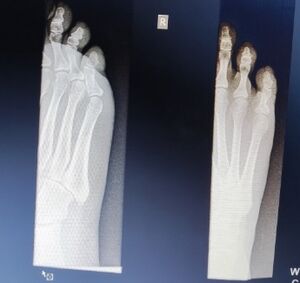
Toe Fractures
Original Editor - Angeliki Chorti
Top Contributors - Angeliki Chorti and Syeda Bushra Zehra Zaidi
Introduction[edit | edit source]
Toe fractures are one of the most commonly diagnosed lower extremity fractures seen by family physicians. They often result from a crushing injury or axial force, such as stubbing a toe. In some cases, joint hyperextension and stress fractures may also be responsible, with studies reporting 14 to 39.6 cases per 10,000 people presenting at emergency departments.[1] [2]Although toe fractures predominantly involve the first and fifth toe, fractures of the lesser digits are more common than those of the great toe.[3] The proximal phalanx is the most usual fracture site, because of its greater length compared with the rest of the toe bones. [4]
Mechanisms of injury[edit | edit source]
Toe fractures are usually the result of direct trauma such as crushing from striking objects, [3] [5] axial forces e.g. stubbing a toe, falls, and sports and recreational activity. A sudden abduction force applied to the digit against an object is the most common mechanism of injury. Stubbed toe can occur when flexion of the distal phalanx in conjunction with a proximal shearing force causes a fracture or subluxation.
Indirect trauma such as hyperflexion or hyperextension can also lead to avulsion fractures, but these types of injuries are less common. [5]
Types of Toe Fractures[edit | edit source]
Toe fractures can vary in type and severity depending on the location and extent of the injury. The common types of toe fractures include:
- Simple Fracture (Closed Fracture): This is the most common type of toe fracture, where the bone breaks without puncturing the skin. Simple fractures can be non-displaced or displaced. Non-displaced fractures occur when the ends of the fracture remain together, while displaced fractures involve partial or complete separation of the fractured bone(s). [4]
- Compound Fracture (Open Fracture): In a compound fracture, the broken bone pierces the skin, exposing it to the external environment. These fractures have a higher risk of infection due to the open wound. [1]
- Avulsion Fracture: An avulsion fracture occurs when a small piece of bone is pulled away from the main bone by a tendon or ligament. This type of fracture is more common in athletes or individuals involved in sports with sudden movements or excessive stretching.[6]
- Comminuted Fracture: In a comminuted fracture, the bone shatters into multiple fragments. This type of fracture can be more challenging to treat and may require surgical intervention.[7]
- Intra-articular Fracture: Intra-articular fractures involve the joint surface of the toe. These fractures can be more complex and may require specialised management to ensure proper joint function and minimize the risk of arthritis.[7]
- Dislocation Fracture: Dislocation fractures involve both a joint dislocation and a fracture of the involved bone. These injuries require immediate medical attention to address both the dislocation and the fractured bone.[8]
Clinical presentation[edit | edit source]
When a toe fracture occurs, it often presents with specific signs and symptoms that aids the diagnosis and assessment of the injury. The clinical presentation of toe fractures typically includes the following:
- Pain and Tenderness: The primary complaint of individuals with a toe fracture is localised pain and tenderness at the site of the injury. The affected toe may be sensitive to touch, and the pain intensity can vary depending on the severity of the fracture.
- Swelling and Bruising: Swelling (oedema) is a common accompanying feature of toe fractures. The injured toe may appear visibly swollen, and there could be bruising (ecchymosis) around the fracture site due to internal bleeding from damaged blood vessels.
- Difficulty Bearing Weight: Toe fractures can make it challenging to bear weight on the affected foot, especially during walking or standing. Individuals may attempt to avoid putting pressure on the injured toe, altering their gait pattern to minimise pain.
- Painful Ambulation: Walking or bearing weight on the injured toe can be painful. As a result, individuals may exhibit a limp or walk gingerly to reduce discomfort.
