Charcot-Marie-Tooth Disease Case Study
Abstract[edit | edit source]
Charcot Marie Tooth disease is a common progressive form of peripheral neuropathy affecting motor and sensory systems. This fictional case study presents a 23-year-old male diagnosed with Charcot Marie Tooth disease (CMT1A). The subjective and objective findings are stated at initial assessment and at 3 month follow up to monitor his progress with physiotherapy. Physiotherapy interventions are aimed at improving aspects of the patient's body structure/function, activity, and participation following the ICF model. Goals are patient-centered, and treatment aims to improve ROM, strength, balance, endurance and pain management. An interdisciplinary team approach is taken to manage various aspects of this case, including referral for podiatrist, pharmacological interventions, and OT. The patient is motivated to slow the progression of the disease and based on the outcome measure scores it is evident that the patient is able to maintain, if not improve, their functional status and quality of life with physical therapy intervention.
Introduction[edit | edit source]
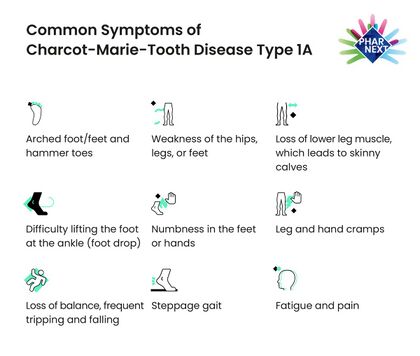
This case will examine a 23-year-old male diagnosed with CMT1A. This genetically inherited neuromuscular disorder affects over 2.6 million people worldwide and is the most common form of peripheral neuropathy [2]. Genetic mutations can be autosomal dominant, autosomal recessive or X-linked. There are 6 subtypes of CMT (CMT1A, CMT1B, CMT2, CMT3, CMT4, CMTX1) differentiated by either demyelination or progressive axonal degeneration. Between different subtypes common symptoms may include altered sensation, impaired motor function and atrophy beginning in the distal lower extremity (feet, ankles) prior to the upper extremity due to long nerves affected first and reduced deep tendon reflexes. Due to this presentation, patients with CMT often have altered gait and foot deformities (pes cavus).Concomitant diabetes or acute/chronic inflammatory demyelinating polyradiculoneuropathy leads to a more severe disease progression [3].
The purpose of this case study is to inform readers about the presentation of CMT in a previously active and young person with mild severity and how physiotherapy can assist in moderating quality of life and functional activities in this progressive disease. The case will act as an easily accessible, free, online resource for healthcare professionals and families to reference. Severity and presentation of this disease will differ among individuals and even between family members, ranging from no/mild symptoms to severe impairments requiring a wheelchair or respiratory failure requiring assisted ventilation [3][4]. This case study will allow physical therapists to differentiate the needs of a patient’s specific progression and the appropriate interventions and goals to maintain or improve quality of life.
Client Characteristics[edit | edit source]
The patient is a 23-year-old male, who is a recent Teacher’s College graduate now working as a high school teacher in a medium-sized city in Ontario. His hobbies include playing and coaching badminton and riding his bike with his partner on the weekends. The patient was referred to physiotherapy after a diagnosis from a neurologist with Type 1a of CMT and has been receiving physiotherapy treatment for 4 months. His main complaints are limitations on standing tolerance at work and on sports participation. He has noticed changes in his balance and sensation in his feet.
Examination Findings[edit | edit source]
Subjective[edit | edit source]
History of Present Illness
A 23-year-old male was diagnosed by neurologist 4 months ago with demyelinating Charcot Marie Tooth Disease (CMT1A) based upon family history, nerve conduction testing, and exclusion of other neurological conditions such as diabetic neuropathy. After initially presenting to their family physician they were referred to a neurologist for the following signs and symptoms over the previous year: persistent pins and needles in the feet bilaterally, balance disturbances, pain in the lower extremities and muscle cramping. They fractured their wrist due to a fall 1 year ago and received physiotherapy treatment for a sprained ankle 1.5 years ago, but are otherwise healthy. They are not currently on any medications and have been referred to physiotherapy for treatment.
