Morel-Lavallée lesion: Difference between revisions
(Defintion, epidemiology/aetiology, pathophysiology added) |
(clinical presentation, complications and classification added) |
||
| Line 5: | Line 5: | ||
A Morel-Lavallée lesion (MLL) was first described in 1853<ref name=":0">Diviti S, Gupta N, Hooda K, Sharma K, Lo L. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5449878/pdf/jcdr-11-TE01.pdf Morel-Lavallee lesions-review of pathophysiology, clinical findings, imaging findings and management]. Journal of clinical and diagnostic research: JCDR. 2017 Apr;11(4):TE01.</ref> <ref name=":1">Singh R, Rymer B, Youssef B, Lim J. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6126206/pdf/main.pdf The Morel-Lavallée lesion and its management: a review of the literature]. Journal of orthopaedics. 2018 Dec 1;15(4):917-21.</ref>. It is a closed soft-tissue degloving injury<ref name=":0" /><ref name=":2">Zairi F, Wang Z, Shedid D, Boubez G, Sunna T. [https://reader.elsevier.com/reader/sd/pii/S1877056816000335?token=193AFCCCD9D35EF9227D6E4A8B2D40CD82BE93612C9E4AE3D66FCFDFAE18AF664140FDCB451AEEEC9F156AAC2CD3531C&originRegion=eu-west-1&originCreation=20221125075833 Lumbar Morel-Lavallée lesion: case report and review of the literature]. Orthopaedics & Traumatology: Surgery & Research. 2016 Jun 1;102(4):525-7.</ref><ref name=":3">LaTulip S, Rao RR, Sielaff A, Theyyunni N, Burkhardt J. [https://downloads.hindawi.com/journals/criem/2017/3967587.pdf Ultrasound utility in the diagnosis of a Morel-Lavallée lesion]. Case Reports in Emergency Medicine. 2017 Feb 1;2017.</ref><ref name=":4">Depaoli R, Canepari E, Bortolotto C, Ferrozzi G. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4353822/pdf/40477_2015_Article_157.pdf Morel-Lavallée lesion of the knee in a soccer player]. Journal of ultrasound. 2015 Mar;18(1):87-9.</ref><ref name=":5">Mettu R, Surath HV, Chayam HR, Surath A. [https://www.researchgate.net/publication/320866983_Chronic_Morel-Lavallee_Lesion_A_Novel_Minimally_Invasive_Method_of_Treatment Chronic Morel-Lavallée lesion: a novel minimally invasive method of treatment]. Wounds. 2016 Nov 1;28(11):404-7.</ref> that usually occurs after blunt trauma<ref name=":0" /><ref name=":1" /><ref name=":2" /><ref name=":4" />. In recent literature, it can also be referred to as Morel-Lavallée seroma or effusion, post-traumatic soft tissue cysts or post-traumatic extravasations<ref name=":1" />. | A Morel-Lavallée lesion (MLL) was first described in 1853<ref name=":0">Diviti S, Gupta N, Hooda K, Sharma K, Lo L. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5449878/pdf/jcdr-11-TE01.pdf Morel-Lavallee lesions-review of pathophysiology, clinical findings, imaging findings and management]. Journal of clinical and diagnostic research: JCDR. 2017 Apr;11(4):TE01.</ref> <ref name=":1">Singh R, Rymer B, Youssef B, Lim J. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6126206/pdf/main.pdf The Morel-Lavallée lesion and its management: a review of the literature]. Journal of orthopaedics. 2018 Dec 1;15(4):917-21.</ref>. It is a closed soft-tissue degloving injury<ref name=":0" /><ref name=":2">Zairi F, Wang Z, Shedid D, Boubez G, Sunna T. [https://reader.elsevier.com/reader/sd/pii/S1877056816000335?token=193AFCCCD9D35EF9227D6E4A8B2D40CD82BE93612C9E4AE3D66FCFDFAE18AF664140FDCB451AEEEC9F156AAC2CD3531C&originRegion=eu-west-1&originCreation=20221125075833 Lumbar Morel-Lavallée lesion: case report and review of the literature]. Orthopaedics & Traumatology: Surgery & Research. 2016 Jun 1;102(4):525-7.</ref><ref name=":3">LaTulip S, Rao RR, Sielaff A, Theyyunni N, Burkhardt J. [https://downloads.hindawi.com/journals/criem/2017/3967587.pdf Ultrasound utility in the diagnosis of a Morel-Lavallée lesion]. Case Reports in Emergency Medicine. 2017 Feb 1;2017.