Patellofemoral Instability
Original Editors - Assia Dad as part of the Vrije Universiteit Brussel's Evidence-based Practice project
Top Contributors - Claudia Karina, Julie Plas, Admin, Michelle Lee, Rachael Lowe, Assia Dad, Kim Jackson, 127.0.0.1, Kai A. Sigel, WikiSysop and Niels Cornand
Definition/Description[edit | edit source]
A frequent cause of knee pain and knee disability is patellofemoral instability. Patellofemoral instability can be defined in different ways. One way is when the patient has undergone a traumatic dislocation of the patella. It can also describe a sign on physical examination, signifying the ability of the patella to be translated out of the trochlear groove of the femur in a passive manner. Moreover, patellofemoral instability can be a symptom, when the patient gives a feeling that the knee “gives way’’. This feeling occurs when the patella slips out of the trochlear groove. The relationships between the symptoms, injuries and diseases of the patellofemoral joint are often confusing for the therapist.[[|]][1]
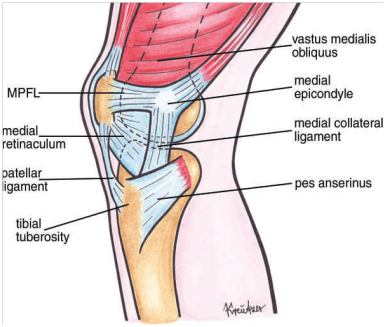
Figure1 Drawing of anatomic structures of the knee (medial view). Anatomic structures obscuring the MPFL have been left [2]
Clinically Relevant Anatomy[edit | edit source]
The patella is the largest sesamoid bone. It is located within the complex of the quadriceps and patellar tendon. Through its articulation with the femoral trochlea, the patellofemoral joint forms a highly complex unit with potential for joint instability. Patellofemoral joint stability is multifactorial and can be categorized into static and dynamic stabilizers. [3]
1) Static stabilizers:
- The medial side exists of three ligaments: The medial patellofemoral ligament (MPFL), the patellomeniscal ligament (MPML) and patellotibial ligament (MPTL): These are the primary ligamentous structures constraining lateral movement of the patella, the MPFL is the most important one. The MPFL is a continuation of the deep retinacular surface of the vastus medialis obliquus (VMO). It runs transversely between the proximal half of the medial border of the patella to the femur between the medial epicondyle and the adductor tubercle, forming the second layer between the superficial medial retinaculum and the capsule. [3]
- The anatomy of the lateral side is more complex:
- The vastus lateralis (anterior) and the superficial oblique retinaculum (further posteriorly) are part of the superficial.
- The deep layer mirrors the medial structures and consists of the lateral patellofermoral ligament (LPFL), the deep transverse retinaculum and the patellotibial ligament (LPTL).
- The LPTL attaches directly to the distal pole of the patella and sends fibers both into the lateral meniscus and into the underlying tibia. The LPFL is not attached directly to the femur, but indirectly via the proximal and distal attachments of the iliotibial band (ITB). Thus the tightness of the ITB (dynamic stabilizer) will influence the lateral stability force inferred by the lateral retinacular structures.
- The medial and lateral retinacular structure's' are most effective within the range of 20 ° flexion and full extension, during which the patellofemoral joint is most vulnerable due to the lack of resistance offered by other stabilizing structures.
- Trochlear geometry: The shape of the trochlea is concave. When the patella enters the trochlea, it allows for the inherent stability of the patellofemoral joint.
- Patellar geometry: The patella is convex and this congruity between the patella and the trochlea provides some constraint to the patellofemoral joint. When the knee begins to bend, the initial contact area is the distal and lateral patella facet. With further flexion, the contact area on the patella articular surface moves more proximally until in deep flexion where the medial facet has then made contact.
- Patellar height: the height of the patella also contributes to patellofemoral joint stability. Engagement of the patella depends entirely on patella height.
- Limb alignment: The angle between the pull of the quadriceps and the axis of the patella tendon (Q-angle) is very important. In males, the angle is 8 to 10° and in females, it is 15 ± 5°. [3]
2) Dynamic stabilizers:
- The quadriceps is a dynamic stabilizer of the patella. The patella is used as biomechanical lever, magnifying the force exerted by the quadriceps on knee extension.
- The patella also centralises the divergent forces of the quadriceps and transmits the tension around the femur to the patellar tendon.
Epidemiology /Etiology[edit | edit source]
There are two ways to develop patellofemoral instability by dislocation of the patella. It can develop after a traumatic dislocation of the kneecap in which the medial kneecap-stabilisers are stretched or ruptured, which eventually can result in recurrent dislocations of the patella. The other way is caused by anatomical anomaly of the knee joint.
