A New Protocol for Plantar Heel Pain: Difference between revisions
No edit summary |
No edit summary |
||
| Line 28: | Line 28: | ||
* Single leg mini squat (half squat) | * Single leg mini squat (half squat) | ||
[[File:PHPS reproduction exercises.jpg|frameless|305x305px]]Figure 1. Two clinical tests reproducing PHP | |||
Figure 1. Two clinical tests reproducing PHP | |||
This raised the question of why these tests would provoke pain in the heel (Figure 2) <ref name=":4" />. Considering that PHPS is associated with weight-bearing, could the reproduction of the pain be attributed to an increase in weight-bearing? Yet, looking at the motions, the weight is shifted from the heel to the forefoot which means reduced weight-bearing on the heel. If not because of increased weight-bearing, could these tests then be causing an increase in stress in the plantar fascia? But once again if analysing the motions during the test, during the: | This raised the question of why these tests would provoke pain in the heel (Figure 2) <ref name=":4" />. Considering that PHPS is associated with weight-bearing, could the reproduction of the pain be attributed to an increase in weight-bearing? Yet, looking at the motions, the weight is shifted from the heel to the forefoot which means reduced weight-bearing on the heel. If not because of increased weight-bearing, could these tests then be causing an increase in stress in the plantar fascia? But once again if analysing the motions during the test, during the: | ||
| Line 36: | Line 35: | ||
* Single leg mini squat, dorsiflexion of the ankle will increase fascial tension which is again reduced by flexion of the knee <ref name=":4" />. | * Single leg mini squat, dorsiflexion of the ankle will increase fascial tension which is again reduced by flexion of the knee <ref name=":4" />. | ||
If there is then an increase in fascial tension, it will be minimal considering how movements cancel each other out. | If there is then an increase in fascial tension, it will be minimal considering how movements cancel each other out. | ||
[[File:Reasoning for PHP provocation by tests.jpg|frameless]] | |||
Figure 2. Proposed reasons for the pain provocation in the heel | Figure 2. Proposed reasons for the pain provocation in the heel | ||
Following these findings, Saban & Masharawi <ref name=":3" /> investigated if these tests were able to reproduce heel pain in a larger population, and conducted a clinical trial involving 40 patients with a typical presentation of PHP (Figure 3) <ref name=":4" />. | Following these findings, Saban & Masharawi <ref name=":3" /> investigated if these tests were able to reproduce heel pain in a larger population, and conducted a clinical trial involving 40 patients with a typical presentation of PHP (Figure 3) <ref name=":4" />. | ||
[[File:Inclusion criteria for study by Saban and Masharawi 2017.jpg|frameless|450x450px]] | |||
Figure 3. Inclusion criteria for participants in the trial assessing the reliability of three clinical tests for assessing PHP <ref name=":3" /><ref name=":4" /> | Figure 3. Inclusion criteria for participants in the trial assessing the reliability of three clinical tests for assessing PHP <ref name=":3" /><ref name=":4" /> | ||
| Line 45: | Line 48: | ||
Three tests were included in the study - the single-leg static stance test, single-leg half squat and the single-leg heel raise with test measures as described in Figure 4 <ref name=":3" /><ref name=":4" />. | Three tests were included in the study - the single-leg static stance test, single-leg half squat and the single-leg heel raise with test measures as described in Figure 4 <ref name=":3" /><ref name=":4" />. | ||
[[File:Description of clinical tests used for Ax of PHPS.jpg|frameless|500x500px]] | |||
Figure 4. Description of the clinical tests used <ref name=":3" /><ref name=":4" />. P1 refers to the appearance of pain. | Figure 4. Description of the clinical tests used <ref name=":3" /><ref name=":4" />. P1 refers to the appearance of pain. | ||
| Line 54: | Line 60: | ||
Figure 5. Outcome measures utilised <ref name=":3" /><ref name=":4" /> | |||
[[File:Outcome measures in Saban and Mashawari 2017.jpg|frameless|450x450px]] | |||
'''Figure 5'''. Outcome measures utilised <ref name=":3" /><ref name=":4" /> | |||
