Breathing Pattern Disorders: Difference between revisions
Rachael Lowe (talk | contribs) No edit summary |
Rachael Lowe (talk | contribs) No edit summary |
||
| Line 6: | Line 6: | ||
== Introduction == | == Introduction == | ||
'''Breathing Pattern Disorders''' (BPD) are abnormal respiratory patterns. They range from simple upper chest breathing to, at the extreme end of the scale, hyperventilation. This is not a disease process, simply alterations in breathing patterns that interfere | '''Breathing Pattern Disorders''' (BPD) are abnormal respiratory patterns. They range from simple upper chest breathing to, at the extreme end of the scale, hyperventilation. This is not a disease process, simply alterations in breathing patterns that interfere with normal respiratory processes. They can however, co-exist with disease such as COPD or heart disease. | ||
BPDs are | BPDs are whole person problems, especially in long term conditions where dysfunctional breathing can destabilise mind and muscles, mood and metabolism<ref name="Peters">Peters, D. Foreword In: Recognizing and Treating Breathing Disorders. Chaitow, L., Bradley, D. and Gilbert, C. Elsevier, 2014</ref>. They can play a part in, for instance, chronic fatigue, pain, fibromyalgia and some aspects of anxiety and depression. | ||
== Clinically Relevant Anatomy == | == Clinically Relevant Anatomy == | ||
| Line 14: | Line 14: | ||
add text here relating to '''''clinically relevant''''' anatomy of the condition<br> | add text here relating to '''''clinically relevant''''' anatomy of the condition<br> | ||
== Epidemiology == | == Epidemiology == | ||
It is often reported that around 10% of patients in a population are diagnosed hyperventilation syndrome. However, far more people have a more subtle, yet likely clinically significant, breathing pattern disorder. Dysfunctional breathing is more | It is often reported that around 10% of patients in a population are diagnosed hyperventilation syndrome. However, far more people have a more subtle, yet likely clinically significant, breathing pattern disorder. Dysfunctional breathing is more prevalent in women (14%) than in men (2%)<ref name="Thomas">Thomas, M., McKinley, R.K., Freeman, E., et al. The prevalence of dysfunctional breathing in adults in the community with and without asthma. Prim Care Respir J, 2005, 14, 78-82</ref> | ||
== Etiology<br> == | == Etiology<br> == | ||
| Line 22: | Line 22: | ||
Breathing pattern disorders involve being in a constant state of inhalation. This leads to hypocapnia - the deficiency of carbon dioxide in the blood due to hyperventilation - leading to respiratory alkalosis, and eventually hypoxia or the reduction of oxygen to tissue. | Breathing pattern disorders involve being in a constant state of inhalation. This leads to hypocapnia - the deficiency of carbon dioxide in the blood due to hyperventilation - leading to respiratory alkalosis, and eventually hypoxia or the reduction of oxygen to tissue. | ||
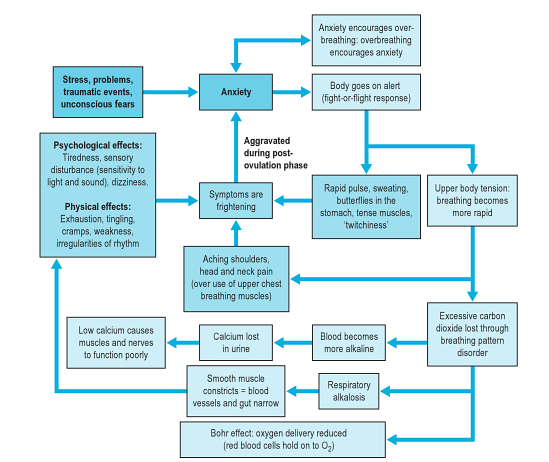
This diagram shows the stress-anxiety-breathing flow chart demonstrating multiple possible effects and influences of breathing pattern disorders. | This diagram shows the stress-anxiety-breathing flow chart demonstrating multiple possible effects and influences of breathing pattern disorders. | ||
<br> | |||
[[Image:Breathing-pattern-disorders-flow-chart.png|center|Stress-anxiety-breathing flow chart showing multiple possible effects and influences of breathing pattern disorders]]<br> | |||
[[Image:Breathing-pattern-disorders-flow-chart.png|center|Stress-anxiety-breathing flow chart showing multiple possible effects and influences of breathing pattern disorders]]<br> | |||
== Clinical Presentation == | == Clinical Presentation == | ||
| Line 38: | Line 38: | ||
== Outcome Measures == | == Outcome Measures == | ||
Nijmegen Questionnaire | Nijmegen Questionnaire | ||
== Management / Interventions<br> == | == Management / Interventions<br> == | ||
Management commonly requires the removal of causative factors and the rehabilitation of habitual acquired dysfunctional breathing patterns. In order to achieve this most efficiently it may be necessary to restore normal function of the respiratory system such as thoracic mobility and muscle tone and length. | |||
== Differential Diagnosis<br> == | == Differential Diagnosis<br> == | ||
Revision as of 09:13, 25 March 2014
Original Editor - Your name will be added here if you created the original content for this page.