Functional Status
The patient lives alone in a 1-bedroom apartment with an elevator, is independent in all activities of daily living, and does not use a mobility device for ambulation. They present to physiotherapy describing difficulties ambulating over snow and uneven terrain, difficulties running, jumping or cutting, and chronic ankle sprains. Although previously active, their daily activity levels have decreased significantly over the past 6 months. They currently walk approximately 1 km once a week, but are unable to fully participate in recreational sporting activities. They would like to be able to actively play badminton along with their students rather than just observe.
Objective[edit | edit source]
Observation
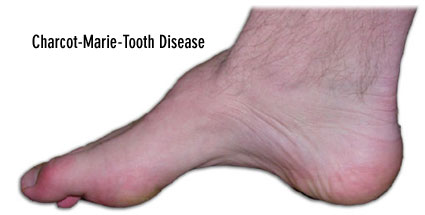
Spinal alignment appears normal. Atrophy and hypotonia is noted bilaterally in the plantar flexors and tibialis anterior. No atrophy is apparent in the upper extremity. The feet exhibit pes cavus and a mild hammer toe is noted bilaterally. Skin appears normal and intact.
Neurological Assessment
Superficial Sensations
Light touch
- Decreased sensation is noted below the midpoint between the ankle and knee joint
- No sensation in the distal feet and toes
Pinprick
- Absent at the first metatarsal joint and medial and lateral malleolus
- Diminished at the midpoint between the ankle and knee joints on the anterior and posterior surfaces bilaterally
- Normal in the upper leg tested 5 cm proximal to the medial and lateral femoral condyles
Deep Sensations
Proprioception
- Decreased position sense bilaterally at the ankle and 1st MTP joint
Vibration perception (tested with a 128 Hz tuning fork)
- Absent sensation at the first metatarsal joint bilaterally
- Impaired sensation at the medial malleolus bilaterally
Upper Motor Neuron Reflexes
Negative Babinski and Hoffman
Vitals
Pedal and radial pulses are strong and regular
| Deep Tendon Reflexes (DTR) | ||
| Right | Left | |
| Biceps | 2 (normal) | 2 (normal) |
| Triceps | 2 (normal) | 2 (normal) |
| Patellar | 2 (normal) | 2 (normal) |
| Achilles | 1 (diminished) | 1 (diminished) |
Range of Motion
Active range of motion (AROM): hip extension 5 degrees bilaterally and 10 degrees ankle dorsiflexion bilaterally. All other AROM is within normal limits.
Passive range of motion (PROM) of the upper and lower extremities are within normal limits. End-feels are normal.
| Manual Muscle Testing (MMT) | ||
| Right | Left | |
| Dorsiflexion | 4 | 4 |
| Plantar flexion | 4 | 4 |
| Inversion | 4 | 4 |
| Eversion | 4- | 4- |
| Knee extension | 4 | 4 |
| Knee flexion | 4 | 4 |
| Hip flexion | 5 | 5 |
| Hip extension | 4+ | 4+ |
| Shoulder flexion | 5 | 5 |
| Shoulder extension | 5 | 5 |
| Elbow flexion | 5 | 5 |
| Elbow extension | 5 | 5 |
| Wrist flexion | 4+ | 4+ |
| Wrist extension | 4+ | 4+ |
For more information on the pathophysiology and observation of symptoms of Charcot-Marie-Tooth, presented in a metaphorical manner, this video may be helpful:
Observational Gait Analysis
The use of technology when analyzing gait can ensure accuracy and improve our observations as physiotherapists[7]. When analyzing gait, an economical and transferable solution of wearing an ankle monitor was implemented into the assessment[8].
- Decreased stride length and cadence.
- Mild foot drop with increased contact in early stance, reduced plantar flexion at toe-off and increased hip and knee flexion in mid swing phase.
Outcome Measures
Charcot Marie Tooth Disease Neuropathy Score[9]: score of 9 indicating mild disease severity.
10 minute walk test: max speed performed in 9 seconds, with a rate of 1.1m/s indicating community ambulation.
Hand dynamometer[10]: performed bilaterally 3 times with an average score of 38 kg for the right hand and 34 kg for the left.
Community Balance and Mobility Scale[11]: score of 72 indicating ability to function with mild impairment within the community and with more complex functional tasks.
Fatigue Severity Scale[12]: score of 23 indicating mild fatigue with functional activities.
Neuropathic Pain Symptom Inventory[13]: score of 24 indicating some neuropathic pain within the lower extremity.
Charcot-Marie Tooth Health Index[14]: self-reported score of 30, indicating disease has some effect on quality of life but not debilitating.
