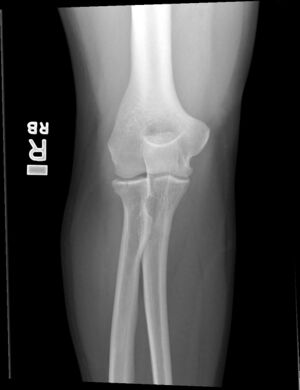
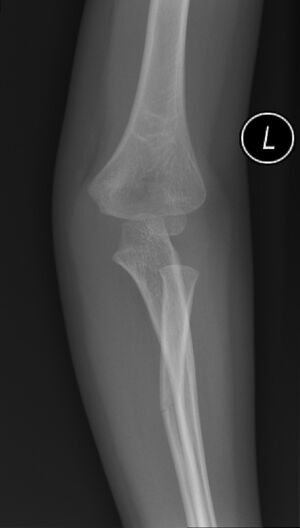
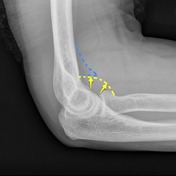
Proximal Radial Head Fracture
Description[edit | edit source]
The radius, located in lateral forearm, is the smaller of the two bones that form the forearm. The radius articulates with the ulna, the second bone in the forearm. These two bones and their articulations form the radioulnar and radiocarpal joints at the elbow and the wrist, respectively.
Radius fractures include the proximal portion of the radius, the neck, and head. This type of fracture is common in adults. Proximal radial fractures occur when falling on an outstretched hand (FOOSH), which pushes the radius into the humerus, or direct trauma to the elbow. Fractures at the proximal radius place the radial head at higher risk for avascular necrosis (AVN).[1]
Clinically Relevant Anatomy[edit | edit source]
The elbow is a synovial hinge joint made up of three articulations– the humeroulnar, humeroradial, and radioulnar. The arm’s humerus meets the forearm’s ulna and radius to create the hinge, while the radius and ulna articulate to create a pivot joint to allow forearm pronation and supination.
Notable landmarks of the proximal radius include the radial head, neck, and tuberosity. The head is round with a flat though slightly concave surface. The flat surface articulates with the humerus. The circumference of the head is contained within the annular ligament and against the radial notch of the ulna where it rotates and glides during pronation and supination. The radial tuberosity serves as an attachment site for the biceps brachii and supinator brevis muscles.[2]
Epidemiology/Etiology[edit | edit source]
Epidemiology[edit | edit source]
Proximal radial head fractures are most common in ages 20-64.[3] However, radial head fractures are seen more in younger men than women. This discrepancy is associated with men experiencing more falls associated with sports or heights whereas women tend to experience fractures later in life due to falls and fragility of the bone.[4]
Etiology[edit | edit source]
The most common mechanism of injury to the radial head is falling on an outstretched hand or falling with the elbow in extension and the forearm pronated, which directs the trauma force through the wrist and forearm to the head of the radius. Some common associated injuries with this type of fracture can be ligamentous such as a lateral collateral ligament (LCL) or medial collateral ligament (MCL) injuries. Dislocation of the elbow can also produce what is known as the “terrible triad” which consists of a dislocation of the elbow, a radial head fracture, and a coronoid fracture.[3]
Characteristics/Clinical Presentation[edit | edit source]
Types of Fractures[edit | edit source]
Proximal radial head fractures, commonly described using Mason classification, have four grades. The orthopedic surgeon determines the diagnosis of different Mason fractures, and they decide the interventions needed. The surgeon’s decision is guided by the diagnostic imaging, Radiographs, MRI, or CT scans.[5] Possible interventions include immobilization that may involve splinting, slings, and or surgery.