The aims of this study were to investigate whether | The aims of this study were to investigate whether | ||
| Line 64: | Line 73: | ||
The procedure of the study involved an interview and completion of the functional status questionnaire by the patient, followed by an assessment of the patient by Rater 1 using the three clinical tests and a re-assessment of the same tests 30 minutes later by Rater 2 as a measurement of the interrater reliability of the tests. The patient was reassessed by Rater 1 one week later in order to establish the intrarater reliability of the clinical tests (Figure 6) <ref name=":3" />. | The procedure of the study involved an interview and completion of the functional status questionnaire by the patient, followed by an assessment of the patient by Rater 1 using the three clinical tests and a re-assessment of the same tests 30 minutes later by Rater 2 as a measurement of the interrater reliability of the tests. The patient was reassessed by Rater 1 one week later in order to establish the intrarater reliability of the clinical tests (Figure 6) <ref name=":3" />. | ||
Figure 6. The procedure of the clinical trial <ref name=":3" /><ref name=":4" /> | [[File:Study procedure Saban and Masharawi 2017.jpg|frameless|450x450px]] | ||
'''Figure 6'''. The procedure of the clinical trial <ref name=":3" /><ref name=":4" /> | |||
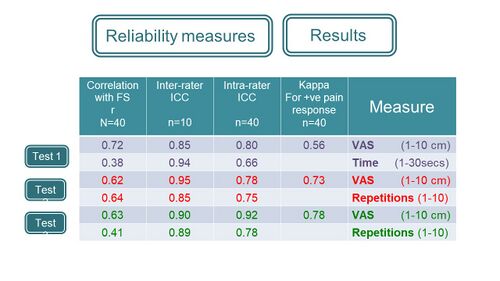
Moderate to high levels of interrater and intrarater reliability were reported for all the tests and a correlation was reported between the level of pain (VAS) and the functional scale (LEFS) (Figure 7) <ref name=":3" />. | Moderate to high levels of interrater and intrarater reliability were reported for all the tests and a correlation was reported between the level of pain (VAS) and the functional scale (LEFS) (Figure 7) <ref name=":3" />. | ||
Figure 7. Reliability indices for the clinical tests <ref name=":3" /><ref name=":4" /> | [[File:Reliability of the measures used in Saban and Masharawi 2017.jpg|frameless|500x500px]] | ||
'''Figure 7'''. Reliability indices for the clinical tests <ref name=":3" /><ref name=":4" /> | |||
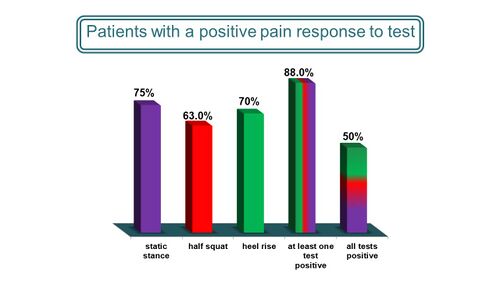
The results of the frequency of a positive pain response for each individual test as well as a combination of the tests can be found in Figure 8 <ref name=":3" /><ref name=":4" />. | The results of the frequency of a positive pain response for each individual test as well as a combination of the tests can be found in Figure 8 <ref name=":3" /><ref name=":4" />. | ||
Figure 8. Frequency of a positive pain response for the clinical tests | [[File:Frequency of positive pain response Saban and Masharawi 2017.jpg|frameless|500x500px]] | ||
'''Figure 8'''. Frequency of a positive pain response for the clinical tests | |||
It is important to also mention that some of the patients only experienced pain towards the end of the testing protocol, which indicates that many repetitions might be needed in order to reproduce the patient’s pain. | It is important to also mention that some of the patients only experienced pain towards the end of the testing protocol, which indicates that many repetitions might be needed in order to reproduce the patient’s pain. | ||
| Line 80: | Line 95: | ||
Considering the presence of pain in the heel with PHPS, the source of pain has often been assumed to be at the level of the heel, which is a prime example of the thought distortions described by Daniel Kahneman when he posed his quiz question (Figure 9) <ref name=":5">Kahneman D. [https://www.amazon.com/Thinking-Fast-Slow-Daniel-Kahneman/dp/0374533555 Thinking, fast and slow]. New York: Farrar, Straus & Giroux. 2011.</ref>. If one opens the mind and looks further, it becomes clear that the pain experienced in PHPS might not be in the heel after all <ref name=":4" />. | Considering the presence of pain in the heel with PHPS, the source of pain has often been assumed to be at the level of the heel, which is a prime example of the thought distortions described by Daniel Kahneman when he posed his quiz question (Figure 9) <ref name=":5">Kahneman D. [https://www.amazon.com/Thinking-Fast-Slow-Daniel-Kahneman/dp/0374533555 Thinking, fast and slow]. New York: Farrar, Straus & Giroux. 2011.</ref>. If one opens the mind and looks further, it becomes clear that the pain experienced in PHPS might not be in the heel after all <ref name=":4" />. | ||
