Rotator Cuff Tendinopathy
Original Editors - Miguel Gonzalez-Rodriguez
Top Contributors - Miguel Gonzalez-Rodriguez, Naomi O'Reilly, Admin, Shauni Van Overstraeten, Kim Jackson, Tim Secretin, Jan Alderweireldt, Tarina van der Stockt, Fasuba Ayobami, Rachael Lowe, Simisola Ajeyalemi, Lucinda hampton, Jess Bell, Uchechukwu Chukwuemeka, Wanda van Niekerk, Evan Thomas, Anthony Mertens, 127.0.0.1, Lauren Lopez, Margaux Jacobs and Kai A. Sigel
Definition/Description
Rotator Cuff Tendinopathy, according to Lewis et al [1], "refers to pain and weakness, most commonly experienced with movements of shoulder external rotation and elevation, as a consequence of excessive load on the rotator cuff tissues". The patho-etiology of rotator cuff tendinopathy is multifactorial and can be attributed to extrinsic and intrinsic mechanisms, as well as to environmental factors. Rotator cuff tendinopathy is not a homogenous entity because of the diverse nature of the factors involved and hence, different treatment interventions are required, which take these specific mechanisms/factors into account.
Clinically Relevant Anatomy
The Rotator Cuff is a common name for the group of 4 distinct muscles and their tendons that provide strength and stability during motion of the shoulder. The muscles arise from the scapula and connect to the head of the humerus, forming a cuff at the glenohumeral joint. Cranial to the rotator cuff, there is a bursa that covers and protects the muscle tendons as they are in close contact to the surrounding bones.[2] The rotator cuff muscles include: [3]
| Origin on Scapula | Insertion on Humerus | Primary Function | |
|---|---|---|---|
| Supraspinatus | Supraspinous Fossa | Superior Facet of Greater Tuberosity | Abduction |
| Infraspinatus | Infraspinous Fossa | Middle Facet of Greater Tuberosity | External Rotation |
| Teres Minor | Lateral Border of Scapula | Inferior Facet of Greater Tuberosity | External Rotation |
| Subscapularis | Subscapular Fossa | Lesser Tuberosity of Humeral Neck | Internal Rotation |
Epidemiology
A prevalence of up to 30% of the population experience shoulder pain in their lives and up to 50% of the population experience at least one episode of shoulder pain annually. We can say that shoulder disorders are extremely common. 54% of people with shoulder disorders reports symptoms are still present after three years. [4] Rotator Cuff Tendinopathy is seen as the most common type of shoulder pain as it is seen in about 30% of the overall population. [5]There is an increased incidence of shoulder pain in individuals who participate in repetitive overhead activities including repetitive throwing sports like baseball or volleyball, occupations such as painting or carpentry. Rotator Cuff Tendinopathy incidence also increases with age, which needs to be considered when we talk about Rotator Cuff disorders. The following conditions can be grouped under the term Rotator Cuff Tendinopathy: "tendinitis, tendinosis, paratendinosis or partial tears of the Rotator Cuff tendons" and should exclude: "subacromial impingement syndrome, subdeltoid bursitis, Frozen Shoulder and full thickness tears"[5].
Occupational Risk Factors:[6][edit | edit source]
Awkward Postures
Static Postures
Heavy Work
Direct Load Bearing
Repetitive Arm Movements
Working with hands above shoulder height
Lack of Rest
Risk Factor for Tendinopathy:[edit | edit source]
Metabolic Disorders: Non-familial Hypercholesterolaemia, Diabetes [8]
Muscle Imbalance
Decreased Flexibility
Overweight
Advancing Age[9]
Certain Sports (Repetitive Arm Motion) [10]
Etiology[edit | edit source]
According to Lewis et al[1] the definitive cause for Rotator Cuff Tendinopathy remains uncertain but proposed mechanisms include intrinsic, extrinsic or combined factors as can be seen in Figure.1 below.