Clinical Impression[edit | edit source]
Analysis[edit | edit source]
A 23-year-old male reported to their family physician experiencing lower extremity sensory and balance deficits 1 year ago and was diagnosed with Charcot Marie Tooth Disease (CMT1A) by a neurologist 4 months ago. Disease severity is determined to be mild as evaluated by the CMTNS and the patient reported QoL measure is optimistic. Referral to mental health supports is not indicated at this time. Impairments predominantly affect the lower legs bilaterally. DTR are reduced at the Achilles, but otherwise normal. Sensory deficits are evident in the distal leg which increase the risk of foot sores. Strength deficits are observed in all directions at the ankle and may increase the risk of falls, ankle injuries, and lower limb contractures. The patient demonstrates a mild foot drop with a minor steppage gate. Walking speed is below age-matched healthy control, but is currently within the limits of safe community ambulation. If disease severity increases above a CMTNS score of 11 the patient may benefit from foot orthoses and should be referred as appropriate. The patient can usually maintain balance on even terrain, but indicates he has challenges over complex, uneven terrain and in dynamic environments. There is no current need for a gait aid, however this may be considered with disease progression. Minimal impairments in the upper extremity are observed, however grip and wrist strength measures were below average values. Referral to an occupational and/or hand therapist may be considered depending on changes in future disease status. The patient lives alone, but has adequate social supports. They report no major limitations in occupational duties and are independent in all ADLs, however they are unable to safely run, jump or participate in sport. The patient is suitable for PT treatment in maintaining and improving strength and balance, preventing LE contractures and sores, reducing risk of falls, monitoring disease progression and maintaining functional independence.
Prognosis[edit | edit source]
They have a relatively good prognosis as they are young, there are no impairments affecting the upper limbs, they were previously active, and are otherwise healthy. Disease is progressive, but slow therefore the patient should be continually monitored and reassessed at regular intervals particularly over the next 10 years.
Problem List[edit | edit source]
- Sensory deficits in distal lower extremities and risk of foot sore
- Increased falls risk due to strength deficits in ankle (all directions), proprioceptive deficits and drop foot
- Reduced hip extension and ankle dorsiflexion AROM
- Balance deficits over uneven terrain
- Decreased walking speed for age
- Neuropathic pain in lower extremities, somewhat affecting functional activities
- Mild fatigue with completing ADL’s
- Limitations in sport participation
Intervention[edit | edit source]
Patient-centered Treatment Goals[edit | edit source]
Short-term goal (STG) 1 (body structure/function): Within 4 weeks, increase ankle dorsiflexion AROM by 5° bilaterally. Ankle DF is currently 10° bilaterally, which is less than the expected value of 20°.
-Reasoning: Increasing ankle DF and preventing the progression of contractures will allow for more normal gait mechanics.
Long-term goal (LTG) 1 (body structure/function): Within 3 months, increase knee (flexion, extension) and hip (flexion, extension) MMTs to 5/5 bilaterally, maintain ankle dorsiflexion, plantarflexion, and inversion MMTs at 4/5 and ankle eversion at 4-/5 bilaterally.
-Reasoning: Supported by literature, as 12-weeks of moderate resistance exercise has been found to increase MMT values in CMT patients [15]. However, based on the patient’s foot deformities and the progressive nature of the disease, maintenance of current ankle strength is more realistic than MMT improvement.
STG2 (activity): Within 4 weeks, hold single leg stance on a wobble board for 30-seconds bilaterally.
-Reasoning: Increasing his proprioceptive abilities is crucial to reducing ankle rolling. A wobble board will provide greater challenge by decreasing stability and increasing mobility and will prepare him for uneven surfaces encountered in daily life.
LTG2 (activity): Within 3 months, increase score on “Running with Controlled Stop” Item on Community Balance Mobility Scale from 1/5 (runs, time >5.00 sec) to 3/5 (runs, time >3.00 but ≤5.00 sec., with controlled stop, both feet on line).
-Reasoning: Improving the patient’s ability to run at an increased speed and incorporating controlled stops in his balance training program will allow the patient to return to playing badminton safely.
STG3 (participation): Within 2 weeks, assist the supply coach with 1-hour of badminton practice after school, with a maximum of two 5-min sitting breaks.