- Deformity: In some cases, particularly with displaced fractures, there may be visible deformity of the affected toe. The toe may appear misaligned, bent, or at an unusual angle compared to the adjacent toes.
- Limited Range of Motion: Toe fractures can lead to reduced flexibility and limited range of motion in the affected toe. Attempts to move the toe might exacerbate pain and discomfort.
- Nailbed Injuries and Subungual Hematomas: Associated injuries to the nailbed can occur in toe fractures. Subungual hematomas (blood collection under the nail) may also be observed, especially if the injury involves the toenail. [5] [9]
Diagnosis[edit | edit source]
Diagnosing toe fractures is a comprehensive process that combines clinical evaluation, medical history, and imaging studies. Prompt and accurate diagnosis is crucial to understand the type and severity of the fracture, guiding appropriate treatment and avoiding future complications. [4] Here are the usual steps involved in diagnosing toe fractures:
- Clinical Evaluation: A thorough physical examination of the injured toe is conducted to assess for tenderness, swelling, bruising, deformity, and limited range of motion. The patient's medical history is obtained, including information about the injury's mechanism.
- X-ray Imaging: X-rays are commonly used to diagnose toe fractures. Standard anteroposterior (AP) and oblique views provide visualisation of the bones and the presence of fractures. Displacement, if any, is also assessed to plan appropriate treatment.
- Ultrasonography: In certain cases, ultrasonography complements the diagnosis, especially when X-rays are inconclusive or when soft tissue involvement is suspected. It offers detailed images of ligaments and tendons and aids in evaluating joint stability.
- MRI or CT Scan (less common): For complex or severe cases, MRI or CT scans may be utilised to assess the extent of the injury, particularly if joint involvement or less visible fractures are suspected.
Differential Diagnosis[edit | edit source]
To rule out other potential causes of toe pain and swelling, a differential diagnosis is conducted, considering conditions like sprains, dislocations, or bone infections.
Specialist Consultation[edit | edit source]
In complex cases, consulting an orthopedic specialist or a podiatrist ensures specialised opinion and appropriate management. [5] [9]
Management[edit | edit source]
The management of toe fractures depends on various factors, including the type of fracture, the degree of displacement, and the overall health of the patient. The primary goals of treatment are to alleviate pain, promote healing, prevent complications, and restore normal foot function.
It must be noted here that the majority of toe fractures are non- or minimally displaced, making conservative treatment the typical approach.[1]
Here are the common approaches to managing toe fractures:
- Conservative Management:
- Buddy Taping: For stable, non-displaced fractures, adjacent toes are taped together to provide support and prevent excessive movement, allowing the fractured toe to heal. [10]Buddy taping is a well-known method for treating injuries of the toes, especially proximal interphalangeal (PIP) injuries. [10] However, care must be taken to ensure compliance and avoid skin injuries on the adhesive area of the tape.[10]
- Rigid-Sole Shoe: Wearing a stiff-soled shoe or a postoperative shoe helps protect the injured toe from further trauma and provides additional stability during walking or weight-bearing activities.[5]
- Reduction and Immobilisation:
- Displaced Fractures: In cases where the fractured bone ends are significantly separated, a healthcare professional may perform a reduction procedure to realign the bones [5] After reduction, the toe is immobilised with buddy taping, a splint, cast, or rigid-sole shoe for proper healing.[11] Treatment is warranted for four to six weeks. [9]
- When the displaced fracture involves the first toe, referral for stabilisation of the reduction may be needed. [5] Great toe fractures are treated with a short leg walking boot or cast with toe plate for two to three weeks, then a rigid-sole shoe for an additional three to four weeks. [9]
- Surgical Intervention:
- Open Reduction and Internal Fixation (ORIF): Complex or severely displaced fractures may require surgical intervention. During ORIF, the surgeon realigns the fractured bones and uses screws, plates, or wires to hold the fragments in place for stable healing. [12]
- Medication:
- Pain Management: Over-the-counter pain relievers such as acetaminophen or nonsteroidal anti-inflammatory drugs (NSAIDs) can help manage pain and reduce inflammation during the healing process.[5]
- Physical Therapy:
- Toe Exercises: Once the fracture has started healing, physical therapy may be recommended to improve toe flexibility, range of motion, and strength.[5]
Additional Information[edit | edit source]
Description: In this video Dr. Pelto will discuss about toe fracture xray, when to seek for toe fracture treatment, gout and infection.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Van Vliet-Koppert ST, Cakir H, Van Lieshout EM, De Vries MR, Van Der Elst M, Schepers T. Demographics and functional outcome of toe fractures. J Foot Ankle Surg. 2011 May-Jun;50(3):307-10.