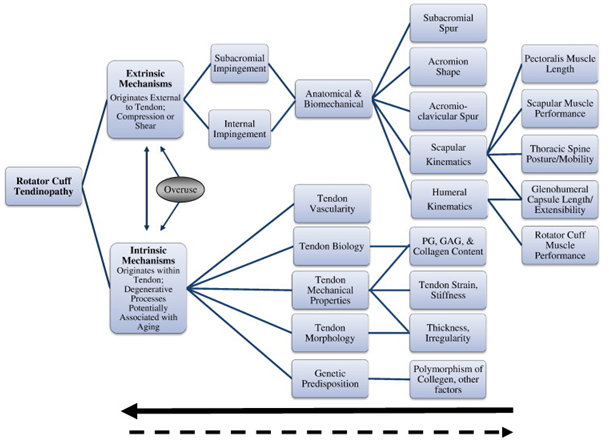
Extrinsic factors are caused by compression on the rotator cuff tendon, on the bursal side of the tendon and thus encroaching upon the subacromial space. This compression can be caused by anatomical variants of the acromion, subacromial - and AC joint spurs[12] alterations in scapular or humeral kinematics, postural abnormalities, rotator cuff and scapular muscle performance deficits, decreased extensibility of the pectoralis minor or posterior shoulder and overuse[12]. There is also an unique extrinsic mechanism, termed internal impingement where there is compression of the posterior articular surface of the tendons between the humeral head and glenoid and which is not related to the subacromial space narrowing. [13][14] Muscle fatigue or weakness could lead to the narrowing of the subacromial space and thus rehabilitation could address this. [5]
Intrinsic factors that contribute to rotator cuff tendon degradation with tensile or shear overload are alterations in biology, mechanical properties, morphology and vascularity. So the intrinsic factors have an influence on the morphology and performance of the tendon.[13][14] Age, genetics and poor biomechanics[5], overuse, and trauma[12] are also considered intrinsic factors, with an increase in load on the tendon seen as the most important. [5]
Characteristics/Clinical Presentation
The symptoms or characteristics of rotator cuff tendinopathy are pain in the area of the four rotator cuff tendons and tenderness located in the shoulder-joint with a dull character, especially with overhead reaching, reaching behind the back, lifting, and sleeping on the affected side. More relevant in elevation of the shoulder and abduction, unable to reach higher than 90° abduction, anteflexion of the upper arm. The ADL can cause quite a bit of pain. The pain is not sudden but will gradually increase and is been there for some time. Associated with pain is the growing weakness of your shoulder and inability to move.[15] [16] There could also be a local swelling.
Differential Diagnosis
Shoulder pain is a common presenting problem with a number of different causes, it is essential to determine the difference between a rotator cuff tendinopathy and some of the following shoulder problems;
- Adhesive Capsulitis (Frozen Shoulder)
- Biceps Rupture
- Bicipital Tendinopathy
- Cervical Disc Disease
- Cervical Spondylosis
- Cervical Sprain and Strain
- Complex Regional Pain Syndromes
- Osteoarthritis
- Rheumatoid Arthritis
- Shoulder Pain in Hemiplegia
- Thoracic Outlet Syndrome (TOS)
Diagnostic Procedures[edit | edit source]
Diagnosing is based on several aspects like the history of the patient. In addition, tests will be used to implicate an isolated structure. The diagnosis of a rotator cuff tendinopathy will be made based on the response to clinical tests. Supporting examinations like ultrasound, radiographs, radionucleotide isotope scan, magnetic resonance imaging (MRI), computed axial tomography (CT), electromyography, nerve conduction, single photon emission computed tomography, diagnostic analgesic injection and blood tests are sometimes used to strengthen the diagnosis.[4]
Diagnostic ultrasound is considered the best tool to diagnose Rotator Cuff Tendinopathies [5], partial thickness tears, thickened subacromial bursa and rule out a full thickness tear[17]. An MRI-scan can also be used to diagnose Rotator Cuff tendinopathies and partial rotator cuff tears.[5][17]
Outcome Measures
An Visual Analogue scale is used to describe pain in the shoulder-joint after the joint is palpated by the physiotherapist. This is not the only one, you can also use the Shoulder Pain And Disability Index (SPADI). A questionnaire filled in by the patient.[18]
Examination[edit | edit source]
Two clinical tests can be performed to assess Rotator Cuff tendinopathy.[19][20]
The first is called the “Empty Can test”. The patient stands up with his shoulders in 90°abduction, 30° horizontal adduction and in complete end range rotation. The therapist fixates his hands on the upper arm of the patient and provides a downward pressure while the patient tries to maintain his position.
