Ankylosing Spondylitis (Axial Spondyloarthritis)
Original Editor - Thomas Rodeghero, Mathieu Henrotte
Lead Editors
Definition/Description[edit | edit source]
| [1] |
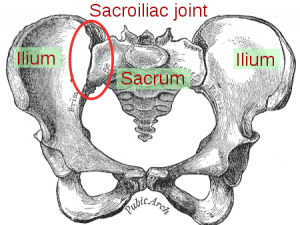
Ankylosing spondylitis (also called Bechterew's disease) is a spondyloarthritis of the spine and pelvis. Affected joints progressively become stiff and sensitive due to a bone formation at the level of the joint capsule and cartilage. Regions most affected by the disease are the axial skeleton and sacroiliac joints. It causes a decreased range of motion and gives the spine an appearance similar to bamboo, hence the alternative name "bamboo spine".
Other joints such as hips, knees, ankles, shoulders and temporomandibular joints may also be affected by the disease but in the majority of cases, the back and neck are the most affected regions. Ankylosing spondylitis (AS) is often associated with other chronic inflammatory diseases such as reactive arthritis, psoriatic arthritis, juvenile chronic arthritis, ulcerative colitis, iritis and Crohn’s disease, which can be used as signs for the diagnosis of AS.
Clinically Relevant Anatomy[edit | edit source]
File:Axial skeleton.png Axial Skeleton |
Epidemiology /Etiology[edit | edit source]
The etiology of AS is not fully understood at this time, although a strong genetic link has been determined.[2] In addition, a direct relationship between AS and the major histocompatibility human leukocyte antigen (HLA)-B27 has also been determined.[3] The exact role of this antigen is unknown but is believed to act as a receptor for an inciting antigen leading to AS.
Ninety percent of patients with AS seem to have a deficit of this antigen but not everyone with this deficit develops the condition. This is why the exact role of the B27 antigen is still to be determined in the cause of AS. [4]
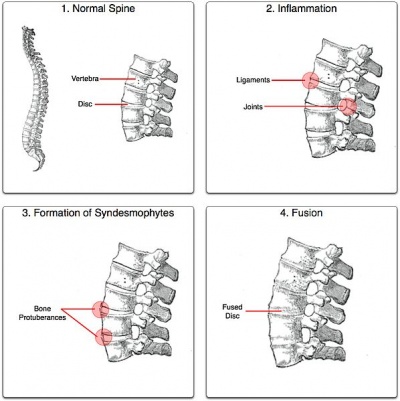
The most supported information known about the pathological process of AS is that it affects the subchondral granulation tissue and creates small lesions, ultimately leading to joint erosion.[5] In the spine this occurs at the junction of the vertebrae and the annular fibres of the intervertebral disc. These lesions in the annulus eventually undergo ossification, leading to a 'fusion' effect of the spinal segments and the similarity in appearance to bamboo.
Characteristics/Clinical Presentation[edit | edit source]
AS is predominantly seen in males in a 3:1 ratio and the onset of symptoms generally occurs in late adolescent years to early adulthood. Onset of symptoms past the age of 45 is uncommon.
The clinical presentation is usually an insidious onset of back pain in the sacroiliac (SI) joints and gluteal regions. Morning stiffness lasting greater than 30 minutes is a common subjective complaint, as well as waking up in the second half of the night. Pain is usually exacerbated with rest and relieved with physical activity. Complaints of intermittent breathing difficulties may also be a common complaint because AS may cause a decrease in chest expansion.
Common physical findings include:
- Forward flexed, or stooped, posture
- Decreased spinal segmental mobility
- Tenderness on palpation of the SI regions
- Bamboo spine
Differential Diagnosis
[edit | edit source]
Common disorders to consider as differential diagnoses with AS are:
- Fractures and/or dislocation
Diagnostic Procedures[edit | edit source]
The diagnosis of AS is commonly made through a combination of thorough subjective and physical examinations, laboratory data and imaging studies. Common laboratory data include the presence of the HLA-B27 antigen, although its presence is not required for a diagnosis of AS. In addition, high C-reactive proteins (CRP) are found in approximately 75% of people with AS.[6] However, this test is discouraged because it is associated with a high rate of false positives due to the fact that high CRP occurs in 10% of the caucasian population.[4]
Standard questionnaires can be used as part of the assessment to sketch the evolution of the disease.[7] Available questionnaires include:
- AMOR criteria
- BASDAI index
- BASFI index
- BAS-G index
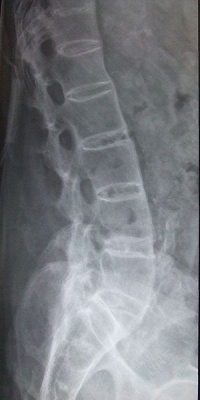
The New York criteria for diagnosing AS combines physical findings with radiograph studies. Physical findings include limitations of lumbar spine motion in three planes, pain (or history of pain) at the thoraco-lumbar junction or lumbar spine and a limitation of chest expansion to one inch or less measured at the 4th intercostal space. Radiographic findings are graded on a scale of 0 to 4 where 0 represents normal findings and 4 represents complete ankylosis.[8] A definitive diagnosis is considered with the following combinations.
- Grade 3 or 4 at bilateral SI joints on radiograph with at least one physical finding
- Grade 3 or 4 unilaterally (or Grade 2 bilaterally) with two physical findings
Outcome Measures[edit | edit source]
Certain quality of life or global rating of change outcome measures may be most appropriate in the physical therapy setting because AS often affects the patient on a more general level. However, since AS affects the spine, outcome measures such as the Oswestry Disability Index (ODI) and Neck Disability Index (NDI) may also be appropriate. Laboratory values, such as the CRP, are used to monitor the effectiveness of medication treatments.
Examination[edit | edit source]
add text here related to physical examination and assessment
| [9] | [10]
Medical Management
|