Acute Myeloid Leukemia Case Study
Author/s[edit | edit source]
Chelsea Bentley, Aubrey Jacobi, Lauren Jones, Gina Pottkotter, and MegAnne Punt from the Bellarmine University Physical Therapy Program's Pathophysiology of Complex Patient Problems Project.
Patient Characteristics[edit | edit source]
- 66 year old male, named Bert
- Retired Navy Seal and school bus driver
- Current Volunteer at Veteran’s Affairs Hospital in Louisville, KY
- Lives with wife of 45 years
- Type II diabetic, controlled
- Left Transtibial Amputation secondary to diabetic ulcer
- Previous physical therapy in acute, rehabilitation, and outpatient settings following surgery
Examination[edit | edit source]
SUBJECTIVE:
- Chief Complaint: Patient presents to outpatient physical therapy clinic (2 months post discharge), with desire for further prosthetic training. Patient’s prior outpatient PT included gait training and stair training with use of cane. Now, patient desires more independence without assistive device and further training to accommodate his increased activity level in the community with his volunteer work. Patient notes that he feels increasingly tired after a day of volunteering, therefore he wants more endurance training with his prosthetic.
- Medical History: [1]
• Previous history of smoking, 30 pack years
• Quit smoking at age 48, when he was diagnosed with Type II diabetes
• Diabetic ulcer on L heel, led to transtibial amputation approximately 1 year ago
• Patient reports history of anemia while in hospital post-op - Recent onset of headaches, 3 out of 10 on pain scale[1]
- Patient reports shortness of breath with increased activity[1]
- 1 year post-operation from amputation
• Discharged from outpatient physical therapy 2 months prior to current visit
Self Report Outcome Measures:
- Pain Scale:
• Headaches reported 3 out of 10 on Visual Analog Scale
• Otherwise, patient complains of no pain - Short Form 36 Questionnaire (Quality of Life Measure)[2]
• Physical Functioning Score (PF) of 45 (significant decrease in physical functioning )
• Role limitations due to physical health (RP) score of 25 (significant limitations)
• Vitality Score of 20 (significant decrease in quality of life)
• Physical Health overall largely impacted, score of 31
• Mental Health, stable with score of 59
• Scores under 50 represent significant impact
Physical Performance Measures:
- Amputee Mobility Predictor
• Score of 37/47
• Indicates Functional Level 3/K3[3] - 5 Time Sit Stand Test (endurance)[4]
• 12.5 seconds (average for age group 11.4 secs, fall risk over 12 seconds)[5]
OBJECTIVE:
- Vital Signs:[6]
• Blood Pressure 110/75 mmHg
• Heart Rate 64bpm
• Respiratory Rate 18bpm(at rest)
• Temperature 99.4°F
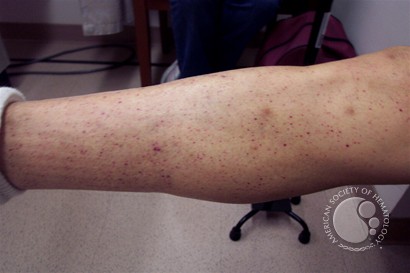
- Petechaie and bruising noted on patients R lower leg and ankle, also minor spots noted on residual limb (example in the picture below)[6][7]
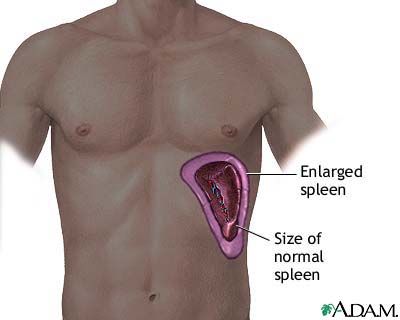
- Due to fever, palapation of abdomen revealed enlarged spleen and tenderness (example of enlarged spleen (splenomegaly) in the picture below)[8]
- Upper and lower quarter screen ROM WNL.
- All deep tendon reflexes present and symmetrical
- Sensation diminished over L residual limb and R foot
- Hip flexion 4-/5 bilaterally, Shoulder abduction 4-/5 bilaterally, shoulder flexion 4-/5 bilaterally. All other manual muscle tests within normal limits.