In the “Hawkin’s Test”, the patient stands with the shoulders abducted to 90° and internally rotates the forearm. The presence of pain with movement is an indicator of a possible pathology.
With the modified Belly Press Test the patient stands or sits with the affected hand flat on the abdomen and elbow close to the body. The patient needs to bring the elbow forward and straighten the wrist. The final belly-press angle of the wrist needs to be measured with a goniometer. A belly-press angle difference of 10° between affected and unaffected side indicates a tendinopathy.[21][22]
Medical Management[edit | edit source]
There can be different treatment used in medical management. But not all are strongly evidence based. The use of non-steroidal anti-inflammatory drugs (NSAID’s) like ibuprofen and aspirin may have a pain reducing effect. A second option is a corticosteroid injection, which is commonly administered as a treatment for tendon disorders. It has side-effects like skin atrophy, over-sensitivity at the site of the injection and discoloration of the skin. Repetitive injections will also weaken the structure of the tendons. Medical examiners often prescribe immobilization. And the last medical management is surgical treatment. Very good results have been achieved with surgery, but it will only be chosen if conservative treatment doesn’t work.
Studies show that there may be no difference in pain between surgery and different exercise programs. There may also be no difference between open surgery and arthroscopic surgery, but people might recover sooner with arthroscopic surgery. Surgery can have several side effects, including pain, infection, difficulty moving the shoulder after the operation, wasting of the shoulder muscles, and the need to have another surgical procedure. These side effects have been shown to be independent of the type of surgery (open or arthroscopic). [23]
The effect of of subacromial corticosteroid injection is supported by the available evidence, although the effect may be small and short-term. Furthermore, it wouldn’t be better than NSAID.
Also the effects of localized microwave diathermy on disability, shoulder function and pain are equivalent to those elicited by subacromial corticosteroid injections.[24]
Furthermore, the injection of platelet-rich plasma also proves to be effective for significant improvement on pain, function and pain outcomes.[25]
Physical Therapy Management
Physical therapy of rotator cuff problems aims to reduce pain and swelling of the tendons, to achieve normal range of motion and eventually strengthen the shoulder. Initially rest and ice are used to decrease pain. It’s very important that patients initially avoid activities that increase pain and symptoms. The physiotherapist should guide the patient on when to resume these activities again.
The physiotherapist can use techniques like massage to prepare the muscles for range of motion and strength exercises. It’s important for the patient to do the exercises in the correct order; first stretching and range of motion exercises and then muscle strengthening exercises. With a decrease in shoulder internal rotation, the posterior capsule should be tested and stretched if tight[17].
Kinesiotaping has been shown to have an effect on the treatment of rotator cuff tendinopathy. But further research is needed. [26]
Ultrasound percutaneous treatment of rotator cuff calcific tendinitis should have success in short-term outcome. There is an improvement in function and symptoms are reduced in soft and middle-sized calcifications, in young adults.[27]
It has been shown that exercises are effective and support the improvement of the shoulder tendinopathy compared to no treatment or placebo.[28]
There is little to no evidence from rotator cuff tendinopathy research to guide a specific treatment regime[17].
