2D Slow-Motion Video Data Motion Analysis Techniques
Original Editor - Merinda Rodseth based on the course by
Damien Howell
Top Contributors - Merinda Rodseth, Kim Jackson, Tarina van der Stockt, Jess Bell and Thomas Longbottom
Introduction[edit | edit source]
Screening and assessment are important in any medical care model and in physiotherapy, it involves the analysis of movement patterns.[1] The analysis of human movement is of great interest for performance, injury prevention and optimal recovery from injury or trauma.[2][3] Most studies published on human kinematics have used three-dimensional (3D) motion analysis systems which are expensive, time-consuming and generally not widely available in clinical practice.[4] With developments in technology, more cost-effective solutions are available for assessing the human body and two-dimensional (2D) imaging has become an alternative to costly 3D systems.[2][5] Two-dimensional video analysis has since become popular in clinical practice as it only requires a digital video camera and digitising software, which are universally available, reasonably cheap and mostly portable.[6][7] Video analysis involves the “systematic observation and interpretation of video to improve objectivity and reduce bias and subjectivity that are inherent in human observation”.[8]
Windt et al [9] proposed a clinical decision-making framework consisting of four clinical questions to consider before investing in new technology, two of which were answered in the previous discussion on the benefits of 2D slow-motion video analysis:
- Will the information promised in the new technology be helpful? Conclusion: It has many benefits and indications and is of value when dealing with clients.
- Can you trust the information that it provides? Conclusion: Yes, it can be trusted.
- Can you integrate, manage and analyse this new information effectively?
- Can you implement this new technology in your practice?
Question three and four of the framework will be discussed in this page, with a specific focus on the:
- “How to” techniques of recording, analysing, storing and retrieving video data in order to improve the validity and reliability of the slow-motion analysis of movement impairments
- Identification of key reference points that are useful to describe motion when performing 2D slow-motion video analysis
This approach to 2D slow-motion video analysis is based on the frameworks utilised for radiographs/diagnostic imaging with the generic steps:
- Record the image
- Analyse the image
- Store and retrieve the data
Preparation[edit | edit source]
The first step in preparing to record involves explaining the purpose/necessity of capturing the image/video to the patient and obtaining their permission.[10][11]
“The way you move is contributing to your pain. I would like to analyse the way you move with the help of slow-motion video analysis”. “I see something in the way you move that I would like to show you through the use of an image/video”.
Planning of the recording session involves many factors, such as: [10]
- Staging (while considering privacy)
- Background of the image including the lighting
- Distance from the camera to the patient
- Choosing the camera
- Which views to collect
- Which movements elicit the pain and/or are the deviant movements
- Plan for the end-point of the video (e.g. record the patient moving when in pain)
Equipment Considerations and Set-Up[edit | edit source]
1. Choose a camera
- Standard, traditional digital camera
- Smartphone
- Tablet (benefit - larger screen to share the video with the patient)
2. Decide on the orientation of the smartphone/tablet
- Landscape (generally suggested as the better option)
- Portrait
3. Mount the camera on a stable tripod or alternatively hold it in the hand (stable camera mounting) [11]
4. Maximise the camera-to-subject distance - “far enough”[12]
5. Maximise the size of the image [11]
6. Add a “grid” to the screen
7. Align the optical axis of the camera perpendicular (at an angle of 90°) to the plane of motion (be perpendicular to the motion and far away from the subject[12]
8. Account for Parallax error
When performing a video analysis, certain procedures must be carefully followed in order to minimise systematic and random errors.[11] With 2D analysis, the movement being analysed must be confined to a single, pre-defined plane - the plane of motion. Any movement measurements outside of this plane are subject to perspective error/parallax error.[11]
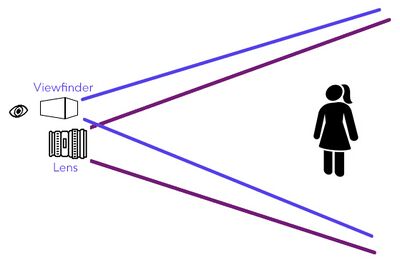
Parallax is “a displacement or difference in the apparent position of an object viewed along two different lines of sight”[13] and is caused by viewing an individual at an oblique angle as they walk through the camera field.[6] Camera parallax also occurs when the lens and the viewfinder/display are offset on the camera.[10][13] This creates the effect that the position or direction of an object appears to differ when viewed from different positions (as seen through the viewfinder versus the lens of the camera). Parallax is most noticeable when objects/people are close to the camera and become relatively insignificant at longer distances.[13][14] To prevent parallax errors when filming:[10]
- Only measure angles and linear displacements when the patient is perpendicular to the camera lens (sagittal/side-view movements) [4][15]
