Achilles Tendinopathy Toolkit: Section D - Exercise Programs
Original Editor - Kim Jackson for The BC Physical Therapy Tendinopathy Task Force:
Prof. Alex Scott, Dr Joseph Anthony, Dr Allison Ezzat, Prof Angie Fearon, JR Justesen, Dr Allison Ezzat, Dr Angie Fearon, Carol Kennedy, Michael Yates, Paul Blazey and Alison Hoens.
Top Contributors - Lucy Aird, Kim Jackson, Admin, Wanda van Niekerk and Rishika Babburu
Introduction[edit | edit source]
Exercise is a key component of the rehabilitation programme to aid the return to function and activity. In order to achieve the best recovery possible it is important, that after a period of rest, focus on tendon loading is considered. How the programme is implemented will depend on an individual's response to pain and the amount of degenerative changes that have occurred. The following programmes, Phased Achilles Tendon Loading Programme and 12-Week Eccentric Loading Programme look at tendon loading over a period of time.
Phased Achilles Tendon Loading Program[edit | edit source]
This programme is based on a protocol developed by Silbernagel et al.[1]. The programme gradually increases the load on the Achilles tendon and calf muscle over a six month period. Running and jumping are included but their inclusion are dependent upon pain which is monitored using a pain-monitoring model.
Phase 1: Weeks 1-2[edit | edit source]
Patient status: Pain and difficulty with all activities, difficulty performing ten 1‐legged heel raises
Goal: Start to exercise, gain understanding of their injury and of pain‐monitoring model
Treatment program: Perform exercises every day
- Pain‐monitoring model information and advice on exercise activity
- Circulation exercises (moving foot up/down)
- Two‐legged heel raises standing on the floor (3 sets of 10‐15 repetitions/set)
- One‐legged heel raises standing on the floor (3 sets of 10)
- Sitting heel raises (3 sets of 10)
- Eccentric heel raises standing on the floor (3 sets of 10)
Phase 2: Weeks 2-5[edit | edit source]
Patient status: Pain with exercise, morning stiffness, pain when performing heel raises
Goal: Start strengthening
Treatment program: Perform exercises every day
- Two‐legged heel raises standing on edge of stair (3 sets of 15)
- One‐legged heel raises standing on edge of stair (3 sets of 15)
- Sitting heel raises (3 sets of 15)
- Eccentric heel raises standing on edge of stair (3 sets of 15)
- Quick‐rebounding heel raises (3 sets of 20)
Phase 3: Weeks 3–12 (longer if needed)[edit | edit source]
Patient status: Handled the phase 2 exercise program, no pain distally in tendon insertion, possibly decreased or
increased morning stiffness
Goal: Heavier strength training, increase or start running and/or jumping activity
Treatment program: Perform exercises every day and with heavier load 2‐3 times/week
- One‐legged heel raises standing on edge of stair with added weight (3 sets of 15)
- Sitting heel raises (3 sets of 15)
- Eccentric heel raises standing on edge of stair with added weight (3 sets of 15)
- Quick‐rebounding heel raises (3 sets of 20)
- Plyometric training
Phase 4: Week 12–6 months (longer if needed)[edit | edit source]
Patient status: Minimal symptoms, morning stiffness not every day, can participate in sports without difficulty
Goal: Maintenance exercise, no symptoms
Treatment program: Perform exercises 2‐3 times/week
- One‐legged heel raises standing on edge of stair with added weight (3 sets of 15)
- Eccentric heel raises standing on edge of stair with added weight (3 sets of 15)
- Quick‐rebounding heel raises (3 sets of 20)
12-Week Eccentric Loading Program[edit | edit source]
A study on the effect of heavy load eccentric calf muscle training in recreational athletes with a long duration of symptoms and a diagnosis of chronic Achilles tendinosis (degenerative changes) by Alfredson et al.[2] suggest the following 12 week programme.
Patient status week 0: Achilles tendon pain - no running activities. Lower eccentric and concetric calf uscle strength onthe injured side compared to the non-injured side.
Training Schedule[edit | edit source]
All exercises were 7 days per week. Patients were told to continue to exercise with pain unless it became disabling.
Patients were allowed to jog during their 12‐week rehabilitation so long as it caused only mild discomfort.
Exercises are performed twice a day with the knee extended and then repeated with the knee flexed:
- 3 x 15 repetitions twice per day with extended knee
- 3 x 15 repetitions twice per day with a flexed knee.
Figure 1. From an upright body position and standing with all body weight on the forefoot and the ankle joint in plantar flexion lifted by the non‐injured leg (A), the calf muscle was loaded eccentrically by having the patient lower the heel with the knee straight (B) and with the knee bent (C).
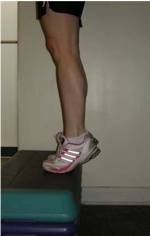
|

|

|
| A | B | C |
Figure 2. Once the eccentric loads were performed at body weight without any discomfort, subjects were given a backpack that was successively loaded with weight. In this way their eccentric loading was gradually increased. If very high weights ended up becoming needed then the subject used a weight machine.
Resources[edit | edit source]
- Click to go back to the Main Achilles Tendinopathy Toolkit page
- Click to go back to Section A - Clinical Evaluation
- Click to go back to Section B - Outcome Measures
- Click to go back to Section C - Summary of Evidence and Recommendations for Interventions
- Click to continue to Section E - Low Level Laser Therapy Dosage Calculation
- Click to continue to Section F - Medical and Surgical Interventions
- UBC Achilles Tendinopathy Toolkit
References[edit | edit source]
- ↑ Silbernagel KG, Thomeé R, Eriksson BI, Karlsson J. Continued sports activity using a pain monitoring model during rehabilitation in patients with Achilles tendinopathy. Am J Sports Med. 2007;35(6):897‐905.
- ↑ Alfredson H, Pietila T, Jonsson P, Lorentzon R. Heavy‐load eccentric calf muscle training for the treatment of chronic Achilles tendinosis. Am J Sports Med. 1998;26(3):360‐66.