[[File:Quiz question Daniel Kahneman.jpg|frameless|500x500px]]'''Figure 9'''. Quiz question by Daniel Kahneman <ref name=":4" /><ref name=":5" /> | |||
Figure 9. Quiz question by Daniel Kahneman <ref name=":4" /><ref name=":5" /> | |||
== Treatment Protocol for PHP == | == Treatment Protocol for PHP == | ||
Similar to the literature on assessment tools for PHPS, no definite conclusions have been made for the treatment of PHPS due to a lack of high-quality evidence <ref name=":0" /><ref name=":1" /><ref name=":2" /><ref name=":3" /><ref>Rasenberg N, Bierma-Zeinstra SM, Bindels PJ, van der Lei J, van Middelkoop M. [https://bjgp.org/content/bjgp/69/688/e801.full.pdf Incidence, prevalence, and management of plantar heel pain: a retrospective cohort study in Dutch primary care]. British Journal of General Practice. 2019 Nov 1;69(688):e801-8. </ref>. Hence, following the discussion on the assessment of PHP, it is necessary to raise the question of how then to progress to the treatment thereof. If the provocation of the heel pain is not from an increase in weight-bearing or fascial stress, could it then be due to a contraction of the calf muscle considering that the | Similar to the literature on assessment tools for PHPS, no definite conclusions have been made for the treatment of PHPS due to a lack of high-quality evidence <ref name=":0" /><ref name=":1" /><ref name=":2" /><ref name=":3" /><ref>Rasenberg N, Bierma-Zeinstra SM, Bindels PJ, van der Lei J, van Middelkoop M. [https://bjgp.org/content/bjgp/69/688/e801.full.pdf Incidence, prevalence, and management of plantar heel pain: a retrospective cohort study in Dutch primary care]. British Journal of General Practice. 2019 Nov 1;69(688):e801-8. </ref>. Hence, following the discussion on the assessment of PHP, it is necessary to raise the question of how then to progress to the treatment thereof. If the provocation of the heel pain is not from an increase in weight-bearing or fascial stress, could it then be due to a contraction of the calf muscle considering that the | ||
| Line 92: | Line 105: | ||
Manual palpation of the plantar flexor muscles in the posterior calf on the affected leg in patients with PHPS revealed stiff, incompliant and painful soft tissue <ref name=":6">Saban B, Deutscher D, Ziv T. [https://www.sciencedirect.com/science/article/abs/pii/S1356689X13001471?via%3Dihub Deep massage to posterior calf muscles in combination with neural mobilization exercises as a treatment for heel pain: a pilot randomized clinical trial]. Manual Therapy. 2014 Apr 1;19(2):102-8. </ref>. Following the lack of evidence for the effective treatment of PHPS, a treatment protocol directed at the posterior calf muscles was proposed by Saban et al <ref name=":6" />. The aim of their study was to compare deep soft tissue massage to the posterior calf with muscles to a more common treatment approach directed to the area of the heel (Figure 10) <ref name=":6" />. | Manual palpation of the plantar flexor muscles in the posterior calf on the affected leg in patients with PHPS revealed stiff, incompliant and painful soft tissue <ref name=":6">Saban B, Deutscher D, Ziv T. [https://www.sciencedirect.com/science/article/abs/pii/S1356689X13001471?via%3Dihub Deep massage to posterior calf muscles in combination with neural mobilization exercises as a treatment for heel pain: a pilot randomized clinical trial]. Manual Therapy. 2014 Apr 1;19(2):102-8. </ref>. Following the lack of evidence for the effective treatment of PHPS, a treatment protocol directed at the posterior calf muscles was proposed by Saban et al <ref name=":6" />. The aim of their study was to compare deep soft tissue massage to the posterior calf with muscles to a more common treatment approach directed to the area of the heel (Figure 10) <ref name=":6" />. | ||
Figure 10. Aim of the study by Saban et al <ref name=":6" /> | [[File:Aim of study posterior calf treatment for PHPS Saban 2014.jpg|frameless|450x450px]] | ||
'''Figure 10'''. Aim of the study by Saban et al <ref name=":6" /> | |||
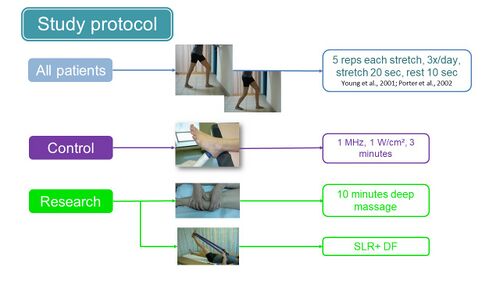
