Chronic Bronchitis: Difference between revisions
(edited images) |
No edit summary |
||
| (19 intermediate revisions by 3 users not shown) | |||
| Line 3: | Line 3: | ||
'''Top Contributors''' - {{Special:Contributors/{{FULLPAGENAME}}}} | '''Top Contributors''' - {{Special:Contributors/{{FULLPAGENAME}}}} | ||
</div> | </div> | ||
== Definition/Description == | |||
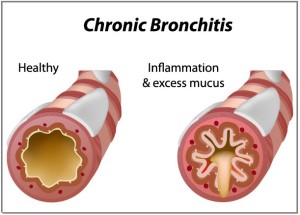
[[File:What-is-Chronic-Bronchitis-2-300x215.jpg|alt=|right|frameless]]Chronic [[Bronchitis]] (CB) is defined as a chronic cough and [[sputum]] production for at least 3 months a year for 2 consecutive years. <ref name="Kim and Criner">Kim V, Criner GJ. Chronic Bronchitis and Chronic Obstructive Pulmonary Disease. Am J Respir Crit Care Med 2013;187:228-237</ref> | |||
It is covered under the umbrella term of [[Chronic Obstructive Pulmonary Disease Rehabilitation Class|Chronic Obstructive Pulmonary Disease (COPD)]]. The COPD spectrum ranges from [[Emphysema]] to Chronic Bronchitis. Many patients have characteristics of both, putting them somewhere along the spectrum.<ref name="Kim and Criner" /> | |||
== | * CB is the [[Inflammation Acute and Chronic|inflammation]] and excessive mucus build-up in the bronchi.<ref name="British Lung Foundation">British Lung Foundation. COPD: Chronic obstructive pulmonary disease. Available from: http://www.blf.org.uk/Page/chronic-obstructive-pulmonary-disease-COPD (accessed 4 May 2015).</ref> | ||
* Emphysema occurs when the [[Alveoli|alveolar]] membrane breaks down . | |||
The overall prognosis for most patients is poor, with many patients being disabled from the progressive [[Dyspnoea|shortness of breath]]<ref name=":0" />. The prevalence of the disease has a great impact on society and on health care systems [[Global Health|around the world]]. | |||
== Epidemiology == | == Epidemiology == | ||
The occurrence of Chronic bronchitis | |||
* In the general population has been documented to vary between 3% to 7% of healthy adults. | |||
* It is estimated to be as high as 74% among those diagnosed to have COPD. | |||
Subjects under the age of 50 years who are otherwise healthy and have chronic bronchitis are at a higher risk of morbidity and mortality when compared to healthy subjects. | |||
The increasing prevalence of chronic bronchitis is thought to be associated with increasing age, [[Smoking and Exercise|tobacco smoking]], occupational exposure, and socioeconomic status.<ref name=":0">Widysanto A, Mathew G. [https://www.ncbi.nlm.nih.gov/books/NBK482437/?report=reader Chronic Bronchitis]. StatPearls [Internet]. 2020 Aug 23.Available from: https://www.ncbi.nlm.nih.gov/books/NBK482437/?report=reader<nowiki/>(accessed 24.5.2021)</ref> | |||
There | == Etiology == | ||
There are many known causes of chronic bronchitis. | |||
The most important causative factor is exposure to cigarette smoke either due to active smoking or passive inhalation. Other causes include: | |||
* Inhaled irritants to the respiratory tract eg smog, industrial pollutants, airborne chemicals (eg ammonia and sulfur) can cause chronic bronchitis. | |||
* Repeated exposure to [[Viral Infections|viral infections]] can cause chronic bronchitis. | |||
* People with an associated background in [[Respiratory Disorders|respiratory diseases]] eg [[asthma]], [[Cystic Fibrosis|cystic fibrosis]], or [[bronchiectasis]] have a higher predisposition to develop chronic bronchitis. | |||
