Polymyalgia Rheumatica
Original Editors - Nicki Spencer from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Nicki Spencer, Naaike Verhaeghe, Claire Knott, Admin, Elaine Lonnemann, Kim Jackson, Rachael Lowe, Ines Musabyemariya, 127.0.0.1, Wendy Walker, Evan Thomas, Ina De Maeyer and WikiSysop
Definition/Description [edit | edit source]
Polymyalgia rheumatica (PMR) is a rheumatic inflammatory disorder that has an unknown cause.[1] It causes inflammation of the large muscles of the body and can be accompanied by systematic symptoms including malaise, fatigue, fever, and weight loss.[2] In patients with PMR, the synovial membranes and bursae that line and lubricate the joints become inflamed, causing pain and discomfort. Unlike in some other inflammatory diseases, there is no associated permanent damage to the joints or the muscles.[2] Polymyalgia rheumatic is also known as muscular rheumatism.[3] PMR is a heterogeneous disease with a major impact on QOL. [4]
Clinically Relevant Anatomy[edit | edit source]
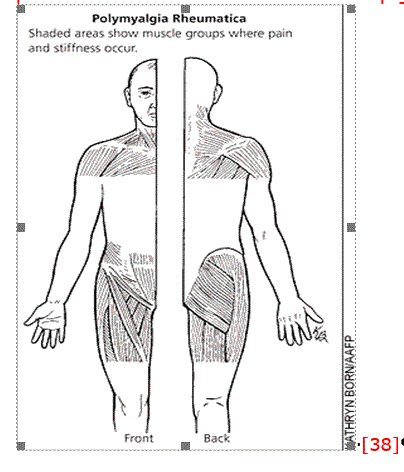
PMR is a condition that causes many (poly) painful muscles (myalgia)[5]. PMR characteristically presents with pain and stiffness in the shoulder and hip girdles and an elevated acute phase response. [6]
Epidemiology/etiology[edit | edit source]
Although polymyalgia rheumatic occurs worldwide, the highest incidence is seen in Scandinavian countries and in people of the northern European descent. [16] In the United States the lifetime risk of developing PMR is estimated at 2.43% for women and 1.66% for men. The lowest incidence rates occur at the more southern European countries like Italy, and Spain. [7]
PMR is most commonly diagnosed in persons over the age of 50, PMR has a prevalence of approximately 7 in 100 for people over 50 years of age and 4 in 10,000 in adults over 60 years of age. The prevalence is gender dependent with the ratio of men to women affected 1:2. [3] The disease is more common in Caucasian.
[8]
Some of the characteristics of PMR suggest that infectious disease expose could be an environmental factor. The disease has a very sudden onset and new cases occur in cycles, which could indicate an infection as the source. Attention has been focused on Chlamydia, Mycoplasma, parainfluenza virus or parvovirus B19 as possible infections responsible for developing PMR. Inheritance of the disorder has been suggested due to findings in some genetic studies and the pattern seen in family histories.[9] The gene(s) that could be responsible for PMR have not been definitively identified. The HLA-DRB104 and HLA-DRB01 alleles have both been found to have a possible link to PMR and GCA although this remains controversial.[10]
There may be an imbalance between immunosuppressive T-regulatory (Treg) lymphocytes and proinflammatory T-helper 17 (Th17) cells in PMR and giant cell arteritis (GCA). The frequency of Treg cells circulating appears to be reduced in patients with PMR compared with aged-matched volunteers. While on the other hand TH17 cells appear to be increased. [9]
Characteristics/Clinical Presentation[edit | edit source]
The onset of PMR is very sudden. Individuals can usually remember the exact time and day that symptoms began. Individuals often wake up one morning with extreme stiffness and soreness for no apparent reason. Synovitis and bursitis of the shoulder and hip are the cause of the patient's pain and symptoms are typically bilateral[10]
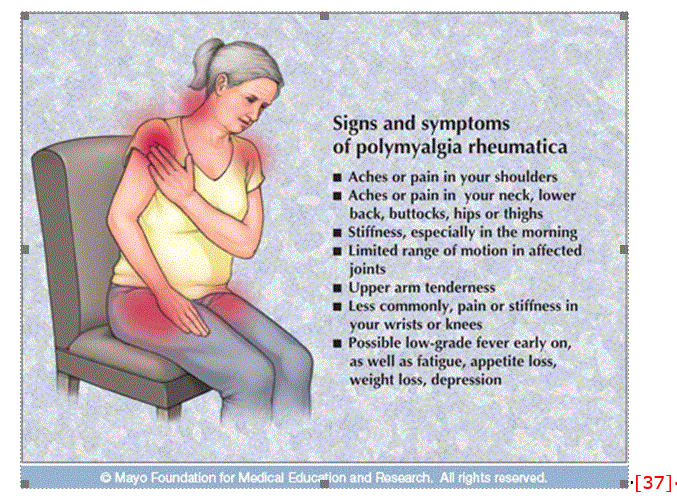
Other symptoms that are found in 40-50% of patients and include:
• stiffness after rising in the morning lasting 30 min or longer or after resting
• weakness
• fatigue
• malaise
• low-grade fever
• sweats
• headache
• weight loss
• depression
• vision changes
The symptom pattern is characteristic to PMR, although, several other autoimmune, infectious, endocrine and malignant disorders can present with similar symptoms. Ruling out the other illnesses is very important.