Mason Type 1[edit | edit source]
Mason Type 1 fractures are a fissure or margin sector fracture with a non-displaced or a minimally displaced radius with <2 mm discrepancy.[6][7] These fractures can be challenging to identify on a radiograph when the fracture is non-displaced. A CT or MRI scan is needed for further investigation. When dealing with a Mason Type 1 fracture of the proximal radius, there is no mechanical restriction of supination and pronation that occurs in the forearm.[7]
A five percent (5%) chance of a non-union occurs with a Mason Type 1 fracture of the proximal radius.[7] A proximal radius non-union can cause the radial head to subluxate. However, removal of associated fragments of the fracture does not improve the likelihood of subluxation.[7]
Mason Type 2[edit | edit source]
A Mason Type 2 radial head fracture is evident when the radial head is partially fractured with a >2mm displacement.[8]
Mason Type 3[edit | edit source]
Mason Type 3 fractures are complete breaks or comminuted, broken into multiple pieces or fragments. Mason Type 3 fractures can be further described by subclasses. Type 3a is complete displacement of the radial head from the shaft, with the fracture through the radial neck. Type 3b is an articular fracture with the head breaking into two or more pieces. Type 3c involves articular fracture that is rotated and impacted.[8]
Differential Diagnosis[edit | edit source]
The high probability of other injuries occurring with a fall on an outstretched hand (FOOSH) suggests radiographs, MRI, and sometimes CT scan are required to verify the diagnosis and to certify the integrity of all surrounding structures and tissues.[4]
Possible injuries that should be considered and ruled out with a radial head fracture are capitellum fractures, distal radius fractures, distal radio-ulnar joint dislocations, medial collateral ligament (MCL) ruptures, biceps tendon ruptures, triceps tendon ruptures, and elbow dislocations.[4]
Diagnostic Procedures[edit | edit source]
The primary diagnostic tool used for identifying radial head fractures is radiograph. Mason Type 1 fractures do not always show on radiographs. In such cases, a ‘sail sign’ might indicate a fracture. A ‘sail sign’ is a silhouette on a radiograph caused by an enlarged fat pad at the elbow. Current studies are looking at the use of sonography in detecting occult fractures more quickly. Current diagnostic procedures can take upward of three weeks before identifying fracture.[9]
Outcome Measures[edit | edit source]
The Disabilities of the Arm, Shoulder and Hand is an outcome measure used to determine the abilities of a patient’s upper extremity. The questionnaire lists daily activities such as opening a jar, carrying shopping bags, dressing, etc. The patient rates the difficulty of individual activities in this questionnaire 1 to 5, with 1 being ‘No Difficulty’ and 5 being ‘Unable.’ Note that some questions are phrased differently so 1 to 5 range is relabeled as needed, such as ‘None’ to ‘Extreme’ or ‘Strongly Disagree’ to ‘Strongly Agree.’ The score is calculated using the formula ([sum of n responses/n]-1)(25). n = completed items. The score and level of disability have a positive correlation. An additional module is provided for patients using workman compensation or athletes and musicians.[14]
The QuickDASH is a modified version of the DASH outcome measure that is shorter but with evidence of being as precise as the DASH.[15] The QuickDASH contains only 11 questions and utilizes the same rating scale and scoring formula.
These two outcome measures can be utilized with Mason Type 1, 2, and 3 fractures regardless of mechanism of injury.[14]
Examination[edit | edit source]
The mechanism of injury is often falling on an outstretched hand or direct trauma to the elbow. Radial head fractures are common alongside elbow dislocation. Swelling and bruising of the posterior elbow may be visible. Swelling and heat are palpable. Type III fractures may cause visible deformity. The patient has limited active elbow extension/flexion and forearm pronation/supination. Some may experience limited wrist movement as well. Passive range of motion (PROM) is limited due to pain. Empty end feels of muscle guarding can be expected. Palpation of the radial head is painful. Some patients experience numbness in the forearm, hands, and fingers.[16]
Medical Management[edit | edit source]
Non-Surgical Treatment[edit | edit source]
There should be a brief period of immobilization of the arm, which mainly applies to Mason Type 1 fractures. This can be accomplished by the patient utilizing a sling, which is recommended for no longer than 7 days.[3]
Surgical Treatment[edit | edit source]
- An open reduction internal fixation (ORIF) of the radial head has been shown to be beneficial for Mason Type 2 and 3 fractures.
