Gait
Introduction[edit | edit source]
Human gait depends on a complex interplay of major parts of the nervous, musculoskeletal and cardiorespiratory systems.
- The individual gait pattern is influenced by age, personality, mood and sociocultural factors.
- The preferred walking speed in older adults is a sensitive marker of general health and survival.
- Safe walking requires intact cognition and executive control.
- Gait disorders lead to a loss of personal freedom, falls and injuries and result in a marked reduction in the quality of life[1].
Definitions[edit | edit source]
- Gait - the manner or style of walking.
- Gait Analysis - An analysis of each component of the three phases of ambulation is an essential part of the diagnosis of various neurologic disorders and the assessment of patient progress during rehabilitation and recovery from the effects of neurologic disease, a musculoskeletal injury or disease process, or amputation of a lower limb.
- Gait speed
- The time it takes to walk a specified distance, usually 6 m or less. Slower speeds correlate with an increased risk of mortality in geriatric patients.[2]
- Normal walking speed primarily involves the lower extremities, with the arms and trunk providing stability and balance.
- Faster speeds - body depends on the upper extremities and trunk for propulsion, balance and stability with the lower limb joints producing greater ranges of motion.[3]
- Gait cycle is a repetitive pattern involving steps and strides[4]
- Step is one single step
- Stride is a whole gait cycle.
- Step time - time between heel strike of one leg and heel strike of the contralateral leg[4].
- Step width - the mediolateral space between the two feet[4].
The demarcation between walking and running occurs when periods of double support during the stance phase of the gait cycle (both feet are simultaneously in contact with the ground) give way to two periods of double float at the beginning and the end of the swing phase of gait (neither foot is touching the ground)[5].
The Gait Cycle[edit | edit source]
The sequences for walking that occur may be summarised as follows:[6]
- Registration and activation of the gait command within the central nervous system.
- Transmission of the gait systems to the peripheral nervous system.
- Contraction of muscles.
- Generation of several forces.
- Regulation of joint forces and moments across synovial joints and skeletal segments.
- Generation of ground reaction forces.
The normal forward step consists of two phases: stance phase; swing phase,
- The Stance phase occupies 60% of the gait cycle, during which one leg and foot are bearing most or all of the bodyweight
- The Swing phase occupies only 40% of it[4], during which the foot is not touching the walking surface and the bodyweight is borne by the other leg and foot.
- In a complete two-step cycle both feet are in contact with the floor at the same time for about 25 per cent of the time. This part of the cycle is called the double-support phase.Gait cycle phases: the stance phase and the swing phase and involves a combination of open and close chain activities.[3]
The 90 second video below gives the basics of this cycle
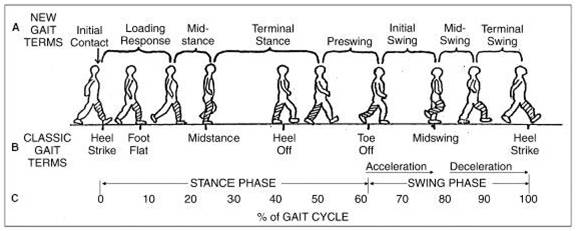
Phases of the Gait Cycle (8 phase model):[4][8][edit | edit source]
- Initial Contact
- Loading Response
- Midstance
- Terminal Stance
- Pre swing
- Initial Swing
- Mid Swing
- Late Swing.[9]
Heel Strike (or initial contact) -
Short period, begins the moment the foot touches the ground and is the first phase of double support.[3]
Involves:
- 30° flexion of the hip: full extension in the knee: ankle moves from dorsiflexion to a neutral (supinated 5°) position then into plantar flexion.[3][4]
- After this, knee flexion (5°) begins and increases, just as the plantar flexion of the heel increased.[4]
- Plantar flexion is allowed by eccentric contraction of the tibialis anterior
- Extension of the knee is caused by a contraction of the quadriceps
- Flexion is caused by a contraction of the hamstrings,
- Flexion of the hip is caused by the contraction of the rectus femoris.[4]
Foot Flat (or loading response phase)
- Body absorbs the impact of the foot by rolling in pronation.[3]
- Hip moves slowly into extension, caused by a contraction of the adductor magnus and gluteus maximus muscles.