In their study, participants were divided into a study and a control group with the control group receiving a stretching protocol and ultrasound with commonly used settings, and the study group receiving the same stretching protocol but combined with deep tissue massage of the posterior calf muscles and a neural stretch (Figure 11) <ref name=":6" />. | In their study, participants were divided into a study and a control group with the control group receiving a stretching protocol and ultrasound with commonly used settings, and the study group receiving the same stretching protocol but combined with deep tissue massage of the posterior calf muscles and a neural stretch (Figure 11) <ref name=":6" />. | ||
Figure 11. Study protocol of the study by Saban et al <ref name=":6" /> | [[File:Study protocol Saban et al 2014.jpg|frameless|500x500px]] | ||
'''Figure 11'''. Study protocol of the study by Saban et al <ref name=":6" /> | |||
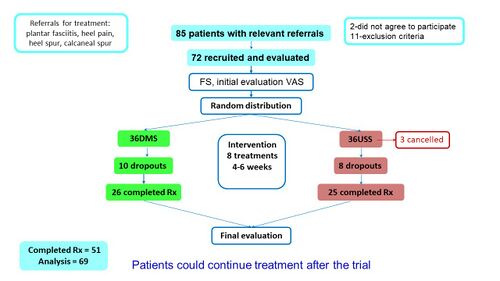
The outcome measures used in the study included a functional status questionnaire (computerised version of LEFS) as the primary outcome and the level of first-step pain in the morning (VAS) as a secondary measure <ref name=":6" />. A visual representation of the flow of patients through the study can be found in Figure 12 <ref name=":6" />. | The outcome measures used in the study included a functional status questionnaire (computerised version of LEFS) as the primary outcome and the level of first-step pain in the morning (VAS) as a secondary measure <ref name=":6" />. A visual representation of the flow of patients through the study can be found in Figure 12 <ref name=":6" />. | ||
Figure 12. Flow of patients through the study by Saban et al <ref name=":6" /> | [[File:Flow of patients through study by Saban et al 2014.jpg|frameless|500x500px]] | ||
'''Figure 12'''. Flow of patients through the study by Saban et al <ref name=":6" /> | |||
The characteristics of the patients at baseline were also compared by groups to look for similarities between groups at baseline. No statistically significant differences were found between groups at baseline and patients displayed similar ages, similar chronicity of the problem and similar scores on the functional scale and VAS scale at intake (Figures 13 and 14) <ref name=":6" />. | The characteristics of the patients at baseline were also compared by groups to look for similarities between groups at baseline. No statistically significant differences were found between groups at baseline and patients displayed similar ages, similar chronicity of the problem and similar scores on the functional scale and VAS scale at intake (Figures 13 and 14) <ref name=":6" />. | ||
Figure | Figure 13. Baseline patient characteristics by treatment group | ||
Figure 14. Baseline patient characteristics by treatment group | |||
The outcome measures used in the study included a functional status questionnaire (computerised version of LEFS) as the primary outcome and the level of first-step pain in the morning (VAS) as a secondary measure (Saban 2014). A visual representation of the flow of patients through the study can be found in Figure 12 (Saban 2014). | The outcome measures used in the study included a functional status questionnaire (computerised version of LEFS) as the primary outcome and the level of first-step pain in the morning (VAS) as a secondary measure (Saban 2014). A visual representation of the flow of patients through the study can be found in Figure 12 (Saban 2014). | ||
Revision as of 17:42, 11 August 2021
Original Editor - Merinda Rodseth based on the course by
Bernice Saban
Top Contributors - Merinda Rodseth, Jess Bell, Kim Jackson and Rucha Gadgil
Introduction[edit | edit source]
The previous literature reviews on the risk factors, assessment tools and treatment options for plantar heel pain (PHP) identified a lack of support for any of the commonly used assessment and treatment options for PHP [1][2][3][4]. This highlighted the need for appropriate assessment and treatment tools to assess and manage PHP which led to the development of a new tool for PHP[5]. This protocol involves:
- an assessment tool
- manual therapy and
- exercises
A comprehensive physical examination is essential for the effective diagnosis and management of plantar heel pain syndrome (PHPS) and effective assessment tools are required.
