Idiopathic Toe Walking: Difference between revisions
No edit summary |
No edit summary |
||
| Line 5: | Line 5: | ||
== Introduction == | == Introduction == | ||
Idiopathic toe walking (ITW) is a diagnostic term used to describe a condition in otherwise healthy, ambulant children who present with a toe-toe gait. It is a diagnosis of exclusion, where no determinable pathology exists.<ref name=":3" /> | Idiopathic toe walking (ITW) is a diagnostic term used to describe a condition in otherwise healthy, ambulant children who present with a toe-toe gait. It is a diagnosis of exclusion, where no determinable pathology exists.<ref name=":3">Van Kuijk AA, Kosters R, Vugts M, Geurts AC. [https://medicaljournalssweden.se/jrm/article/view/15636 Treatment for idiopathic toe walking: a systematic review of the literature]. Journal of rehabilitation medicine. 2014 Nov 1;46(10):945-57.</ref> It is also known as toe walking, habitual toe walking, and congenital short tendo calcaneus.<ref name=":1">Le Cras S, Bouck J, Brausch S, Taylor-Haas A. [https://daniz53y71u1s.cloudfront.net/documents/idiopathic-toe-walking-pdf-new-9.pdf Evidence-based Clinical Care Guideline for Management of Idiopathic Toe Walking]. Cincinnati Children's Hospital Medical Center. Guideline 040, pages 1-17 (2011).</ref> | ||
In ITW, there is an absence of heel strike during initial contact and the foot does not make full contact during the stance phase of [[gait]]. Weight is kept primarily on the forefoot, often on the metatarsal heads.<ref name=":3" /> <ref name=":0">Dilger N. [https://footprintspediatrictherapy.com/wp-content/uploads/2015/01/Dilger_ITW.pdf Idiopathic Toe Walking: A diagnosis of Exclusion or a Developmental Marker]. Los Angeles, California. Footprints Pediatric Physical Therapy. 2005.</ref><blockquote>It can be defined as: “an equinus gait, initially without fixed contractures, with passive dorsiflexion range of motion (ROM) of the plantar flexor musculature to dorsiflex to at least neutral (0°) with the subtalar joint inverted and with the knee extended."<ref name=":0" /></blockquote>ITW may initially present during pre-walking skill acquisition, at the start of independent walking, or within 6 months of the initiation of independent walking.<ref name=":1" /> Some individuals will toe walk intermittently while others will toe walk exclusively.<ref name=":5">Eskay K. Idiopathic Toe Walking Course. Plus, 2023.</ref> | |||
Toe walking can occur in other conditions, including neurological conditions, myopathy, neuromuscular disorders, orthopaedic disorders, such as clubfoot, developmental delay, [[Autism Spectrum Disorder|autism spectrum disorder]] (ASD), etc.<ref name=":3" /><ref name=":0" /><ref>Donne JH, Powell JA, Fahey MC, Beare R, Kolic J, Williams CM. [https://onlinelibrary.wiley.com/doi/10.1111/apa.16821 Some children with idiopathic toe walking display sensory processing difficulties but not all: a systematic review]. Acta Paediatrica. 2023.</ref> These conditions are distinct from ITW.<ref name=":5" />{{#ev:youtube|L8__feVE3lI|300}}<ref>Paediatric Foot & Ankle. Toe Walking What Every Parent Should Know. Available from: https://www.youtube.com/watch?v=L8__feVE3lI [last accessed 25/04/2022]</ref> | |||
ITW | == Epidemiology and Aetiology == | ||
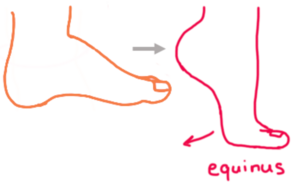
Reports of the incidence of ITW vary considerably, from to 2-5%<ref name=":1" /><ref name=":2">Lorentzen J, Willerslev‐Olsen M, Hüche Larsen H, Svane C, Forman C, Frisk R, Farmer SF, Kersting U, Nielsen JB. [https://physoc.onlinelibrary.wiley.com/doi/epdf/10.1113/JP275539 Feedforward neural control of toe walking in humans]. The Journal of physiology. 2018 Jun;596(11):2159-72.</ref> to 7-24%.<ref>[https://pubmed.ncbi.nlm.nih.gov/9009544/ Sobel] E, Caselli MA, Velez Z. Effect of persistent toe walking on ankle equinus. Analysis of 60 idiopathic toe walkers. Journal of the American Podiatric Medical Association. 1997 Jan;87(1):17-22.</ref> ITW affects boys more than girls.<ref>Caserta AJ, Pacey V, Fahey MC, Gray K, Engelbert RH, Williams CM. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6778693/ Interventions for idiopathic toe walking]. Cochrane Database of Systematic Reviews. 2019(10).</ref>[[File:Equinus illustration.png|thumb|Equinus foot/ Forefoot weight bearing]] | |||