- Knee flexes to 15° to 20° of flexion. [4]
- Ankle plantarflexion increases to 10-15°.[3][4]
Midstance
- Hip moves from 10° of flexion to extension by contraction of the gluteus medius muscle.[4]
- Knee reaches maximal flexion and then begins to extend.
- Ankle becomes supinated[3] and dorsiflexed (5°), which is caused by some contraction of the triceps surae muscles.[3]
- During this phase, the body is supported by one single leg.
- At this moment the body begins to move from force absorption at impact to force propulsion forward.[3]
Heel Off
- Begins when the heel leaves the floor.
- Bodyweight is divided over the metatarsal heads.[3]
- 10-13° of hip hyperextension, which then goes into flexion.
- Knee becomes flexed (0-5°)[4]
- Ankle supinates and plantar flexes.[4]
Toe Off/pre-swing
- Hip becomes less extended.
- Knee is flexed 35-40°
- Plantar flexion of the ankle increases to 20°.[3][4]
- The toes leave the ground.[4]
Early Swing
- Hip extends to 10° and then flexes due to contraction of the iliopsoas muscle[4] 20° with lateral rotation.[3][4]
- Knee flexes to 40-60°
- Ankle goes from 20° of plantar flexion to dorsiflexion, to end in a neutral position.[3]
Mid Swing
- Hip flexes to 30° (by contraction of the adductors) and the ankle becomes dorsiflexed due to a contraction of the tibialis anterior muscle.[4]
- Knee flexes 60° but then extends approximately 30° due to the contraction of the sartorius muscle.[3][4](caused by the quadriceps muscles).[3][4]
Late Swing/declaration
- Hip flexion of 25-30°
- Locked extension of the knee
- Neutral position of the ankle.[3]
Range of Motion during Gait
Ground Reaction Force during Gait
Muscular Activity during Gait
Gait Cycle - Anatomical Considerations[edit | edit source]
- Pelvic region - anterior-posterior displacement, which alternates from left to right. Facilitates anterior movement of the leg (each side anterior-posterior displacement of 4-5°).[3][4][8]
- Frontal plane - varus movement in the: foot between heel-strike and foot-flat and between heel-off and toe-off; hip, in lateral movements (when the abductors are too weak, aTrendelenburg gaitcan be observed).[3][8] Valgus movement between foot-flat and heel off in the feet.
- A disorder in any segment of the body can have consequences on the individual's gait pattern.[13][14]
Gait Disorders[edit | edit source]
Gait disorders - altered gait pattern due to deformities, weakness or other impairments eg loss of motor control or pain[15].
Prevalence increases with age and the number of people affected will substantially increase in the coming decades due to the expected demographic changes.
- Lead to a loss of personal freedom and to reduced quality of life.
- Precursors of falls and therefore of potentially severe injuries in elderly persons[1].
Gait Descriptions[edit | edit source]
This is not an exhaustive list.
- Antalgic gait a limp adopted so as to avoid pain on weight-bearing structures, characterized by a very short stance phase.
- Ataxic gait an unsteady, uncoordinated walk, with a wide base and the feet thrown out, coming down first on the heel and then on the toes with a double tap.This gait is associated with cerebellar disturbances and can be seen in patients with longstanding alcohol dependency. People with 'Sensory'Disturbances may present with a sensory ataxic gait. Presentation is a wide base of support, high steps, and slapping of feet on the floor in order to gain some sensory feedback. They may also need to rely on observation of foot placement and will often look at the floor during mobility due to a lack of proprioception.
- Equine gait a walk accomplished mainly by flexing the hip joint; seen in crossed leg palsy.
- Parkinsonian Gait (seen in parkinson's disease and other neurologic conditions that affect the basal ganglia). Rigidity of joints results in reduced arm swing for balance. A stooped posture and flexed knees are a common presentation. Bradykinesia causes small steps that are shuffling in presentation. There may be occurrences of freezing or short rapid bursts of steps known as ‘festination’ and turning can be difficult.[16]
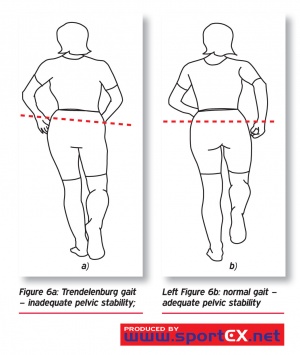
- Trendelenburg gait, the gait characteristic of paralysis of the gluteus medius muscle, marked by a listing of the trunk toward the affected side at each step.
