Methicillin-Resistant Staphylococcus Aureus: Difference between revisions
No edit summary |
No edit summary |
||
| Line 7: | Line 7: | ||
== Definition/Description == | == Definition/Description == | ||
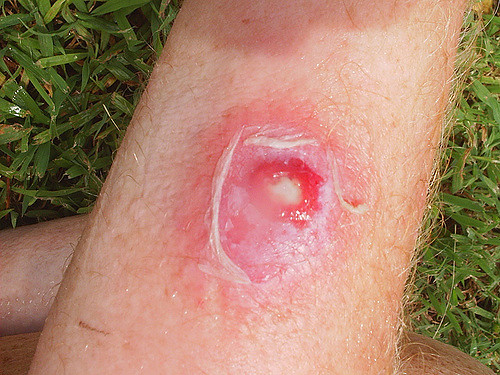
[[Image:Definition of MRSA.jpg|left|MRSA infection.]]Methicillin-Resistant Staphylococcus Aureus (MRSA) is defined as a type of bacterial staph infection that is non-responsive to antibiotics normally prescribed to treat such infections. <ref>Mayo Clinic Staff. MRSA infection - Mayo Clinic [Internet]. Mayoclinic.org. 2016 [cited 1 April 2016]. Available from: http://www.mayoclinic.org/diseases-conditions/mrsa/basics/definition/con-20024479</ref> MRSA was first described in 1961-1962 in a patient whose infection was resistant to the drug Methicillin, which was discovered in 1960.<ref>Millar B, Loughrey A, Elborn J, Moore J. Proposed definitions of community-associated meticillin-resistant Staphylococcus aureus (CA-MRSA). Journal of Hospital Infection. 2007;67(2):109-113.</ref><ref>Skov R, Gudlaugsson O, Hardardottir H, Harthug S, Jakobsen T, Jørn Kolmos H et al. Proposal for common Nordic epidemiological terms and definitions for methicillin-resistant Staphylococcus aureus (MRSA). Scandinavian Journal of Infectious Diseases. 2008;40(6-7):495-502.</ref> The incidence of MRSA greatly increased in the United States in the 1980s and was especially emerging in patients who used intravenous drugs.K2 | [[Image:Definition of MRSA.jpg|left|MRSA infection.]]Methicillin-Resistant Staphylococcus Aureus (MRSA) is defined as a type of bacterial staph infection that is non-responsive to antibiotics normally prescribed to treat such infections.<ref name="K1">Mayo Clinic Staff. MRSA infection - Mayo Clinic [Internet]. Mayoclinic.org. 2016 [cited 1 April 2016]. Available from: http://www.mayoclinic.org/diseases-conditions/mrsa/basics/definition/con-20024479</ref> MRSA was first described in 1961-1962 in a patient whose infection was resistant to the drug Methicillin, which was discovered in 1960.<ref name="K2">Millar B, Loughrey A, Elborn J, Moore J. Proposed definitions of community-associated meticillin-resistant Staphylococcus aureus (CA-MRSA). Journal of Hospital Infection. 2007;67(2):109-113.</ref><ref name="K3">Skov R, Gudlaugsson O, Hardardottir H, Harthug S, Jakobsen T, Jørn Kolmos H et al. Proposal for common Nordic epidemiological terms and definitions for methicillin-resistant Staphylococcus aureus (MRSA). Scandinavian Journal of Infectious Diseases. 2008;40(6-7):495-502.</ref> The incidence of MRSA greatly increased in the United States in the 1980s and was especially emerging in patients who used intravenous drugs.<ref name="K2" /> | ||
The bacteria from which MRSA arises, staphylococcus aureus, is found in the skin and in the nostrils of one third of all people and do not show any symptoms of having been exposed to the bacteria. These carriers of the bacteria are then exposing the bacteria to all of the items that they touch as well as expelling it into the air where it will remain until the item is next cleaned.<ref>Robinson J, Edgley A, Morrell J. MRSA care in the community: why patient education matters. British Journal of Community Nursing. 2014;19(9):436-441.</ref> | The bacteria from which MRSA arises, staphylococcus aureus, is found in the skin and in the nostrils of one third of all people and do not show any symptoms of having been exposed to the bacteria. These carriers of the bacteria are then exposing the bacteria to all of the items that they touch as well as expelling it into the air where it will remain until the item is next cleaned.<ref name="K4">Robinson J, Edgley A, Morrell J. MRSA care in the community: why patient education matters. British Journal of Community Nursing. 2014;19(9):436-441.</ref> | ||
Most cases of MRSA occur in those who have recently been in a hospital, work in a healthcare setting, or have had a recent surgery. This is known as hospital-acquired MRSA (HA-MRSA). K1 | Most cases of MRSA occur in those who have recently been in a hospital, work in a healthcare setting, or have had a recent surgery. This is known as hospital-acquired MRSA (HA-MRSA).<ref name="K1" /><ref name="K2" /> Other cases of MRSA are known as community-assiciated MRSA (CA-MRSA) or non-HA-MRSA.<ref name="K1" /><ref name="K2" /> This occurs when the infection has no correlation with a hospital setting and affects otherwise healthy individuals. CA-MRSA is spread from skin to skin contact and poor hygiene practices. At risk populations for CA- MRSA include high school athletes, childcare workers, prisoners, and those who live in crowded conditions.<ref name="K1" /><ref name="K2" /> CA-MRSA has emerged globally and is “now endemic within the USA.” <ref name="K2" /><br> | ||
