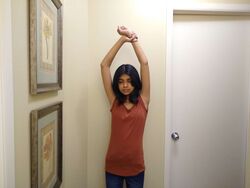Diaphragm Rehabilitation
Top Contributors - Carin Hunter, Jess Bell, Kim Jackson and Ewa Jaraczewska
Introduction[edit | edit source]
Rehabilitation is a vital part of recovery; it is integral to the treatment plan for physiotherapists. However, this muscle is often overlooked in the rehabilitation plan of patients who sustain an injury which causes damage to the diaphragm[1] [2], or who have been on a ventilator. The diaphragm, the main respiratory muscle, works constantly throughout the day and performs many different breaths and breath holds. Retraining the diaphragm is, therefore, crucial for optimal function.
Causes of Diaphragm Dysfunction[edit | edit source]
Some causes of diaphragm dysfunction are discussed below:
Surgical Diagnoses[edit | edit source]
- Congenital Diaphragmatic Hernia: One or more of a person's abdominal organs (i.e. stomach, spleen, liver, intestines) move upwards into the chest through a defect in the diaphragm. Congenital hernias are considered a medical emergency and require prompt surgery.[3]
- Acquired Diaphragmatic Hernia (ADH): Usually caused by a penetrating injury (e.g. gunshot wound, stabbing) or a blunt injury (e.g. fall, motor vehicle accident). Penetrating injuries are a far more common cause of diaphragmatic rupture and subsequent hernias than blunt injuries.[4]
Diaphragm Atrophy Secondary to Mechanical Ventilation[edit | edit source]
- After an individual has been on mechanical ventilation for an extended time, they may experience disuse atrophy. This is caused by decreased protein synthesis,[5] increased proteolysis[6] or combination of both factors after mechanical ventilation.
- Oxidative stress is "defined as a disturbance in the balance between the production of reactive oxygen species (free radicals) and antioxidant defences".[7] Oxidative stress starts to occur within six hours of continuous mechanical ventilation, and it is linked to diaphragmatic dysfunction and weakness.[8] This phenomenon also occurs in skeletal muscles but takes longer to set in.[9]
- A 2017 study by Grosu and Lee[10] concluded no relationship exists between changes in diaphragm thickness and extubation outcome.[10] However, Goligher et al.[11] concluded that diaphragmatic atrophy that developed while a patient was on mechanical ventilation had a strong influence over the clinical outcome: "Targeting an inspiratory effort level similar to that of healthy subjects at rest might accelerate an individual's liberation from ventilation."[11]
- There are several studies to highlight the benefits of early rehabilitation in ICU. Early rehabilitation can lessen the dysfunction caused by mechanical ventilation and assist a patient's extubation.[12]
- The Manual Evaluation Diaphragm[13] (MED) Scale is the only evaluation scale in the world to generate a value for the mobility of the diaphragm.
- The MED Scale has been designed to use a therapist's palpation skills during an evaluation. This means it is the first non-instrumental evaluation tool for assessing the diaphragm function.
- Please read the following article for more information on The Diaphragm Muscle Manual Evaluation Scale.[14]
Diaphragm Weakness Secondary to Traumatic Event[edit | edit source]
- Paradoxical breathing occurs when the diaphragm moves in the opposite direction than it is supposed to:
- The abdomen draws in during inhalation and draws out on exhalation. [15]
- It leads to shortness of breath, fatigue, and tachypnea (fast breathing)
- The causes of paradoxical breathing include obstructive sleep apnea, trauma or injury to the chest wall, nerve damage (examples: Guillaine-Barre Syndrome, muscular dystrophy, multiple sclerosis), or weak respiratory muscles as a consequence of neurological conditions (amyotrophic lateral sclerosis).