- Hemiplegic gait a gait involving flexion of the hip because of foot-drop[17] and circumduction of the leg.
- Steppage gait the gait in foot-drop in which the advancing leg is lifted high in order that the toes may clear the ground. It is due to paralysis of the anterior tibial and fibular muscles, and is seen in lesions of the lower motor neuron, such as multiple neuritis, lesions of the anterior motor horn cells, and lesions of the cauda equina.
- Stuttering gait a walking disorder characterized by hesitancy that resembles stuttering; seen in some hysterical or schizophrenic patients as well as in patients with neurologic damage.
- Tabetic gait an ataxic gait in which the feet slap the ground; in daylight the patient can avoid some unsteadiness by watching his feet.
- Waddling gait exaggerated alternation of lateral trunk movements with an exaggerated elevation of the hip, suggesting the gait of a duck; characteristic of muscular dystrophy.
- Diplegic Gait (Spastic gait). Spasticity is normally associated with both lower limbs. Contractures of the adductor muscles can create a ‘scissor’ type gait with a narrowed base of support. Spasticity in the lower half of the legs results in plantarflexed ankles presenting in ‘tiptoe’ walking and often toe dragging. Excessive hip and knee flexion is required to overcome this
- Neuropathic Gaits. High stepping gait to gain floor clearance often due to foot drop[13][15][18][2]
Causes of gait disorders[edit | edit source]
They include neurological, orthopedic, medical and psychiatric conditions and multifactorial etiology becomes more common with advancing age, making classification and management more complex. Any gait disorder should be thoroughly investigated in order to improve patient mobility and independence, to prevent falls and to detect the underlying causes as early as possible. Thorough clinical observation of gait, careful history taking focussed on gait and falls and physical, neurological and orthopedic examinations are basic steps in the categorization of gait disorders and serve as a guide for ancillary investigations and therapeutic interventions.
Musculoskeletal Causes[edit | edit source]
Pathological gait patterns resulting from musculoskeletal are often caused by soft tissue imbalance, joint alignment or bony abnormalities affect the gait pattern as a result[15].
Hip Pathology[edit | edit source]
- Arthritis is a common cause of pathological gait. An arthritic hip has reduced range of movement during swing phase which causes an exaggeration of movement in the opposite limb ‘hip hiking[15][20].
- Excessive Hip Flexion can significantly alter gait pattern most commonly due to; • Hip flexion contractures • IT band contractures, • Hip flexor spasticity, • Compensation for excessive knee flexion and ankle DF, • Hip pain • Compensation for excess ankle plantar flexion in mid swing. The deviation of stance phase will occur mainly on the affected side. The result is forward tilt of the trunk and increased demand on the hip extensors or increased lordosis of the spine with anterior pelvic tilt. A person with reduced spinal mobility will adopt a forward flexion position in order to alter their centre of gravity permanently during gait.
- Hip Abductor Weakness. The abductor muscles stabilise the pelvis to allow the opposite leg to lift during the swing phase. Weak abductor muscles will cause the hip to drop towards the side of the leg swinging forward. This is also known as Trendelenburg gait[18]
- Hip Adductor Contracture. During swing phase the leg crosses midline due to the weak adductor muscles, this is known as ‘scissor gait’[18]
- Weak Hip Extensors will cause a person to take a smaller step to lessen the hip flexion required for initial contact, resulting in a lesser force of contraction required from the extensors. Overall gait will be slower to allow time for limb stabilisation. Compensation is increased posterior trunk positioning to maintain alignment of the pelvis in relation to the trunk[18]
- Hip Flexor Weakness results in a smaller step length due to the weakness of the muscle to create the forward motion. Gait will likely be slower and may result in decreased floor clearance of the toes and create a drag
Knee Pathologies[edit | edit source]
- Weak Quadriceps. The quadriceps role is to eccentrically control the knee during flexion through the stance phase. If these muscles are weak the hip extensors will compensate by bringing the limb back into a more extended position, reducing the amount of flexion at the knee during stance phase. Alternatively heel strike will occur earlier increasing the ankle of plantar flexion at the ankle, preventing the forward movement of the tibia, to help stabilise the knee joint[18].