- ↑ Rennie L, Court-Brown CM, Mok JY, Beattie TF. The epidemiology of fractures in children. Injury. 2007 Aug;38(8):913-22.
- ↑ 3.0 3.1 Fife D, Barancik JI. Northeastern Ohio Trauma Study III: incidence of fractures. Ann Emerg Med. 1985 Mar;14(3):244-8.
- ↑ 4.0 4.1 4.2 American Academy of Orthopaedic Surgeons. Toe and Forefoot Fractures. Available from: https://orthoinfo.aaos.org/en/diseases--conditions/toe-and-forefoot-fractures/ [accessed 1/8/2023]
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 5.8 Hatch RL, Hacking S. Evaluation and management of toe fractures. Am Fam Physician. 2003 Dec 15;68(12):2413-8.
- ↑ York PJ, Wydra FB, Hunt KJ. Injuries to the great toe. Curr Rev Musculoskelet Med. 2017 Mar;10(1):104-12.
- ↑ 7.0 7.1 Hermel MB, Gershon-Cohen J. The nutcracker fracture of the cuboid by indirect violence. Radiology. 1953 Jun;60(6):850-4.
- ↑ English TA. Dislocations of the metatarsal bone and adjacent toe. J Bone Joint Surg Br. 1964 Nov;46(4):700-4.
- ↑ 9.0 9.1 9.2 9.3 Bica D, Sprouse RA, Armen J. Diagnosis and Management of Common Foot Fractures. Am Fam Physician. 2016 Feb 1;93(3):183-91.
- ↑ 10.0 10.1 10.2 Won SH, Lee S, Chung CY, Lee KM, Sung KH, Kim TG, Choi Y, Lee SH, Kwon DG, Ha JH, Lee SY, Park MS. Buddy taping: is it a safe method for treatment of finger and toe injuries? Clin Orthop Surg. 2014 Mar;6(1):26-31.
- ↑ Mittlmeier T, Haar P. Sesamoid and toe fractures. Injury. 2004 Sep 1;35(2):87-97.
- ↑ Nishikawa D, Duarte F, Netto C, Monteiro A, Albino R, Fonseca F. Internal Fixation of Displaced Intra-articular Fractures of the Hallux Through a Dorsomedial Approach. A Technical Tip. Foot & Ankle Specialist. 2017; 11(1):77-81.
- ↑ Donald E. Pelto, DPM. Toe Breaks (Fractures) - Is there anything I can do?. Available from: https://www.youtube.com/watch?v=EUKwTUcOu6g [accessed 2/8/20023]
- ↑ Donald E. Pelto, DPM. How Occupational How Do I Do Toe Strapping? (Dislocated and Fractured Toe). Available from: https://www.youtube.com/watch?v=2hvnRKrvhKs [accessed 2/8/20023]
- ↑ ePainAssist. Broken Toe or Fractured Toe: Treatment, Symptoms, Prognosis. Available from: https://www.youtube.com/watch?v=wrBwyJGkgJ4 [accessed 2/8/20023]
- ↑ fdfac. Buddy Splint for Toe Fractures - San Francisco Podiatrist. Available from:https://www.youtube.com/watch?v=PSwxQpDxZWo[accessed 2/8/20023]