Differential Diagnosis[edit | edit source]
There are many conditions that can mimic PMR, like rheumatoid arthritis (RA) and spondyloarthropathies (SpA). Pain and swelling of the distal joints, like feet, hands and wrists should raise concern for an inflammatory arthritis. Some patients may present swelling and pitting edema of the hands and the feet, because of a tenosynovitits. The so called remitting seronegative symmetrical synovitis with pitting edema syndrome.[10]
PMR must be differentiated from :
Rheumatological diseases such as:
- Rheumatoid Arthritis
- Spondyloarthropathy
- Crystalline Arthritis (calcium pyrophosphate disease and calcium hydroxyapatite disorders)
- Remitting seronegative symmetric synovitis with pitting oedema syndrome
- Connective tissue diseases
- Vasculitis (giant cell arteritis, antineutrophil cytoplasmic antibody-associated vasculitis).
- Inflammatory myopathies (dermatomyositis, polymyositis )
Non-inflammatory musculoskeletal disorders such as
- Rotator-cuff diseases (rotator cuff tears, rotator cuff tendinopathy)
- Adhesive capsulitis
- Degenerative joint disease (degeneratieve disc disease)
- Fibromyalgia
- Endocrinopathies
- Thyroid diseases
- Disorders of the parathyroid gland
- Infections - viral or bacterial i.e. sepsis, ends carditis, septic arthritis
- Mycobacterial – eg tuberculosis
- Malignant diseases
- Parkinsonism
- Depression
- Hypovitaminosis D
- Drug-induced myopathy-eg, from statins
Diagnostic Procedures[edit | edit source]
Polymyalgia rheumatica is a clinical diagnosis . A careful history and physical examination are crucial in distinguishing this syndrome from other disorders that may present similarly, especially seronegative RA and paraneoplastic syndrome. Laboratory findings are non specific and show characteristic features of systemic inflammation. These include; anaemia, leukocytosis and raised markers of inflammation (ESR and CRP) and sometimes liver tests such as transaminases or alkaline phosphatase are raised. Some clinicians use an erythrocyte sedimentation rate (ESR) of higher than 30 or 40 mm/hr as a diagnostic criterium; however, 6-20% of patients with the disease have a normal sedimentation[11]. Auto-antibodies including rheumatoid factor and antibody to cyclic citrullinated peptide, are usually negative, and if positive, RA must be considered.
Shoulder, hip, neck and upper arm pain associated with PMR is usually bilateral and symmetrical. Tenderness to palpation is expected however muscle weakness is not a feature of PMR. Usually, there will be minimal muscle atrophy unless the disease progression is advanced, when disuse atrophy can occur[12]. Active range of motion is generally reduced due to pain. The 24-hour picture pattern of PMR typically presents with severe morning stiffness that improves somewhat by the evening and following periods of rest. Pain may radiate and mild synovitis may be seen in the wrist and knees. Associated systemic symptoms may include fatigue, fever and weight loss.
Radiographs of the affected joints in PMR are only useful for excluding alternative conditions. In the classification study of the EULAR/ACR, they found a high specificity for ultrasonography for discriminating PMR from other shoulder conditions (89%), but not for discriminating PMR from RA (70%)[13]
Ultrasound (US) may be of value in the diagnosis of PMR. Shoulder abnormalities found using US, such as bursitis and tenosynovitis of the long head of the biceps tendon, is more likely to be seen in patients with PMR. However, in the absence of suggestive clinical features, the presence of isolated US abnormalities should not lead to a diagnosis of PMR.[14]
Diagnostic Criteria[edit | edit source]
There are two sets of diagnostic criteria that have been created for PMR.