The aetiology of ITW is unknown:<ref name=":6">Kononova S, Kashparov M, Xue W, Bobkova N, Leonov S, Zagorodny N. [https://www.mdpi.com/1422-0067/24/17/13204 Gut microbiome dysbiosis as a potential risk factor for idiopathic toe-walking in children: a review]. Int J Mol Sci. 2023 Aug 25;24(17):13204. </ref> | |||
ITW | * ITW is associated with ankle equinus.<ref>Caserta A, Morgan P, McKay MJ, Baldwin JN, Burns J, Williams C. [https://jfootankleres.biomedcentral.com/articles/10.1186/s13047-022-00576-x Children with idiopathic toe walking display differences in lower limb joint ranges and strength compared to peers: a case control study]. Journal of Foot and Ankle Research. 2022 Dec;15(1):1-8.</ref> Individuals with ITW often present with tightness or reduced range in their ankle plantar flexors, which develops over time with persistent toe walking. Ankle dorsiflexion range of motion also decreases with time.<ref name=":5" /> Reduced range of motion was initially thought to be a causal factor, but in more recent studies it is believed to occur as a ''result'' of ITW.<ref name=":3" /> | ||
* There may be a genetic component to ITW in some individuals<ref name=":6" /> - a strong family history is present in some children with ITW.<ref>Bauer JP, Sienko S, Davids JR. Idiopathic Toe Walking: [https://journals.lww.com/jaaos/fulltext/2022/11150/idiopathic_toe_walking__an_update_on_natural.7.aspx An Update on Natural History, Diagnosis, and Treatment.] Journal of the American Academy of Orthopaedic Surgeons. 2022 Nov 15;30(22):e1419-30.</ref> | |||
* There is a positive correlation between ITW and individuals who have language delays and learning disabilities.<ref name=":5" /> | |||
* There is an unconfirmed relationship between ITW and some sensory processing disorders<ref name=":5" /> (e.g. in children with tactile, proprioceptive, vestibular and visual processing issues<ref name=":6" />). | |||
** Please note, that the diagnosis of ITW does not apply to individuals who have autism spectrum disorder or developmental delay.<ref name=":5" /> | |||
* It has been suggested that ITW occurs due to hyperactive reflexes - i.e. a delay in maturation of the corticospinal tract results in a lack of inhibition of the stretch reflexes and subsequent increased deep tendon reflexes. A literature review performed by Lorentzen et al.<ref name=":2" /> found that corticospinal pathways are active and important at the level of the presynapse of motor neurons of the ankle plantar flexors. | |||
== Diagnosis == | == Diagnosis == | ||
Diagnosis is one of exclusion. | Diagnosis is one of exclusion. The following conditions must be ruled out in the differential diagnosis:<ref name=":3" /><ref name=":4">Caserta AJ, Pacey V, Fahey M, Gray K, Engelbert RH, Williams CM. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6778693/ Interventions for idiopathic toe walking]. Cochrane Database Syst Rev. 2019 Oct 6;10(10):CD012363. </ref> | ||
* Neuromotor disease | * Neuromotor disease | ||
* [[Congenital and Acquired Neuromuscular and Genetic Disorders|Neuromuscular disease]] | * [[Congenital and Acquired Neuromuscular and Genetic Disorders|Neuromuscular disease]] | ||
* [[Cerebral Palsy Introduction|Cerebral palsy]] | * [[Cerebral Palsy Introduction|Cerebral palsy]] | ||
* [[Spina Bifida]] | * [[Spina Bifida|Spina bifida]] | ||
* [[Tethered Cord Syndrome|Tethered cord syndrome]] | * [[Tethered Cord Syndrome|Tethered cord syndrome]] | ||
* [https://emedicine.medscape.com/article/413899-overview Spinal dysraphism] | * [https://emedicine.medscape.com/article/413899-overview Spinal dysraphism] | ||
| Line 50: | Line 34: | ||
[https:// | [https://www.sciencedirect.com/science/article/abs/pii/S0966636210002158 The Toe-walking tool] is a series of questions that has been proposed as a means to help distinguish ITW from other conditions. | ||