* Chronic [[Gastroesophageal Reflux Disease|gastroesophageal reflux]] is a well documented but less frequent cause of chronic bronchitis<ref name=":0" />. | |||
* There is also a [[Genetic Conditions and Inheritance|genetic factor]] associated with COPD, it is a deficiency in alpha-1-antitrypsin. This genetic marker is indicative of Emphysema, but many patients on the COPD spectrum have characteristics of both Emphysema and CB.<ref name="British Lung Foundation" /> | |||
== Pathophysiology == | |||
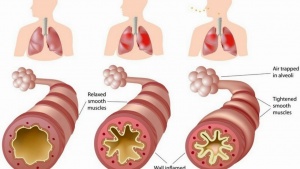
[[File:Maxresdefault1.jpg|300x300px|alt=|right|frameless]]Chronic bronchitis is thought to be caused by overproduction and hypersecretion of mucus by goblet cells. Epithelial cells lining the airway response to toxic, infectious stimuli by releasing inflammatory mediators and eg pro-inflammatory [[cytokines]]. | |||
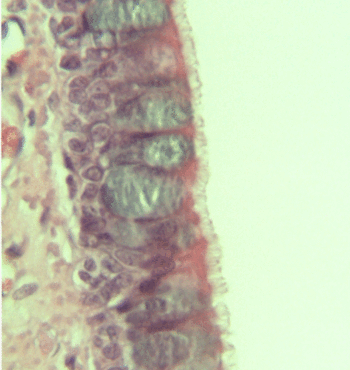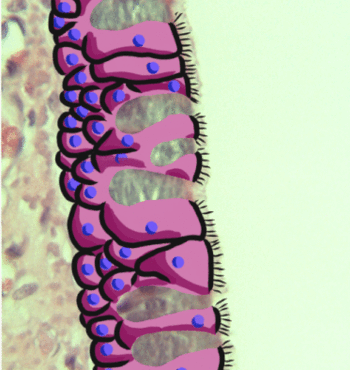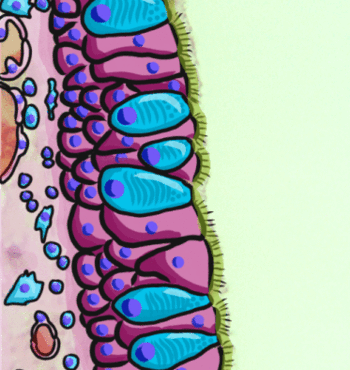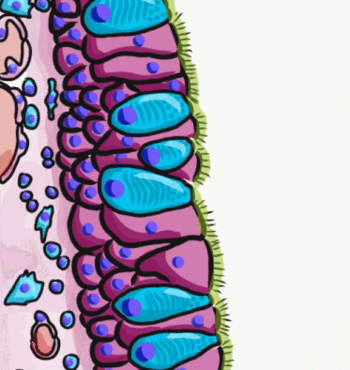
During an acute exacerbation of chronic bronchitis, the bronchial mucous membrane becomes hyperemic and edematous with diminished bronchial mucociliary function. This, in turn, leads to airflow impediment because of luminal obstruction to small airways. The airways become clogged by debris and this further increases the irritation. The characteristic cough of bronchitis is caused by the copious secretion of mucus in chronic bronchitis.<ref name=":0" />[[File:Goblet cells.gif|right|frameless|370x370px]]Image 2: Pseudostratified epithelium, highlighting the pseudostratified epithelial cells, goblets cells (shown in blue), then underlying [[Connective Tissue Disorders|connective tissue]] | |||
* Smokers with moderate COPD and CB had a greater number of goblet cells in their peripheral airways<ref name="Kim and Criner" />, which increases the potential of mucus in the lungs (a greater number of small airways were blocked with mucus increases the severity of the disease).<ref name="Kim and Criner" /> | |||
* Mucus hypersecretion is one of the risks associated with cigarette smoke exposure, viral infections, bacterial infections, or inflammatory cell activation. When combined with poor ciliary function, distal airway occlusion, ineffective cough, [[Muscles of Respiration|respiratory muscle]] weakness, and reduced [[Spirometry|peak expiratory flow]] clearing secretions is extremely difficult and requires high energy consumption. <ref name="Kim and Criner" /> | |||
Mucus hypersecretion is one of the risks associated with cigarette smoke exposure, viral infections, bacterial infections, or inflammatory cell activation. When combined with poor ciliary function, distal airway occlusion, ineffective cough, respiratory muscle weakness and reduced peak expiratory flow clearing secretions is extremely difficult and requires high energy consumption. <ref name="Kim and Criner" / | |||
== Clinical Manifestations == | == Clinical Manifestations == | ||
[[File:Bronchitis.jpg|right|frameless]] | |||
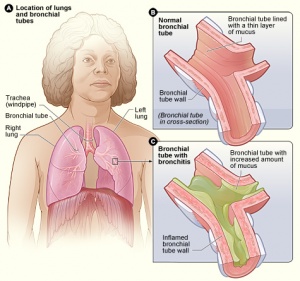
The clinical presentation can be increased exacerbation rate, accelerated decline in lung function, worse health-related quality of life and increase in mortality. <ref name="Kim and Criner" /> | The clinical presentation can be an increased exacerbation rate, accelerated decline in lung function, worse health-related quality of life and an increase in mortality.<ref name="Kim and Criner" /> Common symptoms outlined by the British Lung Foundation include<ref name="British Lung Foundation" />: | ||