- Radial head resection is an option for sedentary patients or when there is continued pain due to an isolated radial head fracture.
- Radial head arthroplasty for comminuted Mason Type 3 fractures that involve greater than 25% of the radial head is another valid option.[3]
Physical Therapy Management[edit | edit source]
Mason Type 1 Fractures[edit | edit source]
Type 1 non-displaced proximal radial fractures should be treated non-operatively, and the patient is given a sling or splint for a few days.[17] Ice can be used as needed to help control the swelling. As pain permits, the patient should perform active range of motion (AROM) in the early stages of rehabilitation, including forearm supination and pronation. An important aspect of this type of fracture is to mobilize the joint early to decrease any complications of post-traumatic stiffness in the joint.[4] ROM should be considered cautiously when the fracture involves one-third of the articular surface. If the fracture does involve one-third of the articular surface, a sling or splinting should be implemented for at least a two-week period.[7]
Mason Type 2 and 3 Fractures[edit | edit source]
An ORIF is used with Mason Type 2 and 3 fractures, which has demonstrated the best recovery results. There are three phases of physical therapy after fixation. In the first phase, which is 0-14 days, the patient begins with elbow flexion and extension AROM. At the end of the second week, the elbow ROM should be 15-105 degrees. After these ROM requirements are met, the patient begins gripping exercises with putty and isometric strengthening exercises for the elbow and wrist. In phase two, which is from 15 days to 6 weeks, the physical therapist should assess the shoulder and wrist strength along with ROM. The patient continues with elbow AROM and an active-assisted range of motion (AAROM). Elbow flexion and extension ROM should be at the full at the end of six weeks. After this time, the patient begins AROM and AAROM supination and pronation. The patient will continue the isometric strengthening exercises from the first phase working specifically on flexion and extension. In phase three, from week 7 to week 12, the patient continues working on AROM and AAROM with supination and pronation. By the eighth week, full pronation and supination should be achieved. The patient should progress isometric strengthening of elbow flexion and extension, along with wrist pronation and supination. The physical therapist also needs to assess and focus on any additional deficits that result from the fracture and or the surgery.[18]
Education[edit | edit source]
If surgery occurs, the splint should be left in place until the patient’s first postoperative visit, which usually occurs 1-2 weeks after the surgery. Showering is allowed on the second day, but care must be taken to keep the splint clean and dry. Submersion of the elbow area is restricted for at least four weeks after surgery.[5]
Once at home, the patient can walk as much as desired. The patient can drive a car once authorized by the surgeon, which is typically four to six weeks after surgery. Returning to work is based on the patient's duties needed to complete their job and must be cleared by the surgeon to return to employment duties.[5]
The patient should expect to see some swelling in/around the arm after the surgery. The patient should contact the surgeon immediately if skin changes with or without discharge or bleeding are noted around the incision site, or if a fever occurs greater than 101°.[5]
What the patient should not be doing for the first 6 weeks is:
- using the arm to push themselves up in bed or a chair.
- using forceful contraction of muscles required to push off.
- overusing the elbow/arm, which can cause difficulties with the healing process.
- lifting objects that are heavier than a glass of water.
- putting the arm in an extreme position, including straight out to the side or behind the patient’s body.
When needed, the patient should ask for assistance with activities.
