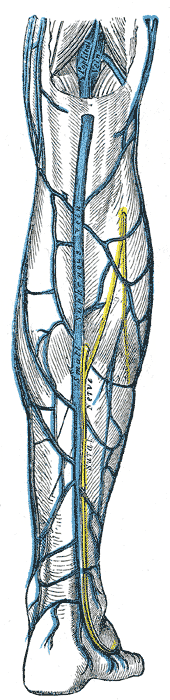
Sural Nerve
Original Editor - Rachael Lowe
Top Contributors - Rachael Lowe, Lucinda hampton, Jin Yoo and Poonam Sepat
Description[edit | edit source]
The Sural Nerve is a cutaneous nerve it provides only sensation, the areas being
- Posterolateral aspect of the distal third of the leg
- Lateral aspect of the foot, heel, and ankle.
It is formed by terminal branches of the tibial and common peroneal nerves that join together in the superficial aspect of the distal third of the leg. See image R Sural Nerve Yellow
- It is purely sensory and easily located anatomically, making it a commonly used site for peripheral nerve biopsies and harvesting for nerve grafting.[1]
Function[edit | edit source]
The sural nerve is purely sensory and it supplies sensation to the lower lateral leg, lateral heel, ankle and dorsal lateral foot.
Clinical relevance[edit | edit source]
Damage to the sural nerve due to injury can occur due to
- Trauma,
- Fractured calcaneus,
- Damage from surgery in the region eg Achilles repair
This injury may not cause significant deficit or disability due to overlap of other nerves.
As the sural nerve is purely sensory function dysfunction results in only a relatively trivial deficit. For this reason, it is often used for nerve biopsy, as well as the donor nerve for nerve grafts. However, there is also evidence of a higher complication rate than peronial nerve biopsy leading to post-operative pain, dysaesthesia and parasthesia during follow ups.[3]
The pathway of the nerve includes a non-extensible anatomic fibrous arcade, beyond which it runs superficially in the distal third of the leg. This arch is wide, thick, and unyielding and may fit tightly around the nerve, causing chronic, frictional irritation. Symptoms most commonly associated with irritation of the sural nerve include chronic (because the diagnosis is usually missed for a long time) pain in the posterior aspect of the leg, usually exacerbated with physical exertion. Radiating pain/tingling into the foot may occur distally, which may or may not be accompanied by referred pain proximally in the calf.
long-term diabetes leads to axonal degeneration in the sural nerves. This condition typically manifests with altered sensation and pain in the area supplied by sural nerve.
Assessment[edit | edit source]
In the case of neural irritation at the location of the fibrous arcade clinical examination may reveals tenderness with palpation posterior and lateral to the myotendonous junction of the Achilles (at the location of the fibrous arcade).
Monofilament testing has also shown good reliability.[4]
Treatment[edit | edit source]
As with any nerve irritation syndrome manual soft tissue techniques can be used to decrease frictional irritation in the area.
References[edit | edit source]
- ↑ Miniato MA, Nedeff N. Anatomy, Bony Pelvis and Lower Limb, Sural Nerve. InStatPearls [Internet] 2019 Sep 6. StatPearls Publishing.Available from:https://pubmed.ncbi.nlm.nih.gov/31536245/ (last accessed 19.9.2020)
- ↑ Dr. Nabil Ebraheim. Sural Nerve Anatomy - Everything You Need To Know - Dr. Nabil Ebraheim. Available from: https://www.youtube.com/watch?v=JAo6GM78tso [last accessed 22/02/2019]
- ↑ Hilton DA. John J. Househam L. Tengah C. Complications following sural and peroneal nerve biopsies. Journal of Neurological Neurosurgery Psychiatry. 2007; 78: 1271-1272
- ↑ Brandsma JW. Wagenaar I. Post E. Nicholls PG. Reliability of Clinical Nerve Function Assessment in Peripheral Neuropathies. Leprosy Review. 2014; 85: 29-35.