- The camera can be fixed while the patient moves back and forth turning through 180° (anterior-posterior view) - obtain at least 2 views
- The patient and the camera can move together - necessitates the use of a gimbal stabiliser to keep the camera steady and prevent jerking
- Stage a triangle ambulation where the camera is fixed and the patient is turning through 60° angles
- Patient runs/walks from point A to B while we film from the right side
- At point B, the patient turns through 180° and we film from his/her left side
- Back at point A, the patient turns 60° and runs straight at the camera (front view) (point C)
- When close to the camera, the patient turns 60° and runs to point B (back view)
- Repeat this a sufficient number of times to obtain a good sampling rate
- Obtaining at least 2 views when filming improves accuracy[3][4][15]
- Anterior-posterior
- Right side view
- Left side view
- Place the camera “far enough away” from the patient being filmed[12]
9. Ensure optimal lighting of the patient[10][11]
- Have the light source behind the camera
- When recording inside, have the windows/lights behind the camera
- For outside filming, ensure the sun is behind the camera and film in a shaded area for easier immediate review of the video
- Fluorescent ceiling lights might be insufficient if filming at night and additional lighting needed for better exposure
- Avoid recording outside at dusk or dawn - difficult to get the correct lighting
- More lighting is needed when recording at frame rates greater than 30 fps or recording in slow-motion
10. Select an appropriate frame rate and decide whether to record in regular speed/slow-motion[10][11]
Frames per second (fps) is a measure of how motion video is displayed. Each frame is a still image. If a video is captured and played back at 30 fps, each second of the video shows 30 distinct still images (therefore 30 images per second). The higher the fps, the smoother the motion appears. Standard smartphones and tablets will record at 30 fps which is generally sufficient for walking and general patient interactions.[1] High-speed activities such as running or sporting activities require higher frame rates (60 fps or more).[10][11][16]
Recordings can be made at regular speed (30 fps) and played back in slow-motion (at 60 fps) or in slow-motion mode at a higher frame rate (100 fps) and played back in slow-motion.
Recording in regular speed:
- Requires less storage space
- Requires less light
- Requires a video playback function in slow motion for giving immediate feedback to the patient
Recording in slow motion:
- Takes more storage space
- Requires more light
- Requires the use of a tripod
- Easy to share in real-time with the patient to give immediate feedback
11. Visualise key landmarks on the body[10][11] - ensure that the body landmarks relevant to the analysis are exposed and can be clearly seen
- Expose the beltline
- Expose the popliteal skin crease at the back of the knee
- For upper extremity expose T1, shoulder blades and elbows
Recording the Image/Video[edit | edit source]
Rehearsing before recording familiarises the patient with the movements to be recorded and allows the clinician to practice the verbal cueing of the patient. Following the rehearsal, capture the recording while ensuring that the end-point is achieved. It is important to obtain sufficient sampling to accommodate for the parallax effect.[10]
Perform a preliminary review and analysis of the video recording with the patient to ensure the video recorded well and there are no videography errors. Assure the patient that this is only a preliminary review and an in-depth analysis will be done after the visit and the results shared at the next visit. The initial analysis can be done using the standard video playback function while incorporating the scrubbing function available on most smartphones/tablets. Scrubbing entails adjusting the speed of the playback through the use of the dot/button on the slide bar and creates a way to do an initial slow-motion analysis.
Making use of the scrubbing function: [10]
- During the video playback, tap and hold the dot/button on the slider bar, then drag it left or right to scrub backwards or forwards at a slow or fast speed
- To change the scrub speed, slide your finger up/down on the slider bar while holding the dot
- The display will change to show the scrub speed. Options include the default, ½ speed, ¼ speed and Fine
Video Editing Software Applications[edit | edit source]
The video motion analysis can also be done with the use of video editing software which allows for other functions as well. When choosing a video editing software application, desirable functions or features to perform slow-motion analysis are:[10]
- Allow a frame-by-frame analysis and capture still images [7][18]
- Split screen function
- Line drawing function
- Zoom function in the software
- Ability to convert the file format from one operating system to another (Windows, iOS, Android)
Of the many video editing software applications available, Kinovea (open-source) and Slow Motion Video Function are particularly useful (see the image below).[1][4][10]
The Initial Video Analysis[edit | edit source]
It is useful to do the initial analysis with the patient in real-time while striving to engage the patient with evoking questions. Keep in mind the framework “pause - prompt - praise” when sharing the video with the patient.[10]
- Pause - “What do you see?”