*Wheezing, particularly breathing out | *Wheezing, particularly breathing out | ||
*Breathlessness when resting or active | *Breathlessness when resting or active | ||
*Tight chest | *Tight chest | ||
*Cough | *Cough | ||
*Producing more mucus or phlegm than usual | *Producing more mucus or phlegm than usual<br> | ||
These symptoms would be persistent for at least 3 months a year for 2 consecutive years to be considered Chronic Bronchitis.<ref name="Kim and Criner" /> | |||
== Evaluation == | |||
The most critical factor in the diagnosis of chronic bronchitis is a typical history to exclude other possible diseases of the lower respiratory tract. | |||
The investigations which assist in confirming the diagnosis of chronic bronchitis are: | |||
*'''[[Blood Tests|Blood test]]:''' This is to see if your symptoms could be due to anemia, or to see if the symptoms are due to the genetic marker alpha-1-antitrypsin deficiency.<ref name="NHS">National Health Services. Chronic Obstructive pulmonary disease. Available from: http://www.nhs.uk/Conditions/Chronic-obstructive-pulmonary-disease/Pages/Introduction.aspx (accessed 4 May 2015)</ref> | |||
* A [[Chest X-Rays|chest x-ray]] in the [[Older People - Patterns of Illness, Physiological Changes and Multiple Pathology|elderly]] and when physical findings suggest pneumonia is important. | |||
* A culture of the sputum when a [[Bacterial Infections|bacterial]] infection is suspected is indicated. | |||
* The additional investigations which are a helpful measurement of oxygen saturation, and [[Pulmonary Function Test|pulmonary function tests]] eg [[spirometry]]<ref name=":0" /> | |||
{{#ev:youtube| | {{#ev:youtube|6kbgZWS5wH0}}<ref>The European Lung Foundation. Spirometry: how to take a lung function test. https://www.youtube.com/watch?v=6kbgZWS5wH0 [last accessed 5/6/15]</ref> | ||
=== Treatment / Management === | |||
[[File:Bronchodilators.png|right|frameless|399x399px]] | |||
The primary aim of treatment for chronic bronchitis is to relieve symptoms, prevent complication and slow the progression of the disease. The primary goals of therapy are aimed at reducing the overproduction of mucus, controlling inflammation and lowering cough. These are achieved by pharmacological as well as nonpharmacological interventions. | |||
The mainstay of pharmacological interventions are the following: | |||
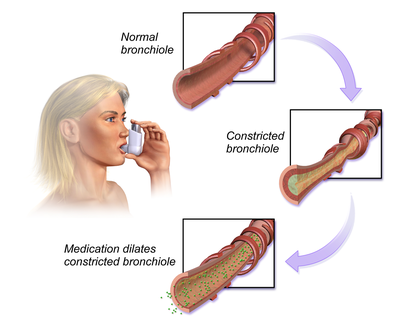
# Bronchodilators: Short and long-acting β-Adrenergic receptor Agonists as well as Anticholinergic help by increasing the airway lumen, increasing ciliary function and by increasing mucous hydration. | |||
# Glucocorticoids: Reduce inflammation and mucus production.Inhaled corticosteroids reduce exacerbation and improve quality of life.However, it is administered under medical supervision and for short periods of time as long-term usage can induce osteoporosis, diabetes, and hypertension. | |||
# Antibiotic therapy: is not indicated in the treatment of chronic bronchitis however macrolide therapy has been shown to have anti-inflammatory property and hence may have a role in the treatment of chronic bronchitis. | |||
# Phosphodiesterase-4 inhibitors: decrease inflammation and promote airway smooth muscle relaxation by preventing the hydrolysis of cyclic adenosine monophosphate a substance when degraded leads to the release of inflammatory mediators. | |||
== Nonpharmacological interventions. == | |||
