Management of Traumatic Brain Injury in Disaster Situations
Original Editor - Naomi O'Reilly
Top Contributors - Naomi O'Reilly, Kim Jackson, Rachael Lowe, Tony Lowe, Admin and Jess Bell
Introduction[edit | edit source]
Disaster, as defined by the United Nations, is a serious disruption of the functioning of a community or society, which involve widespread human, material, economic or environmental impacts that exceed the ability of the affected community or society to cope using its own resources.[1] According to the International Federation of Red Cross & Red Crescent Societies a disaster occurs when a hazard impacts on vulnerable people. The combination of hazards, vulnerability and inability to reduce the potential negative consequences of risk results in the disaster. [2] While disasters can be caused by nature, the human influence on disasters have been widespread throughout the centuries, particularly in relation to conflict situations. Natural disasters and armed conflict are two of the main types of disasters and have marked human existence throughout history resulting in peaks in mortality and morbidity. [3] Find out more about the different types of disasters and disaster management here.
While accurate data is scarce, traumatic brain injury remains a common neurological consequence of disasters, natural and man made. A wide range of mild, moderate, and severe traumatic brain injury occur secondary to overpressure, penetrating wounds, and crush injuries following the huge kinetic energy released by rapid-onset natural disasters. Disaster preparedness planners and emergency medical personnel face a major challenge in preventing and managing neurotrauma within this context. As with any traumatic brian injury, management is complex and individuals often have long-term physical, cognitive and behavioural impairments with residual neurological deficits, medical complications all resulting in lifestyle consequences, which necessitate comprehensive interdisciplinary management, including medical, surgical and rehabilitation. [4]
Key recommendations from a rehabilitation perspective for traumatic brain injury survivors in disaster settings included patient/carer education, general physiotherapy, practice in daily living activities and safe equipment use, direct cognitive/behavioural feedback, basic compensatory memory/visual strategies, basic swallowing/communication, and psychological input. More advanced interventions are generally not applicable following disasters due to limited access to services, trained staff/resources, equipment, funding, and operational issues.
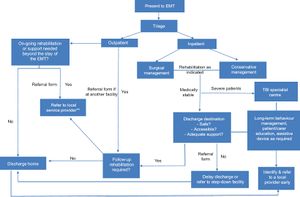
Immediate Emergency Care[edit | edit source]
Early diagnosis and treatment of traumatic brain injuries can be challenging under normal circumstances, but are further exacerbated in the aftermath of disaster due to to the chaotic environment including damaged infrastructure, poor communication and shortages of relevant health and rehabilitation workers, particularly neurotrauma specialists. [5]
During this early stage, immediate diagnosis and treatment remains key to minimise the development of secondary brain injuries, which is a massive challenge, particularly in developing countries where medical infrastructure and availability of state-of-the-art neurological care is already scare and may be further limited as a result of the disaster. Families are often separated, and symptoms of posttraumatic stress disorder can be common during the postacute phase.