- Prompt the patient by asking evoking questions
- “Do you see…?”
- “What do you think you can change?”
- “What ideas do you have to alter the way you walk/run?”
- “How important is this?”
- Praise - Give positive feedback even when weaknesses/problems are identified
Making the Analysis more Reliable[edit | edit source]
The second question asked by Windt et al [9] is “Can you trust the information that it provides?”. The following factors play a role in enhancing the reliability of the video analysis:[10]
1. Develop a workflow system that is consistent, thorough and systematic.[1][15]
- View and analyse from head-to-toe
- View both right and left sides of the body
- View the uninvolved side (assuming that it is less deviant)
- View the involved side
2. Define a standard point or time when the movement is observed and measured.
- When the patient/image is at right angles to the camera
- When pain is provoked, for example during the stance phase
- When the patient is fatigued enough
- When the patient is moving fast enough
- When the deviant movement occurs
3. Use quality improvement processes - video data allows for repeated observations and analyses of movement without fatiguing the patient or generating additional pain/injury which allows the clinician to determine the reliability of the analysis. Quality improvement processes include:
- Self-reflection
- Peer reviews - video reviews between clinicians
- Repeated video observations at different time frames by a solo practitioner
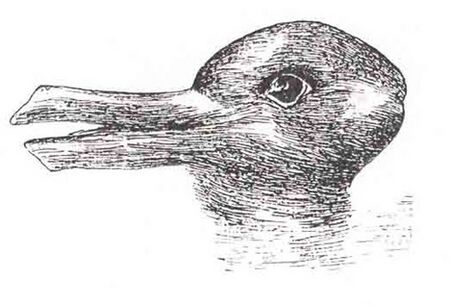
4. Be aware of the influence of confirmation biases - our confirmation biases can affect our perception of images. Sharing images/videos with peers can address the possibility of an individual clinician’s confirmation biases. The image below provides an example of differences in perception, with some people seeing a duck and others a rabbit.[10]
Considerations for Uploading and Transferring Video Data[edit | edit source]
Some factors to consider for uploading/transferring the recorded video data include:
- The necessary hardware to get the data from the camera to storage - USB cable/card slot on computer/card USB adapter/Wi-Fi
- Software applications for transferring the video from a smartphone to the patient’s electronic medical record[19] - dedicated clinical imaging applications are emerging:
- WABA Medical Pics
- Secure Image Transfer
- Clinical Uploader
- PicSafe
Considerations for Storing and Retrieving Video Data[edit | edit source]
After recording the image and doing an initial analysis, it is important to establish a way to store and retrieve the video file as is done with radiographs. Factors to consider include:[10]
- Where to store it? In the cloud, on a hard drive, or possibly even both
- If using a personal camera, store the file in a separate folder from personal images
- Storage needs privacy, security, encryption and password protection [19]
- Rename the video file from the assigned file number to the patient’s medical record number and specify the date of the recording
- Video editing packages also allow for “tagging” keywords: activity, diagnosis, view, preferred original movement, altered intervened movement, other information
- Store raw video data and data regarding the narration of analysis interpretations
- Make use of “trimming” processes - delete or keep audio, resizing images
- Have a systematic backup process
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Parks MT, Wang Z, Siu KC. Current low-cost video-based motion analysis options for clinical rehabilitation: a systematic review. Physical therapy. 2019 Oct 28;99(10):1405-25.
- ↑ 2.0 2.1 Peart DJ, Balsalobre-Fernández C, Shaw MP. Use of mobile applications to collect data in sport, health, and exercise science: A narrative review. The Journal of Strength & Conditioning Research. 2019 Apr 1;33(4):1167-77.
- ↑ 3.0 3.1 Colyer SL, Evans M, Cosker DP, Salo AI. A review of the evolution of vision-based motion analysis and the integration of advanced computer vision methods towards developing a markerless system. Sports medicine-open. 2018 Dec;4(1):1-5.