== Physiotherapy == | |||
[[File:Cardio Boxing Group Fitness Class.jpg|right|frameless]] | |||
The goal of the physiotherapist should involve education, improve exercise tolerance, reduce exacerbations and hospitalization, assist in sputum clearance, and increase thoracic mobility and lung volume. | |||
[[Pulmonary Rehabilitation|Pulmonary rehabilitation]] and [[Respiratory Physiotherapy]]<nowiki/>are important parts of treatment for chronic bronchitis. See links for fantastic detail.. | |||
== Education == | |||
Chronic bronchitis has a significant impact on morbidity and [[Quality of Life|quality of life]]. Education of the individual with CB by the treating clinical staff in terms of the presenting condition, medication use, treatment options, and self-management may help the psychological effects associated with having a chronic condition and promote a proactive approach to management. | |||
The most critical nonpharmacological intervention is [[Smoking Cessation and Brief Intervention|smoking cessation]]. Smoking cessation improves mucociliary function and decreases goblet cell hyperplasia. Smoking cessation has also been shown to reduce airway injury resulting in lower levels of exfoliated mucus in tracheobronchial cells. | |||
== Exercise == | |||
Regular [[Therapeutic Exercise|exercise]] can have positive effects on the management, treatment, and prevention of CB and COPD. [[Aerobic Exercise|Aerobic exercise]] and upper & lower limb resistance training have shown positive changes in the reduction of airflow obstruction, clearing of airways, improved functional capabilities increased energy levels, and sputum expectoration. Exercise programs should be under the supervision of the treating clinical team (eg physiotherpist) and a discussion with the general practitioner should be had before taking part in any exercise program.<ref name="ACSM">Dressendorfer R, Haykowsky M, Eves N. Exercise for Persons with Chronic Obstructive Pulmonary Disease. Available from: http://www.acsm.org/docs/current-comments/exerciseforpersonswithcopd.pdf. (Accessed 6 May 2015).</ref> | |||
=== Physical Fitness === | |||
Aerobic exercise and upper & lower limb resistance training have the ability to increase physical fitness, functional tolerance, energy levels, and decrease concern over the shortness of breath, exacerbations, and hospital visits. Specific guidelines are put in place in concern to exercise for individuals with chronic bronchitis and COPD. The Discussion should be held with the treating clinical team before participation in any exercise program begins. | |||
== Prevention == | == Prevention == | ||
There is presently no cure for CB. However, with lifestyle changes, education and proper management it is possible to prevent exacerbations of the condition. | There is presently no cure for CB. However, with lifestyle changes, education, and proper management it is possible to prevent exacerbations of the condition. | ||
=== Avoiding Irritants === | |||
Being aware of possible irritants within the household, workplace, and places of recreation can help reduce risk factors associated with chronic bronchitis and reduce exacerbations. Irritants to be aware of can include dust, chemicals, vapors, air pollution, and smoke. Proper respiratory protective equipment should be made readily available if contact with irritants in the workplace commonly occurs. <ref name="Mayo">Mayo Clinic Staff. Diseases and Conditions. COPD Prevention. 2014. Available from: http://www.mayoclinic.org/diseases-conditions/copd/basics/prevention/CON-20032017. Accessed 6 May 2015).</ref> | |||