As a result, early deployment of specialised emergency medical teams to meet the immediate needs of disaster victims is a key element of the immediate emergency response, and is guided by a range of World Health Organization initiatives, including Emergency Response Frameworks (Standards and Guidelines); Coordination Mechanisms, Emergency Medical Team Accreditation Process ensuring that rehabilitation professionals form part of the Emergency Medical Teams. [5][6]
Specialised care teams are defined by the World Health Organization as “national or international teams embedded into Emergency Medical Teams or a national facility to provide specialist care”, which may include rehabilitation teams and are deployed based on the response to meet specific needs required at the request of the host health authorities. These teams should be multidisciplinary and need to be integrated into a disaster response and management plan and their skills need to be shared with local rehabilitation and health-care providers through mentoring and educating/training." [4]
A specialised care team that is focused on traumatic brain injury rehabilitation in a disaster setting should include; [4][6]
| Rehabilitation Interventions | General Applicability of Recommendations in Disaster Settings | |
|---|---|---|
| Weak | ||
| Team Composition | Minimum Technical Standard;
A traumatic brian injury specialised rehabilitation team should be led by a rehabilitation physician and comprise of at least three other professionals from different disciplines, including rehabilitation medicine, nursing, physiotherapy, occupational therapy, speech and language therapy, and psychology. In addition, a team lead is required to represent the care team at health coordination level | |
| Qualification and Experience | Minimum Technical Standard;
Rehabilitation professionals in a traumatic brian injury specialised care team should have at least 6 months’ experience working in a traumatic brain injury unit or with traumatic brain injury patients in a major trauma center and at least 3 years of postqualifying clinical experience At least one team member, preferable the team leader, should have experience in emergency response and all team members should have undergone training in working in austere environments | |
| Rehabilitation Equipment | Minimum Technical Standard;
Specialized care teams for rehabilitation should have capability to rapidly provide the equipment here. | |
| Length of Stay | Minimum Technical Standard;
A team that embeds into a local facility should plan to stay for at least 1 month with evidence of a exit strategy and release mechanism. | |
Rehabilitation[edit | edit source]
The overriding objective of traumatic brain injury care in disaster settings has now extended well beyond survival and acute management to successful implementation of rehabilitation structures to work towards reintegration of the individual with a traumatic brain injury back into home and community. The World Health Organization minimum standards for rehabilitation recommendations for managing patients with traumatic brain injury following a disasters include; [4][7]
- Cognitive and neurological changes should be monitored and regularly assessed
- Early referral to a step-down facility using local rehabilitation providers and support networks, as required
- Appropriate mobility aids prescribed for long-term mobility deficits using local service provider
- Patients with long term or permanent nerve injury considered for orthotic device, sought from a local provider
- Referral pathways identified for microsurgery for appropriate patients
Rehabilitation is a vital element of the treatment and management process post traumatic brain injury in a disaster setting and should prepare individuals with long-term impairment, their care providers and local rehabilitation personnel to manage their ongoing needs over a longer term and should be started early following any disaster.[7] Rehabilitation should focus on comprehensive assessment for neurological and functional limitations and individualised treatment program for specific functional goals with ongoing monitoring of outcomes. The goal of rehabilitation in a disaster setting is to improve functional outcomes, minimise secondary complications, and successful reintegration into the community, with an emphasis on patient and care giver education and self-management. Survivors of traumatic brain injury need support for acquisition of essential skills for maximum return to their previous level of functional independence, regardless of whether specific impairments can be eliminated. [4]
Role of the Physiotherapist[edit | edit source]
Physiotherapists initially involved in disaster settings, were physiotherapists employed in military service including the United States and British Armed Forces, whose primary role involved triage of acute orthopaedic trauma, wound care, as well as respiratory care in critical settings. Despite the range of roles these physiotherapists and others have provided in disasters situations, many disaster response organisers did not know how to utilise physiotherapist skills to provide maximum effect as a result of a lack of clearly defined roles within the emergency response teams in disaster settings.[8] Historically physiotherapists were not routinely included in immediate post disaster emergency medical teams, but this is slowly changing and physiotherapists are now being recognised for the role they can play in disaster response. Discussions between the World Confederation for Physical Therapy and physiotherapists involved in humanitarian responses identified a need to advocate for the presence of rehabilitation professionals, including physiotherapists, in all phases of disaster management and to affirm the need for the establishment or development of physiotherapy services in disaster settings through strengthening of the physiotherapists role in preparedness and promotion of our role within emergency medical teams. This led to development of a wide range of resources and increased awareness of physiotherapists role, and with that an increase in physiotherapists involved in all phases of disaster management.[8]