-Reasoning: Patients with CMT tend to fatigue easily and as this patient has greatly reduced his activity, setting gradual goals that utilize Cognitive Behavioural Therapy pacing techniques is important.
LTG3 (participation): Within 3 months, be able to stand and independently coach 1-hour of badminton practice after school without sitting to rest.
-Reasoning: 3 months will allow him to gradually increase his responsibilities at work until he can independently coach practice. An ankle foot orthosis device will not be used at this time because his CMTNS is below 11, but this is a potential option if his abilities decrease.
Management Program[edit | edit source]
Increasing Strength and Balance: Increasing ankle strength in those with CMT disease type 1A is crucial, as muscle imbalance has been shown to occur prior to foot deformity [16]. It is also important for this individual who is involved with sports that involve quick steppage reactions because CMT patients have been shown to have weaker foot evertors when compared to invertors, leading to a higher risk of inversion ankle sprains [17]. The patient will be taught banded dorsiflexion, plantar flexion, inversion, eversion exercises (using a theraband; 3 sets of 10) and heel raises (3 sets of 10). The heel raises will be taught on two feet on a flat surface and progressed to single leg heel raises on an elevated surface. Increasing hip strength will be done using glute bridges and quadruped kickbacks (3 sets of 10).
Walking, Running, and Endurance: Lessening the functional impact of his drop foot will be done via gait training, utilizing neuromuscular electrical stimulation to stimulate the tibialis anterior muscle. No ramp time will be used to facilitate normal gait mechanics. Once the patient demonstrates improvement with walking, moderate-intensity resistance exercise and low-impact aerobic exercise will be encouraged to maintain muscle strength and improve cardiorespiratory fitness [18]. Since this patient enjoys going for bike rides on the weekends, this could involve bike riding, and cycle ergometer protocols below maximum fatigue threshold 3 days per week for 12 weeks have been shown to be effective for those will neuromuscular disease [4]. Encouraging the patient to go for 3 bike rides a week with his partner will make this more meaningful and realistic. Running in the clinic will only begin once the patient demonstrates increased fatigue tolerance.
Education and Pain Management: Continuing education will be provided to the patient on progression of the disease and the importance of continuing in his activities as best as he can. Standing and walking provide a passive stretch to the foot intrinsics, which can help prevent the development or progression of contractures [19]. As a teacher, this patient is on his feet for many hours of the day, which will keep the feet in a stretched position. In addition, studies have shown that lower health-related quality of life in these individuals correlates with limb weakness and pain [20]. This suggests that helping this individual return to badminton, an activity he enjoys, through increasing lower extremity strength and implementing pain-management strategies may increase his quality of life. Muscle cramping is a common complaint in this population, so a proper 5-min warm-up on the stationary bike prior to completing his exercises will be used. At the end of his session, he will also perform a 5-min walk to cool down and complete 10-min of stretching major muscle groups. On days where he is experiencing more pain, low-f TENS will be used at the beginning of treatment to allow for completion of his program (Pulse frequency: 2pps, Pulse duration: 200us, Amplitude: to visible contraction, 20-30min). Sensation testing will be completed in advance of the use of TENS and if it is used over areas with diminished sensation he will be monitored very closely throughout the duration of its use.[21] Due to sensation concerns, the patient will be taught how to monitor for foot sores and the feet will be checked regularly in-clinic. Consulting with the rest of the healthcare team will also be necessary to ensure other factors such as hydration needs are being met.
Outcome[edit | edit source]
With our patient being highly motivated to slow the progression of CMT and the impact it will have on his life, he has been committed to meeting his short- and long-term goals. He has followed his interventions as prescribed by the physio team and has shown improvement or a good level of maintenance after 3 months. His range of motion in ankle dorsiflexion increased by 3 degrees up 13 degrees, just under his short-term goal of 15 degrees. In addition, his MMTs have increased for his stabilizing joints in the lower extremity, mainly his hips and knees. These were 5/5 bilaterally which will also help promote symmetry with any gait issues. The strength training for his feet have been more difficult to improve upon as the natural progression of the disease effects more distal limbs initially. His MMTs for DF and PF have unfortunately stayed the same but his inversion and eversion have both improved; 4+/5 and 4/5 respectively. The hand dynamometer values did not show any significant change in either direction. At the 3-month time point, all outcome measures were retested as well. There was a slight increase of the 10MWT up to 1.16 m/s most likely due to the strength and aerobic training. The CBMS score increased by 6 points up to 78/96 which is not a minimally detectable change[11]. This increase is indicated by the running with controlled stop training he has been working on. He has been able to improve his CMTHI score, decreasing it to 18/100 based on improvements in strength and balance, however, there are still deficits in his distal upper extremities and issues regarding his personal life. This new diagnosis of CMT for him has been difficult to come to terms with. Finally, there were slight improvement in both the neuropathic pain symptom inventory (20/100) and the fatigue severity scale (19/63) since his initial physio appointment which will help improve his quality of life including being able to assist the badminton coach for longer periods of time.
