Moving and Handling
Original Editors - Samuel Winter
Top Contributors - Leana Louw, Samuel Winter and Lucinda hampton
Introduction[edit | edit source]
Moving and handling forms a key part of most occupations. It refer to moving and handling loads like objects or people.[1] This page will look into the ergonomics behind the safe moving and handling practices relating to physiotherapy.
See here Ergonomics
Handling principles[2][edit | edit source]
- Be prepared - know where the load is going, have the correct attitude, knowledge, skill and clothing
- Take note of floor surface and surroundings, as well as area moving to
- Test the weight that you know what to expect
- Use a firm grip
- Keep the weight close to your body ensuring the center of gravity is close to your base of support
- Pre-position your feet in the direction of movement
- Use a stable, broad base of support (bending your knees as a lower center of gravity is more stable)
- Maintain your lumbar lordosis to avoid excessive lumbar flexion) and activate your abdominal stabilizers (transverse abdominus)
- Bend your knees and lift the weight by extending your knees
- Avoid fast, uncontrolled movements, especially with turning
- Do not rotate your body during the movement, lift and rotate your feet - make sure your footware is appropriate
- Use your body weight and an appropriate lever where applicable
- If more than one person involved, clear instructions should be given - e.g. leader and follower
- Use mechanical aids for extra heavy objects
- ABC:
- Alignment (bend your knees, keep your pelvis neutral)
- Breathe (normal)
- Control (1/3)
Overview of Techniques[edit | edit source]
Preparation[3]
- Ensure clothing (including footwear) are appropriate
- Ensure all participants are aware of the task, including the order of specific task and end position of the patient
- Get the equipment ready and in order, with required accessories
- Prepare the environment, clear route and access ways are clear, move objects, and the destination is ready
- Prepare client, explain what will happen and what they are expected to do. Ensure clothes, including footwear, are appropriate, ensure they have any aids they need
- Choose a lead caregiver
- Count down "ready, steady, move" prior to the task
Communication between caregiver and patient[3]
- Talk through the steps prior
- Ask if OK as being moved
- Ask how they felt after the transfer
Moving and handling[edit | edit source]
Work stations[edit | edit source]
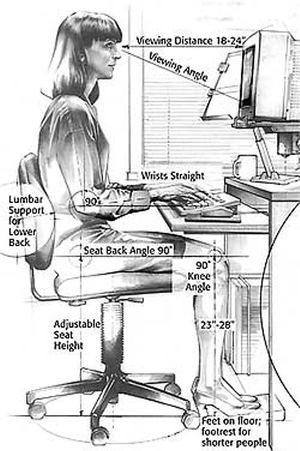
Workstation adjustment is a very important aspect to aim to prevent repetitive strain injuries for desk workers by improving posture. The following principles need to be taken into account:[4]
- Keep your head in a balanced position with chin tucked
- Computer screen:
- Positioned to be able to look down at a 15 degree angle
- Screen and work surface should be glare and reflection free
- Tiltable screen
- Height adjustable swivel stand screen
- Keyboard should be detached and flat
- Thin based desk with maximum thigh space
- Feet should be flat on ground or footrest available for positioning
- Shoulders relaxed
- Forearms horisontal
- Keep wrists in balanced position
- Chair:
- Adequate lower back support at belt level
- Ideally height and angle adjustable backrest
- Adjustable height (e.g. gas lift)
- 5 star stable base (wheels)
- No obstructions to leg movement
- Adequate illumination, ideally from the side
Mobilisation[edit | edit source]
Sitting[5][edit | edit source]
Preparation[edit | edit source]
- Check a patients weight-bearing status with colleagues, medical notes, the client and family if needed
- Consider hoisting if non-weight bearing, never put weight through a patients non-weight bearing leg
- Make sure the patient knows what to expect during the transfer
Supervising sitting repositioning[edit | edit source]
- Patient places feet flat of the floor and slightly under the chair
- Patient leans forwards so weight is over their knees
- Patient stands, moves as far back into the seat as possible OR pushes back on armrests and their feet to slide back into the seat
Assistance Sitting[edit | edit source]
- Ask client to feel for chair on back of legs, reach for armrests and slowly lower themselves
- Encourage client to bend at the hips
Standing[5][edit | edit source]
Supervising standing[edit | edit source]
- Patient places hands on armrests, feet flat of the floor and slightly under the chair
- Pt moves slightly closer to the edge of the seat
- Pt sits forwards, "nose over toes"
- If needed, the patient rocks backwards and forwards
- Patient leans forwards so weight is over their knees
- Carer counts down "ready, steady, stand". On stand, the patient pushes up into a standing position
Assistance Standing[edit | edit source]
- Caregiver adopts the lunge position, beside the patient
- Outside hand is flat on the front of patients shoulder, inside arm across lower back
- With weight starting on the back foot, carer rocks forward with the client
- Check clients arms are free and in front
Making use of a hoist
- Apply hoist sling
- Position hoist sling
- Position hoist
- Position sling bar and attach sling straps to hoist
- Instruct client to stand
- Reposition hoist
- Instruct client to sit
Bed Mobility[edit | edit source]
Rolling in bed[edit | edit source]
Supervised[5]
- Patient turns head in direction of roll
- Patient flexes knee further from the direction of roll
- Places arm across their chest in direction of roll
- Client rolls over, pushing with outside of foot and reaching across body
- Client completes roll
Assistance[5]
- Patient turns head in direction of roll
- Patient flexes knee further from the direction of roll
- Patient crosses arms against chest
- Therapist stands in direction of roll and places one hand on furthest shoulder, other on the furthest hip
- Client is rolled onto their side
Moving in bed[5][edit | edit source]
- Teach the patient to do a bridge to move up and down in the bed
- Patient to hold on to head of bed with arms and pull themselves up. This can be done in combination with a bridge, and works well in patients with an increased BMI, or that have specific lower limb weight bearing limitations/pain, preventing them to do an optimal bridge.
