Assessment of Plantar Heel Pain - A Literature Review
Original Editor - Merinda Rodseth based on the course by
Bernice Saban
Top Contributors - Merinda Rodseth, Jess Bell, Kim Jackson, Ewa Jaraczewska and Olajumoke Ogunleye
Introduction[edit | edit source]
The diagnosis of plantar heel pain syndrome (PHPS) is predominantly based on the symptoms of the patient together with manual palpation of the painful heel.[1][2] Validation of this diagnosis through the use of a reliable clinical test is, however, still elusive. This is significant as valid assessment tools are necessary to ensure optimal management. These tools not only ensure health professionals can assess the status of the patient, but they also highlight the efficacy of treatment and guide which treatment methods to use.
This article will provide an analysis of the available literature on the assessment of PHPS.
Assessment Tools for PHPS[edit | edit source]
A variety of tests have been proposed for the assessment and diagnosis of PHPS, but none have been accepted as the “gold standard”.[1] This necessitates an analysis of the available research to identify which of the proposed tests are reliable and valid for assessing PHPS (Figure 1).
Figure 1. Assessment tools for PHPS [3]
Windlass Test[edit | edit source]
The “windlass mechanism” describes the way in which the plantar fascia supports the foot during weight-bearing activities while providing information about the biomechanical stresses placed on the plantar fascia.[4] Hicks[5] originally described the foot and its ligaments as an “arch-like triangular structure” with the plantar fascia forming the base/tie-rod that runs from the calcaneus to the phalanges.[4] In the propulsive phase of gait, the plantar fascia is wound around the head of the first metatarsal during ankle and hallux dorsiflexion. This shortens the distance between the calcaneus and the metatarsals. The shortening of the plantar fascia that results from dorsiflexion of the big toe simulates the “windlass” (tightening rope/cable) mechanism.[4]
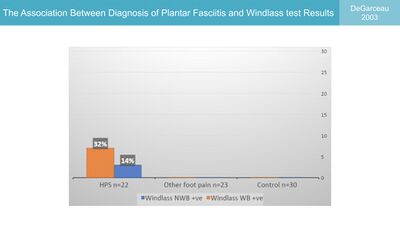
The Windlass Test, therefore, induces strain on the plantar fascia through forced dorsiflexion of the great toe. This strain is associated with increased pain at the site of the insertion of the plantar fascia in patients with plantar fasciitis.[6] However, when De Garceau et al. [6] studied the association between the diagnosis of plantar fasciitis and the results of the windlass test, they found that even though the test is specific for PHPS, it has a low rate of sensitivity which limits its value in clinical evaluation (Figure 2).
Figure 2. The association between the diagnosis of plantar fasciitis and the windlass test results [3][6]
The strain induced with first metatarsal extension was also not limited to the plantar fascia alone, but included various structures in the foot, including the tibial nerve and the medial plantar nerve.[7]
Palpation of the Painful Heel Area[edit | edit source]
Manual palpation of the heel by thumb pressure is a common tool used by clinicians to locate the exact site of pain. It has been proposed that this can aid with both diagnosis and the prescription of treatment in patients with PHPS.[3][8][9][10] No study has, however, quantified the mechanical pressure needed to elicit pain in patients with PHPS and no clinical trials exist to support it as a valid assessment tool for PHPS.[3][8]
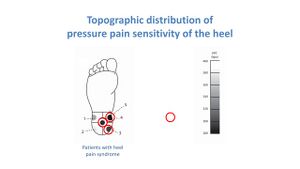
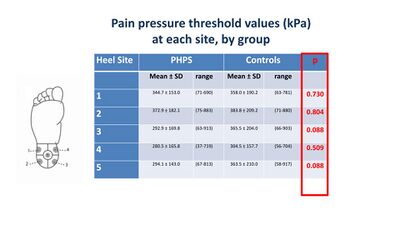
Saban and Masharawi[8] used pain pressure threshold (PPT) to assess the area and extent of pain sensitivity in individuals with and without heel pain (Figure 3). They identified the anterior medial heel as the most sensitive location in the heel, but no significant differences were found between those with and without heel pain (Figure 4). This means the test is not sensitive enough for PHPS and is, therefore, not a diagnostic tool for heel pain. [8]
Imaging[edit | edit source]