- Severe Quadriceps Weakness or instability at the knee joint will present in hyperextension during the initial contact to stance phase. The knee joint will ‘snap’ back into hyperextension as the bodyweight moves forwards over the limb[18]
- Knee Flexion Contraction will cause a limping type gait pattern. The knee is restricted in extension, meaning heel strike is limited and step length reduced. To compensate the person is likely to ‘toe walk’ during stance phase. Knee flexion contractures of more than 30 degrees will be obvious during normal paced gait. Contractures less then this will be more evident with increased speeds[15][18].
Ankle Pathologies[edit | edit source]
- Ankle Dorsiflexion Weakness results in a lack of heel strike and decreased floor clearance. This leads to an increased step height and prolonged swing phase[18].
- Calf Tightening or Contractures due to a period of immobilisation or trauma will cause reduced heel strike due to restricted dorsiflexion. The compensated gait result will be ‘toe walking’ on stance phase, reduced step length, and excessive knee and hip flexion during swing phase to ensure floor clearance[15].
Foot Pathologies[edit | edit source]
- Hallux Rigidus results in a lack of dorsiflexion of the great toe. The MPJ uses the windlass effect to raise the arch and stiffen the foot during dorsiflexion of the hallux. This stiffness increases the efficiency of the propulsion portion of the gait cycle. To be efficient in creating stiffness, the hallux should be able to dorsiflex at least 65 degrees.
Leg length discrepancy[edit | edit source]
Leg length discrepancy can be as a result of an asymmetrical pelvic, tibia, or femur length or for other reasons such as scoliosis or contractures. The gait pattern will present as a pelvic dip to the shortened side during the stance phase with possible ‘toe walking’ on that limb. The opposite leg is likely to increase its knee and hip flexion to reduce its length[15].
Antalgic Gait[edit | edit source]
- Antalgic gait due to knee pain presents with decreased weight bearing on the affected side. The knee remains in flexion and possible toe weight-bearing occurs during stance phase[15]
- Antalgic gait due to ankle pain may present with a reduced stride length and decreased weight bearing on the affected limb. If the problem is pain in the forefoot then toe-off will be avoided and heel weight-bearing used. If the pain is more in the heel, toe weight-bearing is more likely. General ankle pain may result in weight-bearing on the lateral border[15][18].
- Antalgic gait due to hip pain results in a reduced stance phase on that side. The trunk is propelled quickly forwards with the opposite shoulder lifted in an attempt to even the weight distribution over the limb and reduce weight-bearing. Swing phase is also reduced[15].
Summary of Gait Deviations[edit | edit source]
| Observed Gait Deviation | Likely Impairement | Compensation/Mechanical Rationale |
| Hip | ||
| Backward leaning of the trunk during loading phase | Weak Hip Extensors | The line of gravity of the trunk moves behind the hips thereby reducing the need for hip extension torque |
| Forward bending of the trunk during loading response | Weak Quadriceps | The trunk is moved forward to bring the line of gravity anterior to the axis of rotation of the knee and reducing the need for knee extensors |
| Lateral trunk lean towards the stance (Compensated Trendelenburg Gait) | Marked weakness of the hip abductors
Hip pain |
Shifting of the trunk over the unaffected lower extremity reduces the demand of the hip abductors |
| Hip Circumduction
(semicircle movement of the hip during swing phase) |
Hip flexor weakness | Semicircle movement includes the combination movement of hip flexion, hip abduction and forward rotation of the pelvis |
| Knee | ||
| Flexed position of the knee during stance despite normal range of motion at the knee joint | Impairement at the ankle or the hip joint
(Compensation occurring at the knee joint) |
Exaggerated hip flexion or ankle dorsiflexion during stance results in flexion of the knee |
| Excessive knee flexion during swing phase | Reduced ankle dorsiflexion of the swing limb | Increase toe clearance of the swing limb.
