Breath Stacking
Original Editor - Khloud Shreif.
Top Contributors - Khloud Shreif, Kim Jackson, Nikhil Benhur Abburi and Admin
Introduction[edit | edit source]
Bad posture, altered breathing patterns, previous history of a respiratory disorder or even surgical intervention are all factors that can affect the oxygen intake, oxygenation of the blood, lung tidal volume and the clearance of secretions because of an ineffective cough. A simple technique, that addresses both oxygen intake and retained secretions, is known Breath stacking (BS),a technique in which a person is encouraged to breathe in slowly at intervals, stacking one breath on top of the other. This technique allows the lungs take in more oxygen than normal inspiration by encouraging the patient to breathe in slowly breathing and stacking one breath on top of other as tolerance allows, followed by a short hold before slow expiration. It is a technique that can be done with our without equipment depending upon the patient's ability and has been shown to improve:
- Blood oxygenation - during chest expansion it allows more surface area for oxygen diffusion in the blood
- Minimise the risk of a chest infection - Increased lung expansion helps to mobilise secretions
- Cough efficacy - Patients who applied BS show improvement in cough[1], swallowing
Indications[edit | edit source]
There are many patient groups this has shown to be an effective technique to improve lung capacity and clear secretions, for example a study by Feitosa et al showed that it a greater effect on increased lung volumes than convention spirometry.[4] Other studies have shown that it can improve alveolar recruitment by improving lung mechanics and gas exchange in patients with a neuromuscular disease[5], and acute lung injury[6]. A study by Rafiq et al also suggested that it can minimise the risk of chest infections in patients with Amyotrophic Lateral Sclerosis (ALS) by improving the efficacy of coughing to clear secretions.[7] Indications for using BS include:
- Restricted chest movement
- Decreased lung capacity due to muscle weakness
- Inability to cough
- Retained secretions
Technique[edit | edit source]
In many cases, this technique can be performed without equipment but for patients who have difficulting breathing on their own equipment can be used to assist and improve the outcome[8]. It is important to note that equipment is for personal use only not to be shared. A typical example of equipment needed:
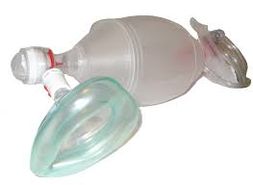
- Modified resuscitator i.e a balloon or Modified Ambu bag
- A face mask or mouthpiece
- Attached by an extension tube (for the modified resuscitator) suitable only for BS
- One way valve
Instructions[edit | edit source]
- Sit upright with shoulders backwards and the back supported. This position can also be adapted to reclining or lying supine, but should not be done with a slouched posture
- Hold the face mask firmly around the mouth (if unable to hold this independently assistance can be given by a caregiver or by placing the mouthpiece in the mouth.
- Take a deep breath in while you or caregiver squeeze the bag - hold the breath in don't breath out
- Take another breath in (on top of the previous ones) and repeat for about two to four times without exhaling
- Hold your breath in for 2-3 second remove the mask then breath out through your mouth. If secretions are present instead of exhalation you can follow this by a cough
- This is one breath stacking cycle
- Repeat for 3-5 cycle of BS twice per day (or more if needed)
If there is caregiver or assistance squeezing the bag you need to coordinate breathing with his/her.[edit | edit source]
Caution[edit | edit source]
Although this a safe non-invasive technique it is important to stop the treatment if the patient presents with any of the following:
- Dizziness
- Chest discomfort
- Chest pain
Cleaning the Equipment[edit | edit source]
It is important to protect the client from risk of infection and therefore, after each use, the equipment needs to cleaned[11]:
- The facemask or mouthpiece can be rinsed in soapy, warm water then allowed to dry naturally.
- A Modified Ambu bag should never be cleaned with water, but instead wiped with detergent, dried and then sent for sterilisation.
Resources[edit | edit source]
References[edit | edit source]
- ↑ Castrillo LD, Lacombe M, Boré A, Vaugier I, Falaize L, Orlikowski D, Prigent H, Lofaso F. Comparison of two cough-augmentation techniques delivered by a home ventilator in subjects with neuromuscular disease. Respiratory care. 2019 Mar 1;64(3):255-61.
- ↑ Armstrong A. Developing a breath-stacking system to achieve lung volume recruitment. British Journal of Nursing. 2009 Oct 22;18(19):1166-9.
- ↑ Dias CM, Vieira Rde O, Oliveira JF, Lopes AJ, Menezes SL, Guimarães FS. Three physiotherapy protocols: effects on pulmonary volumes after cardiac surgery. J Bras Pneumol. 2011 Jan 1;37(1):54-60.
- ↑ de Sá Feitosa LA, Barbosa PA, Pessoa MF, Rodrigues‐Machado MD, de Andrade AD. Clinimetric properties of breath‐stacking technique for assessment of inspiratory capacity. Physiotherapy Research International. 2012 Mar;17(1):48-54.
- ↑ Armstrong A. Developing a breath-stacking system to achieve lung volume recruitment. British Journal of Nursing. 2009 Oct 22;18(19):1166-9.
- ↑ Porto EF, Tavolaro KC, Kumpel C, Oliveira FA, Sousa JF, de Carvalho GV, de Castro AA. Comparative analysis between the alveolar recruitment maneuver and breath stacking technique in patients with acute lung injury. Revista Brasileira de terapia intensiva. 2014 Apr;26(2):163.
- ↑ Rafiq MK, Bradburn M, Proctor AR, Billings CG, Bianchi S, McDermott CJ, Shaw PJ. A preliminary randomized trial of the mechanical insufflator-exsufflator versus breath-stacking technique in patients with amyotrophic lateral sclerosis. Amyotrophic Lateral Sclerosis and Frontotemporal Degeneration. 2015 Nov 27;16(7-8):448-55.
- ↑ Crowe J, Rajczak J, Elms B. Safety and effectiveness of breath stacking in management of persons with acute atelectasis. Physiotherapy Canada. 2006 Oct;58(4):306-14.
- ↑ AmyandpALSvideos. Simple Breath Stacking. Available from: http://www.youtube.com/watch?v=JlgeRoI5vCw[last accessed 12/4/2020]
- ↑ AmyandpALSvideos. Breath Stacking ll, With Resuscitation Bag. Available from: http://www.youtube.com/watch?v=mi-2nPrRHME[last accessed 12/4/2020]
- ↑ World Health Organization. Practical guidelines for infection control in health care facilities. Chapter 4 - Environmental Management Practices. Accessed 26 March 2020