== Prevalence == | == Prevalence == | ||
Revision as of 23:33, 9 April 2016
Original Editors - Students from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Kory Reynolds, Sarah Tassinari, Lucinda hampton, Elaine Lonnemann, 127.0.0.1, Kim Jackson, Evan Thomas, WikiSysop and Nupur Smit Shah
Definition/Description[edit | edit source]
Methicillin-Resistant Staphylococcus Aureus (MRSA) is defined as a type of bacterial staph infection that is non-responsive to antibiotics normally prescribed to treat such infections.[1] MRSA was first described in 1961-1962 in a patient whose infection was resistant to the drug Methicillin, which was discovered in 1960.[2][3] The incidence of MRSA greatly increased in the United States in the 1980s and was especially emerging in patients who used intravenous drugs.[2]
The bacteria from which MRSA arises, staphylococcus aureus, is found in the skin and in the nostrils of one third of all people and do not show any symptoms of having been exposed to the bacteria. These carriers of the bacteria are then exposing the bacteria to all of the items that they touch as well as expelling it into the air where it will remain until the item is next cleaned.[4]
Most cases of MRSA occur in those who have recently been in a hospital, work in a healthcare setting, or have had a recent surgery. This is known as hospital-acquired MRSA (HA-MRSA).[1][2] Other cases of MRSA are known as community-assiciated MRSA (CA-MRSA) or non-HA-MRSA.[1][2] This occurs when the infection has no correlation with a hospital setting and affects otherwise healthy individuals. CA-MRSA is spread from skin to skin contact and poor hygiene practices. At risk populations for CA- MRSA include high school athletes, childcare workers, prisoners, and those who live in crowded conditions.[1][2] CA-MRSA has emerged globally and is “now endemic within the USA.” [2]
Prevalence[edit | edit source]
According to the 2012 US Census Data[5]
- Non-Dialysis Patients: 65,296
- Dialysis Patients: 14,041
- TOTAL 75,309
Characteristics/Clinical Presentation[edit | edit source]
add text here
Associated Co-morbidities[edit | edit source]
Characteristics of Patients at Time of Detection/Identification of MRSA[6][7]
- Heart Disease
- Asthma
- Diabetes Mellitus
- End-Stage Renal Disease
- End-Stage Liver Disease
- Immunocompromised, Non-cancer
- Solid-Organ Cancer
- Hematologic Malignancy
Medications[edit | edit source]
add text here
Diagnostic Tests/Lab Tests/Lab Values[edit | edit source]
Clinical Laboratories for MRSA, according to the Clinical and Laboratory Standards Institute (CLSI)[8]
Broth Microdultion Testing with the addition of one of the following:
- A plate containing 6 μg/ml of oxacillin in Mueller-Hinton agar supplemented with 4% NaCl as alternative methods of testing for MRSA
- Latex Agglutination Test for PBP2 - tests for the mecA gene (Staphylococcal resistance to oxacillin/methicillin happens when an altered penicillin-binding protein, PBP2a, is produced.)
- Cefoxitin Disk Screen Test
Typically the broth test and agar test are the main tests for detecting MRSA, and the cefoxitin disk screen test can be used as a back-up test.
Interpretation of Susceptibility of Staphylococci to Oxacillin
| Susceptible | Resistant | |
| Oxacillin MIC Test | S. Aureus ≤ 2 μg/ml CoNS ≤ 0.25 μg/ml |
S. Aureus ≥ 4 μg/ml CoNS ≥0.5 μg/ml |
| Cefoxitin MIC Test | S. Aureus ≤ 4 μg/ml CoNS N/A |
S. Aureus ≥ 8 μg/ml CoNS N/A |
| Cefoxitin Disk Diffusion Test | S. Aureus ≥ 22 mm CoNS ≥ 25 mm |
S. Aureus ≤ 21 mm CoNS ≤ 24 mm |
• Detecting oxacillin/methicillin resistance can be difficult because of the presence of multiple populations (susceptible and resistant) may coexist within one culture of staphylococci.
• Oxacillin and cefoxitin are tested instead of methicillin because methicillin isn’t as readily available in the US as it once was. Oxacillin detects subpopulations well and cefoxitin activates mecA gene better, making it a more accurate test than other using oxacillin.
• Methicillin and oxacillin are in the same class of drugs. Methicillin has historically been the drug of choice for detecting resistance, hence the name MRSA. Even though the preferred drug of choice for testing has changed, the name had remained the same.
According to Centers for Disease Control and Prevention, there are additional tests to detect oxacillin/methicillin resistance but the most common and reliable tests have been listed above.