The Bird/Wood criteria[15], which includes:
• Bilateral shoulder stiffness
• Duration onset < 2 weeks
• Initial ESR > 40 mm/hour
• Stiffness > 60 minutes
• Age > 65 years
• Depression and/or weight loss
• Bilateral upper arm tenderness
If any 3 or more of the above criteria, or greater than 1 criteria and a clinical abnormality of the temporal artery, are present in a patient then PMR is probable. Definite PMR is characterised by probable PMR that has a positive response to corticosteroid therapy.
The Hunder criteria[15], which includes:
• Patient age > 50 years
• Bilateral aching and tenderness for > 1 month of neck or torso, shoulders or upper arms, and hips or thighs
• ESR > 40 mm/hour
• Exclusion of other diagnoses
All the above Hunder criteria must be present to have a diagnosis of definite PMR.
Both of the above criteria have been found to have a sensitivity of >90%.
The European League Against Rheumatism and American College of Rheumatology have developed classification criteria rather then diagnostic criteria, which must still be validated, and can only be applied to patients in whom new-onset bilateral shoulder pain is not attributable to an alternative diagnosis: [11]
The European League Against Rheumatism and American College of Rheumatology provisional criteria for classification of polymyalgia Rheumatica[16][17][edit | edit source]
Clinical criteria for scoring algorithm
2 points - Morning stiffness lasting more than 45 min
1 point - Hip pain or restricted range of motion
2 points - Absence of rheumatoid factor and antibody to cyclic citrullinated peptide
1 point - Absence of other joint involvement
Ultrasound criteria for scoring algorithm
1 point - At least 1 shoulder with subdeltoid bursitis, biceps tenosynovitis, or glenohumeral synovitis;
and at least one hip with synovitis or trochanteric bursitis
1 point - Both shoulders with subdeltoid bursitis, biceps tenosynovitis, or glenohumeral synovitis
Inclusion criteria for use of this classification system:
- age 50 years or older
- bilateral shoulder pain
- abnormal ESR, C-reactive protein, or both. With only clinical criteria, a score of greater than 4 had a sensitivity of 68 % and a specificity of 78 % for discriminating polymyalgia rheumatic form comparison patients.
With combination of clinical criteria and ultrasound criteria, a score of greater than 5 had a sensitivity of 66 % and specific of 81 % for discriminating patients with the disorder from comparison
Treatment[edit | edit source]
PMR is generally treated with a long course of corticosteroids. There is no consensus on the initial dosage and subsequent titration of the corticosteroid dosage. Some suggest an initial dose of 15-20 mg/day of prednisone and then a slow tapering over several weeks or months to find a maintenance dosage.Although PMR responds very well to corticosteroids, there is still concern for the adverse effects that occur with long-term steroid use. This includes diabetes, osteoporosis, hypertension, worsening of cataracts, muscle weakness, and infection. Patients taking corticosteroids must have their blood sugar, blood pressure, and body weight routinely checked. Due to the increased risk for osteoporosis, vitamin D and calcium supplements should be initiated when the corticosteroids are initiated.[18]
Complete clinical remission may take up to 5 years to occur.[19]
Physical Therapy Management [edit | edit source]
There is currently no evidence for the use of physical therapy in the treatment of patients with PMR. However, it is still important to be aware that patients may still be referred to you with a primary diagnosis of PMR, or with PMR as a co-morbidity. Physical therapy can be incorporated as a valuable component of a therapeutic regiment for this patient group in order to reduce the risk of early functional impairment and severe disability.[20] A combination of exercise therapy and education is recommended in the treatment of PMR.
Multidisciplinary Team in management of PMR[edit | edit source]
Research suggests that low-dose glucocorticoids effectively alleviate musculoskeletal symptoms related to PMR. In some countries, PMR management involves a collaborative effort between various experts in rheumatology, occupational therapy, physical therapy, rehabilitation, social work, nursing, manual therapy, podiatry, dietary, psychology, vocational counselling, and orthopedic surgery. However, the effectiveness of this approach in enhancing the health outcomes of PMR patients' needs to be more adequately studied[21].
References[edit | edit source]
- ↑ Goodman, Snyder. Differential Diagnosis for Physical Therapists: Screening for Referral. St. Louis Missouri. 2007.