== Biomechanical Changes == | |||
As a child with ITW ages, certain biomechanical changes occur as a result of toe walking. | |||
* Shortened tendon achilles and contractures of the foot and ankle joints. This is more common in older children presenting with ITW.<ref name=":1" /><ref name=":3" /><ref name=":0" /> | |||
* Children with ITW develop foot pronation and, potentially, significant foot abduction (out-toeing). They may also have excessive tibial torsion.<ref name=":5" /> | |||
* Muscle biopsies indicate that children with ITW have a higher percentage of [[Muscle Fibre Types|type I muscle fibres]] in the gastrocnemius muscle rather than type II muscle fibres.<ref name=":0" /> <ref name=":2" /> | |||
== Management == | == Management == | ||
Initial management is conservative | Initial management for ITW is conservative. Surgical intervention is usually undertaken when conservative measures have been exhausted.<ref name=":1" /> <ref name=":3" /><ref name=":4" /><ref>Harkness-Armstrong, C., Maganaris, C., Walton, R., Wright, D.M., Bass, A., Baltzoloulos, V. and O’Brien, T.D., 2022. [https://link.springer.com/article/10.1007/s00421-022-04913-7 Children who idiopathically toe-walk have greater plantarflexor effective mechanical advantage compared to typically developing children]. ''European Journal of Applied Physiology'', ''122''(6), pp.1409-1417.</ref> | ||
=== Conservative management === | === Conservative management === | ||
| Line 62: | Line 50: | ||
* Serial casting | * Serial casting | ||
* [[Introduction to Orthotics]] | * [[Introduction to Orthotics|Orthotics]] or night splints | ||
* Footwear | * Footwear | ||
* Auditory feedback | * Auditory feedback | ||
* Physiotherapy | * Physiotherapy | ||
* | * Botulinum toxin type A (BTX) | ||
== Physiotherapy management == | === Physiotherapy management === | ||
As with all therapeutic interventions, initial | As with all therapeutic interventions, the initial consultation begins with a thorough assessment, followed by treatment and reassessment. | ||
=== Assessment === | === Assessment === | ||
Components of a | Components of a physiotherapy examination are detailed in the Cincinnati Children’s Hospital Medical Centre’s Guideline in the Management of Idiopathic Toe Walking.<ref name=":1" /> It includes the following: | ||
* Subjective examination | * Subjective examination | ||
| Line 91: | Line 67: | ||
* Gait examination | * Gait examination | ||
* Gross motor skills | * Gross motor skills | ||
For more information, please see: [https://daniz53y71u1s.cloudfront.net/documents/idiopathic-toe-walking-pdf-new-9.pdf Evidence-based Clinical Care Guideline for Management of Idiopathic Toe Walking].<ref name=":1" /> | |||
==== Subjective examination ==== | ==== Subjective examination ==== | ||
| Line 96: | Line 73: | ||
* Birth history | * Birth history | ||
* Medical history | * Medical history | ||
* Developmental history: | * Developmental history, including: | ||
* [[Child Development|Gross motor skills development]] | ** [[Child Development|Gross motor skills development]] | ||
* Balance concerns | ** Balance concerns | ||
* Onset of toe walking | ** Onset of toe walking | ||
* Family history of toe walking, and/or any conditions associated with toe walking | * Family history of toe walking, and/or any conditions associated with toe walking | ||
* Current and past therapeutic interventions | * Current and past therapeutic interventions, such as, occupational therapy, physiotherapy, speech therapy etc.<ref name=":1" /> | ||
==== Objective screening ==== | ==== Objective screening ==== | ||
* Pain assessment using an appropriate pain scale | * Pain assessment using an appropriate pain scale | ||
* Speech and language screening | * Speech and language screening | ||
* Short [https://www.makingstridesofvirginia.org/wp-content/uploads/2018/12/Child-Sensory-Profile001-Age-4-thru-14.pdf Sensory Profile] (for ages 3 years to 10 years 11 months) | ** Use the communication subsection of the Ages and Stages Questionnaire for ages 4 months to 60 months, if indicated | ||