The following are suggestions to include in the rehabilitation:
Kinetic chain exercises[17]
Correcting technique and training errors [17]
Correcting scapulo-humeral rhythm and glenohumeral instability [17]
Isometric exercises to reduce pain
Isometrics for analgesic effect has been shown in patellar tendinopathy [29]
A small pilot study used isometric exercises for patients with rotator cuff tendinopathy. The patients did external rotation exercises and progressed from 3-5 times/day and 10-20 second holds for a week. The study showed a decrease in VAS scale and noted that further research is needed in this area [30]
- Isometric exercises would be more effective than isotonic exercises (eccentric and concentric) in pain and strength improvements and also lead to faster gains in function. [31]
Studies have shown that other interventions like laser-and ultrasound therapy don’t support the effectiveness of therapy progression.[28]
On the other hand, benefit from ESWT (Extracorporeal shock wave therapy) has been demonstrated in calcific tendonitis of the rotator cuff[17]
Stretching and range of motion exercises :
pendulum exercise: bend forward and dangle a fully extended arm at shoulder height 90° from the body
posterior capsule stretching: reach with your affected arm across your body and use the other arm to pull the affected arm closer to your body.
- When symptoms allow (5-6 weeks), you can begin to give strengthening exercises.
Level of evidence 5.
- scapular squeezes - outward rotation exercise - inward rotation exercise - abduction exercise
Once the rehabilitation is complete it is important to keep the shoulder muscles strong to maintain fitness and to prevent injury. Most people with Rotator Cuff Tendinopathy see improvement after 6-12 weeks of rehabilitation.[32][33]
Information, advice and instructions
Rotator Cuff Tendinopathy indicates a problem with your shoulder muscles. It can be caused by an overload of the four muscles located in that region, or an inflammation of one of the tendons. Other causes of a tendinopathy can be found in impingement of the bursa and calcification of the tendons from the rotator cuff muscles.
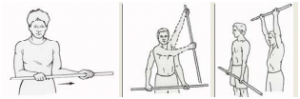
Mobilization exercise with a cane
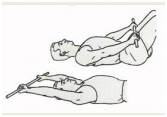
At the beginning of the training program, patients have a lack of range of motion. Active assisted motion may for instance be performed with a cane. It is important that the exercises are performed within the pain limits.[34]Start position: The patient lies on his back, with bended knees, on the table with the cane in his two hands. He puts his unaffected arm at the bottom of the cane and the affected arm at the top. Exercise: The patient moves the cane with his unaffected arm. He brings his affected arm slowly upwards and downwards and repeats the exercise 25 times. (Elevation and depression)[35][36]
Other movements: external rotation and abduction
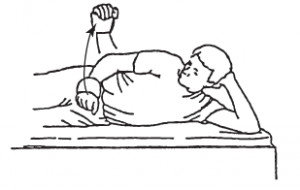
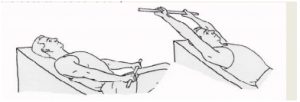
Upon external rotation the patient also lies on his back on the table with a cane in his hands. The elbows are bend in ninety degrees. Just like in the other exercise, it’s the unaffected arm that moves the other arm in external rotation.
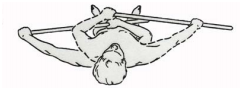
For abduction the patient moves the cane as far as possible away from the body without compensation.
You can make this exercise more difficult when you ask the patient to lie on a 45° support or to perform the exercise in a standing position.
The frequency of every exercise is 2-3 times a day, every day.
