Patellofemoral Osteoarthritis
Introduction[edit | edit source]
Osteoarthritis (OA) of the knee is a commonly diagnosed condition with up to 25% of people having signs of Patellofemoral (PF) OA and up to 40% of these people have isolated PF OA[1]. Tibiofemoral (TF) OA tends to be more focused on in research and management as compared to PF OA. However, PF OA contributes to a significant proportion of patients symptoms and functional impairments and should be addressed. Patellofemoral Pain Syndrome is thought to be a precursor to PF OA, but longitudinal studies have yet to conclusively prove this.
Diagnosis [edit | edit source]
To date, there are no specific diagnostic criteria to diagnose PF OA formally. A combination of clinical signs and symptoms as well as radiographic information from X-rays and MRIs are used to diagnose PF OA.
Clinical Features[edit | edit source]
- Anterior knee pain (especially on loading activities eg stair climbing) - this is usually the significant finding in PF OA.
- Knee crepitus
- Swelling
- Pain on Patellofemoral joint (PFJ) compression
- Stiffness after sitting
- Valgus knee deformity
- Reduced Quadriceps Strength
It is important to note that pain may not necessarily be originating from the PF joint itself. The surrounding structures such as the fat pad, ligaments, bursae, muscles etc can also contribute to symptoms[3][4]
Imaging[edit | edit source]
Xray and MRI can both be used to diagnose PF OA. It is important to note that findings on radiological investigations do not always correlate to clinical symptoms. It has been found that in certain individuals who have positive findings on X-ray or MRI do not have any knee pain or other symptoms of PF OA.[3]
X-ray[edit | edit source]
X-ray is most commonly performed in the diagnosis of PF OA. In TF OA the Kellgren and Lawrence (KL) grading system is used; however, there is no standardised scoring system for PF OA. In research, the KL grading system has been used to score PF OA, but it has not been validated for this purpose.
A skyline view is most appropriate to best view the PFJ. The presence of osteophytes, as well as joint space narrowing, confirms the clinical findings for PF OA.
X-rays can be used to interpret the morphology of the PFJ such as the shape of the trochlear where a shallow trochlear has been associated with PF OA.
MRI [edit | edit source]
MRIs findings such as cartilage lesions, osteophytes and bone marrow lesions at the PFJ can be used in the diagnosis of PF OA. There are no formal diagnostic criteria at present to diagnose PFJ on MRI.[3]
Patellofemoral Osteoarthritis and Tibiofemoral Osteoarthritis[edit | edit source]
PF OA and TF OA can be found in isolation or combination. There does seem to be a relationship between the 2 and having either PF or TF OA is a risk factor for developing the other. The PFJ is often the first joint to present with symptoms[3]. It is still unsure as to whether PF OA will always progress to combined OA.[1]
Outcome Measures[edit | edit source]
At present, there are no evidence-based patient-reported outcome measures specifically for PF OA. The KOOS (Knee injury and Osteoarthritis outcome scores) [5] and WOMAC can be used, but they are outcomes focused on general knee OA and not specific for PF OA. Performance tests such as the Timed Up and Go can be used in a PF OA population. However, this test may not be appropriate in the early stages of PF OA as it may not challenge the joint enough.[1]
Risk Factors[edit | edit source]
Abnormal Joint Alignment[edit | edit source]
Patellofemoral, as well as tibiofemoral alignment, has been implicated in PF OA. Treatment targeted at correcting imbalances may be helpful to treat symptoms and prevent progression of the condition.
Patellofemoral alignment[edit | edit source]
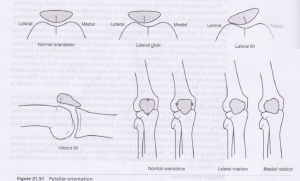
The following alignment patterns of the patella have been shown to be a potential risk factor for PF OA. [6]
- Lateral translation
- Lateral tilt
- Proximal translation (Patella Alta)
A recent study conducted in 2019 by Macri et al used MRI to confirm that those 3 patella positions are commonly found in patients presenting with PF OA.[6]
These alignment problems are commonly found in patients with PFJ pain. It is hypothesised that by correcting these alignment issues the progression to PF OA could possibly be prevented. This is currently still a theory and has not been proven.
