Hyperkalemia: Difference between revisions
No edit summary |
No edit summary |
||
| Line 81: | Line 81: | ||
add text here | add text here | ||
== Medical Management (current best evidence) == | == Medical Management (current best evidence) == | ||
[[Image:Afp20060115p283-f2.gif]] | |||
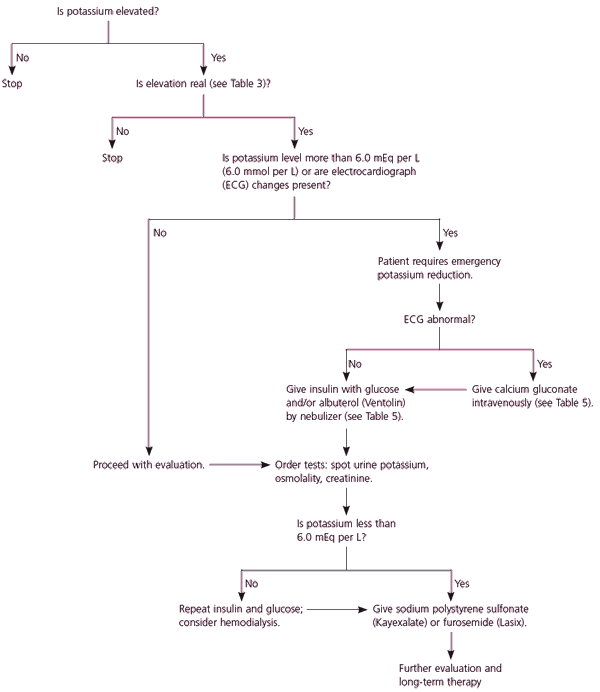
Figure 2: Algorithm for the management of hyperkalemia.<ref name="Hollander-Rodriguez and Calvert" /> | |||
{| style="width: 764px; height: 290px" border="1" cellspacing="1" cellpadding="1" width="764" | {| style="width: 764px; height: 290px" border="1" cellspacing="1" cellpadding="1" width="764" | ||
| Line 87: | Line 95: | ||
| colspan="6" | '''TABLE 5<br>Medications Used in Acute Treatment of Hyperkalemia''' | | colspan="6" | '''TABLE 5<br>Medications Used in Acute Treatment of Hyperkalemia''' | ||
|- | |- | ||
| '''Medication''' | | '''Medication''' | ||
| '''Dosage''' | | '''Dosage''' | ||
| '''Onset''' | | '''Onset''' | ||
| '''Length of Effect''' | | '''Length of Effect''' | ||
| '''Mechanism of Action''' | | '''Mechanism of Action''' | ||
| '''Cautions''' | | '''Cautions''' | ||
|- | |- | ||
| Calcium gluconate | | Calcium gluconate | ||
| 10 to 20 mL of 10 percent solution IV over two to three minutes | | 10 to 20 mL of 10 percent solution IV over two to three minutes | ||
| immediate | | immediate | ||
| 30 minutes | | 30 minutes | ||
| Protects myocardium from toxic effects of calcium; no effect on serum potassium level | | Protects myocardium from toxic effects of calcium; no effect on serum potassium level | ||
| Can worsen digoxin toxicity | | Can worsen digoxin toxicity | ||
|- | |- | ||
| insulin | | insulin | ||
| Regular insulin 10 units IV with 50 mL of 50 percent glucose | | Regular insulin 10 units IV with 50 mL of 50 percent glucose | ||
| 15 to 30 minutes | | 15 to 30 minutes | ||
| two to six hours | | two to six hours | ||
| Shifts potassium out of the vascular space and into the cells; no effect on total body potassium | | Shifts potassium out of the vascular space and into the cells; no effect on total body potassium | ||
| Consider 5 percent dextrose solution infusion at 100 mL per hour to prevent hypoglycemia with repeated doses. Glucose unnecessary if blood sugar elevated above 250 mg per dL (13.9 mmol per L) | | Consider 5 percent dextrose solution infusion at 100 mL per hour to prevent hypoglycemia with repeated doses. Glucose unnecessary if blood sugar elevated above 250 mg per dL (13.9 mmol per L) | ||
|- | |- | ||
| Albuterol (Ventolin) | | Albuterol (Ventolin) | ||
| 10 to 20 mg by nebulizer over 10 minutes (use concentrated form, 5 mg per mL) | | 10 to 20 mg by nebulizer over 10 minutes (use concentrated form, 5 mg per mL) | ||
| 15 to 30 minutes | | 15 to 30 minutes | ||
| two to three hours | | two to three hours | ||
| Shifts potassium into the cells, additive to the effect of insulin; no effect on total body potassium | | Shifts potassium into the cells, additive to the effect of insulin; no effect on total body potassium | ||
| May cause a brief initial rise in serum potassium | | May cause a brief initial rise in serum potassium | ||
|- | |- | ||
| Furosemide (Lasix) | | Furosemide (Lasix) | ||
| 20 to 40 mg IV, give with saline if volume depletion is a concern | | 20 to 40 mg IV, give with saline if volume depletion is a concern | ||
| 15 minutes to one hour | | 15 minutes to one hour | ||
| four hours | | four hours | ||
| Increases renal excretion of potassium | | Increases renal excretion of potassium | ||