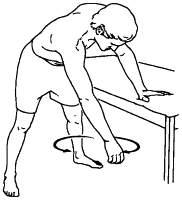
Exercise without a cane
To improve the range of motion with rotator cuff tendinopathy we can start performing pendulum exercises. To do this you must lean with your non-affected arm on a table. The affected arm is just hanging and you let it dangle. Then you can make different figures with your arm, so it swings like a pendulum. You can make small or large circles (clockwise or counterclockwise), you can go forward and backwards or from side to side. It is important that the patient doesn’t make this an active exercise, but assures these movements are generated by trunk motion.[37] (LOE 5)The muscles must be completely relaxed. Do this exercise for about 3 minutes and move your arm about 10 to 20 cm in each direction. In addition, pendulum exercises can be initiated during this time. These can be done at home, twice a day.[38](LOE 2B)
Resistance training to increase the mobility
It is proven that resistance training can be used to increase mobility. It was also proved that improving strength was associated with an improvement of other factors, namely: muscle and bone mass, balance, and also mobility. Those factors are important in our daily life.[39](LOE 2B) As such, resistance exercise training is a suitable means to increase muscle size, strength and mobility. The gains from this training are variable and will be better in younger than in older adults.[40] (LOE 5)
Strength training
You can start with strength training when the patient demonstrates adequate passive and active glenohumeral range of motion, absent of substitution patterns, with acceptable scapulothoracic kinematics
The patient progresses to isotonic and light closed chain stability exercises. The internal and external rotators are strengthened by utilizing said motions with the arm below shoulder height accompanied by elastic resistance and a towel roll placed between the arm and trunk to encourage proper technique, thereby minimizing substitution patterns.
For training the M. serratus anterior you perform the bear hug exercise. You stand with the back toward the wall, knees slightly bent, and the feet shoulder-width apart. You flex your elbows to 45°, the arms are abducted 60° out from the trunk, and the shoulder is internally rotated to 45°. The patient then performs horizontal adduction of both upper extremities, following an imaginary arc at approximately 60 degrees of elevation until they obtain maximum scapular protraction by touching their fists together as to mimic a hugging motion around a cylindrical object. Afterwards you return to starting position.
For strengthening the trapezius and rhomboid musculature you perform the sport row cord exercise.
You stand still and pull the cords till you form 90° with your humerus, which directs downwards, and your radius and ulna, which directs forward.
Advanced training of the muscles
When you start with these exercises the remodeling phase is almost complete, and the rotator cuff tissue is almost mature. The patient should be pain free with activities of daily living. In addition, the patient must not show dyskenisia when performing active motions at multiple angles.
Progressive strengthening of the posterior rotator cuff muscles, is accomplished by performing an exercise. You stand in a standing position, while performing external rotation of the shoulder at 45 degrees of abduction utilizing elastic resistance. By performing this exercise you ensure high levels of activation of the Teres Minor and the Infraspinatus. The supraspinatus muscle is optimally generated, by perfoming external rotation at 90° of abduction.
To strengthen the serratus anterior further, you perform an exercise standing, facing away from the elastic resistance attachment with the hands held at shoulder width and chest height, holding onto the resistance band or cord. Next, the upper extremities are extended forward away from the body similar to a bench press motion at approximately 120°of a forward elevation followed by protraction of the scapula. In addition the push- up with a plus progression strengthens the serratus anterior even further. It begins with gradually increasing the gravity resistance. It starts by pressing against a wall, then an edge and eventually the floor.
Advanced rhythmic stabilization
The patient stabilizes their upper extremity in a position of 90° of external rotation and 90° of forward elevation in the scapular plane. Once in this position the patient must maintain this position against elastic oscillations with a rubber bar. Additionally, advanced closed chain stability exercises are performed in the quadruped position, while stepping on and off steps of various heights and angles. Propioceptive neuromuscular facilitation can be implemented to continue the progression of rhythmic stabilization.
Self-managed exercise program
This is a self-managed exercise program to address pain and disability associated with rotator cuff tendinopathy. There are several subdivisions in the program namely; week 0, week 3-4, week 6-8 and week10-12. Each subdivision has its own exercises and its own difficulties. It is important to follow the program correctly and to properly apply the exercises[41](LOE 1A)[42](LOE 1B)
The exercises are prescribed by a physiotherapist but independently performed by the patient. It involves exercising the affected shoulder against gravity, with a resistive therapeutic band or hand weig[43]ht. It should be executed twice a day over 3 sets of 10 to 15 repetitions. This exercise can be uncomfortable for the patient but is prescribed to ensure the discomfort is manageable(LOE 1B)
Self-managed exercise program:
Week 0: Baseline assessment & start of treatment
Resisted isometric shoulder abduction (or lateral rotation or flexion etc) against a wall, or resisted shoulder abduction from 0°-30° using moderate resistance from Theraband.