According to Pete Skelton, Physiotherapist and Rehabilitation Project Manager at Humanity and Inclusion and UK International Emergency Trauma Register member, ‘Physiotherapy is starting to become a central part of the global humanitarian response... and we play a critical role, which goes way beyond just rehabilitation. The role of physiotherapists in emergency situations differs significantly depending on the context.... but may include working in a field hospital providing acute surgical care, working on an outpatient basis, providing care in people’s homes or providing prosthetic provision in a temporary clinic.’ [9]
Humanity & Inclusion has played a huge role in working towards integration of rehabilitation into the UK Emergency Medical Team, which has involved the recruitment and training of rehabilitation professionals to join the teams, and working with partner organisations to ensure the field hospital is fully equipped and accessible with all relevant equipment required by rehabilitation professionals. This has enabled early access to rehabilitation including the provision of essential equipment such as wheelchairs and orthotics, psychosocial support, and onward referral.[9]
Responsibilities[edit | edit source]
You are only expected to work to your level of expertise, knowledge and competence. If an assessment is needed that you are not competent to complete, ask and see if there is anyone else available or who will be available in the future to complete it if it can wait for specific expertise. The assessment of a patient in a humanitarian crisis where possible should still be the same as the assessment you would complete in a typical brain injury setting.[10]
Role in Preparation Phase[edit | edit source]
Physiotherapists have a significant contribution to make in disaster preparedness and should be included in disaster management planning and implementation. Specific humanitarian and clinical training and registering with international medical teams or international non-governmental organisations (INGOs) is key for any physiotherapists interested in international humanitarian response.[8]
Role in Response Phase[edit | edit source]
Growing evidence supports the role that rehabilitation, including physiotherapy, should be considered a central part of the disaster response from the onset of a disaster with physiotherapists involved not only in direct provision of rehabilitation, but also involved in assessment, coordination, psycho-social support and advocacy. Rehabilitation in humanitarian disasters is best provided by experienced local providers, with support from specialist disaster response rehabilitation expertise as resquired, working as an integral part of specially trained emergency medical teams.[8]
Before commencing rehabilitation ensure that any contaminant injuries have been treated/ stabilised and consider what influence these may have on your treatment choices, as it is unlikely that patients will present only with an acquired brain injury following a sudden onset disaster. Likely other injuries are fractures, amputations and especially spinal cord injury that can be easily missed.[10]
The use of detailed outcome measures may not be appropriate in the early stages of an emergency response, but as you enter the rehabilitation phase you still need to be able to demonstrate change in your patient’s abilities in order to help shape future therapy sessions and rehab goals.[10]
Role in Recovery Phase[edit | edit source]
Physiotherapists provide a key link between disaster response and recovery through rehabilitation capacity building and planning service delivery, accessibility, and inclusion. As is normally expected with traumatic brain injury rehabilitation, planning for recovery should be initiated as early as possible and should incorporate a team based approach. Where possible, the recovery phase should be locally led and following a disaster will also often incorporate a range of multi-agency stakeholders, often supported by international respondents. Where these international respondents are physiotherapists, a large part of their role should focus on local capacity building, through training, service development, and the establishment of formal education programmes where they are absent.[8]
The following report and clinical manual provide more detailed information in relation to the role of the Physiotherapist in a disaster setting and outline the assessment process to consider when working with individuals with a traumatic brain injury.
The Role of Physical Therapists in Disaster Management
This report highlights the need for physical therapist involvement in disaster management and particularly in Emergency Medical Teams and provides information for physical therapists who want to work in the field, and national and international agencies who are already working in the field. Each section includes information on the role of the physical therapists and details guidelines and resources to support practice in disaster management. [8]
Rehabilitation in Sudden Onset Disasters - Chapter.8 Acquired Brain Injury
This module was developed by Association of Chartered Physiotherapists in Neurology (ACPIN) members with a special interest in brain injury, working in collaboration with Handicap International. The acquired brain injury chapter aims to provide an overview of how to provide acute rehabilitation for patients with brain injury in an austere, emergency situation, when working as part of a medical team. It is based on best available evidence in the UK, with consideration for particular challenges seen in a humanitarian environment.