Patella’s that are positioned higher (increased proximal translation) have been associated with worse PF OA symptoms. This could potentially due to a lack of stability as there is more time that the patella is not snug in the trochlear.
Tibiofemoral Alignment[edit | edit source]
Varus and valgus angles at the knee can affect the PFJ. Lateral PF OA is more commonly seen in knees with valgus deformities and medial PF OA in varus deformities.[7] It appears that in general valgus deformities target the PFJ more. Isolated PF OA is more commonly found in knees with valgus. Combined PF and TF OA, as well as isolated TF OA, is more commonly found in knees with varus deformities[6].
Abnormal Trochlear Morphology[edit | edit source]
A shallow trochlear is a risk factor for the development of PF OA[7]. Multiple studies have shown that the more severe PF OA patients present with shallow trochlear. They often have increased osteophytes, greater joint space narrowing and more cartilage loss as compared to people with deeper trochlear.[7]
Abnormal Kinetics and Kinematics [edit | edit source]
Decreased quadriceps strength has been shown to be a significant risk factor in PFJ symptoms and development of PF OA.[3] Weakness or dysfunction in the proximal muscles at the hip have been implicated in PF OA such as gluteus medius, minimus and lower hip abductors.[3]
Teng et al (2015) found that progression of PF OA is related to increased peak knee flexion in the terminal stance of gait.[8] Patients with tight hip flexors or those that lack hip extension due to joint stiffness may need to increase knee flexion to forwardly translate foot, as well as those with reduced dorsiflexion due to tight calf muscles or ankle stiffness.[4] Treatments targeted to correct these biomechanical faults may slow the progression of PF OA.
Altered joint alignment, as discussed above, is often not a structural problem and is caused by muscular imbalances. For example, weak quadricep muscles may influence the lateral translation or tilt of the patella. A long patella ligament may cause an increased proximal translation of the patella. Weak hip abductors can also lead to increased femoral internal rotation and abduction leading to altered patellofemoral alignment.[7]
Body Mass Index[edit | edit source]
Adults that suffer from PF pain tend to have a higher BMI [9]. And those with PF OA have a much greater body mass index (BMI) than controls[9].
There is a debate about the association between BMI and PF OA. Is this finding because PF Pain leads to decreased activity and as such BMI increases? Or, is it that the adipose tissue produces adipokines and creates an inflammatory environment that contributes to joint degeneration?
Increased load from an increased BMI has also been proposed as a pain mechanism and cause of PF OA. However, OA is more commonly found in non-weight bearing joints of obese people as well, and these joints do not have an increased load due to BMI.[9] Obese individuals with knee OA were found to have an elevated interleukin-6, and this may contribute to the inflammatory profile that accelerates cartilage degeneration. It has not yet been researched as to whether a reduction in BMI can ultimately change symptoms and radiological findings in PF OA.
Treatment[edit | edit source]
Management in PF OA cannot be a “one size fits all” approach. Patients need to be sub-grouped and bespoke treatment plans created to address their particular risk factors and biomechanical faults.
Taping and Bracing[edit | edit source]
The goal of patellar taping and bracing is to affect the joint alignment. Callaghan et al (2015) determined in their RCT that wearing a Q-brace for 6 weeks alters the volume of bone marrow lesions as well as pain for people with PF OA.[10] The Q brace alters patella position as well as improves patella contact with the trochlea[3]. Taping the patella has also shown to be effective, but its mechanism of action is uncertain and has not been studied to date[3].
Exercise[edit | edit source]
Exercise continues to be the recommended treatment in osteoarthritis in general. In PF OA targeted exercises based on individual patients assessment would be best practice to manage symptoms and prevent further degeneration. There is limited evidence on exercise in PF OA specifically[3] however it has been suggested that improving the function vastus medialis oblique (VMO) muscle in patients with patellofemoral disorders reduces the pressure applied on the lateral cartilage within the patellofemoral joint thus helps to reduce symptoms [11].