Week 3-4: initial follow-up & progression
Resisted shoulder abduction from 80 to 120° using light weight, e.g. tin of food.
Week 6-8: Second follow-up & progression
Resisted shoulder abduction from 80 to 120° with progressively increasing repetition and weight, e.g heavy Theraband or dumbbell.
Week 10-12: Final follow-up & discharge
Final assessment to identify any non-resolved functional limitations and progress loaded exercises as required, e.g. press-up, pull-up.
References
- ↑ 1.0 1.1 Lewis J, McCreesh K, Roy JS, Ginn K. Rotator Cuff Tendinopathy: Navigating the Diagnosis-Management Conundrum. Journal of Orthopaedic & Sports Physical Therapy. 2015;45(11):923-37.
- ↑ Di Giacomo G., Pouliart N.,Costantini A.,De Vita A., Atlas of Functional Shoulder Anatomy. Italy:Springer, 2008. p232.
- ↑ Gray,H. Anatomy of the Human Body. Philadelphia: Lea and Febiger, 1918; Bartleby.com, 2000
- ↑ 4.0 4.1 Lewis JS. Rotator Cuff Tendinopathy/Subacromial Impingement Syndrome: Is it Time for a New Method of Assessment? Br J Sports Med 2009;43(4):259-64
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 Abat F, Alfredson H, Cucchiarini M, Madry H, Marmotti A, Mouton C, et al. Current trends in tendinopathy: consensus of the ESSKA basic science committee. Part I: biology, biomechanics, anatomy and an exercise-based approach. Journal of experimental orthopaedics. 2017;4(1):18. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5449348/ [Accessed 2nd May 2018]
- ↑ Sommerich CM, McGlothlin JD, Marras WS. Occupational Risk Factors Associated with Soft Tissue Disorders of the Shoulder: A Review of Recent Investigations in the Literature. Ergonomics. 1993; 36(6):697-717.
- ↑ Gaida JE, Ashe MC, Bass SL, Cook JL. Is Adiposity an Under‐recognized Risk Factor for Tendinopathy? A Systematic Review:Arthritis Care & Research. 2009;61(6):840-9.
- ↑ 8.0 8.1 Abate M, Schiavone C, Salini V, Andia I. Occurrence of Tendon Pathologies in Metabolic Disorders. Rheumatology. 2013;52(4):599-608.
- ↑ Grusky AZ, Giri A, O'Hanlon D, Jain NB. The relationship of aging and smoking with rotator cuff disease: a systematic review and meta-analysis. American Journal of Physical Medicine & Rehabilitation. 2022 Apr;101(4):331-40.
- ↑ Cohen RB, Williams GR. Impingement Syndrome and Rotator Cuff Disease as Repetitive Motion Disorders. Clinical Orthopaedics and Related Research. 1998;351:95-101.
- ↑ Seitz AL, McClure PW, Finucane S, Boardman ND, Michener LA. Mechanisms of Rotator Cuff Tendinopathy: Intrinsic, Extrinsic, or Both?. Clinical Biomechanics. 2011 Jan 1;26(1):1-2.
- ↑ 12.0 12.1 12.2 Factor D, Dale B. Current Concepts of Rotator Cuff Tendinopathy. International journal of sports physical therapy. 2014;9(2):274. Available from: https://members.physio-pedia.com/wp-content/uploads/2018/01/ijspt-04-274.pdf [Accessed 3rd May 2018]
- ↑ 13.0 13.1 Seitz AL, McClure PW, Finucane S, Boardman ND, Michener LA. Mechanisms of Rotator Cuff Tendinopathy: Intrinsic, Extrinsic, or Both? Clinical Biomechanics. 2011;26(1):1-2.