| Only effective if adequate renal response to loop diuretic | | Only effective if adequate renal response to loop diuretic | ||
|- | |- | ||
| Sodium polystyrene sulfonate (Kayexalate) | | Sodium polystyrene sulfonate (Kayexalate) | ||
| Oral: 50 g in 30 mL of sorbitol solution Rectal: 50 g in a retention enema | | Oral: 50 g in 30 mL of sorbitol solution Rectal: 50 g in a retention enema | ||
| One to two hours (rectal route is faster) | | One to two hours (rectal route is faster) | ||
| four to six hours | | four to six hours | ||
| Removes potassium from the gut in exchange for sodium | | Removes potassium from the gut in exchange for sodium | ||
| Sorbitol may be associated with bowel necrosis. May lead to sodium retention | | Sorbitol may be associated with bowel necrosis. May lead to sodium retention | ||
|} | |} | ||
IV = intravenously | IV = intravenously | ||
*--Medications listed from most to least urgent.<ref name="Hollander-Rodriguez and Calvert" /><br><br><br><br><br><br><br> | *--Medications listed from most to least urgent.<ref name="Hollander-Rodriguez and Calvert" /><br><br><br><br><br><br><br> | ||
Revision as of 22:52, 26 March 2013
Original Editors -Courtney Ahlers & Jessica Ketterer from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Lead Editors - Your name will be added here if you are a lead editor on this page. Read more.
Definition/Description[edit | edit source]
Hyperkalemia is characterized by an elevated serum potassium level greater than 5.5 mmol/L and is classified as an electrolyte abnormality. [1] Acute hyperkalemia is often preceded by issues such as illness, dehydration, or introduction of medications that affect potassium levels. [2]
Prevalence[edit | edit source]
Approximately 1 to 10 percepnt of hospital patients are affected by hyperkalemia. [2]
The mortality rate for patients with hyperkalemia is approximately 1 in 1000. [1]
Characteristics/Clinical Presentation[edit | edit source]
Hyperkalemia most commonly occurs in patients with chronic renal failure. [2]
Associated Co-morbidities[edit | edit source]
| Table 1
Disorders Causing Hyperkalemia | |
| Disorders leading to hyperkalemia caused by impaired renal excretion of potassium | Disorders leading to hyperkalemia caused by shift of potassium into the extracellular space |
| acquired hyporeninemic hypoaldosteronism | acidosis |
| Addison's disease | damage to tissue from rhabdomyolysis, burns, or trauma |
| congenital adrenal hyperplasia (recessive or autosomal dominant) | familial hyperkalemic periodic paralysis |
| mineralocorticoid deficiency | hyperosmolar states (uncontrolled diabetes, glucose infusions) |
| primary hypoaldosteronism or hyporeninemia | tumor lysis syndrome |
| pseudohypoaldosteronism | insulin deficiency or resistance |
| renal insufficiency or failure | |
| systemic lupus erythematosus | |
| type IV renal tubular acidosis | |
Medications[edit | edit source]
add text here
Diagnostic Tests/Lab Tests/Lab Values[edit | edit source]
add text here
Etiology/Causes[edit | edit source]
Hyperkalemia is typically caused when the kidneys can no longer excrete potassium, when the body is unable to effectively move potassium fro the extracellular space to within the cell, or a combination of the two. [2]
Systemic Involvement[edit | edit source]
add text here
Medical Management (current best evidence)[edit | edit source]
Figure 2: Algorithm for the management of hyperkalemia.[2]
| TABLE 5 Medications Used in Acute Treatment of Hyperkalemia | |||||
| Medication | Dosage | Onset | Length of Effect | Mechanism of Action | Cautions |
