrial cancer comprise of obesity, type 2 diabetes, smoking, and physical inactivity.[7][8]
- Insulin resistance has been positively correlated with endometrial cancer risk.[9]
- Lower circulating levels of adiponectin and higher leptin levels have been related to a raised risk for endometrial cancer.[10][11][12]
- Continuous exposure to estrogen. ( hormone replacement therapy)
- Nulliparity.[13]
- Tamoxifen.[14]
Clinical Presentation[15][edit | edit source]
- Abnormal uterine bleeding
- Postmenopausal symptoms
- Abnormal vaginal discharge
- Pyometra (a secondary infection that occurs as a result of hormonal changes in the female's reproductive tract)
- Abdominal pain
- Abdominal distention
Assessment[15][edit | edit source]
- Office-based pipelle sampling- A endometrial biopsy procedure done quickly at visiting doctor's office without any kind of anaesthesia. A speculum is gently inserted into the vaginal opening to get a clear view of the cervix. A solution is then applied around the cervix to clean it. A suction tube is inserted to collect tissue samples while holding the cervix with another instrument. The sample collected is then analyzed at the lab.
- Biopsy
- Dilation and curettage or hysteroscopy
Non-Conservative Management[edit | edit source]
1.The traditional remedy for endometrial cancer is surgery involving
- Total hysterectomy with bilateral salpingo-oophorectomy
- Lymph node assessment[15]
- Pelvic washings
- Pelvic and paraaortic lymphadenectomy[16]
2. Radiotherapy
3. Chemotherapy
Physiotherapy Management[edit | edit source]
Goals and Plans of Management[edit | edit source]
- Counselling of patient( e.g. diet requirements, about the condition etc.)
- To perform a complete urogynaecological assessment for protocol planning( pre, peri and post -operative assessment if possible).
- To increase physical activity.
- To increase strength and endurance.
- To reduce fatigue.
- To reduce lymphoedema after surgery. Physiotherapy management of lymphoedema can be read here.
- To plan a tailored exercise programme suitable for the patient.
- To prevent complications ( for eg. urinary incontinence, weakening of pelvic floor muscles).
- To improve quality of life.
EPEC-FAST Programme[edit | edit source]
EPEC-FAST Exercise programme/ intervention consists of 60 min customized(one-to-one) training sessions with a personal trainer, once a week, for 10 consecutive weeks. It can be given to endometrial cancer survivors[17]It is a recently studied exercise programme but still requires further research.
| Exercise Phase | Descriptors | |
|---|---|---|
| Warm-up | ||
| 10 min | Low intensity warm-up using an exercise bike or a treadmill | |
| Exercise phase | ||
| 40 min | Aerobic exercise (20 min)Walking on a treadmill or cycling on an exercise bike. The exercise phase will be performed at a level of 40–60% of the maximum heart rate. | |
| Pillar strength training (10 min)Consists of 4 exercises to improve stability and strength of the hip, and 3 exercises to improve core stability and strength. Patients are recommended to perform 8 repetitions of each of the hip stability movements per leg, and a set of 10–15 repetitions of each core muscle exercise. A stability ball may be used to facilitate some of the exercises | ||
Hip movements:
|
Core movements:
| |
| Resistance training (10 min)Consists of 1 set of 8 to 12 repetitions of 8 exercises that include all the major muscle groups. After initial phase of repetitions, this can be increased up to 20–25 repetitions (40–60% of 1 RM) during 1 session. A dumbbell, stability ball or bench may be used to facilitate the exercises.
Exercises:
| ||
| Cool down | ||
| 10 min | Set of 6 stretching and flexibility exercises. Four repetitions of each of the following muscle groups will be performed for10–30 s.
| |
Follow Up[edit | edit source]
When endometrial cancers recur, most of them are detected within the first 2 years after treatment. The patient should undergo examination every 3– 4 months for the first 2 years, every 6 months for the next 3 years, and yearly after 5 years.[16]Vaginal cytology should be performed at least on yearly basis.[16]
References[edit | edit source]
- ↑ Tanos P, Dimitriou S, Gullo G, Tanos V. Biomolecular and Genetic Prognostic Factors That Can Facilitate Fertility-Sparing Treatment (FST) Decision Making in Early Stage Endometrial Cancer (ES-EC): A Systematic Review. International Journal of Molecular Sciences. 2022 Feb 28;23(5):2653.