Imaging is generally useful for acquiring accurate diagnoses, prompting appropriate treatment and determining prognosis.[2] Various imaging methods, including conventional radiograph, ultrasound and magnetic resonance imaging (MRI), have been used to assess various structures implicated in plantar heel pain (Figure 5).[1][2][3][11][12][13]
Figure 5. Imaging modalities and tissues examined [3]
Imaging of the plantar fascia
Individuals with PHPS were found to be 105 times more likely to present with a thickened plantar fascia measuring more than 4.0 mm compared to those without making it a reliable sign of PHPS.[2][12]
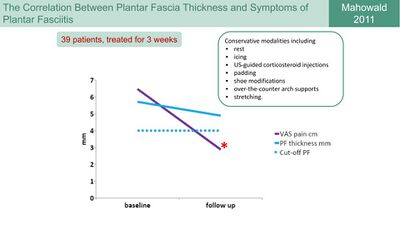
Following this, Mahowald et al. [14] investigated the correlation between plantar fascia thickness and symptoms of plantar fasciitis as a way to gauge the efficacy of treatment modalities. They found that a reduction in pain correlated strongly with a reduction in plantar fascia thickness. The thickness of the plantar fascia, however, remained above 4 mm, which would still be indicative of PHPS (Figure 6).[3][14]
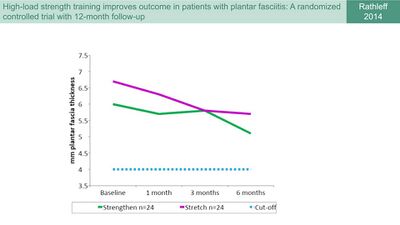
Rathleff et al. [15] used thickness of the plantar fascia as an outcome measure to assess the efficacy of shoe inserts and plantar fascia specific stretching vs shoe inserts and high-load strength training in patients with plantar fasciitis. They also reported a reduction in plantar fascia thickness in both groups, but similarly the plantar fascia thickness remained more than 4 mm (Figure 7).[3][15]
Additional imaging findings related to the plantar fascia can be found in Figure 8.[2][3][3][12]
Figure 8. Additional characteristics of the plantar fascia as evident with imaging [3]
Imaging of other structures in the foot
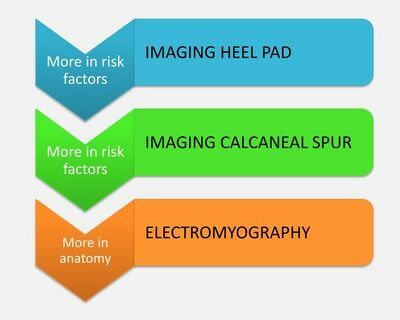
Besides plantar fascia thickness, heel pads and calcaneal spurs are also evident on imaging, but, as discussed here, are not significant in PHPS. The influence of electromyography will be discussed in more depth in the anatomy course (Figure 9).
Figure 9. Imaging of other structures of the foot [3]
Even though medical imaging studies can be useful in detecting abnormalities in the feet of individuals with heel pain, there is still controversy about its ability to identify individuals with PHPS and to reflect meaningful changes in the condition of the patient. It is also not commonly available to many clinicians for the on-site assessment of patients.[1]
Tinel’s Tarsal Tunnel Test[edit | edit source]
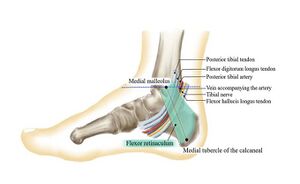
Tarsal tunnel syndrome is an entrapment of the tibial nerve or its branches in the fibrous tarsal tunnel. It has also been proposed as a cause of plantar heel pain (Figure 10).[16][17] Tinel’s tarsal tunnel test, which involves tapping on the tibial nerve at the tarsal tunnel to elicit pain/tingling in the heel, has therefore been suggested as an assessment for PHPS (Figure 10).[3][17] There is, however, currently no evidence to support the use of Tinel’s tarsal tunnel test in PHPS.
Patient Reported Outcomes[edit | edit source]
"Patient Reported Outcomes (PRO) is directly reported by the patient without interpretation of the patient’s response by a clinician or anyone else and pertains to the patient’s health, quality of life, or functional status associated with health care or treatment". [18] Following the lack of objective measures to assess PHPS, many studies have used patient reported outcomes as a way to gauge the efficacy of treatment modalities in individuals with PHPS.[1] Both clinical guidelines on heel pain by the American Physical Therapy Association [9][19] recommended the use of four different PROs in the assessment of PHPS (Figure 11).
Figure 11. Patient reported outcomes recommended by the Clinical Guidelines of the American Physical Therapy Association [3][9][19]
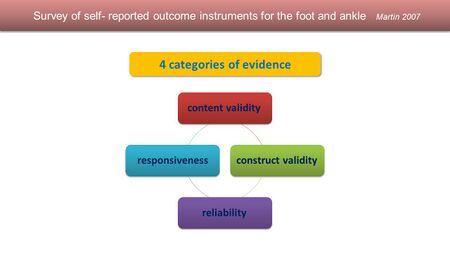
Martin et al. [20] proposed that in order to properly interpret their scores, outcome measures for the foot and ankle should possess four distinct qualities. These qualities should be considered by clinicians when selecting and using an outcome measure (Figure 12).