At the first postoperative visit with the surgeon (1-2 weeks), the patient's staples/stitches are removed, the wound is examined, and radiographs are obtained to ensure proper healing. The patient is given instructions on next steps and plans for the upcoming weeks after everything is evaluated.[5]
Pain Management[edit | edit source]
Applying an ice pack to the injured area, taking NSAIDs such as ibuprofen or acetaminophen, and using a sling are helpful in managing the pain and swelling associated with radial head fractures.[19]
Rehabilitation[edit | edit source]
Non-Surgical Rehabilitation[edit | edit source]
Early ROM for non-operated simple and complex radial head fractures and early AROM and AAROM of the elbow helps prevent the collection of edema, stiffness, and the formation of adhesions in the capsule and annular ligament. It is also imperative for the patient to focus on the surrounding joints such as the shoulder, wrist, hand, and scapulothoracic joint to ensure ROM and use of the arm has been maintained.[10]
Surgical Rehabilitation[edit | edit source]
Regarding surgical intervention, there are two types of fractures: simple and complex. A simple radial head fracture refers to isolated radial head fractures.[10] According to the Mason classification, Type 2 and Type 3 radial head fractures require surgical intervention to stabilize the radius. A complex radial head fracture is classified as additional instability due to other factors outside of the radial head fracture.[10] In both cases, it is recommended that immobilizing the arm is beneficial to protect and support the arm after surgery. However, immobilization of the arm should only be up to 1 week after surgery for simple fractures and up to 3-6 weeks with a long-arm splint for complex fractures.[10]
Recovery[edit | edit source]
Mason Type 1 Fractures[edit | edit source]
Nonsurgical treatment involves a splint or sling for a few days, followed by early and gradual increase in elbow and wrist movement which depend on the pain level.[17] Complications that can occur with a Mason type 1 proximal radius fractures may include loss of active elbow extension, mild loss of forearm pronation and supination, and occasional fatigue and pain with overuse in the forearm.[7] If excessive motion is promoted too early, it is possible to shift and displace the bones.[17]
Mason Type 2 Fractures[edit | edit source]
If the displacement is minimal the treatment involves the patient wearing a sling or a splint for 1 to 2 weeks and should be completed with ROM exercises.[17]
Mason Type 3 Fractures[edit | edit source]
Early stretching movement and elbow flexion is necessary to avoid elbow contractures or stiffness in elbow ROM.[17]
Some Type 3 fractures require the patient be placed in a splint or sling for a short period of time. The surgeon will recommend the patient not weight-bear through the arm or wrist or lift objects that are heavier than a couple pounds for 6 to 12 weeks.[17] Fractures that occur in the proximal portion of the radial head will result in loss of elbow ROM. The patient should perform exercises to restore ROM and strength to return to their functional activities. A second surgery may be required to remove any scar tissue that develops and limits elbow ROM.[17]
Key Research[edit | edit source]
Swensen et. al discuss outcomes in current treatment of radial head fractures.[20] ORIF of simple fractures is supported by the literature, but optimal treatment of more complex fractures is controversial.
Hacki et. al discuss complications of radial head fracture treatment and detail revisions required.[21]
References[edit | edit source]
- ↑ Proximal radius (radial neck) fractures [Internet]. POSNA. 2022 [cited 2022Apr13]. Available from: https://posna.org/Physician-Education/Study-Guide/Proximal-Radius-(Radial-Neck)-Fractures
- ↑ Gray H. Barnes & Noble. 15th ed. New York, New York: Barnes & Noble; 2010.
- ↑ 3.0 3.1 3.2 3.3 Wang JH, Rajan PV, Castaneda J, Gokkus K. Radial head fractures [Internet]. Orthobullets. 2022 [cited 2022Apr13]. Available from: https://www.orthobullets.com/trauma/1019/radial-head-fractures
- ↑ 4.0 4.1 4.2 4.3 Radial head fractures [Internet]. Radial Head fractures - Musculoskeletal Medicine for Medical Students - OrthopaedicsOne. [cited 2022Apr13]. Available from: https://www.orthopaedicsone.com/display/MSKMed/Radial+Head+fractures
- ↑ 5.0 5.1 5.2 5.3 5.4 Patient education radial head fracture - the Core Institute [Internet]. The Core Institute. 2019 [cited 2022Apr14]. Available from: https://thecoreinstitute.com/wp-content/themes/the-core/documents/patient-education/Radial-Head-Fracture-Patient_Education_PE_ELB_%207-09-2019.pdf
- ↑ Krupko T. Core Curriculum V5 Radial Head and Neck Fractures. Orthopaedic Trauma Association;
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 Type I radial head fracture [Internet]. Wheeless' Textbook of Orthopaedics. 2020 [cited 2022Apr13]. Available from: https://www.wheelessonline.com/joints/type-i-radial-head-fracture/
- ↑ 8.0 8.1 Weerakkody Y. Mason classification of radial head fractures: Radiology reference article [Internet]. Radiopaedia Blog RSS. Radiopaedia.org; 2022 [cited 2022Apr13]. Available from: https://radiopaedia.org/articles/mason-classification-of-radial-head-fractures-1?lang=us
- ↑ Malahias M-A, Manolopoulos P-P, Kadu V, Shahpari O, Fagkrezos D, Kaseta M-K. Bedside ultrasonography for early diagnosis of occult radial head fractures in emergency room: a CT-comparative diagnostic study. Arch Bone Jt Surg. 2018Nov;6(6):539–46.