- ↑ 14.0 14.1 Lewis JS. Rotator Cuff Tendinopathy: A Model for the Continuum of Pathology and Related Management. British Journal of Sports Medicine. 2010;44(13):918-23
- ↑ Szczurko O, Cooley K, Mills EJ, Zhou Q, Perri D, Seely D. Naturopathic treatment of rotator cuff tendinitis among Canadian postal workers: a randomized controlled trial. Arthritis Care & Research. 2009;61(8):1037-45.
- ↑ Silverstein BA, Viikari-Juntura E, Fan ZJ, Bonauto DK, Bao S, Smith C. Natural course of nontraumatic rotator cuff tendinitis and shoulder symptoms in a working population. Scandinavian journal of work, environment & health. 2006;32(2):99-108.
- ↑ 17.0 17.1 17.2 17.3 17.4 17.5 17.6 17.7 Landry M. Brukner & Khan's Clinical Sports Medicine. 4th ed. Australia: McGraw-Hill. 2014.
- ↑ Roach KE, Budiman‐Mak E, Songsiridej N, Lertratanakul Y. Development of a Shoulder Pain and Disability Index. Arthritis & Rheumatology. 1991 ;4(4):143-9.
- ↑ http://www.nismat.org/orthocor/exam/shoulder.html
- ↑ Hughes PC, Taylor NF, Green RA. Most Clinical Tests Cannot Accurately Diagnose Rotator Cuff Pathology: A Systematic Review. Australian Journal of Physiotherapy. 2008;54(3):159-70.
- ↑ Jain NB, Wilcox R, Katz JN, Higgins LD. Clinical Examination of the Rotator Cuff. PM R: Author manuscript. 2013; 5(1): 10.1016/j.pmrj.2012.08.019.
- ↑ Myer CA, Hegedus EJ, Tarara DT, Myer DM. A User's Guide to Performance of the Best Shoulder Physical Examination Tests. British Journal of Sports Medicine, 2013;47(14):903-7.
- ↑ Coghlan JA, Buchbinder R, Green S, Johnston RV, Bell SN. Surgery for rotator cuff disease. Cochrane Database Syst Rev 2008;(1):CD005619
- ↑ Rabini A, Piazzini DB. Effects of Local Microwave Diathermy on Shoulder Pain and Function in Patients With Rotator Cuff Tendinopathy in Comparison to Subacromial Corticosteroid Injections: A Single-Blind Randomized Trial. Journal of Orthopaedic & Sports Physical Therapy. 2012; 42: 363-370
- ↑ Scarpone M, Rabago D, Snell E, DeMeo P, Ruppert K, Pritchard P et al. Effectiveness of platelet-rich plasma Injection for rotator cuff tendinopathy: a prospective Open-label study. Glob Adv Health Med. 2013; 2(2): 26–31.
- ↑ De Oliveira FCL, de Fontenay BP, Bouyer LJ, Desmeules F, Roy JS. Effects of kinesiotaping added to a rehabilitation programme for patients with rotator cufftendinopathy: protocol for a single-blind, randomised controlled trial addressing symptoms, functional limitations and underlying deficits. BMJ Open. 2017;7(9):e017951.
- ↑ Bazzocchi A, Pelotti P, Serraino S, Battaglia M, Bettelli G, Fusaro I et al. Ultrasound imaging-guided percutaneous treatment of rotator cuff calcific tendinitis: success in short-term outcome. Br J Radiol 2016;89(1057):20150407.
- ↑ 28.0 28.1 Littlewood C, May S, Walters S. A Review of Systematic Reviews of the Effectiveness of Conservative Interventions for Rotator Cuff Tendinopathy. SAGE. 2017; 5(3) https://doi.org/10.1111/sae.12009
- ↑ Rio E, Kidgell D, Purdam C, Gaida J, Moseley GL, Pearce AJ et al. Isometric exercise induces analgesia and reduces inhibition in patellar tendinopathy. Br J Sports Med. 2015;49:1277–1283.
- ↑ Parle PJ, Riddiford-Harland DL, Howitt CD, Lewis JS. Acute rotator cuff tendinopathy: does ice, low load isometric exercise, or a combination of the two produce an analgaesic effect? Br J Sports Med. 2017; 51(3):208-209.