Assessment Tools for Plantar Heel Pain[edit | edit source]
Assessment tools have over time become more sophisticated and technologically advanced but even these advancements did not aid in the effective assessment of PHP. Historically, physical examination tests have been an essential part of clinical assessments as they are more
- readily available
- less expensive
than diagnostic imaging methods [6].
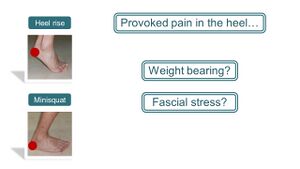
In pursuit of accurately assessing PHPS, two tests were found to reproduce the heel pain experienced by an individual with PHPS during a regular foot and ankle evaluation, namely the (Figure 1) [5]
- Single leg heel raise
- Single leg mini squat (half squat)
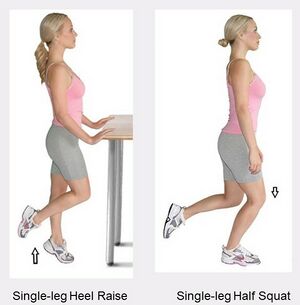 Figure 1. Two clinical tests reproducing PHP
Figure 1. Two clinical tests reproducing PHP
This raised the question of why these tests would provoke pain in the heel (Figure 2) [5]. Considering that PHPS is associated with weight-bearing, could the reproduction of the pain be attributed to an increase in weight-bearing? Yet, looking at the motions, the weight is shifted from the heel to the forefoot which means reduced weight-bearing on the heel. If not because of increased weight-bearing, could these tests then be causing an increase in stress in the plantar fascia? But once again if analysing the motions during the test, during the:
- Single leg heel raise, the increased extension of the toes might increase tension in the facia, but plantar flexion at the heel again reduces the tension
- Single leg mini squat, dorsiflexion of the ankle will increase fascial tension which is again reduced by flexion of the knee [5].
If there is then an increase in fascial tension, it will be minimal considering how movements cancel each other out.
Figure 2. Proposed reasons for the pain provocation in the heel
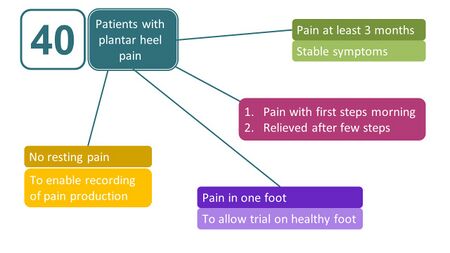
Following these findings, Saban & Masharawi [4] investigated if these tests were able to reproduce heel pain in a larger population, and conducted a clinical trial involving 40 patients with a typical presentation of PHP (Figure 3) [5].
Figure 3. Inclusion criteria for participants in the trial assessing the reliability of three clinical tests for assessing PHP [4][5]
Three tests were included in the study - the single-leg static stance test, single-leg half squat and the single-leg heel raise with test measures as described in Figure 4 [4][5].
Figure 4. Description of the clinical tests used [4][5]. P1 refers to the appearance of pain.