(This is accompanied with increased hip flexion) |
| Knee is kept in extension during loading phase
(No extension thrust is observed) |
Weak quadriceps | Anterior trunk lean is observed during early stance, thereby moving the line of gravity of the trunk slightly anterior to the axis of rotation |
| Reduced knee flexion during swing phase | Knee extension contracture | Hip hiking or hip circumduction will be observed as compensation |
| Ankle | ||
| Foot slap
Quick ankle plantar flexion occurring after heel contact |
Weakness in ankle dorsiflexors | None/less active dorsiflexion occurs during swing phase
Normal dorsiflexion can occur during stance phase (if there is normal range of motion at the ankle joint) |
| Drop Foot
Ankle remains in plantar flexion during swing phase |
Weakness in ankle dorsiflexors | To prevent toes from dragging during the swing phase hip circumduction, hip hiking or exaggerated hip and knee flexion will be noted |
Below are links to videos demonstrating normal gait and various gait abnormalities:
| [22] | [23] |
Age-Related Gait Changes[edit | edit source]
Ageing is marked with cognitive decline, reduction in joint motion due to osteopenia and osteoporosis.[24] And most especially plantar flexors loss that reduce stance phase in this population with reduction in acuity for auditory, vestibular, visual and somatosensory system.[25] [26] This factors interplay to results in increase in prevalence of gait disorders among older adults.
Also, any threat to balance induces changes in the strategies for standing and walking - the stance and gait base is widened, bipedal floor contact is prolonged, step length becomes shorter, the feet are lifted less high during the swing phase, walking becomes slower and the posture becomes stooped.
- The fear of falling and the actual risk of falling increase with age.
- Older persons are therefore more likely to use these protective gait strategies.
- As muscle power diminishes and proprioception and vision become impaired with age,
- body sway on standing, which is constantly present to a slight degree, increases.
- In younger persons this sway can be compensated by activating the muscle groups around the upper ankle joints. Older persons shift this compensation to the proximal muscle groups around the hips due to loss of distal proprioception.
- This requires an increased reliance on vestibular afferent, which undergo less change during the ageing process.
- The preferred walking speed in apparently healthy elderly subjects declines by 1 % per year from a mean of 1.3 m/s in the seventh decade to a mean of 0.95 m/s in those aged over 80 years (caused by a decrease in step length rather than by a change in cadence).
- Gait changes are to some degree a consequence of normal ageing however individual walking speed in elderly subjects is a strong indicator of general health and survival[1]
Some specific changes observed in elements of gait as affected in older adults are not limited to:
- reduction in gait velocity (speed of walking) due to shorter steps but at the same rate (cadence).
- And increase in time spent in double stance phase
Because of multi-decline in body physiological functions and prevalent of multi-morbidity among this population it is not uncommon to have mixtures of neurological and musculoskeletal related gait disorders in this population.[27] Common gait disorders in older adults under neurological causes are sensory ataxia, Parkinsonism & frontal gait disorders. While non-neurological ( includes hip and knee osteoarthritis.[28]
Gait Analysis[edit | edit source]
- The analysis of the gait cycle is important in the biomechanical mobility examination to gain information about lower limb dysfunction in dynamic movement and loading.[29]
- When analyzing the gait cycle, it is best to examine one joint at a time.[3]
- Objective and subjective methods can be used.[30][31]
Subjective
- Different gait patterns - We might ask the individual to walk normally, on insides and outsides of feet, in a straight line, running (all the time looking to compare sides and understanding of "normal").
- Ask/observe the type of footwear the patient uses (a systematic review suggests shoes affect velocity, step time, and step length in younger children's gait[32]).
Objective
An objective approach is quantitative and parameters like time, distance, and muscle activity will be measured. Other objective methods to assess the gait cycle that use equipment include:[33][31]
- Video Analysis and Treadmill
- Electronic and Computerized Apparatus
- Electronic Pedometers
- Satellite Positioning System[30]
Qualitative methods to assess and analyse gait include: [31]
- Rancho Los Amigos Hospital Rating List[34]
- Ten Meter Walking Test[35]
- 6 Minute Walk Test
- 2 Minute Walk Test
- Dynamic Gait Index
- Emory Functional Ambulation Profile[36]
- Timed Up and Go Test[37] This test is statistically associated with falling in men, but not in women.