Figure 12. Categories of evidence for PROs [3][20]
Following this, Martin et al. [20] recommended the use of five instruments in individuals with foot and ankle-related pathology, four of which also coincided with those proposed by the Clinical Guidelines of the American Physical Therapy Association (Figure 13).[9][19]
Figure 13. Self-reported outcome measures for the foot and ankle [3][9] [19][20]
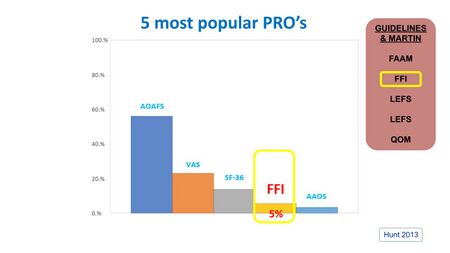
In a meta-analysis study of the foot and ankle literature from 2002-2011, Hunt et al. [21] identified 139 different questionnaires for foot pain. The five most popular PROs used included the Foot Function Index (FFI), which was also included in the Clinical Guidelines (Figure 14).[9][19][21]
Figure 14. The five most popular PROs for ankle and foot pain [3][21]
Figure 15 contains a few concluding points that should be considered when using PROs.[3]
Figure 15. Conclusion on PROs [3]
PROs might be ideal for determining the patient’s perception of their abilities, but fail to fully capture the extent of the patient’s functioning.[1] PROs are therefore more useful for assessing a series of treatments rather than individual treatments.[1]
What do Physiotherapists do?[edit | edit source]
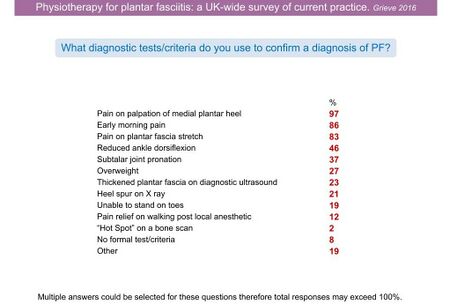
Because there is a lack of objective measures for assessing PHPS, Grieve and Palmer [22] conducted an online survey by UK physiotherapists on the current approach to plantar fasciitis. They received 257 completed questionnaires in response to their survey. A summary of their findings is displayed in Figure 16. [3][22]
Figure 16. Current Practice of Physiotherapists for diagnosing plantar fasciitis [3][22]
However, each of these factors can be faulted based on a lack of supporting evidence, as discussed here. This reiterates that there is a lack of evidence for physical examination tests to be used in the clinical assessment of patients with PHPS and brings us to the aim of this course series - the introduction of a new protocol for PHPS. Saban and Masharawi[1] have identified three clinical tests that can provoke the relevant heel pain in individuals with PHPS and, therefore, be useful in assessing PHPS. These tests are as follows:
- Single-leg static stance
- Single-leg half squat
- Single-leg heel raise
Conclusion[edit | edit source]
Based on the review of available literature, the following are assessment recommendations for plantar heel pain:
- The Windlass test is not sensitive enough for diagnosis of PHPS
- Palpation and Pressure Point Threshold are not recommended for PHPS assessment
- Imaging of plantar fascia assessing tissue thickness is useful as a diagnostic tool for patients with plantar heel pain. However, it does not measure the change in patients' condition.
- No evidence supports Tinel's Tarsal Tunnel Test as an assessment tool for PHPS.
- Patient Reported Outcomes (PROs) can be used to evaluate an entire series of treatments. PROs are commonly used for research purposes.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 Saban B, Masharawi Y. Three single leg standing tests for clinical assessment of chronic plantar heel pain syndrome: static stance, half-squat and heel rise. Physiotherapy. 2017 Jun 1;103(2):237-44.
- ↑ 2.0 2.1 2.2 2.3 2.4 Draghi F, Gitto S, Bortolotto C, Draghi AG, Belometti GO. Imaging of plantar fascia disorders: findings on plain radiography, ultrasound and magnetic resonance imaging. Insights into imaging. 2017 Feb;8(1):69-78.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 3.16 3.17 3.18 3.19 3.20 3.21 3.22 3.23 3.24 Bernice Saban 2021. Assessment of Plantar Heel Pain - A Literature Review. Plus Course. 2021
- ↑ 4.0 4.1 4.2 Bolgla LA, Malone TR. Plantar fasciitis and the windlass mechanism: a biomechanical link to clinical practice. Journal of athletic training. 2004 Jan;39(1):77.