| Calcium gluconate | 10 to 20 mL of 10 percent solution IV over two to three minutes | immediate | 30 minutes | Protects myocardium from toxic effects of calcium; no effect on serum potassium level | Can worsen digoxin toxicity |
| insulin | Regular insulin 10 units IV with 50 mL of 50 percent glucose | 15 to 30 minutes | two to six hours | Shifts potassium out of the vascular space and into the cells; no effect on total body potassium | Consider 5 percent dextrose solution infusion at 100 mL per hour to prevent hypoglycemia with repeated doses. Glucose unnecessary if blood sugar elevated above 250 mg per dL (13.9 mmol per L) |
| Albuterol (Ventolin) | 10 to 20 mg by nebulizer over 10 minutes (use concentrated form, 5 mg per mL) | 15 to 30 minutes | two to three hours | Shifts potassium into the cells, additive to the effect of insulin; no effect on total body potassium | May cause a brief initial rise in serum potassium |
| Furosemide (Lasix) | 20 to 40 mg IV, give with saline if volume depletion is a concern | 15 minutes to one hour | four hours | Increases renal excretion of potassium | Only effective if adequate renal response to loop diuretic |
| Sodium polystyrene sulfonate (Kayexalate) | Oral: 50 g in 30 mL of sorbitol solution Rectal: 50 g in a retention enema | One to two hours (rectal route is faster) | four to six hours | Removes potassium from the gut in exchange for sodium | Sorbitol may be associated with bowel necrosis. May lead to sodium retention |
IV = intravenously
- --Medications listed from most to least urgent.[2]
Physical Therapy Management (current best evidence)[edit | edit source]
Potassium levels < 3.2 mEq/L or > 5.1 mEq/L contraindicated for physical therapy intervention due to the potential for arrhythmia and tetany.[3]
Alternative/Holistic Management (current best evidence)[edit | edit source]
add text here
Differential Diagnosis[edit | edit source]
Pseudohyperkalemia occurs when lab reports indicate elevated serum potassium levels but the patient does not actually have elevated serum potassium. This phenomenon occurs most commonly with destruction of red blood cells with collection of blood specimen.[2]
Case Reports/ Case Studies[edit | edit source]
add links to case studies here (case studies should be added on new pages using the case study template)
Resources
[edit | edit source]
add appropriate resources here
Recent Related Research (from Pubmed)[edit | edit source]
see tutorial on Adding PubMed Feed
Failed to load RSS feed from http://eutils.ncbi.nlm.nih.gov/entrez/eutils/erss.cgi?rss_guid=1NGmwZeh8JwVIzrKgHG1LrDm0izTr7ViJiDkSYAY2BW5hiXsx0|charset=UTF-8|short|max=10: Error parsing XML for RSS
References[edit | edit source]
see adding references tutorial.
- ↑ 1.0 1.1 Raymond C, Sood A, Wazny L. Treatment of hyperkalemia in patients with chronic kidney disease--a focus on medications. CANNT Journal [serial on the Internet]. (2010, July), [cited March 22, 2013]; 20(3): 49-54. Available from: CINAHL with Full Text. http://search.ebscohost.com/login.aspx?direct=true&amp;amp;amp;amp;amp;db=c8h&amp;amp;amp;amp;amp;AN=2010782358&amp;amp;amp;amp;amp;site=ehost-live (accessed 22 Mar 2013)
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Hollander-Rodriguez JC, Calvert, Jr. JF. Hyperkalemia. American Family Physician 2006; 73(2):283-290. Available from: PubMed. http://www.ncbi.nlm.nih.gov/pubmed/16445274 )22 March 2013)
- ↑ Goodman CC & Fuller KS. In K Falk editor. Pathology: Implications for the Physical Therapist. St. Louis: Saunders Elsevier; 2009. pp.150, 157, 187-189, 480, 558, 927, 1243, 1640-1641