This video demonstrates the sequence of paradoxical breathing:
Techniques to Strengthen the Diaphragm[edit | edit source]
- Sandbag breathing
- Deep chest breathing
- Bellow’s breath
- Intercostal stretching breath
- Focused diaphragmatic breath
- Diaphragm stretches
- Transversus abdominis activation
- Straw breathing
- Cat-cow pose[16]
1. Sandbag Breathing[edit | edit source]
The patient lies in a supine position (Figure 1). Their spine should be straight (i.e. not bent to either side). A sandbag is placed on the patient's belly.
Help the patient to establish a flow of relaxed breathing with the following three steps:[16]
- Feel the breath flowing out and in repeatedly
- Soften the abdomen and feel it rise on inhalation and fall on exhalation
- Let the breath flow, and do not pause between breaths
2. Deep Chest Breathing[edit | edit source]
The patient should sit on the floor and place two yoga blocks on the floor behind them. One block should be lying flat, and the other should be at medium height. The patient must then lay their shoulder blades on the flat block and their head on the medium height block, as shown in Figure 2. They should be instructed to relax their arms out to each side with their palms facing up and legs stretched out in front. In this position, they should inhale deeply and allow their chest to rise fully.[16]
On exhalation, the patient should allow their stomach to lower first, followed by the diaphragm, then the lungs and lastly the chest. This exercise should be repeated nine times with a regular breath between each repetition.[16]
Deep chest breathing will help to improve tone in the diaphragm and the intercostal muscles.[16]
3. Bellow’s Breath[edit | edit source]
Bellow’s breath is considered a detoxifying breathing exercise. To perform this exercise, the client needs to be in a seated position. Once comfortable, the client should inhale through their nose. On exhalation, they should snap their stomach muscles in, forcing the exhalation. This breathing pattern should be performed for 30 seconds, gradually increasing the pace.[16]
4. Intercostal Stretching Breath[edit | edit source]
To perform an intercostal stretching breath, the patient begins in standing. Ask them to stretch both arms over their head. Inhale deeply, and on the exhale, they should stretch both arms to the right. This stretches the intercostal muscles on the left side of the body. As they inhale, they should come back to the centre.[16]
On the next exhale, they should stretch their arms to the left, creating a stretch in the right intercostal muscles. Repeat two more times on each side.[16]
5. Focused Diaphragmatic Breath[edit | edit source]
When performing a focused diaphragmatic breath, the patient must first understand exactly where their diaphragm is. Take their fingers and place them on the bottom of their sternum. Instruct them to take a few breaths and feel their diaphragm move under their fingers.[16]
To perform this breathing exercise, the patient must tense their stomach muscles and keep their fingers on the diaphragm. Inhale and exhale several times, focusing on the diaphragm’s movement. This exercise can help increase awareness of and tone the diaphragm.[16]
6. Diaphragm Stretches [edit | edit source]
To perform a diaphragm stretch,[17] the patient should begin in supine, in 90/90 hip-knee flexion. Place the heels of the patient's hands on their proximal thighs (near hip creases). They should perform a few relaxed breaths through their nose.[18]
After a deep inhalation and full exhalation, the client should push their hands into their thighs. At this point, they should think about inhaling without breathing any air. Then ask them to suck their belly in and expand their ribs, which creates a vacuum. The client should then move their spine/pelvis slightly through flexion and extension. Introducing lateral shifts will also increase the stretch in different diaphragm parts. Breathe normally during one or two cycles and repeat five times.[18]
7. Transversus Abdominis Activation[edit | edit source]
When performing transversus abdominis activation,[17] the patient should lie on their back with their knees bent (crook lying). They should position their feet hip-width apart and put a block lengthwise between their thighs. Make sure their pelvis and lower back are in neutral. Ask them to place their fingertips on their lower abdomen (i.e. just between their anterior superior iliac spines).[18]