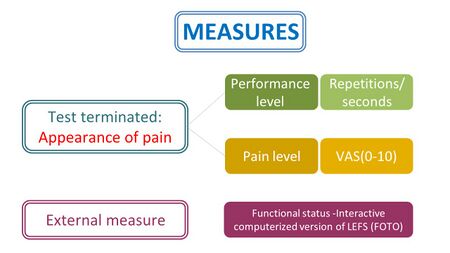
The measures used to assess the tests included (Figure 5):[4][5]
- the appearance of the first painful sensation (P1) assessed with the visual analogue scale (VAS) and including the level of achievement of the performance (repetitions/seconds)
- The functional status of the patient, measured using a computerised version of the Lower Extremity Functional Scale (LEFS)
Figure 5. Outcome measures utilised [4][5]
The aims of this study were to investigate whether
- these tests were reliable and valid in patients with PHPS
- Combining the three tests would enhance the possibility of a positive test response from each patient [4][5]
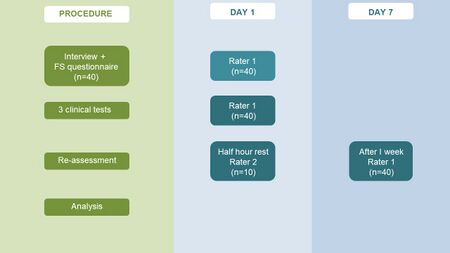
The procedure of the study involved an interview and completion of the functional status questionnaire by the patient, followed by an assessment of the patient by Rater 1 using the three clinical tests and a re-assessment of the same tests 30 minutes later by Rater 2 as a measurement of the interrater reliability of the tests. The patient was reassessed by Rater 1 one week later in order to establish the intrarater reliability of the clinical tests (Figure 6) [4].
Figure 6. The procedure of the clinical trial [4][5]
Moderate to high levels of interrater and intrarater reliability were reported for all the tests and a correlation was reported between the level of pain (VAS) and the functional scale (LEFS) (Figure 7) [4].
Figure 7. Reliability indices for the clinical tests [4][5]
The results of the frequency of a positive pain response for each individual test as well as a combination of the tests can be found in Figure 8 [4][5].
Figure 8. Frequency of a positive pain response for the clinical tests
It is important to also mention that some of the patients only experienced pain towards the end of the testing protocol, which indicates that many repetitions might be needed in order to reproduce the patient’s pain.
In conclusion on the assessment tools, the study by Saban & Masharawi [4] indicates the existence of simple, relevant and reliable clinical tests to use for patients with PHPS that are performance-based, easily applied and appropriate for the assessment of PHPS.
Considering the presence of pain in the heel with PHPS, the source of pain has often been assumed to be at the level of the heel, which is a prime example of the thought distortions described by Daniel Kahneman when he posed his quiz question (Figure 9) [7]. If one opens the mind and looks further, it becomes clear that the pain experienced in PHPS might not be in the heel after all [5].
 Figure 9. Quiz question by Daniel Kahneman [5][7]
Figure 9. Quiz question by Daniel Kahneman [5][7]
Treatment Protocol for PHP[edit | edit source]
Similar to the literature on assessment tools for PHPS, no definite conclusions have been made for the treatment of PHPS due to a lack of high-quality evidence [1][2][3][4][8]. Hence, following the discussion on the assessment of PHP, it is necessary to raise the question of how then to progress to the treatment thereof. If the provocation of the heel pain is not from an increase in weight-bearing or fascial stress, could it then be due to a contraction of the calf muscle considering that the
- heel raise test incorporates concentric contraction of the calve muscles and the
- half-squat test involves eccentric contraction of the calve muscles?
Manual palpation of the plantar flexor muscles in the posterior calf on the affected leg in patients with PHPS revealed stiff, incompliant and painful soft tissue [9]. Following the lack of evidence for the effective treatment of PHPS, a treatment protocol directed at the posterior calf muscles was proposed by Saban et al [9]. The aim of their study was to compare deep soft tissue massage to the posterior calf with muscles to a more common treatment approach directed to the area of the heel (Figure 10) [9].