* Complete the Short [https://www.makingstridesofvirginia.org/wp-content/uploads/2018/12/Child-Sensory-Profile001-Age-4-thru-14.pdf Sensory Profile] (for ages 3 years to 10 years 11 months) by the first treatment visit as a sensory processing screen<ref name=":1" /> | |||
==== Physical examination ==== | ==== Physical examination ==== | ||
* | * The neurological assessment should include: | ||
* [[Clonus of the Ankle Test| | ** Assessing for muscle tone of ankle plantar flexors and knee flexors using the [[Modified Ashworth Scale]] | ||
* | ** Assessing for [[Clonus of the Ankle Test|clonus]] | ||
* | * The musculoskeletal examination should include: | ||
* Muscle length | ** Range of motion (ROM) testing: | ||
** [[Thomas Test|Thomas test]] (hip flexors) | *** Passive ROM of ankle dorsiflexion in subtalar neutral (STN), with knee, flexed and extended | ||
** Hamstring length test. | *** Active ROM of ankle dorsiflexion with knee extended | ||
** Lower extremity | ** Muscle length testing, including: | ||
** Thigh foot angle | *** [[Thomas Test|Thomas test]] (hip flexors) | ||
** Hindfoot/forefoot alignment in | *** Hamstring length test. Hamstring length varies based on age. [https://pubmed.ncbi.nlm.nih.gov/8989707/#:~:text=The%20straight%20leg%2Draise%20test,children%20younger%20than%202%20years. The hamstring index] summarises these length changes. | ||
* Standing posture | ** Lower extremity alignment, including: | ||
* | *** Thigh foot angle | ||
** Anterior tibialis | *** Hindfoot/forefoot alignment in subtalar neutral (in non-weight bearing) | ||
** Gastrocnemius | ** Standing posture | ||
* | ** Strength of the following muscles using manual muscle testing and/or functional assessments: | ||
*** Anterior tibialis | |||
*** Gastrocnemius | |||
** Assess trunk and core<ref name=":1" /> | |||
* Gait examination: | |||
** Observational Gait Scale | |||
** Parent report of percentage of time toe walking<ref name=":1" /> | |||
*Gross motor skills assessment, including: | |||
**Squatting to/from standing position, position of foot squatting | |||
**Transitioning from floor to stand | |||
** Stairs | |||
** Balance, including: | |||
*** Static and dynamic balance | |||
*** Single limb stance | |||
*** Balance beam | |||
*** Jumping and hopping | |||
** Coordination | |||
** Determine the need for standardised testing<ref name=":1" /> | |||
Further details in progressive reassessment during follow-up consultation can be found in the [https://daniz53y71u1s.cloudfront.net/documents/idiopathic-toe-walking-pdf-new-9.pdf Cincinnati Children’s Hospital Medical Centre’s Guideline.]{{#ev:youtube|BIUrcHDLD1M|}}<ref>AMy Sturkey. #5 A Comparison of Walking in Typical vs Toe Walkers: Pediatric Physical Therapy for Toe Walkers. Available from:https://www.youtube.com/watch?v=BIUrcHDLD1M [last accessed 26/04/2022</ref> | |||
=== | === Physiotherapy intervention === | ||
A physiotherapist's role in the management of ITW is multidimensional and includes the following<ref name=":0" />. | |||
* Hands-on therapy | |||
** Active and passive range exercises, with an emphasis on ankles range of motion and ensuring that exercises are performed in subtalar neutral | |||
** Strength training, partiuclarly anterior tibialis and the trunk muscles | |||
** Gait training, including treadmill training | |||
** Kinesiotaping along tibialis anterior | |||
** Home exercise programme prescription | |||
* | * In addition to the above, the physiotherapist will also be involved in footwear, casting and orthotic intervention. | ||
=== | === Surgical management === | ||
Surgical interventions described in the literature include: | |||
* | * [https://www.researchgate.net/figure/Diagrams-of-other-techniques-of-aponeurotic-lengthening-showing-a-Vulpius-b-Baker-and_fig3_12462539 Vulpius procedure] (gastrocnemius recession surgery)<ref name=":3" /><ref name=":4" /> | ||