- ↑ 4.0 4.1 4.2 4.3 Dingenen B, Barton C, Janssen T, Benoit A, Malliaras P. Test-retest reliability of two-dimensional video analysis during running. Physical therapy in Sport. 2018 Sep 1;33:40-7.
- ↑ Numata H, Nakase J, Kitaoka K, Shima Y, Oshima T, Takata Y, Shimozaki K, Tsuchiya H. Two-dimensional motion analysis of dynamic knee valgus identifies female high school athletes at risk of non-contact anterior cruciate ligament injury. Knee Surgery, Sports Traumatology, Arthroscopy. 2018 Feb;26(2):442-7.
- ↑ 6.0 6.1 Alahmari A, Herrington L, Jones R. Concurrent validity of two-dimensional video analysis of lower-extremity frontal plane of movement during multidirectional single-leg landing. Physical Therapy in Sport. 2020 Mar 1;42:40-5.
- ↑ 7.0 7.1 Finkbiner MJ, Gaina KM, McRandall MC, Wolf MM, Pardo VM, Reid K, Adams B, Galen SS. Video movement analysis using smartphones (ViMAS): a pilot study. Journal of visualized experiments: JoVE. 2017(121).
- ↑ Hendricks S, Till K, Den Hollander S, Savage TN, Roberts SP, Tierney G, Burger N, Kerr H, Kemp S, Cross M, Patricios J. Consensus on a video analysis framework of descriptors and definitions by the Rugby Union Video Analysis Consensus group. British journal of sports medicine. 2020 May 1;54(10):566-72.
- ↑ 9.0 9.1 Windt J, MacDonald K, Taylor D, Zumbo BD, Sporer BC, Martin DT. “To Tech or Not to Tech?” A Critical Decision-Making Framework for Implementing Technology in Sport. Journal of Athletic Training. 2020 Sep;55(9):902-10.
- ↑ 10.00 10.01 10.02 10.03 10.04 10.05 10.06 10.07 10.08 10.09 10.10 10.11 10.12 10.13 10.14 10.15 Howell D. Techniques of Two-Dimensional Slow-Motion Video Data Motion Analysis Course. Plus , 2022.
- ↑ 11.0 11.1 11.2 11.3 11.4 11.5 11.6 11.7 11.8 Payton C, Bartlett R. Eds. Biomechanical Evaluation of Movement in Sport and Exercise: The British Association of Sport and Exercise Sciences Guidelines. Routledge; 2008.
- ↑ 12.0 12.1 12.2 Stephens J, Bostjancic M, Koskulitz T. A study on parallax error in video analysis. The Physics Teacher. 2019 Mar;57(3):193-5.
- ↑ 13.0 13.1 13.2 Camerapedia Fandom. Parallax. [Accessed 9 Nov 2021].
- ↑ Wikipedia. Parallax. Available from https://en.wikipedia.org/wiki/Parallax [Accessed 9 November 2021].
- ↑ 15.0 15.1 15.2 Souza RB. An evidence-based videotaped running biomechanics analysis. Physical Medicine and Rehabilitation Clinics. 2016 Feb 1;27(1):217-36.
- ↑ van der Kruk E, Reijne MM. Accuracy of human motion capture systems for sport applications; state-of-the-art review. European Journal of Sport Science. 2018 Jul 3;18(6):806-19.
- ↑ Kellan Reck. Video Frame Rates Explained. Published April 18 2018. Available from https://www.youtube.com/watch?v=Iwog2NN6iBw [last accessed 12 November 2021].
- ↑ Puig-Diví A, Escalona-Marfil C, Padullés-Riu JM, Busquets A, Padullés-Chando X, Marcos-Ruiz D. Validity and reliability of the Kinovea program in obtaining angles and distances using coordinates in 4 perspectives. PloS one. 2019 Jun 5;14(6):e0216448.
- ↑ 19.0 19.1 Chandawarkar R, Nadkarni P. Safe clinical photography: best practice guidelines for risk management and mitigation. Archives of Plastic Surgery. 2021 May;48(3):295.
- ↑ Let’s Teach Science. Video Analysis Considerations. Published Aug 30 2020. https://www.youtube.com/watch?v=4SW0D_ywZYQ [last accessed 12 November 2021].