Figure 10. Aim of the study by Saban et al [9]
In their study, participants were divided into a study and a control group with the control group receiving a stretching protocol and ultrasound with commonly used settings, and the study group receiving the same stretching protocol but combined with deep tissue massage of the posterior calf muscles and a neural stretch (Figure 11) [9].
Figure 11. Study protocol of the study by Saban et al [9]
The outcome measures used in the study included a functional status questionnaire (computerised version of LEFS) as the primary outcome and the level of first-step pain in the morning (VAS) as a secondary measure [9]. A visual representation of the flow of patients through the study can be found in Figure 12 [9].
Figure 12. Flow of patients through the study by Saban et al [9]
The characteristics of the patients at baseline were also compared by groups to look for similarities between groups at baseline. No statistically significant differences were found between groups at baseline and patients displayed similar ages, similar chronicity of the problem and similar scores on the functional scale and VAS scale at intake (Figures 13 and 14) [9].
Figure 13. Baseline patient characteristics by treatment group
Figure 14. Baseline patient characteristics by treatment group
The outcome measures used in the study included a functional status questionnaire (computerised version of LEFS) as the primary outcome and the level of first-step pain in the morning (VAS) as a secondary measure (Saban 2014). A visual representation of the flow of patients through the study can be found in Figure 12 (Saban 2014).
Figure 13. Baseline patient characteristics by treatment group [5][9]
Figure 14. Baseline patient characteristics by treatment group [5][9]
Completion rates were similar between groups and also corresponded to those of 2 other studies investigating similar aspects to the study (Figure 15) [9][10][11].
Figure 15. Treatment completion rates [9][10][11]
The results on the primary outcome of the study indicated that even though both groups improved on the functional scale, the deep massage group (DMS) improved by 15 points compared to the 6 point improvement in the Ultrasound/control (USS) group (Figure 16) [9]. Wang et al [12] indicated that a change of 8 points is needed for any change to be clinically significant and therefore, even though the USS improved statistically, there was no real clinical change whereas the DMS improved both statistically and clinically (Figure 16) [9].
Figure 16. Results of the functional scale scores [5][9]
The level of first-step pain in the morning (VAS) decreased similarly in both groups with no significant difference (Figure 17) [9]. This could indicate that the complaint of first-step pain in the morning might only be one part of PHPS and that patients have other functional limitations that were picked up by the functional scale score (LEFS) [5].
Figure 17. Results of VAS for first-step pain in the morning [5][9]
In the study by Saban et al [9], deep massage therapy to the posterior calf muscles and neural mobilisation combined with stretching exercises had superior short-term functional scale outcomes compared to ultrasound treatment with stretching exercises. This treatment protocol is easy to use and effective for PHP and could therefore be recommended for individuals with PHPS [5][9].
There are, however, some limitations to this study, including:[9]
- No record of daily self-exercise compliance
- Short-term results only
- DMS group performed one additional exercise (SLR with Dorsiflexion) thereby introducing an additional variable into the trial
This treatment approach is also supported by two other studies performed by Renan-Ordine et al [13] (Figure 18) and Ajimsha et al [14] (Figure 19). Renan-Ordine et al [13]suggested myofascial trigger point therapy of the calf for PHP but the results of the study are not that clear and the clinical effect is unknown (Figure 18). Amjisha et al [14] investigated the effect of myofascial release of the calf in PHP and found a clear difference between groups with the myofascial release group performing much better compared to the control sham ultrasound group (Figure 19).
Figure 18. Results of the study by Renan-Ordine et al [13][5]
Figure 19. Results of the study by Ajimsha et al [14][5]
Conclusion[edit | edit source]
This new protocol for the assessment and treatment of PHP is showing promising results for the management of PHPS [9][13][14][15]. The next lecture in this series will investigate the anatomical features behind this protocol followed by details on how to apply this technique and manage a treatment session with a patient.
References[edit | edit source]
- ↑ 1.0 1.1 Morrissey D, Cotchett M, J'Bari AS, Prior T, Griffiths IB, Rathleff MS, Gulle H, Vicenzino B, Barton CJ. Management of plantar heel pain: a best practice guide informed by a systematic review, expert clinical reasoning and patient values. British Journal of Sports Medicine. 2021 Mar 30.