Summarization of Examination/Clinical Impression[edit | edit source]
Following evaluation, the patient presents with signs and symptoms consistent with proximal muscle weakness. Patient demonstrates diminished sensation in bilateral lower extremities. The patient presents with increased fatigue, headaches, and adventitious breath sounds consistent with possible infection. The patient’s 5 Time Sit-to-Stand outcome measure indicates decreased ability to perform ADLs due to fatigue. Additionally, Mr. Bert’s AMP score indicates the ability to perform most activities, but the patient’s self-report demonstrates limitation due to restricted endurance. Due to the patient’s risk factors of diabetes and age coupled with enlarged spleen upon palpation and tenderness, physical therapy recommends referral back to the primary care physician for further evaluation and blood work.
Risk Factors for AML Noted in Clinical Presentation[1]
- Age (greater than 63 y/o increases risk for AML; 80% of AML cases occur in adults)
- Male
- History of Smoking
- Diabetes
- History of Anemia
Signs and Symptoms[1]
- Petechiae
- Fatigue
- Headache
- Proximal muscle weakness
- Enlarged spleen
- Signs of possible infection (low grade fever, adventitious breath sounds)
The clinical impression of this patient is that the proximal muscle weakness and increased fatigue are consistent with presentation of acute myeloid leukemia.The patient will be referred back to his primary care physician. The patient would benefit from physical therapy to strengthen proximal muscles and increase cardiovascular endurance.
Interventions[edit | edit source]
Since the patient will be undergoing concurrent cancer treatments, the main focus of the interventions will be aerobic and strength training along with pain management, when necessary. Physical therapy treatment sessions will be symptom dependent and it will be vital to monitor the patient for signs of excessive fatigue. The patient should also be monitored for chemo-induced neuropathies, which could put them at a greater risk for falls.
•Aerobic training – Current literature shows that walking for at least 12 minutes, five times per week for 3 weeks at a pace that would get them a heart rate of RHR+30bpm. This prescription is sufficient to maintain the cardiovascular system and alleviate symptoms of fatigue, anxiety and depression.[9]
•Strength training- Strength training twice a day, 3 times per week, for 10-30 minutes at 40-50% of HRR has been shown to decrease fatigue and depression in patients undergoing chemotherapy. Upper and lower extremity resistance exercises should be used.[10]
•Combination of strength and aerobic training – It is important to include both types of exercise into a patient's regimen. A combination helps to combat the effects of bed rest and deconditioning, which are common with patients undergoing chemotherapy.[11]
•Pain Management –Hot/cold packs, TENS, and massage are all modalities that can be used to decrease pain in patients.
Expected Outcomes[edit | edit source]
After completion of a 6 week aerobic and resistance training the patient should show improvements in physical endurance, as well as aerobic fitness with improvements in peak VO2, and increases in muscle strength for both upper and lower extremities.
At the end of the 6 weeks the patient should also have an increase in body weight, with a decrease in body fat. This is crucial, as most AML patients lose weight throughout the disease process and chemo sessions[12][13]. It is important for the patient to not only gain weight, but to gain lean muscle mass instead of fat.
The patient should also show significant improvements in global quality of life, fatigue, anxiety, and emotional function, as well as improvements in depression. The patient may also experience a decrease in pain, through the use of heat/cold packs as well as pharmaceutics.
Discussion[edit | edit source]
This case study displays a cluster of red flag symptoms that cannot be overlooked in any patient case. What appears to be a simple patient in need of prosthetic training, turns out to be a far more complex case. This is a reminder to all practioners, including physical therapy in this case, to not just assume a patient is as straight forward as they initially appear. Through a detailed patient history, clinical exam findings, and a knowledge of red flag symptoms, the physical therapist is able to ascertain that the patient needs a follow up by a primary care physician.
Also, this case displays the need to understand co-morbidities and risk factors. The patient, Bert, has a history of diabetes and smoking, which are risk factors for numerous conditions. Instead of seeing Bert just as a patient with a prosthetic limb, one must not forget that the reason he has a prosthetic is becasue of his diabetes. When you combine this history, increased fatigue, petechiae, proximal muscle weakness, and enlarged spleen, the physical therapist is able to refer for further testing.