The patient has shown a good understanding of his home exercises and the importance of training the muscles in the feet for slowing the progression of CMT. He also shown competence in the training parameters suitable for his stage of CMT. He has shown a peaked interest in biking with his partner and has said this had made a positive impact on his functional status. At this time, it is not recommended to discharge him as CMT is a progressive disease which will need continual checkups. The frequency of the physiotherapy visits can decrease however, there should be a follow up at least every 6 months. This will give an opportunity to redo the standardized testing and discuss any progressions that need to be made in the at home exercise programs. In addition, talks about being fitted for a gait aid may need to be implemented early so if he were to ever need one, it would be an easy and expected transition.
Other resources to consider in his treatment progression is to get in touch with an occupational therapist for home adaptations such as a raised toilet seat and handrails in the bathroom. An occupational therapist could also help with the overwhelming amount of changes our patient will encounter ranging from both physical challenges to the social or mental challenges. The patient should also get in contact with his family doctor to discuss any pharmaceutical needs that could be addressed such as pain management or management for other sensory symptoms. As well, his family doctor can investigate a referral to a podiatrist or an orthotist as an early intervention option in the case of feet deformities. These services can assist in the prescription of an AFO if needed further into the progression of his disease. If our patient is looking for a more aggressive intervention, we could guide them toward gene therapy as a potential option[22]. This is, however, a more expensive route with only very new research supporting the use so we should be mindful when suggesting this. Advancements in modern technology will make this a more viable option in the future for the implementation of therapies such as gene silencing and gene replacements. Like many neurological diseases, the most beneficial outcomes will be met if our patient is able to reach a wide variety of healthcare providers. Working as a multidisciplinary team will provide access to essential collaboration and ultimately optimize the patient’s quality of life.
As our patient is also a young and mentally competent male, he will be able to benefit from a rehab program centered around technology that he can use at home. This can benefit the patient in a variety of ways including cutting down time in the clinic, distance needed to travel to the clinic, and cost for both patient and provider alike. In the 21st century, many aspects of life are now revolving around technology and physiotherapy is no exception. For patients who suffer from neurological conditions, including our patient with CMT, therapies such as virtual reality games can help with motor performance [23]. Using virtual reality can help by providing real time feedback to the patient and letting the patient choose games that are meaningful to them. For our patient, encouragement for playing interactive games at home such as virtual badminton and biking will ensure higher levels of excitement and willingness to participate in this kind of therapy.
The overall impact of physiotherapy for this patient is to optimize their quality of life. The physiotherapy team will continue to emphasize the importance of doing activities that are meaningful to them and will promote the use of his lower extremities.