</ref><ref name=":4">Depaoli R, Canepari E, Bortolotto C, Ferrozzi G. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4353822/pdf/40477_2015_Article_157.pdf Morel-Lavallée lesion of the knee in a soccer player]. Journal of ultrasound. 2015 Mar;18(1):87-9.</ref><ref name=":5">Mettu R, Surath HV, Chayam HR, Surath A. [https://www.researchgate.net/publication/320866983_Chronic_Morel-Lavallee_Lesion_A_Novel_Minimally_Invasive_Method_of_Treatment Chronic Morel-Lavallée lesion: a novel minimally invasive method of treatment]. Wounds. 2016 Nov 1;28(11):404-7.</ref> that usually occurs after blunt trauma<ref name=":0" /><ref name=":1" /><ref name=":2" /><ref name=":4" />. In recent literature, it can also be referred to as Morel-Lavallée seroma or effusion, post-traumatic soft tissue cysts or post-traumatic extravasations<ref name=":1" />. | ||
== Epidemiology and aetiology == | == Epidemiology and aetiology == | ||
These injuries are uncommon<ref name=":1" /> and there is no consensus on the ratio of men to women. One source reported a 2:1 ratio<ref name=":1" /> while another reported a 1:1 ratio<ref>Christian D, Leland HA, Osias W, Eberlin S, Howell L. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5065277/pdf/jrcr-10-7-30.pdf Delayed presentation of a chronic Morel-Lavallee lesion]. Journal of Radiology Case Reports. 2016 Jul;10(7):30.</ref>. | These injuries are uncommon<ref name=":1" /> and there is no consensus on the ratio of men to women. One source reported a 2:1 ratio<ref name=":1" /> while another reported a 1:1 ratio<ref name=":10">Christian D, Leland HA, Osias W, Eberlin S, Howell L. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5065277/pdf/jrcr-10-7-30.pdf Delayed presentation of a chronic Morel-Lavallee lesion]. Journal of Radiology Case Reports. 2016 Jul;10(7):30.</ref>. | ||
These injuries occur due to blunt trauma after: | These injuries occur due to blunt trauma after: | ||
| Line 22: | Line 22: | ||
Secondary risk factors for an MLL include female gender and BMI of over 25<ref name=":0" />. | Secondary risk factors for an MLL include female gender and BMI of over 25<ref name=":0" />. | ||
== Clinical Presentation == | == Clinical Presentation == | ||
MLL occurs most commonly over the greater trochanter (>60% of cases) | [[File:Morel-lavallee sites.jpg|thumb|400x400px|Case courtesy of Dr Matt Skalski, <a href="https://radiopaedia.org/?lang=us">Radiopaedia.org</a>. From the case <a href="https://radiopaedia.org/cases/22762?lang=us">rID: 22762</a>]] | ||
MLL occurs most commonly over the greater trochanter (>60% of cases)<ref name=":0" /><ref name=":2" /> <ref name=":4" /><ref name=":5" /><ref name=":6" /><ref name=":9" />, proximal femur<ref name=":0" /><ref name=":1" /><ref name=":4" />, buttock<ref name=":1" /><ref name=":2" /><ref name=":4" />, knee<ref name=":2" /><ref name=":4" /><ref name=":5" /><ref name=":9" /> and in rare cases, the lumbar region<ref name=":1" /><ref name=":2" /><ref name=":5" /><ref name=":9" />. It can also occur at the scapula<ref name=":1" /><ref name=":5" />. Delayed presentation (months or years) can occur in up to ⅓ of patients<ref name=":0" /><ref name=":6" />. The most common signs and symptoms include: | |||
* Compressible, fluctuant swollen area<ref name=":0" /><ref name=":1" /><ref name=":4" /><ref name=":6" /><ref name=":7" />. The fluctuant swelling is an essential clinical characteristic<ref name=":7" />. | |||
* Pain<ref name=":0" /><ref name=":1" /><ref name=":3" /><ref name=":6" /> | |||
* Stiffness<ref name=":4" /><ref name=":7" /> | |||
* Cutaneous anaesthesia or hypothesia may be present<ref name=":0" /><ref name=":1" /><ref name=":3" /><ref name=":6" /> | |||
* Ecchymosis may be present<ref name=":7" /> | |||
* Abrasions may be present<ref name=":7" /> | |||