Being aware of possible irritants within the household, | |||
=== Practice Proper Hygiene === | |||
Practicing good hygiene can reduce the spread of germs, bacteria, and infections. This can help reduce the risk factors associated with bronchitis and help reduce exacerbations of chronic bronchitis.<ref name="Health">National Health Services. Bronchitis. 14/07/2014; Available from: http://www.nhs.uk/conditions/Bronchitis/Pages/Introduction.aspx. (Accessed 6 May 2015).</ref> | |||
== References == | == References == | ||
| Line 133: | Line 108: | ||
<references /> | <references /> | ||
[[Category:Cardiopulmonary]] [[Category: | [[Category:Conditions]] | ||
[[Category:Cardiopulmonary]] | |||
[[Category:Cardiopulmonary - Conditions]] | |||
[[Category:Respiratory_Disease]] | |||
[[Category:Respiratory Disease - Conditions]] | |||
[[Category:Glasgow_Caledonian_University_Project]] | |||
Latest revision as of 01:41, 9 July 2021
Original Editors - Students from Glasgow Caledonian University's Cardiorespiratory Therapeutics Project.
Top Contributors - Lindsey Chisholm, Kelly D'Autremont, Lucinda hampton, Kim Jackson, Esraa Mohamed Abdullzaher, Admin, Evan Thomas, Uchechukwu Chukwuemeka, Michelle Lee, WikiSysop and Fasuba Ayobami
Definition/Description[edit | edit source]
Chronic Bronchitis (CB) is defined as a chronic cough and sputum production for at least 3 months a year for 2 consecutive years. [1]
It is covered under the umbrella term of Chronic Obstructive Pulmonary Disease (COPD). The COPD spectrum ranges from Emphysema to Chronic Bronchitis. Many patients have characteristics of both, putting them somewhere along the spectrum.[1]
- CB is the inflammation and excessive mucus build-up in the bronchi.[2]
- Emphysema occurs when the alveolar membrane breaks down .
The overall prognosis for most patients is poor, with many patients being disabled from the progressive shortness of breath[3]. The prevalence of the disease has a great impact on society and on health care systems around the world.
Epidemiology[edit | edit source]
The occurrence of Chronic bronchitis
- In the general population has been documented to vary between 3% to 7% of healthy adults.
- It is estimated to be as high as 74% among those diagnosed to have COPD.
Subjects under the age of 50 years who are otherwise healthy and have chronic bronchitis are at a higher risk of morbidity and mortality when compared to healthy subjects.
The increasing prevalence of chronic bronchitis is thought to be associated with increasing age, tobacco smoking, occupational exposure, and socioeconomic status.[3]
Etiology[edit | edit source]
There are many known causes of chronic bronchitis.
The most important causative factor is exposure to cigarette smoke either due to active smoking or passive inhalation. Other causes include:
- Inhaled irritants to the respiratory tract eg smog, industrial pollutants, airborne chemicals (eg ammonia and sulfur) can cause chronic bronchitis.
- Repeated exposure to viral infections can cause chronic bronchitis.
- People with an associated background in respiratory diseases eg asthma, cystic fibrosis, or bronchiectasis have a higher predisposition to develop chronic bronchitis.
- Chronic gastroesophageal reflux is a well documented but less frequent cause of chronic bronchitis[3].