- ↑ Rita Kinsella, Sallie M. Cowan, Lyn Watson, and Tania Pizza. A comparison of isometric, isotonic concentric and isotonic eccentric exercises in the physiotherapy management of subacromial pain syndrome/rotator cuff tendinopathy: study protocol for a pilot randomised controlled trial. 2017 Nov 14.
- ↑ Speed CA, Richards C, Nichols D, Burnet S, Wies JT, Humphreys H et al. Extracorporeal shock-wave therapy for tendonitis of the rotator cuff. A double-blind, randomised, controlled trial. J Bone Joint Surg Br. 2002;84(4):509-12.
- ↑ Rechardt M, Shiri R, Karppinen J, Jula A, Heliövaara M, Viikari-Juntura E. Lifestyle and metabolic factors in relation to shoulder pain and rotator cuff tendinitis: a population-based study. BMC Musculoskelet Disord. 2010;11:165. doi: 10.1186/1471-2474-11-165.
- ↑ Bang MD, Deyle GD. Comparison of Supervised Exercise With and Without Manual Physical Therapy for Patients With Shoulder Impingement Syndrome. Journal of Orthopaedic & Sports Physical Therapy 2000;30(3):126-137. LOE 1B
- ↑ Ellenbecker TS, Sueyoshi T, Winters M, Zeman D. Descriptive report of shoulder range of motion and rotational strength six and 12 weeks following arthroscopic superior labral repair; North American journal of sports physical therapy. 2008; 3(2): 95–106 LOE 3B
- ↑ Kuhn JE. Exercise in the treatment of rotator cuff impingement: a systematic review and a synthesized evidence-based rehabilitation protocol.Journal of Shoulder and Elbow Surgery, 2008;18(1):138-60. doi: 10.1016/j.jse.2008.06.004.. LOE 1A
- ↑ Long JL, Ruberte Thiele RA, Skendzel JG, Jeon J, Hughes RE, Miller BS et al. Activation of the shoulder musculature during pendulum exercises and light activities.J Orthop Sports Phys Ther. 2010;40(4):230-7. doi: 10.2519/jospt.2010.3095. LOE 5
- ↑ Walther M, Werner A, Stahlschmidt T, Woelfel R, Gohlke F. The subacromial impingement syndrome of the shoulder treated by conventional physiotherapy, self-training, and a shoulder brace: Results of a prospective, randomized study; J shoulder elbow surg. 2004;13(4):417-423. LOE 2B
- ↑ Rhodes EC, Martin AD,Taunton JE, Donnelly M, Warren J, Elliot J. Effects of one year of resistance training on the relation between muscular strength and bone density in elderly women. Br J Sports Med. 2000; 4(1) http://dx.doi.org/10.1136/bjsm.34.1.18. LOE 2B
- ↑ Drummond MJ, Marcus RL, LaStayo PC. Targeting Anabolic Impairment in Response to Resistance Exercise in Older Adults with Mobility Impairments: Potential Mechanisms and Rehabilitation Approaches. Journal of Aging Research. 2012; Article ID 486930, 8 pages. https://doi.org/10.1155/2012/486930 LOE 5
- ↑ Littlewood C, Ashton J, Chance-Larsen K, May S, Sturrock B. Exercise for rotator cuff tendinopathy: a systematic review.Physiotherapy. 2012;98(2):101-9. LOE 1A
- ↑ Ludewig PM, Borstad JD. Effects of a home exercise programme on shoulder pain and functional status in construction workers. Occup Environ Med. 2003;60(11):841-9. LOE 1B
- ↑ Littlewood C Ashton J, Mawson S, May S, Walters S. A mixed methods study to evaluate the clinical and cost-effectiveness of a self-managed exercise programme versus usual physiotherapy for chronic rotator cuff disorders: protocol for the SELF study. BMC Musculoskeletal Disorders.2012.13: 62. doi: 10.1186/1471-2474-13-62 LOE 1B