- ↑ 2.0 2.1 LeGrove L. Polymyalgia rheumatica: management guidelines. Practice Nurse [serial online]. May 8, 2009;37(9):33-37. Available from: CINAHL with Full Text, Ipswich, MA. Accessed April 4, 2011.
- ↑ 3.0 3.1 Reumafonds: polymyalgia rheumatica. http://www.reumalier.be/PDF-FILES/112.juli13_BS_Polymyalgia_Reumatica.pdf. Accessed July 2013. (LOE 5)
- ↑ Hutchings A et al, Clinical outcomes, quality of life, and diagnostic uncertainty in the first year of polymyalgia rheumatica., Arthritis Rheum. 2007 Jun 15;57(5):803-9 LOE: 2a
- ↑ Arthritis New Zealand: http//www.arthritis.org.nz/wp-content/uploads/2012/06/4618_Polymyalgia_Flyer_4-1.pdf
- ↑ Sara Muller et al., The epidemiology of polymyalgia rheumatica in primary care: a research protocol, BMC Musculoskelet Disord. 2012; 13: 102. LOE: 2a
- ↑ Advances and challenges in the diagnosis and treatment of polymyalgia rheumatica; Tanaz A. Kermani et al.; February 6 2014. LOE:2a
- ↑ Siebert S, Lawson T, Wheeler M, Martin J, Williams B. Polymyalgia rheumatica: pitfalls in diagnosis. Journal Of The Royal Society Of Medicine [serial online]. May 2001;94(5):242-244. Available from: MEDLINE, Ipswich, MA. Accessed April 5, 2011.
- ↑ 9.0 9.1 Mayo Clinic: Polymyalgia rheumatica.http://www.mayoclinic.com/health/polymyalgia-rheumatica/DS00441. Accessed March 31, 2011.
- ↑ 10.0 10.1 10.2 Nothnagl T, Leeb B. Diagnosis, Differential Diagnosis and Treatment of Polymyalgia Rheumatica. Drugs &Aging [serial online]. May 2006;23(5):391. Available from: Academic Search Premier, Ipswich, MA. Accessed April 5, 2011.
- ↑ 11.0 11.1 Tanza A Kermani et al, Polymyalgia rheumatic, Lancet 2013 : 381 : 63-72.LOE : 2A
- ↑ Clement J michet etal . Polymyalgia rheumatic . BMJ 2008;336. (LOE: 2A)
- ↑ Advances and challenges in the diagnosis and treatment of polymyalgia rheumatica; Tanaz A. Kermani et al.; February 6 2014. LOE:2a
- ↑ Sakellariou G et al, Ultrasound imaging for the rheumatologist XLIII. Ultrasonographic evaluation of shoulders and hips in patients with polymyalgia rheumatica: a systematic literature review. Clin. Exp. Rheumatol. 2013;31:1-7. LOE : 3A
- ↑ 15.0 15.1 Nothnagl T, Leeb B. Diagnosis, Differential Diagnosis and Treatment of Polymyalgia Rheumatica. Drugs &Aging [serial online]. May 2006;23(5):391. Available from: Academic Search Premier, Ipswich, MA. Accessed April 5, 2011.
- ↑ Dasgupta B et al ,2012 provisional classifi cation criteria for polymyalgia rheumatica: a European League Against Rheumatism/ American College of Rheumatology collaborative initiative, Ann Rheum Dis 2012; 71: 484-92 LOE : 5
- ↑ Dasgupta B et al ,2012 provisional classification criteria for polymyalgia rheumatica: a European League Against Rheumatism/American College of Rheumatology collaborative initiative., Arthritis Rheum, 2012;64:943-54 LOE : 5
- ↑ Nothnagl T, Leeb B. Diagnosis, Differential Diagnosis and Treatment of Polymyalgia Rheumatica. Drugs &Aging [serial online]. May 2006;23(5):391. Available from: Academic Search Premier, Ipswich, MA. Accessed April 5, 2011.
- ↑ Goodman CC, Fuller KS. Pathology: Implications for the Physical Therapist. 3rd ed. St. Louis: Saunders Elsevier; 2009. (LOE 5)
- ↑ Wollenhaupt et al, Geriatric rheumatology: Special aspects of clinical diagnostics and therapy of rheumatic diseases in the elderly, 2000. (LOE 3B)
- ↑ Uhlig, T., Bjørneboe, O., Krøll, F. et al. Involvement of the multidisciplinary team and outcomes in inpatient rehabilitation among patients with inflammatory rheumatic disease. BMC Musculoskelet Disord 17, 18 (2016)