* Secondary dermal changes e.g. discolouration, frank necrosis, drying/cracking<ref name=":0" /><ref name=":7" /> | |||
== Complications == | |||
The necrotic tissue associated with the MLL is particularly susceptible to infection<ref name=":2" /> and if infection occurs, it can lead to | |||
* | * Cellulitis<ref name=":2" /> | ||
* | * Abscess<ref name=":2" /> | ||
* | * Osteomyelitis<ref name=":2" /> | ||
* Necrosis of underlying tissues due to pressure<ref name=":7" /> | |||
* | |||
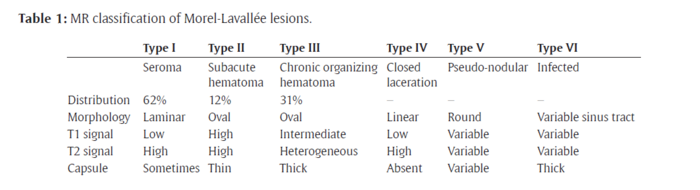
== Classification == | |||
== | Mellado and Bencardino proposed a MRI classification and identified 6 types of MLL based on the lesion chronicity, appearance on MRI and tissue composition <ref name=":1" /><ref name=":10" /><ref name=":6" /><ref name=":7" />. The 6 types include the following: | ||
[[File:MRI classification morel lavallee.png|center|thumb|700x700px|De Coninck, T, Vanhoenacker, F and Verstraete, K. Imaging Features of Morel-Lavallée Lesions. Journal of the Belgian Society of Radiology. 2017; 101(S2): 15, pp. 1–8. DOI: <nowiki>https://doi.org/10.5334/jbr-btr.1401</nowiki>]] | |||
Type I to III are the most common types with Type I being acute, type II, sub-acute and III, chronic<ref name=":6" />. | |||
A more basic acute vs chronic classification was proposed by Shen et al (2013)<ref name=":1" />. The lesion is considered chronic once a capsule is present<ref name=":1" />. | |||
== Diagnostic Procedures | == Diagnostic Procedures == | ||
add text here relating to diagnostic tests for the condition<br> | add text here relating to diagnostic tests for the condition<br> | ||
Revision as of 10:50, 25 November 2022
Definition[edit | edit source]
A Morel-Lavallée lesion (MLL) was first described in 1853[1] [2]. It is a closed soft-tissue degloving injury[1][3][4][5][6] that usually occurs after blunt trauma[1][2][3][5]. In recent literature, it can also be referred to as Morel-Lavallée seroma or effusion, post-traumatic soft tissue cysts or post-traumatic extravasations[2].
Epidemiology and aetiology[edit | edit source]
These injuries are uncommon[2] and there is no consensus on the ratio of men to women. One source reported a 2:1 ratio[2] while another reported a 1:1 ratio[7].
These injuries occur due to blunt trauma after:
MLL can also be iatrogenic e.g. after abdominal liposuction or mammoplasty[1][2][6]
Pathophysiology[edit | edit source]
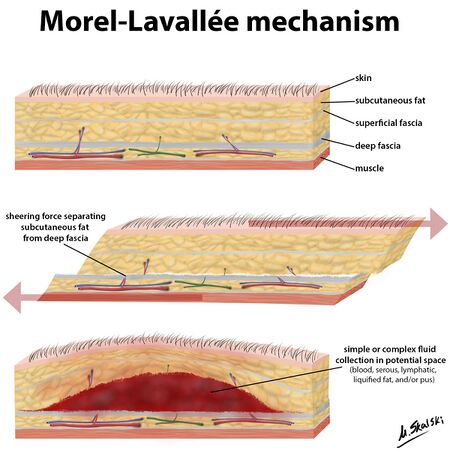
MLL occurs due to shearing forces which separate the skin and subcutaneous tissue from the deep fascia, causing a potential space[1][2][4][5][8][10][11]. Damage to the lymphatic and blood vessels leads to an accumulation of blood and lymph[1][3][4][8][10] and necrotic fat[1][3][8][12] in the potential space, causing a haematoma or seroma[10]. Blood will start to be reabsorbed over time leaving a serosanguinous fluid surrounded by a haemosiderin layer[2]. Inflammation is then induced by the haemosiderin layer leading to a fibrous capsule[2][11]. This fibrous capsule prevents more fluid reabsorption, initiating a chronic MLL[3].
MLL are often associated with pelvic or acetabular fractures but can also occur without a fracture[9].
Secondary risk factors for an MLL include female gender and BMI of over 25[1].
Clinical Presentation[edit | edit source]
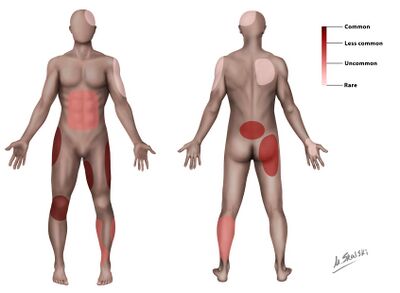
MLL occurs most commonly over the greater trochanter (>60% of cases)[1][3] [5][6][8][11], proximal femur[1][2][5], buttock[2][3][5], knee[3][5][6][11] and in rare cases, the lumbar region[2][3][6][11]. It can also occur at the scapula[2][6]. Delayed presentation (months or years) can occur in up to ⅓ of patients[1][8]. The most common signs and symptoms include:
- Compressible, fluctuant swollen area[1][2][5][8][9]. The fluctuant swelling is an essential clinical characteristic[9].