On exhalation, instruct the patient to drop their belly button, engage their pelvic floor, and squeeze the block between their thighs. During this movement, they should feel the transversus abdominis tensing under their fingertips. It is key that the patient maintains a neutral spine as their belly drops. On inhalation, the belly should relax and soften. This movement should be completed a few times so the patient can learn to recognise the deep activation of their core.[18]
As a progression, the above exercise can be repeated, but instruct the patient to lift both feet an inch off the ground at the end of exhalation. This position is held during inhalation before they place their feet back on the ground.[18]
8. Straw Breathing[edit | edit source]
Instruct your client to hold a straw between their lips for this exercise. They should inhale through their nose and exhale through the straw. By breathing out through a long straw, the exhalation will become longer than the inhalation.[18]
9. Cat-Cow Pose[edit | edit source]
Start this exercise in 4-point-kneeling. Instruct the patient to breathe in through their nose and out through their mouth. When the patient breathes in, instruct them to drop their stomach down towards the floor and hollow/drop their back.[16][19]
Instruct them to round their back and tuck their chin toward their chest when they breathe out. They should hold this position as they exhale. The patient should be encouraged to pause for five seconds at the end of the exhalation, still holding the rounded position. After this, they can inhale through the nose again.[16][19]
8. Diaphragm Stretches in Standing[edit | edit source]
This stretch mostly targets the fibres located between the 12th rib and the central tendon along the inside of the rib cage, which is called the Zone of Apposition.
Instruct the client to stand in a comfortable position. To stretch the left side of the diaphragm, the client should lift the left arm over their head and place the right hand on the left lower ribs.[20]
On exhalation, the client should move into the right lateral spine flexion. This causes the diaphragm to lengthen because of the exhalation and increased distance between the top of the diaphragm and the 12th rib.[20]
The patient should then inhale while returning to the original position. This movement should be repeated five times.[20]
The figures below illustrate the diaphragm stretch in standing.[16]
To progress the exercise, follow these steps:[20]
- Step 1: To increase the stretch, ask the patient to gently push down on left ribs 7-12 with their right hand. This movement is then repeated on the right side (five times on each side). Each time the client moves to the side, they should exhale. On returning to an upright position, they should inhale.[20]
- Step 2: To finish this stretch, the patient should reach up with both arms and clasp their hands together. The patient should laterally flex to the right and then the left. Exhale on lateral flexion and inhale when returning to upright. The client should move to each side four times.[20]
Additional Breathing Techniques[edit | edit source]
Pranayama Breathing Techniques[edit | edit source]
Ujjayi Breathing[edit | edit source]
Bellows Breathing[edit | edit source]
Diaphragm Release[edit | edit source]
Myofascial Release for the Diaphragm[edit | edit source]
References[edit | edit source]
- ↑ Yajima W, Yoshida T, Kondo T, Uzura M. Respiratory failure due to diaphragm paralysis after brachial plexus injury diagnosed by point-of-care ultrasound. BMJ Case Rep. 2022 Feb 28;15(2):e246923.
- ↑ Tavakoli H, Rezaei J, Miratashi Yazdi SA, Abbasi M. Traumatic right hemi-diaphragmatic injury: delayed diagnosis. Surg Case Rep. 2019 Jun 6;5(1):92.
- ↑ Petrosyan M, Shah AA, Chahine AA, Guzzetta PC, Sandler AD, Kane TD. Congenital paraesophageal hernia: Contemporary results and outcomes of the laparoscopic approach to repair in symptomatic infants and children. Journal of pediatric surgery. 2019 Jul 1;54(7):1346-50.
- ↑ Newbury A, Dorfman JD, Lo HS. Imaging and management of thoracic trauma. InSeminars in Ultrasound, CT and MRI 2018 Aug 1 (Vol. 39, No. 4, pp. 347-354). WB Saunders.
- ↑ Ku Z, Yang JI, Menon VA, Thomason DB. Decreased polysomal HSP-70 may slow polypeptide elongation during skeletal muscle atrophy. American Journal of Physiology-Cell Physiology. 1995 Jun 1;268(6):C1369-74.