* [[Achilles Tendon|Tendon achilles]] lengthening<ref name=":3" /><ref name=":4" /> | |||
* Open achilles tendon lengthening via a Z-lengthening or slide technique<ref name=":4" /> | |||
* Baker’s gastrocnemius-soleus lengthening<ref name=":4" /> | |||
Side effects to surgical management noted in Caserta et al.<ref name=":4" /> and Van Kuijk et al.<ref name=":3" /> included excessive ankle dorsiflexion after tendon achilles lengthening. | |||
== Additional Viewing == | == Additional Viewing == | ||
Revision as of 05:09, 11 September 2023
Introduction[edit | edit source]
Idiopathic toe walking (ITW) is a diagnostic term used to describe a condition in otherwise healthy, ambulant children who present with a toe-toe gait. It is a diagnosis of exclusion, where no determinable pathology exists.[1] It is also known as toe walking, habitual toe walking, and congenital short tendo calcaneus.[2]
In ITW, there is an absence of heel strike during initial contact and the foot does not make full contact during the stance phase of gait. Weight is kept primarily on the forefoot, often on the metatarsal heads.[1] [3]
It can be defined as: “an equinus gait, initially without fixed contractures, with passive dorsiflexion range of motion (ROM) of the plantar flexor musculature to dorsiflex to at least neutral (0°) with the subtalar joint inverted and with the knee extended."[3]
ITW may initially present during pre-walking skill acquisition, at the start of independent walking, or within 6 months of the initiation of independent walking.[2] Some individuals will toe walk intermittently while others will toe walk exclusively.[4] Toe walking can occur in other conditions, including neurological conditions, myopathy, neuromuscular disorders, orthopaedic disorders, such as clubfoot, developmental delay, autism spectrum disorder (ASD), etc.[1][3][5] These conditions are distinct from ITW.[4]
Epidemiology and Aetiology[edit | edit source]
Reports of the incidence of ITW vary considerably, from to 2-5%[2][7] to 7-24%.[8] ITW affects boys more than girls.[9]
The aetiology of ITW is unknown:[10]
- ITW is associated with ankle equinus.[11] Individuals with ITW often present with tightness or reduced range in their ankle plantar flexors, which develops over time with persistent toe walking. Ankle dorsiflexion range of motion also decreases with time.[4] Reduced range of motion was initially thought to be a causal factor, but in more recent studies it is believed to occur as a result of ITW.[1]
- There may be a genetic component to ITW in some individuals[10] - a strong family history is present in some children with ITW.[12]
- There is a positive correlation between ITW and individuals who have language delays and learning disabilities.[4]
- There is an unconfirmed relationship between ITW and some sensory processing disorders[4] (e.g. in children with tactile, proprioceptive, vestibular and visual processing issues[10]).
- Please note, that the diagnosis of ITW does not apply to individuals who have autism spectrum disorder or developmental delay.[4]
- It has been suggested that ITW occurs due to hyperactive reflexes - i.e. a delay in maturation of the corticospinal tract results in a lack of inhibition of the stretch reflexes and subsequent increased deep tendon reflexes. A literature review performed by Lorentzen et al.[7] found that corticospinal pathways are active and important at the level of the presynapse of motor neurons of the ankle plantar flexors.
Diagnosis[edit | edit source]
Diagnosis is one of exclusion. The following conditions must be ruled out in the differential diagnosis:[1][13]
- Neuromotor disease
- Neuromuscular disease
- Cerebral palsy
- Spina bifida
- Tethered cord syndrome
- Spinal dysraphism
- Spinal cord tumor
The Toe-walking tool is a series of questions that has been proposed as a means to help distinguish ITW from other conditions.
Biomechanical Changes[edit | edit source]
As a child with ITW ages, certain biomechanical changes occur as a result of toe walking.