1 x assistance:
- Assist to lift pelvis
- Place patient in crook lying
- Put one around patient's shoulders and the other at the back of the scapula
- Assist with pulling upwards when the patient does a bridge
Sitting over the edge of a bed[edit | edit source]
Supervised[6]
- Patient turns to their side, facing the carer
- Patient places outside hand and inside elbow flat on the bed
- Client puts legs over the edge of the bed
- Uses hands and elbow to push up whilst lowering legs to floor
Slide sheets[edit | edit source]
Applying[5]
- Place slide sheets underneath a bed sheet
- Keep edges of slide sheet to edge of the bed
- Push slide sheet under the patient, pushing down on the mattress
- Roll patient to the side and pull through the slide sheets
Pushing client up the bed with slide sheets[5]
- Apply slide sheets
- Place extra pillow at head of the bed
- Enter a lung position
- Patient pushes up the bed with their feet, whilst carers slide up the bed
Removing slide sheets[5]
- Tuck in both sheets on one side
- In a lunge position, a therapist pulls out diagonally from the other side
- Place sheets neatly for next use
Lateral Transfers[edit | edit source]
Sitting to sitting[edit | edit source]
Supervision[5]
- Patient leans forward and slides to the front of the chair
- Client places leading foot in the direction they're going
- Patient reaches forwards to take the far arm of the chair
- The client pushes through their arms and legs
- Client transfers to the other chair
- Client lowers into chair
Therapist stays close by throughout
Assistance without an aid[5]
- Assisted sit to stand (as above)
- Patient instructed to walk or step to another chair
- Patient instructed to reach for the armrests
- Patient sits down
Transfer board and slide sheets[edit | edit source]
- Beds moved together
- Side sheets positioned on transfer board
- Assistance to roll onto the side away from the direction of transfer
- Transfer board placed underneath the patient
- Patient rolled back to neutral
- Patient slide to target bed
- Transfer board and slide sheets removed
Hoisting[edit | edit source]
Applying a sling in bed[5][edit | edit source]
Therapist one:
- folds the sling with labels and handles on the outside
- Position the sling from the base of the spine upwards
- Feed the upper strap under the client's neck
- Fold the upper shoulder loop into sling and roll the upper portion of the sling into the space behind the client's back
Therapist two:
- Locate the loop from under the patient's neck and pull towards you
Both therapists:
- Pull slings towards themselves, removing creases
- Complete the sling positioning, crossing leg loops between legs
Applying a sling to a client in a chair[5][edit | edit source]
- Ask the client to lean forward in the chair
- Place the sling behind the client
- Ensure the bottom of the sling reaches the base of the spine and that the sling is positioned correctly
- Put the leg straps under each leg one at a time
Hoisting from bed to chair[5][edit | edit source]
- Lower the sling bar above the client's chest
- Attach the sling to the bar,
- Slowly raise the patient off the mattress
- Move hoist so the client is over the chair
- Place a hand on the sling bar whilst lowering the patient
- Remove the sling from the bar and move the hoist away
- Remove sling
Resources[edit | edit source]
- Manual Handling Assessment Charts
- Risk Assessment Tool for Pushing and Pulling
- Manual handling at work: A brief guide
- Getting to grips with hoisting people == A brief guide ==
References[edit | edit source]
- ↑ Health and Safety Executive. Moving and handling in health and social care. Available from: https://www.hse.gov.uk/healthservices/moving-handling.htm (accessed 28/06/2020).
- ↑ Early Childhood Education Training and Resource Centre. Correct manual handling principles. Available from: http://www.ectarc.com.au/cybertots/toolbox12_11/shared/resources/html/res_correctmanhand.htm (accessed 26/06/2020).
- ↑ 3.0 3.1 Bridger R. Introduction to ergonomics. Crc Press; 2008.
- ↑ Ergonomics Health Association. How To Create The Ideal Ergonomic Workstation Setup In 2020. Available from: https://ergonomicshealth.com/ergonomic-workstation-setup/ (accessed 28/06/2020).
- ↑ 5.00 5.01 5.02 5.03 5.04 5.05 5.06 5.07 5.08 5.09 5.10 5.11 5.12 Turner A, Foster M, Johnson SE, editors. Occupational therapy and physical dysfunction: principles, skills and practice. Edinburgh: Churchill Livingstone; 2002.
- ↑ Pedretti LW, Early MB, editors. Occupational therapy: Practice skills for physical dysfunction. St. Louis, MO: Mosby; 2001 Feb.