Goal Attainment Scaling
Original Editor - Lauren Heydenrych
Top Contributors - Lauren Heydenrych
Introduction[edit | edit source]
The Shirley Ryan Abilitylab defines Goal Attainment Scaling or GAS as "an individualized outcome measure involving goal selection and goal scaling that is standardized in order to calculate the extent to which a patient's goals are met."[1]
GAS is a goal-setting technique which has a mathematical basis.[2] GAS was first introduced in the 1960s by Kirusek and Sherman. This was originally for the mental health setting. Since then it has been adapted and modified to include a variety of areas and settings.[3]
GAS is important, as it allows the various stakeholders in the rehabilitation process - and primarily the patient - involvement in the measurement and scoring of goals. GAS gives individuals the ability to construct their own outcome measures; this is in contrast to measures that are based on a standard set of tasks. Scoring, however, is performed in a standardised way which in turn allows for statistical analysis.[3]
Advantages in using GAS[edit | edit source]
- Encourages communication and collaboration between multidisciplinary team members.[2]
- Promotes patient involvement. In research cited by Turner-Stokes (2009) goals for rehabilitation are more likely achieved with the involvement of the patient and their family. In addition, more information sharing is noted at the beginning of a rehabilitation process when formalised goal setting is introduced. This in turn allows for negotiation of realistic goals.[2]
Criticisms of GAS[edit | edit source]
- Potential for bias: For example, goals being too easy to attain or measuring change which does not actually occur.[4]
- Lack of interrater reliability. This however improved with training into goal setting and rating. As well as the use of multiple raters.[4]
- A time consuming process. Cited as taking as long as 45 minutes per child in the paediatric setting.[4]
Diagnosis/Conditions which can use GAS[edit | edit source]
- Brain injury
- Cerebral Palsy
- Pain management
- Parkinson's' Disease
- Neurologic Rehabilitation
- Sports and Musculoskeletal
Assessment type[edit | edit source]
Patient-reported outcomes
Description[edit | edit source]
GAS comprises of goals divided into a 5-point scale from -2 to +2.[3]
- Achievement of goal = 0
- Achieved somewhat more than expected outcome = +1
- Achievement of much more than expected goal = +2
- Achievement of somewhat less than expected goal = -1
- Achievement of much less than expected goal = -2
As some goals may be more difficult to achieve than others and some may be more important than others, the option of weighing different goals is a possibility. A spreadsheet to help calculate goals scores, including their weighting can be found at various sites, including Assesschild.com (found in the resources list at the bottom of the page).[3]
There is no set limit to how many or how few goals can be set at any one time. However, it is recommended that 3 is a good number and a maximum of 6 is set.[2]
Procedure[edit | edit source]
1. Identify goals[3]
- Interview patient and/or caregivers to identify a) problem areas and b) priority areas
- Decide on a date of achievement
- Note: Goals should follow the SMART principle.
- Specific, Measurable, Attainable, Realistic and Time-related.
2.Weight goals[3]
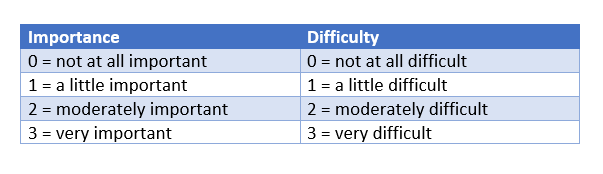
- Done by patient ranking goals by importance or using a weighing scale. Here the team may rank or weigh goals by the expected difficulty in achieving them.
Weight = importance × difficulty
3. Define the expected outcome[3]
- Assign descriptors of results in each case of -2 up to +2. Each level should be as objective and observable as possible.
- This is an opportunity to address unrealistic expectations which may be held by the patient and/or caregivers.
4. Scoring baseline and interval scoring[3][4]
- Usually, baseline scores are rated at -1, unless there is no clinically plausible worse conditionn. In the case of such, -2 is rated. With intervals, it is important that the scaling between each level is as equal as possible. Ideally when change is measured, it is also important that there is only 1 variable of change per scale level. Only when the goal does not remain clinically meaningful, can 2 or more variables be changed within a scale. However, improvement should not be expected to occur simultaneously on these scales. For example:
Goal - Writing letters with assistance of caregiver.
- -2 = Unable to write name, even with assistance.
- -1 = Writes 5 letter with hands-on assistance and verbal cuing given by caregiver.
- 0 = Writes 10 letters with hands-on assistance and verbal cuing by caregiver.
- 1 = Writes 10 letters with verbal cuing
- 2 = Writes 10 letters independently.
In this example, the variables that changed were a. the number of letters written (5 to 10) and b. assistance given (Namely, hands-on, then verbal cueing, then none). While both variables changed in the scale, only 1 variable changed at a time between scale levels.
5. Goal attainment scaling[3]
Goals are reviewed at appointed dates. Here, actual performance is judged at defined levels. The ideal is to have this is performed with the team - including the family.
Baseline scores are compared with currently performed tasks.
The use of weighted values are used within a formula in order to get a standardised score. An excel spreadsheet with the formula can be found on the Assesschild website. A link is found in the resource section.
Otherwise, baseline scores can simply be compared to scores achieved on follow-up, to monitor development or deterioration.