- Shortened tendon achilles and contractures of the foot and ankle joints. This is more common in older children presenting with ITW.[2][1][3]
- Children with ITW develop foot pronation and, potentially, significant foot abduction (out-toeing). They may also have excessive tibial torsion.[4]
- Muscle biopsies indicate that children with ITW have a higher percentage of type I muscle fibres in the gastrocnemius muscle rather than type II muscle fibres.[3] [7]
Management[edit | edit source]
Initial management for ITW is conservative. Surgical intervention is usually undertaken when conservative measures have been exhausted.[2] [1][13][14]
Conservative management[edit | edit source]
Conservative treatment can include the following[13]:
- Serial casting
- Orthotics or night splints
- Footwear
- Auditory feedback
- Physiotherapy
- Botulinum toxin type A (BTX)
Physiotherapy management[edit | edit source]
As with all therapeutic interventions, the initial consultation begins with a thorough assessment, followed by treatment and reassessment.
Assessment[edit | edit source]
Components of a physiotherapy examination are detailed in the Cincinnati Children’s Hospital Medical Centre’s Guideline in the Management of Idiopathic Toe Walking.[2] It includes the following:
- Subjective examination
- Objective examination, including certain screenings
- Physical examination
- Gait examination
- Gross motor skills
For more information, please see: Evidence-based Clinical Care Guideline for Management of Idiopathic Toe Walking.[2]
Subjective examination[edit | edit source]
- Birth history
- Medical history
- Developmental history, including:
- Gross motor skills development
- Balance concerns
- Onset of toe walking
- Family history of toe walking, and/or any conditions associated with toe walking
- Current and past therapeutic interventions, such as, occupational therapy, physiotherapy, speech therapy etc.[2]
Objective screening[edit | edit source]
- Pain assessment using an appropriate pain scale
- Speech and language screening
- Use the communication subsection of the Ages and Stages Questionnaire for ages 4 months to 60 months, if indicated
- Complete the Short Sensory Profile (for ages 3 years to 10 years 11 months) by the first treatment visit as a sensory processing screen[2]
Physical examination[edit | edit source]
- The neurological assessment should include:
- Assessing for muscle tone of ankle plantar flexors and knee flexors using the Modified Ashworth Scale
- Assessing for clonus
- The musculoskeletal examination should include:
- Range of motion (ROM) testing:
- Passive ROM of ankle dorsiflexion in subtalar neutral (STN), with knee, flexed and extended
- Active ROM of ankle dorsiflexion with knee extended
- Muscle length testing, including:
- Thomas test (hip flexors)
- Hamstring length test. Hamstring length varies based on age. The hamstring index summarises these length changes.
- Lower extremity alignment, including:
- Thigh foot angle
- Hindfoot/forefoot alignment in subtalar neutral (in non-weight bearing)
- Standing posture
- Strength of the following muscles using manual muscle testing and/or functional assessments:
- Anterior tibialis
- Gastrocnemius
- Assess trunk and core[2]
- Range of motion (ROM) testing:
- Gait examination:
- Observational Gait Scale
- Parent report of percentage of time toe walking[2]
- Gross motor skills assessment, including:
- Squatting to/from standing position, position of foot squatting
- Transitioning from floor to stand
- Stairs
- Balance, including:
- Static and dynamic balance
- Single limb stance
- Balance beam
- Jumping and hopping
- Coordination
- Determine the need for standardised testing[2]
Further details in progressive reassessment during follow-up consultation can be found in the Cincinnati Children’s Hospital Medical Centre’s Guideline.
Physiotherapy intervention[edit | edit source]
A physiotherapist's role in the management of ITW is multidimensional and includes the following[3].
- Hands-on therapy
- Active and passive range exercises, with an emphasis on ankles range of motion and ensuring that exercises are performed in subtalar neutral
- Strength training, partiuclarly anterior tibialis and the trunk muscles
- Gait training, including treadmill training
- Kinesiotaping along tibialis anterior
- Home exercise programme prescription
- In addition to the above, the physiotherapist will also be involved in footwear, casting and orthotic intervention.
Surgical management[edit | edit source]
Surgical interventions described in the literature include:
- Vulpius procedure (gastrocnemius recession surgery)[1][13]
- Tendon achilles lengthening[1][13]
- Open achilles tendon lengthening via a Z-lengthening or slide technique[13]
- Baker’s gastrocnemius-soleus lengthening[13]
Side effects to surgical management noted in Caserta et al.[13] and Van Kuijk et al.[1] included excessive ankle dorsiflexion after tendon achilles lengthening.