- ↑ 2.0 2.1 Salvioli S, Guidi M, Marcotulli G. The effectiveness of conservative, non-pharmacological treatment, of plantar heel pain: a systematic review with meta-analysis. The Foot. 2017 Dec 1;33:57-67.
- ↑ 3.0 3.1 Babatunde OO, Legha A, Littlewood C, Chesterton LS, Thomas MJ, Menz HB, van der Windt D, Roddy E. Comparative effectiveness of treatment options for plantar heel pain: a systematic review with network meta-analysis. British Journal of Sports Medicine. 2019 Feb 1;53(3):182-94.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 4.13 4.14 Saban B, Masharawi Y. Three single leg standing tests for clinical assessment of chronic plantar heel pain syndrome: static stance, half-squat and heel rise. Physiotherapy. 2017 Jun 1;103(2):237-44.
- ↑ 5.00 5.01 5.02 5.03 5.04 5.05 5.06 5.07 5.08 5.09 5.10 5.11 5.12 5.13 5.14 5.15 5.16 5.17 5.18 5.19 5.20 5.21 5.22 5.23 Bernice Saban 2021. A New Protocol for Plantar Heel Pain. Physioplus Course. 2021
- ↑ Schwieterman B, Haas D, Columber K, Knupp D, Cook C. Diagnostic accuracy of physical examination tests of the ankle/foot complex: a systematic review. International journal of sports physical therapy. 2013 Aug;8(4):416.
- ↑ 7.0 7.1 Kahneman D. Thinking, fast and slow. New York: Farrar, Straus & Giroux. 2011.
- ↑ Rasenberg N, Bierma-Zeinstra SM, Bindels PJ, van der Lei J, van Middelkoop M. Incidence, prevalence, and management of plantar heel pain: a retrospective cohort study in Dutch primary care. British Journal of General Practice. 2019 Nov 1;69(688):e801-8.
- ↑ 9.00 9.01 9.02 9.03 9.04 9.05 9.06 9.07 9.08 9.09 9.10 9.11 9.12 9.13 9.14 9.15 9.16 9.17 9.18 9.19 9.20 9.21 9.22 Saban B, Deutscher D, Ziv T. Deep massage to posterior calf muscles in combination with neural mobilization exercises as a treatment for heel pain: a pilot randomized clinical trial. Manual Therapy. 2014 Apr 1;19(2):102-8.
- ↑ 10.0 10.1 Bezalel T, Carmeli E, Katz-Leurer M. The effect of a group education programme on pain and function through knowledge acquisition and home-based exercise among patients with knee osteoarthritis: a parallel randomised single-blind clinical trial. Physiotherapy. 2010 Jun 1;96(2):137-43.
- ↑ 11.0 11.1 Deutscher D, Horn SD, Dickstein R, Hart DL, Smout RJ, Gutvirtz M, Ariel I. Associations between treatment processes, patient characteristics, and outcomes in outpatient physical therapy practice. Archives of physical medicine and rehabilitation. 2009 Aug 1;90(8):1349-63.
- ↑ Wang YC, Hart DL, Stratford PW, Mioduski JE. Clinical interpretation of a lower-extremity functional scale–derived computerized adaptive test. Physical therapy. 2009 Sep 1;89(9):957-68.
- ↑ 13.0 13.1 13.2 13.3 Renan-Ordine R, Alburquerque-SendÍn F, Rodrigues De Souza DP, Cleland JA, Fernández-De-Las-Penas C. Effectiveness of myofascial trigger point manual therapy combined with a self-stretching protocol for the management of plantar heel pain: a randomized controlled trial. Journal of Orthopaedic & Sports Physical Therapy. 2011 Feb;41(2):43-50.
- ↑ 14.0 14.1 14.2 14.3 Ajimsha MS, Chithra S, Thulasyammal RP. Effectiveness of myofascial release in the management of lateral epicondylitis in computer professionals. Archives of physical medicine and rehabilitation. 2012 Apr 1;93(4):604-9.
- ↑ Pollack Y, Shashua A, Kalichman L. Manual therapy for plantar heel pain. The Foot. 2018 Mar 1;34:11-6.