With the increae in direct access patients, it is imperative that physical therapists perform a thorough evalulation. If the physical therapist would have taken Bert as a patient in need of endurance training, and not performed a full evaluation, a physcian referral would have been missed, and his case of acute myeloid leukemia could have easily been overlooked. To provide the highest quality care, this case reminds everyone within the healthcare spectrum that quality knowledge and appropriate referral is needed to maintain the highest patient care.
Related Pages[edit | edit source]
http://www.physio-pedia.com/Acute_Myeloid_Leukemia
References[edit | edit source]
References will automatically be added here, see adding references tutorial.
- ↑ 1.0 1.1 1.2 1.3 1.4 Mooney, K and Rice, E. Acute Myeloid Leukemia [Internet]. Physiopedia [cited March 3, 2015]. Available from: http://www.physio-pedia.com/Acute_Myeloid_Leukemia.
- ↑ SF-36.org [Internet]. Available at: http://www.sf-36.org/demos/SF-36.html. Accessed March 3, 2015.
- ↑ Gailey RS, Roach KE, Applegate EB, Cho B,Cunniffe B, Licht S, Maguire M, Nash MS. The Amputee Mobility Predictor: an instrument to assess determinants of the lower-limb amputee ability to ambulate. Arch Phys Med Rehabil 2002;83:613-27.
- ↑ Strengthening exercises: lower extremity exercises [internet]. 2013 [cited 2015 March 25]. Available from: http://www.columbialungtransplant.com/guide_e_lowchair.html.
- ↑ Rehab Measures: Five Time Sit to Stand Test. Rehab Measures Database Website. http://www.rehabmeasures.org/Lists/RehabMeasures/DispForm.aspx?ID=1015. Published June 20, 2013. Accessed February 17, 2015.
- ↑ 6.0 6.1 Diseases and Conditions: Acute myelogenous leukemia (AML) [Internet]. Mayo Clinic Website. 2012 [cited March 3, 2015]. Available from: http://www.mayoclinic.org/diseases-conditions/acute-myelogenous-leukemia/basics/definition/con-20043431.
- ↑ Maslak, P. American Society of Hematology Image Bank [internet]. 2008 October 1 [cited 2015 March 25]. Available from: http://imagebank.hematology.org/AssetDetail.aspx?AssetID=3689&AssetType=Asset
- ↑ Splenomegaly [internet]. [cited 2015 March 25]. Available from: http://lookfordiagnosis.com/mesh_info.php?term=splenomegaly&lang=1
- ↑ Chang PH, Lai YH, Shun SC, et al. Effects of a walking intervention on fatigue-related experiences of hospitalized acute myelogenous leukemia patients undergoing chemotherapy: a randomized controlled trial. J Pain Symptom Manage. 2008;35(5):524-34. http://www.ncbi.nlm.nih.gov/pubmed/18280104 (Accessed March 23, 2015).
- ↑ Battaglini CL, Hackney AC, Garcia R, Groff D, Evans E, Shea T. The effects of an exercise program in leukemia patients. Integr Cancer Ther. 2009;8(2):130-8. http://www.ncbi.nlm.nih.gov/pubmed/19679621 (Accessed March 20, 2015).
- ↑ Alibhai, Shabbir M.H.; O’Neill, Sara; Fisher-Schlombs, Karla, et. al. A clinical trial of supervised exercise for adult inpatients with acute myeloid leukemia (AML) undergoing induction chemotherapy. Leuk Res. 2012 Oct; 36(10): 1255–1261. http://www.ncbi.nlm.nih.gov/pubmed/22726923 (Accessed March 20, 2015)
- ↑ Alibhai SMH, O’Neill S, Fisher-Schlombs K, Breunis H, Brandwein JM, Timilshina N, et al. A clinical trial of supervised exercise for adult inpatients with acute myeloid leukemia (AML) undergoing induction chemotherapy. Leuk Res. 2012;36:1255–61.
- ↑ Cheng MJ, Hourigan CS, Smith TJ. Adult Acute Myeloid Leukemia Long-term Survivors. J Leuk (Los Angeles, Calif) [Internet]. 2014 Apr 10 [cited 2015 Mar 18];2(2). Available from: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=4167020&tool=pmcentrez&rendertype=abstract