Additional Viewing[edit | edit source]
Resources[edit | edit source]
Liesa Ritchie-Persaud's Top Tips and Tools for Treating Toe-Walking: https://www.wiredondevelopment.com/single-post/2017/02/17/liesa-persauds-top-tips-and-tools-for-treating-toe-walking
Dr Cylie Williams: A Podiatrist's Perspective on paediatric feet and gait concerns:https://www.wiredondevelopment.com/single-post/2018/04/22/dr-cylie-williams-a-podiatrists-perspective-on-paediatric-feet-and-gait-concerns
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 1.9 Van Kuijk AA, Kosters R, Vugts M, Geurts AC. Treatment for idiopathic toe walking: a systematic review of the literature. Journal of rehabilitation medicine. 2014 Nov 1;46(10):945-57.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 Le Cras S, Bouck J, Brausch S, Taylor-Haas A. Evidence-based Clinical Care Guideline for Management of Idiopathic Toe Walking. Cincinnati Children's Hospital Medical Center. Guideline 040, pages 1-17 (2011).
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 Dilger N. Idiopathic Toe Walking: A diagnosis of Exclusion or a Developmental Marker. Los Angeles, California. Footprints Pediatric Physical Therapy. 2005.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 Eskay K. Idiopathic Toe Walking Course. Plus, 2023.
- ↑ Donne JH, Powell JA, Fahey MC, Beare R, Kolic J, Williams CM. Some children with idiopathic toe walking display sensory processing difficulties but not all: a systematic review. Acta Paediatrica. 2023.
- ↑ Paediatric Foot & Ankle. Toe Walking What Every Parent Should Know. Available from: https://www.youtube.com/watch?v=L8__feVE3lI [last accessed 25/04/2022]
- ↑ 7.0 7.1 7.2 Lorentzen J, Willerslev‐Olsen M, Hüche Larsen H, Svane C, Forman C, Frisk R, Farmer SF, Kersting U, Nielsen JB. Feedforward neural control of toe walking in humans. The Journal of physiology. 2018 Jun;596(11):2159-72.
- ↑ Sobel E, Caselli MA, Velez Z. Effect of persistent toe walking on ankle equinus. Analysis of 60 idiopathic toe walkers. Journal of the American Podiatric Medical Association. 1997 Jan;87(1):17-22.
- ↑ Caserta AJ, Pacey V, Fahey MC, Gray K, Engelbert RH, Williams CM. Interventions for idiopathic toe walking. Cochrane Database of Systematic Reviews. 2019(10).
- ↑ 10.0 10.1 10.2 Kononova S, Kashparov M, Xue W, Bobkova N, Leonov S, Zagorodny N. Gut microbiome dysbiosis as a potential risk factor for idiopathic toe-walking in children: a review. Int J Mol Sci. 2023 Aug 25;24(17):13204.
- ↑ Caserta A, Morgan P, McKay MJ, Baldwin JN, Burns J, Williams C. Children with idiopathic toe walking display differences in lower limb joint ranges and strength compared to peers: a case control study. Journal of Foot and Ankle Research. 2022 Dec;15(1):1-8.
- ↑ Bauer JP, Sienko S, Davids JR. Idiopathic Toe Walking: An Update on Natural History, Diagnosis, and Treatment. Journal of the American Academy of Orthopaedic Surgeons. 2022 Nov 15;30(22):e1419-30.
- ↑ 13.0 13.1 13.2 13.3 13.4 13.5 13.6 13.7 Caserta AJ, Pacey V, Fahey M, Gray K, Engelbert RH, Williams CM. Interventions for idiopathic toe walking. Cochrane Database Syst Rev. 2019 Oct 6;10(10):CD012363.
- ↑ Harkness-Armstrong, C., Maganaris, C., Walton, R., Wright, D.M., Bass, A., Baltzoloulos, V. and O’Brien, T.D., 2022. Children who idiopathically toe-walk have greater plantarflexor effective mechanical advantage compared to typically developing children. European Journal of Applied Physiology, 122(6), pp.1409-1417.
- ↑ AMy Sturkey. #5 A Comparison of Walking in Typical vs Toe Walkers: Pediatric Physical Therapy for Toe Walkers. Available from:https://www.youtube.com/watch?v=BIUrcHDLD1M [last accessed 26/04/2022
- ↑ Liesa Persaud. Toe Walking Video: Base of Support - MedBridge. Available from:https://www.youtube.com/watch?v=BYYFSSIB5h8 [last accessed 26/04/2022]