Guidelines[edit | edit source]
Independently extracted, compared, and categorised evidence-based rehabilitation intervention recommendations for rehabilitation interventions were synthesised from currently published traumatic brain injury Clinical Practice Guidelines, developed by the Department of Labor and Employment (DLE); Scottish Intercollegiate Guidelines Network (SIGN); Department of Veterans Affairs/Department of Defence (DVA/DOD); and American Occupational Therapy Association (AOTA) for applicability in disaster settings. [7] As a result of the complexities related to the environment, resources, service provision, and workforce in disasters settings many recommendations for traumatic brain injury care are challenging to implement and more advanced interventions are generally not applicable due to limited access to services, trained staff/resources, equipment, funding, and operational issues.[7] Patient/carer education, general physical therapy, practice in daily living activities and safe equipment use, direct cognitive/behavioural feedback, basic compensatory memory/visual strategies, basic swallowing/communication, and psychological input are the key recommendations from a rehabilitation perspective that have been fond to be most applicable for survivors of traumatic brain injury in disaster settings. The following table outlines the general applicability of clinical practice guidelines for traumatic brain injury in disaster settings.[7]
| Rehabilitation Interventions | General Applicability of Recommendations in Disaster Settings | ||
|---|---|---|---|
| Weak | Moderate | Strong | |
| Patient Education |
| ||
| Gait, Balance and Mobility |
|
Task-Specific Training
Repetitive Training |
|
| Spasticity and Muscle Tone |
|
|
|
| Sleep Disturbance Management |
| ||
| Cognitive Rehabilitation |
|
|
|
| Behavioural and Emotional Disorders |
|
Comprehensive Neurobehavioural Program
|
|
| Activities of Daily Living |
|
|
|
| Post-Traumatic Headache Management |
|
| |
| Service Delivery |
|
|
|
Summary[edit | edit source]
“Early rehabilitation can greatly increase survival and enhance the quality of life for injured survivors.”[11]
Current advances in disaster response and management have improved survival rates of disaster victims, resulting in increased number of survivors. Traumatic brain injury is one of the more common complex injuries post sudden onset disaster and survivors often have long-term physical, cognitive and behavioural disabilities, residual neurological deficits, medical complications and lifestyle consequences, which necessitate comprehensive interdisciplinary management, including medical, surgical and rehabilitation. The goal of rehabilitation in disaster settings is to improve functional independence and successful reintegration into the community, with an emphasis on patient education and self-management. [4][8]
Physiotherapists are now considered key health care members involved in all phases following sudden onset disaster, including early involvement with emergency medical teams. Several unique areas of skill are offered by physiotherapists, including those of assessing and treating casualties with acute injuries, preventing injury among rescue workers, and possibly preventing or lessening the burden of chronic dysfunction amongst patients after the emergency phase, with a major main strength being our focus on functional outcomes combined with the ability carry out thorough, musculoskeletal and neurological examinations, often with limited resources. [4][8]
There is a need that all rehabilitation professionals have the required clinical skills to effectively manage all commonly seen conditions in an environment that may be unpredictable and with access to limited resources and supervision. To ensure safe and effective clinical practice, national and international standards, including the WCPT Guideline for Standards of Physical Therapy Practice [12] and the wide range of Clinical Guidelines for working in Disaster settings should be consulted.
Resources[edit | edit source]
Clinical Guidelines & Standards[edit | edit source]
Responding Internationally to Disasters: Do’s and Don’ts
When disasters strike, there is always a huge amount of goodwill from rehabilitation professionals around the world who wish to use their skills to support those affected. This brief guidance informs those who are considering responding internationally to a disaster either as individuals or as part of a team. It highlights key questions to consider before departing, whilst working in the disaster area, and on returning home. Responses to these questions considered are presented as “Do’s and Don’ts” which are exempli ed by recommended practices and those to avoid in the real case studies below. The guidance note is not intended to be a step-by-step or technical guide, nor is it exhaustive, and does not supersede any specific guidance provided by your own global professional body. [13]
Minimum Technical Standards and Recommendations for Rehabilitation: Emergency Medical Teams