- Functional Ambulation Categories[38]
- Tinetti-Test[39]
Clinical Bottom Line[edit | edit source]
Good knowledge of anatomy and biomechanics is important to understand the different phases of the gait cycle. When you know the normal pattern, you can see what’s going wrong!
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Pirker W, Katzenschlager R. Gait disorders in adults and the elderly. Wiener Klinische Wochenschrift. 2017 Feb 1;129(3-4):81-95.Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5318488/ (last accessed 27.6.2020)
- ↑ 2.0 2.1 Medical dictionary Gait speed Available from: https://medical-dictionary.thefreedictionary.com/gait+speed (last accessed 28.6.2020)
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 3.16 3.17 3.18 Shultz SJ et al. Examination of musculoskeletal injuries. 2nd ed, North Carolina: Human Kinetics, 2005. p55-60.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 4.13 4.14 4.15 4.16 4.17 4.18 4.19 4.20 Loudon J, et al. The clinical orthopedic assessment guide. 2nd ed. Kansas: Human Kinetics, 2008. p.395-408.
- ↑ The biomechanics of running Tom F. Novacheck Motion Analysis Laboratory, Gillette Children’s Specialty Healthcare, Uni6ersity of Minnesota, 200 E. Uni6ersity A6e., St. Paul, MN 55101, USA Received 25 August 1997; accepted 22 September 1997 Available from:
- ↑ Vaughan CL. Theories of bipedal walking: an odyssey. J Biomech 2001;36(2003):513-523.Available fromhttp://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.468.2414&rep=rep1&type=pdf
- ↑ Nicole Comninellis The Gait Cycle Animation Available from https://www.youtube.com/watch?time_continue=35&v=DP5-um6SvQI
- ↑ 8.0 8.1 8.2 Demos, Gait analysis, (http://www.ncbi.nlm.nih.gov/books/NBK27235/), 2004.
- ↑ Berger W, et al. Corrective reactions to stumbling in man: neuronal co-ordination of bilateral leg activity during gait. J Physiol 1984;357: 109-125.
- ↑ Alexandra Kopelovich. Gait Range of Motion Available from: https://www.youtube.com/watch?v=5Z6shSu96CM [last accessed 31/3/2021]
- ↑ Alexandra Kopelovich. Ground Reaction Force During the Gait Cycle Available from: https://www.youtube.com/watch?v=Y2RHvicAM2o [last accessed 31/3/2021]
- ↑ Alexandra Kopelovich. Gait Muscular Activity & Action. Available from: https://www.youtube.com/watch?v=WuG87mRiY-8[last accessed 31/3/2021]
- ↑ 13.0 13.1 Shi D, et al. Effect of anterior cruciate ligament reconstruction on biomechanical features of knee level in walking: a meta analysis. Chin Med J 2010;123(21):[[1]].
- ↑ Mehrholz J, Harvey LA, Thomas S, Elsner B. Is body-weight-supported treadmill training or robotic-assisted gait training superior to overground gait training and other forms of physiotherapy in people with spinal cord injury? A systematic review. Spinal cord. 2017 Aug;55(8):722-9.
- ↑ 15.0 15.1 15.2 15.3 15.4 15.5 15.6 15.7 15.8 15.9 Malanga G and Delisa J.A. Section One: Clinical Observation. Office of rehabilitation Research and Development No Date. http://www.rehab.research.va.gov/mono/gait/malanga.pdf (accessed 6 February 2010)
- ↑ Radder DL, Lígia Silva de Lima A, Domingos J, Keus SH, van Nimwegen M, Bloem BR, de Vries NM. Physiotherapy in Parkinson’s disease: a meta-analysis of present treatment modalities. Neurorehabilitation and Neural Repair. 2020 Oct;34(10):871-80.
- ↑ da Cunha MJ, Rech KD, Salazar AP, Pagnussat AS. Functional electrical stimulation of the peroneal nerve improves post-stroke gait speed when combined with physiotherapy. A systematic review and meta-analysis. Annals of Physical and Rehabilitation Medicine. 2021 Jan 1;64(1):101388.