Chronic instability of the patellofemoral joint and recurrent dislocation may lead to progressive cartilage damage and severe arthritis if not treated adequately
4.1 Patella dislocation after trauma
Acute traumatic patellar dislocation accounts for approximately 3% of all knee injuries. The leading mechanism of an acute dislocation of the patella is knee flexion with internal rotation on a planted foot with a valgus component. [2] This scenario accounts for 93% of all cases.[4] One of the common findings related to acute, primary, traumatic patellar dislocations is hemarthrosis of the knee, caused by rupture of the medial ligamentous stabilizers of the patella. This causes bleeding into joint spaces resulting in swelling and the formation of bruises around the kneecap. Knee joint effusion is also a typical finding after patellar dislocation. This can cause severe pain and it may limit the clinical examination.
Traumatic kneecap dislocation is typically the result of a sports injury and about 2/3 of the cases occur in young, active patients under the age of 20.[4] In case of traumatic dislocation conservative management may be preferred although nearly half of all patients with a first-time dislocation will suffer additional dislocations.[2] Subjects may even develop patellar instability, (aspecific) pain, patellofemoral arthritis or even chronic patellofemoral instability, depending on the presence and severity of the anatomic damage.[5]
4.2 Patella dislocation with a specific functional or anatomical cause
Dislocations without an acute knee hemarthrosis, which are mainly recurrent dislocations, may be associated to anomalies of the patellofemoral joint. These anomalies include trochlear dysplasia, patella alta, and lateralization of the tibial tuberosity (= excessive lateral distance between the tibial tubercle and the trochlear groove). These are the primary causes of dislocations with an anatomical cause.
Important secondary factors contributing to patellofemoral instability are femorotibial malrotation, genu recurvatum (hyperextended knee), and ligamentous laxity caused by Ehlers-Danlos syndrome, and Marfan syndrome.[2]
Characteristics/Clinical Presentation[edit | edit source]
5.1 Symptoms
Patients experience anterior knee pain and episodes of mechanical instability. [3] The pain can be aggravated by activities such as up and down the stairs, sports such as running, hopping and jumping, and changing direction. Upon functional assessment the patient may struggle with control of the patella, resulting in the patella being pull from midline, therefore to assess this you need to observe what is happening to the patella during static and dynamic movements such as squatting / lunging.
5.2 Risk factors
Patellofemoral instability is an instability of the patella, which can dislocate. This is very painful. It can be caused by a punch onto the patella, but more likely it is caused by a deviating shape of the joint. Some examples of these two causes:
• Insufficient deep articular surface (trochlea dysplasia) [6]
• Insufficient distance between tibial tuberosity and the trochlear quarry [6]
• Insufficiency of the MPFL [6]
• Patella alta (engagement into the trochlea does not occur in the early phase of knee flexion, thus potentiating instability at the patellofemoral joint) [3] [6]
• Knee valgus: an increased Q-angle can affect the patella tracking. [3]
• Inadequate VMO [3]
• A lesion of the medial retinaculum [7]
Differential Diagnosis[edit | edit source]
- Patellar dislocation may take place as a direct traumatic event (acute dislocation of the patella) in a patient with normal patellar alignment. It can also occur in a patient with pre-existing malalignment, especially if there is significant baseline subluxation.
- patellar subluxation: When the patella is transiently or permanently medial or lateral to its normal tracking course, then the patella may articulate abnormally.
Subluxation or lateral translation will involve transient lateral movement of the patella. In general, it is early in knee flexion such that the patient will experience a feeling of pain or instability. This form of patellar subluxation is rather a recurrent dislocation of the patella. It is essential to distinguish between this form of abnormal patellar alignment and tilt.
Types of subluxations:
• Minor Recurrent Subluxation
• Major Recurrent Subluxation
• Permanent Lateral Subluxation
Diagnostic Procedures[edit | edit source]
Patellar instability is normally diagnosed through a comprehensive history of the patient's symptoms and functional objective assessment of the knee. Further scans such as MRI's and Ultrasound imaging can be performed to rule out any structural deficits. Patellofemoral instability can also be examined through a lateral radiography or CT scan. In case of trochlea dysplasia, medical images show different flexion angles and varus movements are limited in the knee. CT scans provide better images than MRI scans. A lateral radiography can provide information about the height of the patella and whether there is trochlea dysplasia. [6]
Outcome Measures[edit | edit source]
There are many outcome measures that can be used with this condition, currently there are no specific reccomendations from COMET therefore it is up to the clinician to clinically reason which outcome measue would be most approprite for their paient. Here are a few:
- Anterior Knee Pain Scale
- Lower Extremity Functional Scale
- Pain Assessment Scales
- Numeric Pain Rating Scale
Examination[edit | edit source]
The first diagnostic step is a detailed history. It is the most important clue for a correct diagnosis.