This document is the result of collaboration between a working group of rehabilitation experts convened by the World Health Organization and external consultations. It is thus based on a collective experience in rehabilitation during responses to recent large-scale emergencies and also on published data. In time, the minimum standards for rehabilitation in emergencies will be part of a broader series of publications based on the Classification and Minimum Standards for Foreign Medical Teams in Sudden Onset Disaster. The purpose of this document is to extend these standards for physical rehabilitation and provide guidance to Emergency Medical Teams (EMTs) on building or strengthening their capacity for and work in rehabilitation within defined coordination mechanisms.[14]
A Guidance Document in simple language for health personnel, setting out their rights and responsibilities in conflict and other situations of violence. It explains how responsibilities and rights for health personnel can be derived from international humanitarian law, human rights law and medical ethics.The document gives practical guidance on: the Protection of Health Personnel, the Sick and the Wounded, Standards of Practice, the Health Needs of Particularly Vulnerable People, Health records and transmission of medical records, Imported Health Care including Military Health Care, Data Gathering and Health Personnel as witnesses to violations of International Law and Working with the Media.[15]
Rehabilitation in Sudden Onset Disasters
The role of rehabilitation professionals in responding to sudden onset disasters, such as earthquakes or tsunamis, is evolving rapidly, and they increasingly find themselves at the forefront of emergency response teams. This manual is designed for Physiotherapists and Occupational Therapists who provide rehabilitation in the immediate aftermath of a sudden onset disaster. It was developed to support volunteers on the UK International Emergency Trauma Register, but with the aim of being relevant to all rehabilitation professionals interested in rapid deployment to austere environments.[16]
The Role of Physical Therapists in Disaster Management
This report highlights the need for physical therapist involvement in disaster management and particularly in Emergency Medical Teams and provides information for physical therapists who want to work in the field, and national and international agencies who are already working in the field. Each section includes information on the role of the physical therapists and details guidelines and resources to support practice in disaster management. It also outines a range of relevenat case studies providing real world exmaples of the roles physiotherapists play in post disaster settings.[8]
Communicable Disease Control in Emergencies - A Field Manual
This manual is intended to help health professionals and public health coordinators working in emergency situations prevent, detect and control the major communicable diseases encountered by affected populations.[17]
Joint Trauma System Clinical Practice Guideline: Neurosurgery and Severe Head Injury (CPG ID:30)
Provides guidelines and recommendations for the treatment and medical management of casualties with moderate to severe head injuries in an environment where personnel, resources and follow-on care may be limited.[18]
Screening Tools[edit | edit source]
Military Acute Concussion Evaluation 2 (MACE 2)
The 2018 Military Acute Concussion Evaluation 2 (MACE 2) is an acute assessment tool for all medically trained personnel who treat service members involved in a potentially concussive event. The MACE 2 incorporates current state-of-the-science traumatic brain injury information, including vestibular-ocular-motor screening.
The Brief Traumatic Brain Injury Screen
The Brief Traumatic Brain Injury Screen (BTBIS), is a 3 Question Defence and Veterans Brain Injury Centre Screening Tool used to identify service members who may need further evaluation for mild traumatic brain injury. It was validated in a small, initial study conducted with active duty service members who served in Iraq/Afghanistan between January 2004 and January 2005.
Relevant Organisations[edit | edit source]
World Health Organization Emergency Medical Teams Initiative
The purpose of the EMT initiative is to improve the timeliness and quality of health services provided by national and international Emergency Medical Teams and enhance the capacity of national health systems in leading the activation and coordination of this response in the immediate aftermath of a disaster, outbreak and/or other emergency. Teams shall also include public health expertise and logistics support either included in the team or as specific public health or logistics rapid response teams.
International Committee of the Red Cross
Established in 1863, the ICRC operates worldwide, helping people affected by conflict and armed violence and promoting the laws that protect victims of war. An independent and neutral organisation, its mandate stems essentially from the Geneva Conventions of 1949. We are based in Geneva, Switzerland, and employ some 16,000 people in more than 80 countries. The ICRC is funded mainly by voluntary donations from governments and from National Red Cross and Red Crescent Societies.
Humanity & Inclusion works alongside disabled and vulnerable people in situations of poverty and exclusion, conflict and disaster.
UK-MED have been responding to emergencies around the world since 1988, when a team of eight Manchester clinicians led by our founder Prof. Tony Redmond, went to Armenia in aid of those who had been hit by a devastating earthquake.