Top Contributors - Rachael Lowe, Leon Chaitow, Admin, Ewa Jaraczewska, Kim Jackson, Jess Bell, Tarina van der Stockt, Wanda van Niekerk, Khloud Shreif, Fasuba Ayobami, Ajay Upadhyay, WikiSysop, Lucinda hampton, 127.0.0.1, Evan Thomas, Scott Buxton, Venus Pagare, Marleen Moll and Olajumoke Ogunleye
Introduction[edit | edit source]
Breathing Pattern Disorders (BPD) are abnormal respiratory patterns. They range from simple upper chest breathing to, at the extreme end of the scale, hyperventilation. This is not a disease process, simply alterations in breathing patterns that interfere with normal respiratory processes. They can however, co-exist with disease such as COPD or heart disease.
BPDs are whole person problems, especially in long term conditions where dysfunctional breathing can destabilise mind and muscles, mood and metabolism[1]. They can play a part in, for instance, chronic fatigue, pain, fibromyalgia and some aspects of anxiety and depression.
Clinically Relevant Anatomy[edit | edit source]
add text here relating to clinically relevant anatomy of the condition
Epidemiology[edit | edit source]
It is often reported that around 10% of patients in a population are diagnosed hyperventilation syndrome. However, far more people have a more subtle, yet likely clinically significant, breathing pattern disorder. Dysfunctional breathing is more prevalent in women (14%) than in men (2%)[2]
Etiology
[edit | edit source]
Breathing pattern disorders involve being in a constant state of inhalation. This leads to hypocapnia - the deficiency of carbon dioxide in the blood due to hyperventilation - leading to respiratory alkalosis, and eventually hypoxia or the reduction of oxygen to tissue.
This diagram shows the stress-anxiety-breathing flow chart demonstrating multiple possible effects and influences of breathing pattern disorders.
Clinical Presentation[edit | edit source]
There are a wide variety of symptoms, the most extreme
Diagnostic Procedures[edit | edit source]
add text here relating to diagnostic tests for the condition
Outcome Measures[edit | edit source]
Nijmegen Questionnaire
Management / Interventions
[edit | edit source]
Management commonly requires the removal of causative factors and the rehabilitation of habitual acquired dysfunctional breathing patterns. In order to achieve this most efficiently it may be necessary to restore normal function of the respiratory system such as thoracic mobility and muscle tone and length.
Differential Diagnosis
[edit | edit source]
add text here relating to the differential diagnosis of this condition
Key Evidence[edit | edit source]
add text here relating to key evidence with regards to any of the above headings
Resources
[edit | edit source]
add appropriate resources here
Case Studies[edit | edit source]
add links to case studies here (case studies should be added on new pages using the case study template)
Recent Related Research (from Pubmed)[edit | edit source]
Extension:RSS -- Error: Not a valid URL: Feed goes here!!|charset=UTF-8|short|max=10
References[edit | edit source]
References will automatically be added here, see adding references tutorial.
- ↑ Peters, D. Foreword In: Recognizing and Treating Breathing Disorders. Chaitow, L., Bradley, D. and Gilbert, C. Elsevier, 2014
- ↑ Thomas, M., McKinley, R.K., Freeman, E., et al. The prevalence of dysfunctional breathing in adults in the community with and without asthma. Prim Care Respir J, 2005, 14, 78-82