- ↑ 18.0 18.1 18.2 18.3 18.4 18.5 18.6 18.7 18.8 University of Washington. Pathologic Gait: Musculoskeletal http://courses.washington.edu/anatomy/KinesiologySyllabus/PathGait1Ortho.pdf (accessed 5 February 2015)
- ↑ Gait Examination. Available from :https://www.youtube.com/watch?v=igHkor7AYUU
- ↑ Mehrholz J, Harvey LA, Thomas S, Elsner B. Is body-weight-supported treadmill training or robotic-assisted gait training superior to overground gait training and other forms of physiotherapy in people with spinal cord injury? A systematic review. Spinal cord. 2017 Aug;55(8):722-9.
- ↑ 1. Neumann, D.A. Kinesiology of the Musculoskeletal System. (3 ed.). : Elsevier; 2017
- ↑ onlinemedicalvideoAbnormal Gait Exam : Myopathic Gait Demonstration. Available fromhttps://www.youtube.com/watch?time_continue=5&v=b5rIEx9SsCo
- ↑ scfpta gait deviation published final 001.wmvAvailable fromhttps://www.youtube.com/watch?time_continue=5&v=b5rIEx9SsCo
- ↑ Pirker W, Katzenschlager R. Gait disorders in adults and the elderly. Wiener Klinische Wochenschrift. 2017 Feb;129(3):81-95.
- ↑ Tzu-wei PH, Shorter KA, Adamczyk PG, Kuo AD. Mechanical and energetic consequences of reduced ankle plantar-flexion in human walking. Journal of Experimental Biology. 2015 Nov 1;218(22):3541-50.
- ↑ Panizzolo FA, Green DJ, Lloyd DG, Maiorana AJ, Rubenson J. Soleus fascicle length changes are conserved between young and old adults at their preferred walking speed. Gait & posture. 2013 Sep 1;38(4):764-9.
- ↑ Pirker W, Katzenschlager R. Gait disorders in adults and the elderly. Wiener Klinische Wochenschrift. 2017 Feb;129(3):81-95.
- ↑ Pirker W, Katzenschlager R. Gait disorders in adults and the elderly. Wiener Klinische Wochenschrift. 2017 Feb;129(3):81-95.
- ↑ Langer PS, et al. A practical manual of clinical electrodynography. 2nd ed. Deer Park: The Langer Foundation for Biomechanics and Sports Medicine Research, 1989.
- ↑ 30.0 30.1 Terrier P, Schutz Y. How useful is satellite positioning system (GPS) to track gait parameters? A review. J Neuro Eng Rehab 2005;2:28.
- ↑ 31.0 31.1 31.2 Deckers JHM, et al. Ganganalyse en looptraining voor de paramedicus, Houten, Bohnfleu van Lonhum, 1996.
- ↑ Cranage S, Perraton L, Bowles KA, Williams C. The impact of shoe flexibility on gait, pressure and muscle activity of young children. A systematic review. Journal of Foot and Ankle Research. 2019 Dec 1;12(1):55.
- ↑ Frigo C, et al. Functionally oriented and clinically feasible quantitative gait analysis method. Med Biol Eng Comput 1998;36:179-185.
- ↑ Shumway-Cook A, Woollacott MH. Motor control: translating research into clinical practice. Lippincott Williams and Wilkins, 2007. p.408.
- ↑ Van Peppen RPS, KNGF-richtlijn Beroerte, 2004, Nederlands Tijdschrift voor Fysiotherapie.
- ↑ Baer RH, Wolf SL. Modified emory functional ambulation profile: an outcome measure for the rehabilitation of post stroke gait dysfunction. Stroke 2001;32(4):973-979.
- ↑ Potsiadlo D, Richardson S. The timed “Up and Go”: a test of functional mobility for frail elderly persons. J Am Geriatr Soc 1991;39(2):142-148.
- ↑ Shephard RJ, Taunton JE. Foot and ankle in sport and exercise, Toronto:Karger, 1987. p30-38.
- ↑ Bautmans I, et al. The feasibility of whole body vibration in institutionalised elderly persons and its influence on muscle performance, balance and mobility: a randomised controlled trial. BMC Geriatr 2005;5:17.