Surgical[edit | edit source]
Patella resurfacing has been suggested as a surgical option in the treatment of PF OA. There has been 1 study to date and this did not show any difference between the intervention and control group[3]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Lankhorst NE, Damen J, Oei EH, Verhaar JA, Kloppenburg M, Bierma-Zeinstra SM, van Middelkoop M. Incidence, prevalence, natural course and prognosis of patellofemoral osteoarthritis: the Cohort Hip and Cohort Knee study. Osteoarthritis and cartilage. 2017 May 1;25(5):647-53.
- ↑ Patellofemoral joint Arthritis Indications for Treatment by Dr. S. Hayasaka. Available from:https://www.youtube.com/watch?v=zKrzvjfkkpg&ab_channel=OrthofracsAOA
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 3.9 van Middelkoop M, Bennell KL, Callaghan MJ, Collins NJ, Conaghan PG, Crossley KM, Eijkenboom JJ, van der Heijden RA, Hinman RS, Hunter DJ, Meuffels DE. International patellofemoral osteoarthritis consortium: consensus statement on the diagnosis, burden, outcome measures, prognosis, risk factors and treatment. In Seminars in arthritis and rheumatism 2018 Apr 1 (Vol. 47, No. 5, pp. 666-675). WB Saunders.
- ↑ 4.0 4.1 Robertson C. Patellofemoral Osteoarthritis Course Slides. Plus. 2019
- ↑ Crossley KM, Macri EM, Cowan SM, Collins NJ, Roos EM. The patellofemoral pain and osteoarthritis subscale of the KOOS (KOOS-PF): development and validation using the COSMIN checklist. British journal of sports medicine. 2018 Sep 1;52(17):1130-6.
- ↑ 6.0 6.1 6.2 Macri EM, d'Entremont AG, Crossley KM, Hart HF, Forster BB, Wilson DR, Ratzlaff CR, Goldsmith CH, Khan KM. Alignment differs between patellofemoral osteoarthritis cases and matched controls: An upright 3D MRI study. Journal of Orthopaedic Research®. 2019 Mar;37(3):640-8.
- ↑ 7.0 7.1 7.2 7.3 Macri EM, Stefanik JJ, Khan KK, Crossley KM. Is tibiofemoral or patellofemoral alignment or trochlear morphology associated with patellofemoral osteoarthritis? A systematic review. Arthritis care & research. 2016 Oct;68(10):1453-70.
- ↑ Teng HL, MacLeod TD, Link TM, Majumdar S, Souza RB. Higher knee flexion moment during the second half of the stance phase of gait is associated with the progression of osteoarthritis of the patellofemoral joint on magnetic resonance imaging. journal of orthopaedic & sports physical therapy. 2015 Sep;45(9):656-64.
- ↑ 9.0 9.1 9.2 Hart HF, Barton CJ, Khan KM, Riel H, Crossley KM. Is body mass index associated with patellofemoral pain and patellofemoral osteoarthritis? A systematic review and meta-regression and analysis. Br J Sports Med. 2017 May 1;51(10):781-90.
- ↑ Callaghan MJ, Parkes MJ, Hutchinson CE, Gait AD, Forsythe LM, Marjanovic EJ, Lunt M, Felson DT. A randomised trial of a brace for patellofemoral osteoarthritis targeting knee pain and bone marrow lesions. Annals of the rheumatic diseases. 2015 Jun 1;74(6):1164-70.
- ↑ Adel J, Koura G, Hamada HA, El Borady AA, El-Habashy H, Balbaa AE, Saab IM. Squatting versus squatting with hip adduction in management of patellofemoral osteoarthritis: A randomized controlled trial. Journal of back and musculoskeletal rehabilitation. 2019 Jan 1;32(3):463-70.