Discussion[edit | edit source]
A 23-year-old male with a recent diagnosis of CMT1a was referred to physiotherapy for treatment and condition management strategies. His presenting complaints were inability to stand for long periods of time, increased difficulties in balance and inability to participate in sports/coaching due to issues with fatigue and coordination. Initial examination revealed normal sensation in the upper body, but decreased sensation between the ankle and knee joint as well as below the ankle joint. Vibration sense was absent at the first metatarsal joint and impaired at the medial malleolus bilaterally while position sense was decreased bilaterally at the ankle and first MTP joint. Upper motor neuron assessment was normal. All reflexes were normal except for the Achilles reflex which was diminished. AROM and PROM were all within normal limits except for a minor decrease in hip extension and ankle dorsiflexion. When testing MMT’s it was evident that the upper limbs and proximal leg muscles did not display any deficits, however the patient was weak in ankle dorsiflexion, plantarflexion, inversion, and eversion. These weaknesses may be the cause for abnormalities observed in the gait such as decreased stride length and cadence, mild foot drop with increased contact in early stance, reduced plantarflexion at toe off and increased hip and knee flexion in mid swing phase. When looking at objective measures, the patient received a score of 9 on the CMTD scale indicating that they have mild disease severity. In our gait analysis they scored 9 seconds on a 10 m walk test (1.11m/s) which is slower than what is expected as the normative value for ages 20-29 is 1.36-1.34m/s but still indicates community ambulation [25]. The patient scored a 72/96 on the CBMS; the average for the healthy population within his age group is 88.71 meaning that there is definite possibility for him to improve on his ability to be independent in the community[26]. Finally, on the CMTHI he scored 30. In the past 4 months of physiotherapy, short- and long-term goals have been created. His goals included: increasing ROM, strength, functional activities, ambulation, sport participation and education. These goals will be achieved with various treatment strategies such as self-management/home exercises, podiatrist referral, family doctor referral for pharmacological interventions, OT referral for at home adaptations and a genetic counsellor referral. This disease is commonly thought of as one that is diagnosed in childhood and thus symptoms may be overlooked in adulthood. Interventions for this and other progressive diseases should aim to slow the progression and help the patient cope with functional ramifications to maintain quality of life. At a 3 month follow up the patient had increased or maintained all his strength and ROM. He was able to also maintain his CBMS score and showed a decrease on his fatigue scale and his CMTHI score indicating to us that he is maintaining, if not improving, in his functional status and quality of life. This case study aims to demonstrate that prognosis for progressive diseases such as this one, MS or MND can potentially expect improvements in function, not just loss.
Self-Study Questions[edit | edit source]
1. How many types of CMT are there?
a) 4
b) 3
c) 1
d) 6
Answer [d]
2. What is the common onset of symptoms?
a) Hand and glove sensory loss
b) Muscle weakness in the LEs and gait disturbances
c) Clumsiness in the hands
d) Hyperreflexia
Answer [b]
3. A higher score on the CMTHI indicates improved function
a) True
b) False
Answer [False]
Additional Patient Resources[edit | edit source]
References[edit | edit source]
- ↑ Pharnext. Charcot-Marie-Tooth Disease Type 1A [Internet]. Pharnext. 2021 [cited 2022May12]. Available from: https://pharnext.com/en/disease/charcot-marie-tooth
- ↑ Charcot-Marie-Tooth Disease Fact Sheet [internet]. National Institute of Neurological Disorders and Stroke; 2018 June. Available from https://www.ninds.nih.gov/health-information/patient-caregiver-education/fact-sheets/charcot-marie-tooth-disease-fact-sheet
- ↑ 3.0 3.1 Pareyson D, Marchesi C. Diagnosis, natural history, and management of Charcot-Marie-Tooth disease. The Lancet Neurology; 2009 07;8(7):654-67. Available from https://www.proquest.com/scholarly-journals/diagnosis-natural-history-management-charcot/docview/201483326/se-2?accountid=6180
- ↑ 4.0 4.1 Ribiere C, Bernardin M, Sacconi S, Delmont E, Fournier-Mehouas M, Rauscent H, Benchortane M, Staccini P, Lantéri-Minet M, Desnuelle C. Pain assessment in Charcot-Marie-Tooth (CMT) disease. Annals of physical and rehabilitation medicine. 2012 Apr 1;55(3):160-73.
- ↑ Nihill C. CMT Image 1 [Internet]. Physiopedia. 2014 [cited 2022May12]. Available from: https://www.physio-pedia.com/File:CMT_Image_1.jpg
- ↑ Pixorize. Charcot-Marie-Tooth USMLE Mnemonic. Available from: https://www.youtube.com/watch?v=xKYUeZyi5_Q [last accessed 05/13/2022]
- ↑ Coghe G, Pau M, Mamusa E, Pisano C, Corona F, Pilloni G, Porta M, Marrosu G, Vannelli A, Frau J, Lorefice L. Quantifying gait impairment in individuals affected by Charcot-Marie-Tooth disease: The usefulness of gait profile score and gait variable score. Disability and Rehabilitation. 2020 Feb 27;42(5):737-42.
- ↑ Saboor A, Kask T, Kuusik A, Alam MM, Le Moullec Y, Niazi IK, et al. Latest research trends in gait analysis using wearable sensors and Machine Learning: A systematic review. IEEE Access. 2020 Jul 25;8:167830–64.
