Fulcrum Test
Definition[edit | edit source]
Fulcrum Test is a clinical test used to diagnose Femoral Shaft Stress Fracture. Stress fractures of the femoral shaft are uncommon and mostly occur at the proximal third of the femur[1]
Clinically Relevant Anatomy[edit | edit source]
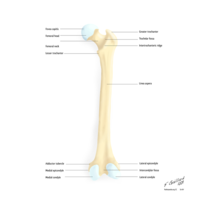
The Femur is the longest bone in the body and extends from the hip to the knee.
The head of the femur articulates with the acetabulum in the pelvic bone forming the hip joint, while the distal part of the femur articulates with the tibia and kneecap, forming the knee joint. It serves as a site of origin and insertion for many muscles and ligaments.
For more detailed information on the anatomy of the Femur
Purpose[edit | edit source]
The fulcrum test is used to aid the diagnosis of femoral shaft stress fractures. It is also useful in assessing the healing response.
If the clinical test is positive during the physical examination, the diagnosis is confirmed by a bone scan or a Magnetic Resonance Imaging scan(MRI)[2]. MRI helps to differentiate stress fractures from other pathological processes, especially neoplastic ones.[3]
Technique[edit | edit source]
The patient is seated on the examination table with his lower legs dangling. The examiner places one of his arms under the symptomatic thigh. The examiner’s arm is used as a fulcrum under the thigh and is moved from distal to proximal thigh as gentle pressure is applied to the dorsum of the knee with the opposite hand. At the point of the fulcrum under the stress fracture, gentle pressure on the knee produced increased discomfort that was often described as sharp pain and accompanied by apprehension. The contralateral leg served as a negative control. The level at which the fulcrum test is positive has always corresponded to the site of the stress fracture in the femoral shaft as seen in a scintigram or radiograph. [4]
Evidence[edit | edit source]
| Reliability[6] | Sensitivity[6] | Positive Likelihood Ratio[6] | Negative Likelihood Ratio[6] |
|---|---|---|---|
| N/A | 1.00 | ∞ | 0.00 |
Clinical Relevance[edit | edit source]
Fulcrum test can be used by the treating physician to localize the affected pain and suggest the diagnosis of femoral shaft stress injuries. Femoral Shaft Stress fractures are managed conservatively with rest, activity modification, and protected weight-bearing. The duration of treatment varies with individual patients, the period of relative rest lasts for 12 weeks.[7]
Related Tests[edit | edit source]
References[edit | edit source]
- ↑ Boden BP, Speer KP. Femoral stress fractures. Clinics in sports medicine. 1997 Apr 1;16(2):307-17.
- ↑ Deutsch AL, Coel MN, Mink JH. Imaging of stress injuries to bone: radiography, scintigraphy, and MR imaging. Clinics in sports medicine. 1997 Apr 1;16(2):275-90.
- ↑ Martin SD, Healy JH, Horowitz S. Stress fracture MRI. Orthopedics. 1993 Jan 1;16(1):75-8.
- ↑ Johnson AW, Weiss Jr CB, Wheeler DL. Stress fractures of the femoral shaft in athletes—more common than expected: a new clinical test. The American Journal of Sports Medicine. 1994 Mar;22(2):248-56.
- ↑ Fulcrum Test| Femoral Stress Fractures. Availale from https://www.youtube.com/watch?v=k2vDNa7hW2c&t=4s
- ↑ 6.0 6.1 6.2 6.3 Snyder J. John Snyder, DPT.
- ↑ Kiel J, Kaiser K. Stress reaction and fractures. InStatPearls [Internet] 2019 Jun 4. StatPearls Publishing.