Patau Syndrome (Trisomy 13)
Introduction[edit | edit source]
Trisomy 13, also known as Patau Syndrome, is a genetic disorder that occurs when an individual has 3 copies of chromosome 13 in their cells which leads to developmental and health abnormalities[1]. It is one of the most common trisomies occurring in 1 per 5,000 births following Trisomy 21, also known as Down Syndrome, and Trisomy 18, also known as Edward's Syndrome[2].
Pathophysiology[edit | edit source]
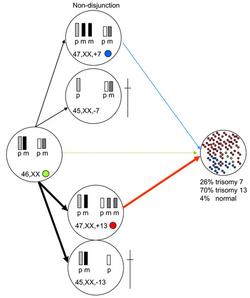
Trisomy 13 occurs due to a chromosomal abnormality during the embryonic development where either there's non-disjunction during meiosis I where one of the parental germ cells fail to separate properly resulting in an extra chromosome 13 or it can be due to a non-disjunction at the level of meiosis II where an existing germ cell with an extra chromosome 13 due to a non-disjunction at the level of meiosis I also fails to separate during meiosis II. Maternal non-disjunctions represent 91% of cases with errors during meiosis I[3]. It is also important to note that Trisomy 13 can also occur due to translocations originating from two acrocentric breaks in the juxtacentromeric region typically occurring between chromosome 13 and 14 and the expression of the phenotype will vary depending on the balance of the translocation[4].
Clinical Presentation[edit | edit source]
Infants diagnosed with Patau Syndrome often have several facial defects including cyclopia, cleft lip, cleft palate, sloppy forehead, small malformed ears, anophthalmia or microphthalmia, micrognathia, and pre-auricular tags[5]. In addition to that, they are presented with several extremity defects include postaxial polydactyly and rocker-bottom feet[6]. Furthermore, Trisomy 13 infants often suffer from central nervous system abnormalities as well with the most common defect being alobar holoprosencephaly[7]. Additionally, various organ systems are also affected by abnormalities including the lungs, liver, kidneys, genitourinary tract, digestive tract, and pancreas[8]. Patients surviving past infancy have a severe psychomotor disorders, intellectual disabilities, and seizures[9].
Diagnostic Procedures[edit | edit source]
The diagnosis of Trisomy 13 can be done prenatally with chorionic villi sampling, amniocentesis and fetal free DNA analysis[10]. In addition to that, prenatal ultrasound can also aid in the detection of central nervous system abnormalities like holoprosencephaly, facial and skeletal anomalies, renal and cardiac defects[11]. Nonetheless, a definite diagnosis is only achievable from a postnatal karyotype and fluorescence in situ hybridization (FISH) techniques[3].
Management[edit | edit source]
At birth, infants diagnosed with Patau syndrome may necessitate post-delivery measures to provide oxygen and assist with breathing. In cases of severe respiratory distress due to facial abnormalities, interventions like intubation or tracheostomy may be required to ensure adequate airway management. For those with associated heart issues, surgical procedures might be necessary to correct common cardiac anomalies. Additionally, various other surgeries could be recommended to address typical abnormalities, including hernia repair, correction of cleft lip, placement of feeding tubes, or orthopedic procedures for corrective purposes[12].
Differential Diagnosis[edit | edit source]
- Edward's Syndrome
- Down Syndrome
- Turner syndrome (monosomy X)
- Klinefelter syndrome (XXY)
- Cri-du-chat syndrome (5p- syndrome)
- Smith-Lemli-Opitz syndrome
- Cornelia de Lange syndrome[13]
References[edit | edit source]
- ↑ Hall HE, Chan ER, Collins A, Judis L, Shirley S, Surti U, Hoffner L, Cockwell AE, Jacobs PA, Hassold TJ. The origin of trisomy 13. American Journal of Medical Genetics Part A. 2007 Oct 1;143(19):2242-8.
- ↑ Springett A, Wellesley D, Greenlees R, Loane M, Addor MC, Arriola L, Bergman J, Cavero‐Carbonell C, Csaky‐Szunyogh M, Draper ES, Garne E. Congenital anomalies associated with trisomy 18 or trisomy 13: A registry‐based study in 16 European countries, 2000–2011. American journal of medical genetics Part A. 2015 Dec;167(12):3062-9.
- ↑ 3.0 3.1 Macias G, Riley C. Trisomy 13: changing perspectives. Neonatal Network. 2016 Jan 1;35(1):31-6.
- ↑ Laudat A, Serero S, Seridi I, Burc-Struxiano L. Trisomy 13 by robertsonian translocation rob (13; 13)(q10; q10)+ 13: about one case. InAnnales de Biologie Clinique 2017 Dec 1 (Vol. 75, No. 6, pp. 695-698).
- ↑ Petry P, Polli JB, Mattos VF, Rosa RC, Zen PR, Graziadio C, Paskulin GA, Rosa RF. Clinical features and prognosis of a sample of patients with trisomy 13 (Patau syndrome) from Brazil. American Journal of Medical Genetics Part A. 2013 Jun;161(6):1278-83.
- ↑ Levy PA, Marion R. Trisomies. Pediatr Rev. 2018 Feb;39(2):104-106.
- ↑ Kruszka P, Muenke M. Syndromes associated with holoprosencephaly. InAmerican Journal of Medical Genetics Part C: Seminars in Medical Genetics 2018 Jun (Vol. 178, No. 2, pp. 229-237).
- ↑ Moerman P, Fryns JP, van der Steen K, Kleczkowska A, Lauweryns J. The pathology of trisomy 13 syndrome: a study of 12 cases. Human genetics. 1988 Dec;80(4):349-56.
- ↑ Tsukada K, Imataka G, Suzumura H, Arisaka O. Better prognosis in newborns with trisomy 13 who received intensive treatments: a retrospective study of 16 patients. Cell Biochemistry and Biophysics. 2012 Jul;63:191-8.
- ↑ Wyllie JP, Wright MJ, Burn J, Hunter S. Natural history of trisomy 13. Arch Dis Child. 1994 Oct;71(4):343-345.
- ↑ Watson WJ, Miller RC, Wax JR, Hansen WF, Yamamura Y, Polzin WJ. Sonographic detection of trisomy 13 in the first and second trimesters of pregnancy. Journal of ultrasound in medicine. 2007 Sep;26(9):1209-14.
- ↑ Lantos JD. Trisomy 13 and 18—treatment decisions in a stable gray zone. Jama. 2016 Jul 26;316(4):396-8.
- ↑ Benn P, Cuckle H, Pergament E. Non‐invasive prenatal testing for aneuploidy: current status and future prospects. Ultrasound in Obstetrics & Gynecology. 2013 Jul;42(1):15-33.