- ↑ Hicks JH. The mechanics of the foot: II. The plantar aponeurosis and the arch. Journal of anatomy. 1954 Jan;88(Pt 1):25.
- ↑ 6.0 6.1 6.2 De Garceau D, Dean D, Requejo SM, Thordarson DB. The association between diagnosis of plantar fasciitis and Windlass test results. Foot & ankle international. 2003 Mar;24(3):251-5.
- ↑ Alshami AM, Babri AS, Souvlis T, Coppieters MW. Biomechanical evaluation of two clinical tests for plantar heel pain: the dorsiflexion-eversion test for tarsal tunnel syndrome and the windlass test for plantar fasciitis. Foot & ankle international. 2007 Apr;28(4):499-505.
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 Saban B, Masharawi Y. Pain threshold tests in patients with heel pain syndrome. Foot & ankle international. 2016 Jul;37(7):730-6.
- ↑ 9.0 9.1 9.2 9.3 9.4 9.5 Martin RL, Davenport TE, Reischl SF, McPoil TG, Matheson JW, Wukich DK, McDonough CM, Altman RD, Beattie P, Cornwall M, Davis I. Heel pain—plantar fasciitis: revision 2014. Journal of Orthopaedic & Sports Physical Therapy. 2014 Nov;44(11):A1-33.
- ↑ Drake C, Mallows A, Littlewood C. Psychosocial variables and presence, severity and prognosis of plantar heel pain: A systematic review of cross‐sectional and prognostic associations. Musculoskeletal Care. 2018 Sep;16(3):329-38. DOI:10.1002/msc.1246
- ↑ Allam AE, Chang KV. Plantar Heel Pain. StatPearls [Internet]. 2021 Feb 5.
- ↑ 12.0 12.1 12.2 Riel H, Cotchett M, Delahunt E, Rathleff MS, Vicenzino B, Weir A, Landorf KB. Is ‘plantar heel pain’a more appropriate term than ‘plantar fasciitis’? Time to move on. Br J Sports Med.2017 Nov;51(22):1576-1577.
- ↑ Drake C, Whittaker GA, Kaminski MR, Chen J, Keenan AM, Rathleff MS, et al. Medical imaging for plantar heel pain: a systematic review and meta-analysis. J Foot Ankle Res. 2022 Jan 22;15(1):4.
- ↑ 14.0 14.1 14.2 Mahowald S, Legge BS, Grady JF. The correlation between plantar fascia thickness and symptoms of plantar fasciitis. Journal of the American Podiatric Medical Association. 2011 Sep;101(5):385-9.
- ↑ 15.0 15.1 15.2 Rathleff MS, Mølgaard CM, Fredberg U, Kaalund S, Andersen KB, Jensen TT, Aaskov S, Olesen JL. High‐load strength training improves outcome in patients with plantar fasciitis: A randomized controlled trial with 12‐month follow‐up. Scandinavian journal of medicine & science in sports. 2015 Jun;25(3):e292-300.
- ↑ Rose B, Singh D. Inferior heel pain. Orthopaedics and Trauma. 2020 Feb 1;34(1):10-6.
- ↑ 17.0 17.1 Rinkel WD, Cabezas MC, Birnie E, Coert JH. The natural history of tarsal tunnel syndrome in diabetic subjects. Journal of Plastic, Reconstructive & Aesthetic Surgery. 2020 Aug 1;73(8):1482-9.
- ↑ Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (editors). Cochrane Handbook for Systematic Reviews of Interventions version 6.4 (updated August 2023). Cochrane, 2023. Available from https://training.cochrane.org/handbook [last access 22.10.2023]
- ↑ 19.0 19.1 19.2 19.3 19.4 McPoil TG, Martin RL, Cornwall MW, Wukich DK, Irrgang JJ, Godges JJ. Heel pain—plantar fasciitis. journal of orthopaedic & sports physical therapy. 2008 Apr;38(4):A1-8.
- ↑ 20.0 20.1 20.2 20.3 Martin RL, Irrgang JJ. A survey of self-reported outcome instruments for the foot and ankle. Journal of Orthopaedic & Sports Physical Therapy. 2007 Feb;37(2):72-84.
- ↑ 21.0 21.1 21.2 Hunt KJ, Hurwit D. Use of patient-reported outcome measures in foot and ankle research. JBJS. 2013 Aug 21;95(16):e118.
- ↑ 22.0 22.1 22.2 Grieve R, Palmer S. Physiotherapy for plantar fasciitis: a UK-wide survey of current practice. Physiotherapy. 2017 Jun 1;103(2):193-200.