References[edit | edit source]
- ↑ United Nations Office for Disaster Risk Reduction. Terminology. http://www.unisdr.org/we/inform/terminology#letter-p [Accessed 29 Sep 2019]
- ↑ International Federation of Red Cross and Red Crescent Societies. What is a Disaster. http://www.ifrc.org/en/what-we-do/disaster-management/about-disasters/what-is-a-disaster/. [Accessed: 9 Jan 2017]
- ↑ Leaning J, Guha-Sapir D. Natural Disasters, Armed Conflict, and Public Health. New England Journal of Medicine. 2013 Nov 7;369(19):1836-42
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 Amatya B, Vasudevan V, Zhang N, Chopra S, Astrakhantseva I, Khan F. Minimum technical standards and recommendations for traumatic brain injury rehabilitation teams in sudden-onset disasters. The Journal of the International Society of Physical and Rehabilitation Medicine. [serial online] 2018 [cited 2019 Oct 19];1:72-94. Available from: http://www.jisprm.org/text.asp?2018/1/2/72/249854
- ↑ 5.0 5.1 Regens JL, Mould N. Prevention and treatment of traumatic brain injury due to rapid-onset natural disasters. Frontiers in public health. 2014 Apr 14;2:28.
- ↑ 6.0 6.1 Vasudevan V, Amatya B, Chopra S, Zhang N, Astrakhantseva I, Khan F. Minimum technical standards and recommendations for traumatic brain injury specialist rehabilitation teams in sudden-onset disasters (for Disaster Rehabilitation Committee special session). Annals of Physical and Rehabilitation Medicine. 2018 Jul 1;61:e120.
- ↑ 7.0 7.1 7.2 7.3 7.4 Lee SY, Amatya B, Judson R, Truesdale M, Reinhardt JD, Uddin T, Xiong XH, Khan F. Applicability of traumatic brain injury rehabilitation interventions in natural disaster settings. Brain injury. 2019 Aug 24;33(10):1293-8. DOI: 10.1080/02699052.2019.1641748
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 8.6 8.7 8.8 World Confederation for Physical Therapy. WCPT Report: The Role of Physical Therapists in Disaster Management. London, UK: WCPT; 2016
- ↑ 9.0 9.1 Chartered Society of Physiotherapists. Physio 15: Physios should be core part of response to humanitarian emergencies. Available from: https://www.csp.org.uk/news/2015-10-23-physio-15-physios-should-be-core-part-response-humanitarian-emergencies (accessed 30/09/2019)
- ↑ 10.0 10.1 10.2 Skelton, P and Harvey, A editors. Rehabilitation in Sudden Onset Disasters. Handicap International/ UK Emergency Medical Team Chapter.8 Acquired Brain Injury. 2015
- ↑ Sphere. The Sphere Handbook 2018 Humanitarian Charter and Minimum Standards for Humanitarian Response. 2018 Available form: https://www.spherestandards.org/handbook-2018/
- ↑ World Confederation for Physical Therapy. WCPT Guideline for Standards of Physical Therapy Practice. London, UK: WCPT; 2011. https://www.wcpt.org/sites/wcpt.org/files/files/Guideline_standards_practice_complete.pdf (Access date 22nd September 2019)
- ↑ Skelton, P and Foo, W editors. Resonding Internationally to Disasters: Do's and Don'ts Guide for Rehabilitation Professionals. 2016
- ↑ Emergency Medical Teams: Minimum Technical Standards and Recommendations for Rehabilitation. Geneva: World Health Organization; 2016. Licence: CC BY-NC-SA 3.0 IGO.
- ↑ Coupland R, Breitegger A. Health Care in Danger. the Responsibilities of Health-Care Personnel working in Armed Conflicts and Other Emergencies. Geneva: ICRC. 2012.
- ↑ Skelton, P and Harvey, A editors. Rehabilitation in Sudden Onset Disasters. Handicap International/ UK Emergency Medical Team 2015
- ↑ Connolly MA, editor. Communicable Disease Control in Emergencies: A Field Manual. World Health Organization; 2005.
- ↑ McCafferty RR, Neal C, Marshall S, Pamplin J, Bell R, Rivet D, Hood B, Cooper P, Stockinger ZT. Neurosurgery and severe head injury (CPG ID: 30). San Antonio, TX: Joint Trauma System. 2017