Etiology/Causes[edit | edit source]
add text here
Systemic Involvement[edit | edit source]
MRSA Infection may affect but are not limited to:[9]
- Bloodstream
- Lungs
- Heart
- Bones
- Joints
Please refer to the ‘Characteristics/Clinical Presentation’ section for more information on the associated signs and symptoms.
Medical Management (current best evidence)[edit | edit source]
add text here
Physical Therapy Management (current best evidence)[edit | edit source]
MRSA is not primarily managed by physical therapy. Instead it is the physical therapist’s role to identify comorbidities that are inhibiting functional activity and treat the patient’s symptoms. When treating a patient with MRSA, it’s important for the physical therapist to know proper disinfecting techniques to prevent the spread of the disease. Precautions to be taken when treating a patient with MRSA include but are not limited to:[10][11][12]
- Buy disinfectants that are registered by the Environmental Protection Agency (EPA)
- Note how to properly apply each product, how long it needs to be left on the surface, if the surface needs to be rinsed prior, if it’s only for specific surfaces, etc.
- Laundering specific clothes, towels and linens separately would be appropriate but not always necessary – wash and dry in the warmest temperate recommended on each piece of linen individually
- All surfaces ad equipment that came in contact with the patient should be cleaned, sometimes individual equipment for the patient with MRSA may be necessary if equipment cannot be properly cleaned
- Use barriers between the patient’s skin and surface when possible
- Physical therapist should wash body parts immediately after making contact with patient’s skin
- Patient should keep all open wounds clean and covered at all times until healed
Differential Diagnosis[edit | edit source]
add text here
Case Reports/ Case Studies[edit | edit source]
Hörner A, Hörner R, Salla A, Nunes M, Garzon L, Rampelotto R et al. Staphylococcal scalded skin syndrome in a premature newborn caused by methicillin-resistant Staphylococcus aureus: case report. Sao Paulo Med J. 2015;133(5):450-453.
Braich P, Aggarwal S, Mukhtar, BA S, Almeida D. Nosocomial keratitis caused by methicillin-resistant Staphylococcus aureus : case report and preventative measures. Journal of Community Hospital Internal Medicine Perspectives. 2015;5(5).
Resources[edit | edit source]
add appropriate resources here
Recent Related Research (from Pubmed)[edit | edit source]
References[edit | edit source]
see adding references tutorial.
- ↑ 1.0 1.1 1.2 1.3 Mayo Clinic Staff. MRSA infection - Mayo Clinic [Internet]. Mayoclinic.org. 2016 [cited 1 April 2016]. Available from: http://www.mayoclinic.org/diseases-conditions/mrsa/basics/definition/con-20024479
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Millar B, Loughrey A, Elborn J, Moore J. Proposed definitions of community-associated meticillin-resistant Staphylococcus aureus (CA-MRSA). Journal of Hospital Infection. 2007;67(2):109-113.
- ↑ Skov R, Gudlaugsson O, Hardardottir H, Harthug S, Jakobsen T, Jørn Kolmos H et al. Proposal for common Nordic epidemiological terms and definitions for methicillin-resistant Staphylococcus aureus (MRSA). Scandinavian Journal of Infectious Diseases. 2008;40(6-7):495-502.
- ↑ Robinson J, Edgley A, Morrell J. MRSA care in the community: why patient education matters. British Journal of Community Nursing. 2014;19(9):436-441.
- ↑ Centers for Disease Control and Prevention. MRSA Tracking. http://www.cdc.gov/mrsa/tracking/index.html (accessed 7 April 2016).
- ↑ Huang S, Hinrichsen V, Datta R, Spurchise L, Miroshnik I, Nelson K et al. Methicillin-Resistant Staphylococcus aureus Infection and Hospitalization in High-Risk Patients in the Year following Detection. PLoS ONE. 2011;6(9):e24340. http://journals.plos.org/plosone/article/asset?id=10.1371%2Fjournal.pone.0024340.PDF (accessed 8 April 2016).
- ↑ Datta R, Huang S. Risk of Infection and Death due to Methicillin‐Resistant Staphylococcus aureus in Long‐Term Carriers. Clinical Infectious Diseases. 2008;47(2):176-181. http://cid.oxfordjournals.org/content/47/2/176.full.pdf+html (accessed 8 April 2016).
- ↑ Centers for Disease Control and Prevention. Laboratory Testing for MRSA. http://www.cdc.gov/mrsa/lab/ (accessed 8 April 2016).
- ↑ MedlinePlus Medical Encyclopedia. MRSA. https://www.nlm.nih.gov/medlineplus/ency/article/007261.htm (accessed 7 April 2016).
- ↑ Centers for Disease Control and Prevention. Environmental Cleaning. http://www.cdc.gov/mrsa/community/environment/index.html (accessed 7 April 2016).
- ↑ Centers for Disease Control and Prevention. Cleaning & Disinfecting Athlete Facilities. http://www.cdc.gov/mrsa/community/environment/athletic-facilities.html (accessed 8 April 2016).
- ↑ Centers for Disease Control and Prevention. Laundry. http://www.cdc.gov/mrsa/community/environment/laundry.html (accessed 8 April 2016).