- There is also a genetic factor associated with COPD, it is a deficiency in alpha-1-antitrypsin. This genetic marker is indicative of Emphysema, but many patients on the COPD spectrum have characteristics of both Emphysema and CB.[2]
Pathophysiology[edit | edit source]
Chronic bronchitis is thought to be caused by overproduction and hypersecretion of mucus by goblet cells. Epithelial cells lining the airway response to toxic, infectious stimuli by releasing inflammatory mediators and eg pro-inflammatory cytokines. During an acute exacerbation of chronic bronchitis, the bronchial mucous membrane becomes hyperemic and edematous with diminished bronchial mucociliary function. This, in turn, leads to airflow impediment because of luminal obstruction to small airways. The airways become clogged by debris and this further increases the irritation. The characteristic cough of bronchitis is caused by the copious secretion of mucus in chronic bronchitis.[3]
Image 2: Pseudostratified epithelium, highlighting the pseudostratified epithelial cells, goblets cells (shown in blue), then underlying connective tissue
- Smokers with moderate COPD and CB had a greater number of goblet cells in their peripheral airways[1], which increases the potential of mucus in the lungs (a greater number of small airways were blocked with mucus increases the severity of the disease).[1]
- Mucus hypersecretion is one of the risks associated with cigarette smoke exposure, viral infections, bacterial infections, or inflammatory cell activation. When combined with poor ciliary function, distal airway occlusion, ineffective cough, respiratory muscle weakness, and reduced peak expiratory flow clearing secretions is extremely difficult and requires high energy consumption. [1]
Clinical Manifestations[edit | edit source]
The clinical presentation can be an increased exacerbation rate, accelerated decline in lung function, worse health-related quality of life and an increase in mortality.[1] Common symptoms outlined by the British Lung Foundation include[2]:
- Wheezing, particularly breathing out
- Breathlessness when resting or active
- Tight chest
- Cough
- Producing more mucus or phlegm than usual
These symptoms would be persistent for at least 3 months a year for 2 consecutive years to be considered Chronic Bronchitis.[1]
Evaluation[edit | edit source]
The most critical factor in the diagnosis of chronic bronchitis is a typical history to exclude other possible diseases of the lower respiratory tract.
The investigations which assist in confirming the diagnosis of chronic bronchitis are:
- Blood test: This is to see if your symptoms could be due to anemia, or to see if the symptoms are due to the genetic marker alpha-1-antitrypsin deficiency.[4]
- A chest x-ray in the elderly and when physical findings suggest pneumonia is important.
- A culture of the sputum when a bacterial infection is suspected is indicated.
- The additional investigations which are a helpful measurement of oxygen saturation, and pulmonary function tests eg spirometry[3]
Treatment / Management[edit | edit source]
The primary aim of treatment for chronic bronchitis is to relieve symptoms, prevent complication and slow the progression of the disease. The primary goals of therapy are aimed at reducing the overproduction of mucus, controlling inflammation and lowering cough. These are achieved by pharmacological as well as nonpharmacological interventions.
The mainstay of pharmacological interventions are the following:
- Bronchodilators: Short and long-acting β-Adrenergic receptor Agonists as well as Anticholinergic help by increasing the airway lumen, increasing ciliary function and by increasing mucous hydration.
- Glucocorticoids: Reduce inflammation and mucus production.Inhaled corticosteroids reduce exacerbation and improve quality of life.However, it is administered under medical supervision and for short periods of time as long-term usage can induce osteoporosis, diabetes, and hypertension.
- Antibiotic therapy: is not indicated in the treatment of chronic bronchitis however macrolide therapy has been shown to have anti-inflammatory property and hence may have a role in the treatment of chronic bronchitis.
- Phosphodiesterase-4 inhibitors: decrease inflammation and promote airway smooth muscle relaxation by preventing the hydrolysis of cyclic adenosine monophosphate a substance when degraded leads to the release of inflammatory mediators.
Nonpharmacological interventions.[edit | edit source]
Physiotherapy[edit | edit source]
The goal of the physiotherapist should involve education, improve exercise tolerance, reduce exacerbations and hospitalization, assist in sputum clearance, and increase thoracic mobility and lung volume.
Pulmonary rehabilitation and Respiratory Physiotherapyare important parts of treatment for chronic bronchitis. See links for fantastic detail..