GAS in the ICF context[edit | edit source]
The ICF or International Classification of Functioning, Disability and Health, developed by the World Health Organization (WHO) is a classification and measurement system of health and health-related domains. It is a framework measuring health and disability from an individual level through to the social and environmental aspects of functioning.[6]The language of the ICF is standardised to allow communication about health information across the world, disciplines and sciences.[7]
When it comes to goal setting, an article by McDougall and Wright (2009)[7] pointed to the fact that goal setting within the rehabilitative environment often focused on impairment-based goals, driven by the health care provider and tended to focus less on aspects of activity and participation. using an assessment tool that was driven by the needs of the patient resulted in more goals geared towards activity and participation. GAS is an ideal tool in this regard.
McDougall and Wright suggested that the ICF-CY, an extension of the ICF for focus on children and youth, was an ideal companion for GAS. The ICF-CY is a good initiator in identifying aspects to focus goal setting, as it encompasses the various levels of functioning. The ICF views health and functioning within environmental and social contexts, meaning that goals are not limited to impairments and physical limitations. This gives an opportunity for interdisciplinary work and an overall holistic view of the clients challenges. It further provides opportunities for families and clients to actively engage in goal setting, orientating health care and other professionals as to what is most important for the client.
Once areas requiring intervention are established, GAS can be used to bring broad, self-defined goals of the client or the family to clear and distinct goals.[7]
Complimentary aspects of both the ICF and GAS include:
- Both systems allow for difference in ability and are orientated towards the individual.
- When using the ICF-CY in particular, both systems facilitate assessment over time, taking into account short and long term goal setting. Short term addressing more of the impairment and activity limitation and long term addressing more of the participation issues.
- Sets of goals monitored over time and taking account of environmental changes help identify environmental impact on outcomes. This makes goals more holistic and family centered.
Reliability[edit | edit source]
In the analysis of systematic reviews within the last decade, it was found that inter-rater reliability (IRR) was good, but varied according to a number of factors including:[8]
- The person scoring - IRR improved when the physician or therapist treating the patient as well as the raters observed the patient directly, instead of a recording being watched.
- Field in question
- Precision of levels described
One study performed by Mailloux et al. (2007) recommended training programs and testing of inter-rater reliability to improve this aspect.[9]
A study performed by King et al (2000) found that IRR could be high (ICC=0.98) when performed at the same occasion [10]
Intra-rater reliability has not been commented on.
Validity[edit | edit source]
One of the criticisms of GAS is that it doesn't measure one clear construct. This is because of the individualistic nature of the goal setting. This makes validity difficult to assess. Despite this, research done in 2016[11] found that content validity produced results that were "good" or "intermediate".
Resources[edit | edit source]
- Goal Attainment Scaling (GAS) in Rehabilitation. A practical guide.
- GAS manual (paediatric orientated)
- GAS at Assesschild.com
- Page at Shirly Ryan Ability Lab website: https://www.sralab.org/rehabilitation-measures/goal-attainment-scale
References[edit | edit source]
- ↑ Shirley Ryan Ability Lab. Goal Attainment Scale. Available from: https://www.sralab.org/rehabilitation-measures/goal-attainment-scale (accessed 09/11/2022)
- ↑ 2.0 2.1 2.2 2.3 Turner-Stokes L. Goal attainment scaling (GAS) in rehabilitation: a practical guide. Clinical rehabilitation. 2009 Apr;23(4):362-70.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 Turner-Stokes L. Goal Attainment Scaling (GAS) in rehabilitation: A practical guide. Clinical Rehabilitation. 2009 Feb [cited 2022 Nov 15];23: 362. Available from: DOI: 10.1177/0269215508101742
- ↑ 4.0 4.1 4.2 4.3 McDougall J, Wright V. The ICF-CY and Goal Attainment Scaling: Benefits of their combined use for pediatric practice. Disability and Rehabilitation. 2009 Jan 1;31(16):1362-72.
- ↑ Ardea Outcomes Inc. How does Goal Attainment Scaling work?. Available from: https://www.youtube.com/watch?v=MCzu0h43cqo [last accessed 17/11/2022]
- ↑ World Health Organisation. International Classification of Functioning, Disability and Health (ICF). Available from: https://www.who.int/standards/classifications/international-classification-of-functioning-disability-and-health (accessed 29/12/2022)
- ↑ 7.0 7.1 7.2 McDougall J, Wright V. The ICF-CY and Goal Attainment Scaling: Benefits of their combined use for pediatric practice. Disability and Rehabilitation. 2009 Jan 1;31(16):1362-72.
- ↑ Assesschild. Standardized Assessments for the Management of Children with Motor Disorders. Goal Attainment Scale (GAS). Available from: https://assesschild.com/goal-attainment-scale (accessed 16/11/2022)
- ↑ Mailloux Z, May-Benson TA, Summers CA, Miller LJ, Brett-Green B, Burke JP, Cohn ES, Koomar JA, Parham LD, Roley SS, Schaaf RC. Goal attainment scaling as a measure of meaningful outcomes for children with sensory integration disorders. The American Journal of Occupational Therapy. 2007 Mar;61(2):254-9.
- ↑ King GA, McDougall J, Palisano RJ, Gritzan J, Tucker MA. Goal attainment scaling: its use in evaluating pediatric therapy programs. Physical & Occupational Therapy in Pediatrics. 2000 Jan 1;19(2):31-52.
- ↑ Gaasterland CM, Jansen-van der Weide MC, Weinreich SS, van der Lee JH. A systematic review to investigate the measurement properties of goal attainment scaling, towards use in drug trials. BMC medical research methodology. 2016 Dec;16(1):1-22.