- Pain[1][2][4][8]
- Stiffness[5][9]
- Cutaneous anaesthesia or hypothesia may be present[1][2][4][8]
- Ecchymosis may be present[9]
- Abrasions may be present[9]
- Secondary dermal changes e.g. discolouration, frank necrosis, drying/cracking[1][9]
Complications[edit | edit source]
The necrotic tissue associated with the MLL is particularly susceptible to infection[3] and if infection occurs, it can lead to
Classification[edit | edit source]
Mellado and Bencardino proposed a MRI classification and identified 6 types of MLL based on the lesion chronicity, appearance on MRI and tissue composition [2][7][8][9]. The 6 types include the following:
Type I to III are the most common types with Type I being acute, type II, sub-acute and III, chronic[8].
A more basic acute vs chronic classification was proposed by Shen et al (2013)[2]. The lesion is considered chronic once a capsule is present[2].
Diagnostic Procedures[edit | edit source]
add text here relating to diagnostic tests for the condition
Management / Interventions
[edit | edit source]
add text here relating to management approaches to the condition
Differential Diagnosis
[edit | edit source]
add text here relating to the differential diagnosis of this condition
Resources
[edit | edit source]
add appropriate resources here
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 Diviti S, Gupta N, Hooda K, Sharma K, Lo L. Morel-Lavallee lesions-review of pathophysiology, clinical findings, imaging findings and management. Journal of clinical and diagnostic research: JCDR. 2017 Apr;11(4):TE01.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 2.18 2.19 2.20 Singh R, Rymer B, Youssef B, Lim J. The Morel-Lavallée lesion and its management: a review of the literature. Journal of orthopaedics. 2018 Dec 1;15(4):917-21.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 Zairi F, Wang Z, Shedid D, Boubez G, Sunna T. Lumbar Morel-Lavallée lesion: case report and review of the literature. Orthopaedics & Traumatology: Surgery & Research. 2016 Jun 1;102(4):525-7.
- ↑ 4.0 4.1 4.2 4.3 4.4 LaTulip S, Rao RR, Sielaff A, Theyyunni N, Burkhardt J. Ultrasound utility in the diagnosis of a Morel-Lavallée lesion. Case Reports in Emergency Medicine. 2017 Feb 1;2017.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 5.8 Depaoli R, Canepari E, Bortolotto C, Ferrozzi G. Morel-Lavallée lesion of the knee in a soccer player. Journal of ultrasound. 2015 Mar;18(1):87-9.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 6.7 6.8 Mettu R, Surath HV, Chayam HR, Surath A. Chronic Morel-Lavallée lesion: a novel minimally invasive method of treatment. Wounds. 2016 Nov 1;28(11):404-7.
- ↑ 7.0 7.1 Christian D, Leland HA, Osias W, Eberlin S, Howell L. Delayed presentation of a chronic Morel-Lavallee lesion. Journal of Radiology Case Reports. 2016 Jul;10(7):30.
- ↑ 8.00 8.01 8.02 8.03 8.04 8.05 8.06 8.07 8.08 8.09 8.10 De Coninck T, Vanhoenacker F, Verstraete K. Imaging features of Morel-Lavallée lesions. Journal of the Belgian Society of Radiology. 2017;101(Suppl 2).
- ↑ 9.00 9.01 9.02 9.03 9.04 9.05 9.06 9.07 9.08 9.09 9.10 9.11 Badjate DM, Jain D, Phansopkar P, Wadhokar OC. A Physical Therapy Rehabilitative Approach in Improving Activities of Daily Living in a Patient With Morel-Lavallée Syndrome: A Case Report. Cureus. 2022 Sep 24;14(9).
- ↑ 10.0 10.1 10.2 Weiss NA, Johnson JJ, Anderson SB. Morel-lavallee lesion initially diagnosed as quadriceps contusion: ultrasound, MRI, and importance of early intervention. Western Journal of Emergency Medicine. 2015 May;16(3):438.
- ↑ 11.0 11.1 11.2 11.3 11.4 Cruz N, Jiménez R. Morel-Lavallée lesion diagnosed 25 years after blunt trauma. International Journal of Surgery Case Reports. 2021 Apr 1;81:105733.
- ↑ Cochran GK, Hanna KH. Morel-Lavallee lesion in the upper extremity. Hand. 2017 Jan;12(1):NP10-3.