Education[edit | edit source]
Chronic bronchitis has a significant impact on morbidity and quality of life. Education of the individual with CB by the treating clinical staff in terms of the presenting condition, medication use, treatment options, and self-management may help the psychological effects associated with having a chronic condition and promote a proactive approach to management.
The most critical nonpharmacological intervention is smoking cessation. Smoking cessation improves mucociliary function and decreases goblet cell hyperplasia. Smoking cessation has also been shown to reduce airway injury resulting in lower levels of exfoliated mucus in tracheobronchial cells.
Exercise[edit | edit source]
Regular exercise can have positive effects on the management, treatment, and prevention of CB and COPD. Aerobic exercise and upper & lower limb resistance training have shown positive changes in the reduction of airflow obstruction, clearing of airways, improved functional capabilities increased energy levels, and sputum expectoration. Exercise programs should be under the supervision of the treating clinical team (eg physiotherpist) and a discussion with the general practitioner should be had before taking part in any exercise program.[6]
Physical Fitness[edit | edit source]
Aerobic exercise and upper & lower limb resistance training have the ability to increase physical fitness, functional tolerance, energy levels, and decrease concern over the shortness of breath, exacerbations, and hospital visits. Specific guidelines are put in place in concern to exercise for individuals with chronic bronchitis and COPD. The Discussion should be held with the treating clinical team before participation in any exercise program begins.
Prevention[edit | edit source]
There is presently no cure for CB. However, with lifestyle changes, education, and proper management it is possible to prevent exacerbations of the condition.
Avoiding Irritants[edit | edit source]
Being aware of possible irritants within the household, workplace, and places of recreation can help reduce risk factors associated with chronic bronchitis and reduce exacerbations. Irritants to be aware of can include dust, chemicals, vapors, air pollution, and smoke. Proper respiratory protective equipment should be made readily available if contact with irritants in the workplace commonly occurs. [7]
Practice Proper Hygiene[edit | edit source]
Practicing good hygiene can reduce the spread of germs, bacteria, and infections. This can help reduce the risk factors associated with bronchitis and help reduce exacerbations of chronic bronchitis.[8]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 Kim V, Criner GJ. Chronic Bronchitis and Chronic Obstructive Pulmonary Disease. Am J Respir Crit Care Med 2013;187:228-237
- ↑ 2.0 2.1 2.2 British Lung Foundation. COPD: Chronic obstructive pulmonary disease. Available from: http://www.blf.org.uk/Page/chronic-obstructive-pulmonary-disease-COPD (accessed 4 May 2015).
- ↑ 3.0 3.1 3.2 3.3 3.4 Widysanto A, Mathew G. Chronic Bronchitis. StatPearls [Internet]. 2020 Aug 23.Available from: https://www.ncbi.nlm.nih.gov/books/NBK482437/?report=reader(accessed 24.5.2021)
- ↑ National Health Services. Chronic Obstructive pulmonary disease. Available from: http://www.nhs.uk/Conditions/Chronic-obstructive-pulmonary-disease/Pages/Introduction.aspx (accessed 4 May 2015)
- ↑ The European Lung Foundation. Spirometry: how to take a lung function test. https://www.youtube.com/watch?v=6kbgZWS5wH0 [last accessed 5/6/15]
- ↑ Dressendorfer R, Haykowsky M, Eves N. Exercise for Persons with Chronic Obstructive Pulmonary Disease. Available from: http://www.acsm.org/docs/current-comments/exerciseforpersonswithcopd.pdf. (Accessed 6 May 2015).
- ↑ Mayo Clinic Staff. Diseases and Conditions. COPD Prevention. 2014. Available from: http://www.mayoclinic.org/diseases-conditions/copd/basics/prevention/CON-20032017. Accessed 6 May 2015).
- ↑ National Health Services. Bronchitis. 14/07/2014; Available from: http://www.nhs.uk/conditions/Bronchitis/Pages/Introduction.aspx. (Accessed 6 May 2015).