- ↑ Murphy, S. M., Herrmann, D. N., McDermott, M. P., Scherer, S. S., Shy, M. E., Reilly, M. M., & Pareyson, D. (2011). Reliability of the CMT neuropathy score (second version) in Charcot-Marie-Tooth disease. Journal of the peripheral nervous system : JPNS, 16(3), 191–198. https://doi.org/10.1111/j.1529-8027.2011.00350.x
- ↑ Hand-held Dynamometer/Grip Strength. [Internet]. Rehabilitation Measures Database Shirley Ryan Ability Lab; 2014 February 7. Available from: https://www.sralab.org/rehabilitation-measures/hand-held-dynamometergrip-strength
- ↑ 11.0 11.1 Community Balance and Mobility Scale [Internet]. Rehabilitation Measures Database Shirley Ryan Ability Lab; 2013 February 9. Available from: https://www.sralab.org/rehabilitation-measures/community-balance-and-mobility-scale#brain-injury
- ↑ Fatigue Severity Scale
- ↑ Bouhassira D, Attal N, Fermanian J, Alchaar H, Gautron M, Masquelier E, et al. Development and validation of the Neuropathic Pain Symptom Inventory. Pain (Amsterdam). 2004;108(3):248–57.
- ↑ Johnson NE, Heatwole C, Creigh P, McDermott MP, Dilek N, Hung M, et al. The Charcot-Marie-Tooth Health Index: Evaluation of a Patient-Reported Outcome: CMT Health Index. Annals of neurology. 2018;84(2):225–33.
- ↑ Aitkens. (1993). Moderate resistance exercise program: its effect in slowly progressive neuromuscular disease. Archives of Physical Medicine and Rehabilitation., 74(7). https://doi.org/10.1016/0003-9993(93)90031-5
- ↑ Rose KJ, Burns J, North KN. Factors associated with foot and ankle strength in healthy preschool-age children and age-matched cases of Charcot-Marie-Tooth disease type 1A. Journal of child neurology. 2010 Apr;25(4):463-8.
- ↑ Vinci P, Perelli SL. Footdrop, foot rotation, and plantarflexor failure in Charcot-Marie-Tooth disease. Archives of physical medicine and rehabilitation. 2002 Apr 1;83(4):513-6.
- ↑ Grandis M, Shy ME. Current therapy for Charcot-Marie-Tooth disease. Current treatment options in neurology. 2005 Jan;7(1):23-31.
- ↑ Skalsky AJ, McDonald CM. Prevention and management of limb contractures in neuromuscular diseases. Physical Medicine and Rehabilitation Clinics. 2012 Aug 1;23(3):675-87
- ↑ Calvert M, Pall H, Hoppitt T, Eaton B, Savill E, Sackley C. Health-related quality of life and supportive care in patients with rare long-term neurological conditions. Quality of life research. 2013 Aug;22(6):1231-8.
- ↑ Vance CGT, Dailey DL, Rakel BA, Sluka KA. Using tens for pain control: The State of the evidence [Internet]. Pain management. U.S. National Library of Medicine; 2014 [cited 2022May12]. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4186747/
- ↑ Johnson N, McCorquodale D, Pucillo E. Management of charcot-marie-tooth disease: Improving long-term care with a multidisciplinary approach. Journal of Multidisciplinary Healthcare. 2016 Jan 9;9:7–19.
- ↑ Lewis GN, Rosie JA. Virtual reality games for movement rehabilitation in neurological conditions: How do we meet the needs and expectations of the users? Disability and Rehabilitation. 2012; 34(22):1880–6.
- ↑ Neuro Rehab VR. Virtual Reality in Physical Therapy by Neuro Rehab VR - Clip from the show Information Matrix TV [video file]. July 15, 2019 [cited 2022 May 12]. Available from https://www.youtube.com/watch?v=xGfsAnWu5os&ab_channel=NeuroRehabVR.
- ↑ Physiopedia. 10 metre walk test [Internet]. Physiopedia. [cited 2022May11]. Available from: https://www.physio-pedia.com/10_Metre_Walk_Test
- ↑ Ryan S. Community balance and mobility scale [Internet]. Shirley Ryan AbilityLab. 2013 [cited 2022May11]. Available from: https://www.sralab.org/rehabilitation-measures/community-balance-and-mobility-scale