- ↑ 10.0 10.1 10.2 10.3 10.4 Case 1: radial head fractureR [Internet]. Radiopaedia. 2021 [cited 2022Apr14]. Available from: https://radiopaedia.org/articles/proximal-radial-fracture-summary?lang=us
- ↑ Frontal [Internet]. Radiopaedia. 2015 [cited 2022Apr14]. Available from: https://radiopaedia.org/cases/proximal-radial-shaft-fracture-with-radial-head-subluxation?lang=us
- ↑ Case 1 [Internet]. Radiopaedia. 2008 [cited 2022Apr14]. Available from: https://radiopaedia.org/articles/sail-sign-elbow-1?lang=us
- ↑ Case 3 [Internet]. Radiopaedia. 2008 [cited 2022Apr14]. Available from: https://radiopaedia.org/articles/sail-sign-elbow-1?lang=us
- ↑ 14.0 14.1 About the DASH [Internet]. DASH. [cited 2022Apr13]. Available from: https://www.dash.iwh.on.ca/about-dash
- ↑ Gummesson C, Ward MM, Atroshi I. The shortened disabilities of the ARM, shoulder and hand questionnaire (Quick Dash): Validity and reliability based on responses within the full-length dash. BMC Musculoskeletal Disorders. 2006;7(1).
- ↑ Radial head fracture: Causes, symptoms, diagnosis, treatment [Internet]. OrthoTexas. 2022 [cited 2022Apr13]. Available from: https://www.orthotexas.com/radial-head-fracture-causes-symptoms-diagnosis-treatment/
- ↑ 17.0 17.1 17.2 17.3 17.4 17.5 17.6 Nonunions - orthoinfo - Aaos [Internet]. OrthoInfo. [cited 2022Apr13]. Available from: https://orthoinfo.aaos.org/en/diseases--conditions/nonunions/
- ↑ Kerns GJ. Dr. Garrett Kerns [Internet]. Dr Garrett James Kerns | Orthopaedic Surgery Specialist Saginaw, MI. [cited 2022Apr13]. Available from: https://www.drgarrettkerns.com/pdfs/office-forms/physical-therapy-protocols/elbow/radial-head-orif-protocol.pdf.
- ↑ Radial head fracture - aftercare: Medlineplus medical encyclopedia [Internet]. MedlinePlus. U.S. National Library of Medicine; [cited 2022Apr13]. Available from: https://medlineplus.gov/ency/patientinstructions/000561.htm
- ↑ Swensen SJ, Tyagi V, Uquillas C, Shakked RJ, Yoon RS, Liporace FA. Maximizing Outcomes in the treatment of radial head fractures. Journal of Orthopaedics and Traumatology. 2019;20(1):1–9.
- ↑ Hackl M, Wegmann K, Hollinger B, El-Zayat BF, Seybold D, Gühring T, et al. Surgical revision of radial head fractures: A Multicenter retrospective analysis of 466 cases. Journal of Shoulder and Elbow Surgery. 2019;28(8):1457–67.