- ↑ Bodine SC, Latres E, Baumhueter S, Lai VK, Nunez L, Clarke BA, Poueymirou WT, Panaro FJ, Na E, Dharmarajan K, Pan ZQ. Identification of ubiquitin ligases required for skeletal muscle atrophy. Science. 2001 Nov 23;294(5547):1704-8.
- ↑ Betteridge DJ. What is oxidative stress?. Metabolism. 2000 Feb 1;49(2):3-8.
- ↑ Zergeroglu MA, McKenzie MJ, Shanely RA, Van Gammeren D, DeRuisseau KC, Powers SK. Mechanical ventilation-induced oxidative stress in the diaphragm. Journal of Applied Physiology. 2003 Sep;95(3):1116-24.
- ↑ Kondo HI, Miura MI, Nakagaki IK, Sasaki SA, Itokawa YO. Trace element movement and oxidative stress in skeletal muscle atrophied by immobilization. American Journal of Physiology-Endocrinology And Metabolism. 1992 May 1;262(5):E583-90.
- ↑ 10.0 10.1 Grosu HB, Ost DE, Im Lee Y, Song J, Li L, Eden E, Rose K. Diaphragm muscle thinning in subjects receiving mechanical ventilation and its effect on extubation. Respiratory care. 2017 Jul 1;62(7):904-11.
- ↑ 11.0 11.1 Goligher EC, Dres M, Fan E, Rubenfeld GD, Scales DC, Herridge MS, Vorona S, Sklar MC, Rittayamai N, Lanys A, Murray A. Mechanical ventilation–induced diaphragm atrophy strongly impacts clinical outcomes. American journal of respiratory and critical care medicine. 2018 Jan 15;197(2):204-13.
- ↑ Dong Z, Liu Y, Gai Y, Meng P, Lin H, Zhao Y, Xing J. Early rehabilitation relieves diaphragm dysfunction induced by prolonged mechanical ventilation: a randomised control study. BMC Pulmonary Medicine. 2021 Dec;21(1):1-8.
- ↑ Bordoni B, Morabito B. The Diaphragm Muscle Manual Evaluation Scale. Cureus. 2019 Apr;11(4).
- ↑ Bordoni B, Morabito B. The Diaphragm Muscle Manual Evaluation Scale. Cureus. 2019;11(4):e4569.
- ↑ Chapman EB, Hansen-Honeycutt J, Nasypany A, Baker RT, May J. A CLINICAL GUIDE TO THE ASSESSMENT AND TREATMENT OF BREATHING PATTERN DISORDERS IN THE PHYSICALLY ACTIVE: PART 1. Int J Sports Phys Ther. 2016 Oct;11(5):803-809.
- ↑ 16.00 16.01 16.02 16.03 16.04 16.05 16.06 16.07 16.08 16.09 16.10 16.11 16.12 Pandya R. Rehabilitating the Diaphragm Course. Plus , 2022
- ↑ 17.0 17.1 Rathore M, Trivedi S, Abraham J, Sinha MB. Anatomical correlation of core muscle activation in different yogic postures. International Journal of Yoga. 2017 May;10(2):59.
- ↑ 18.0 18.1 18.2 18.3 18.4 18.5 Bech-Hanssen G, ed. Why Your Diaphragm Could Be the Core Strength Game-Changer You’ve Overlooked. yoga journal; Sep 28, 2018 ORIGINAL: Nov 7, 2017.
- ↑ 19.0 19.1 Yoga by Candace. Cat/Cow Variation. Available from: https://www.yogabycandace.com/blog/cat-cow-variation-back-pain (accessed 13/02/2022).
- ↑ 20.0 20.1 20.2 20.3 20.4 20.5 Franklin E. Breathing for peak performance. Human Kinetics. Available from: https://us.humankinetics.com/blogs/excerpt/strengthening-and-stretching-routine-for-the-diaphragm (accessed 13/02/2022).