The second diagnostic step is a careful, complete and essential physical examination. The purpose of this examination is to reproduce the symptoms (pain/instability) and to locate the painful zone. The location can indicate which structure is injured, it is truly helpful to compose the diagnosis and to plan the treatment.
The following tests can be used for physical examination:
• Assessment of acute dislocation (deformity and swelling that may mask a persistent lateral subluxation of the patella) [3]
• Lower limb alignment in coronal, sagittal and axial planes. [3]
• Evidence of joint hyper laxity: measured by the Beighton hypermobility score. [3]
• Measurement of the Q-angle: an increase in Q-angle results in an increased valgus vector. This is associated with an increased risk of instability, due to more laterally orientated forces. [3]
• Palpation of the patella: may reveal a palpable defect at the medial patellar margin and tenderness along the course or at the insertion of the MPFL. [3]
• Patellar-glide test: This test is used to evaluate the instability. A medial/lateral displacement of the patella greater than or equal to 3 quadrants, with this test, is consistent with incompetent lateral/medial restraints. Lateral patellar instability is more frequent than medial instability.
• Fairbanks patellar apprehension test: the test is positive, when there is pain and muscle defensive contraction of lateral patellar dislocation with 20°–30° of knee flexion. The positive test indicates that lateral patellar instability is an important part of the patient’s problem. This may be so positive that the patient pulls the leg back when the therapist approaches the knee with his hand, preventing so any contact, or the patient grabs the therapist’s arm. [8] → 100% sensitivity, 88.4% specificity, and overall accuracy of 94.1%
• Patellar-gravel test and J-sign test: these tests will test dynamic patellar tracking, but they are non-specific and have been noted to be absent in most cases of instability. [3]
Physical Therapy Management
[edit | edit source]
Patellofemoral Instability: acute dislocation of the patella[edit | edit source]
Nonoperative treatment:
It is a treatment that consists of immobilization followed by a period of structured rehabilitation. Immobilization is granted for healing of the soft tissues, especially the supporting structures on the medial side of the knee. Today brace treatment with early mobilization has become the norm, instead of the traditional immobilization of 3 to 6 weeks in a cylinder cast.
Most of the time these therapies start with the initial straight-leg raises: Quadriceps setting exercises and three sets of 15 to 20 straight leg raises are done four or five times a day during the acute period. Ice is applied for 20 minutes every 2 to 3 hours to reduce swelling.[3]
It is followed by stationary bicycle for passive and active motion, isotonic and isometric quadriceps strengthening. Between 3 and 8 weeks, the return to full activities was allowed when tenderness weakened and isotonic quadriceps strength was bilateral.
In up to two-third of the knees the results were good to excellent, these results consist of a first-time acute dislocation, compared with only 50% of those with a recurrent dislocation. In general, 73% were satisfied with their knees, but 16% were not and eventually decided to have surgical stabilization.
Those with acute patellar dislocation can expect an extended rehabilitation period before returning to sport, whether immobilized or not.
Patellofemoral Instability: Recurrent Dislocation of the Patella[edit | edit source]
Nonoperative treatment
Surgery is not necessarily needed for patients with patellofemoral malalignment or relaxation of the patella. Adequate results can be achieved with a conservative exercise treatment program. It is very important in the rehabilitation program to strengthen the quadriceps muscle and vastus medialis obliquus (VMO). It’s advised to follow the program which is similar to that followed after acute dislocation, but with more resistive exercises. This program can also be started early. In addition, a stabilization brace of the patella may help to prevent chronic recurrent subluxation.[4]
Key Research[edit | edit source]
Recent Related Research (from Pubmed)
[edit | edit source]
Failed to load RSS feed from http://www.ncbi.nlm.nih.gov/entrez/eutils/erss.cgi?rss_guid=1twh4oYFmCRoDmHROTQ3251NjD_yVyT1VCWLzSZT2ngN8DkQnw|charset=UTF-8|short|max=10: Error parsing XML for RSS
References
[edit | edit source]
- ↑ Fulkerson, J.P. et al., Disorders of the patellofemoral joint, USA, Williams & Wilkins, 1997, p.175-187, 199-216, 275-297
- ↑ G. Diederichs et al., 2010, MR Imaging of patellar instability: Injury Patterns and Assessment of Risk Factors, Radiographics
- ↑ Reuven Minkowitz, M.D., Chris Inzerillo, M.D., and Orrin H.Sherman,M.D., Patella Instability, Bulletin of the NYU Hospital for Joint Diseases 2007
- ↑ Barry P. Boden et al., Patellofemoral instability: evaluation and management, Journal of the American Academy of Orthopaedic Surgeons