- ↑ 2.0 2.1 Sung H, Ferlay J, Siegel RL, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71:209-249.
- ↑ American Cancer Society. Cancer Facts & Figures 2020. American Cancer Society; 2020.
- ↑ World Health Organization; International Agency for Research on Cancer (IARC); Global Cancer Observatory (GCO).
- ↑ Ferlay J, Soerjomataram I, Ervik M, et al. GLOBOCAN 2012 v1.0, Cancer Incidence and Mortality Worldwide. IARC CancerBase No. 11. Lyon, France: International Agency for Research on Cancer; 2013
- ↑ Kasius JC, Pijnenborg JM, Lindemann K, Forsse D, van Zwol J, Kristensen GB, Krakstad C, Werner HM, Amant F. Risk stratification of endometrial cancer patients: FIGO stage, biomarkers and molecular classification. Cancers. 2021 Nov 22;13(22):5848.
- ↑ Deng T, Lyon CJ, Bergin S, Caligiuri MA, Hsueh WA. Obesity, inflammation, and cancer. Annu Rev Pathol. 2016;11:421-449
- ↑ Avgerinos KI, Spyrou N, Mantzoros CS, Dalamaga M. Obesity and cancer risk: emerging biological mechanisms and perspectives. Metabolism. 2019;92:121-135
- ↑ Hernandez AV, Pasupuleti V, Benites-Zapata VA, Thota P, Deshpande A, Perez-Lopez FR. Insulin resistance and endometrial cancer risk: a systematic review and meta-analysis. Eur J Cancer. 2015;51:2747-2758.
- ↑ Ellis PE, Barron GA, Bermano G. Adipocytokines and their relationship to endometrial cancer risk: a systematic review and meta-analysis. Gynecol Oncol. 2020;158:507-516.
- ↑ Gong TT, Wu QJ, Wang YL, Ma XX. Circulating adiponectin, leptin and adiponectin-leptin ratio and endometrial cancer risk: evidence from a meta-analysis of epidemiologic studies. Int J Cancer. 2015;137:1967-1978.
- ↑ Yoon YS, Kwon AR, Lee YK, Oh SW. Circulating adipokines and risk of obesity related cancers: a systematic review and meta-analysis. Obes Res Clin Pract. 2019;13:329-339.
- ↑ Paleari L, Pesce S, Rutigliani M, Greppi M, Obino V, Gorlero F, Vellone VG, Marcenaro E. New insights into endometrial cancer. Cancers. 2021 Mar 24;13(7):1496.
- ↑ Emons G, Mustea A, Tempfer C. Tamoxifen and endometrial cancer: A janus-headed drug. Cancers. 2020 Sep 7;12(9):2535.
- ↑ 15.0 15.1 15.2 Mitric C, Bernardini MQ. Endometrial Cancer: Transitioning from Histology to Genomics. Current Oncology. 2022 Jan 31;29(2):741-57.
- ↑ 16.0 16.1 16.2 Sorosky JI. Endometrial cancer. Obstetrics & Gynecology. 2008 Feb 1;111(2 Part 1):436-47.
- ↑ Smits A, Lopes A, Das N, Bekkers R, Massuger L, Galaal K. Exercise programme in endometrial cancer; protocol of the feasibility and acceptability survivorship trial (EPEC-FAST). BMJ open. 2015 Dec 1;5(12):e009291
- ↑ Zhang X, Haggerty AF, Brown JC, Giuntoli II R, Lin L, Simpkins F, Dean LT, Ko E, Morgan MA, Schmitz KH. The prescription or proscription of exercise in endometrial cancer care. Gynecologic oncology. 2015 Oct 1;139(1):155-9.