Integrating 2D Video Analysis with Symptom Modification Procedure, Intervention & Telehealth
Original Editor - Thomas Longbottom based on the course by
Damien Howell
Top Contributors - Thomas Longbottom, Kim Jackson, Jess Bell and Stacy Schiurring
Introduction[edit | edit source]
The ability to observe and analyse movement is important in the management of movement system impairment syndromes. When deciding whether or not to use 2D slow motion video analysis to facilitate this process, one must consider a number of related issues, including potential indications for and benefits of this practice, possible barriers to its implementation, techniques for capturing the video and conducting the analysis, and specifics regarding the identification of atypical or deviant movement. Finally, the provider considering using this technology needs to determine how best to apply the information learned through this analysis in appropriate symptom modification and interventions designed to alleviate the patient’s identified problems.
The Clinical Reasoning Process[edit | edit source]
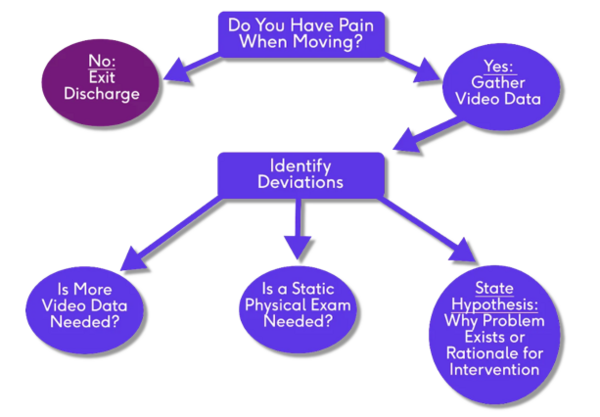
Identify a movement that reproduces the symptoms. Think of this as "poking the bear".[1]
The first step is to observe the movement. A decision will need to be made. Is real-time observation adequate or is 2D slow motion video analysis needed? The movement analysis should lead to a hypothesis of the impairment causing the movement abnormality.[2] This hypothesis can be tested, and the movement analysis may lead the clinician to examine structural variations. For example, if the hypothesised impairment is a problem of weakness, this can be confirmed by strength testing. If the problem is pain, then the search may begin for a movement modification that is accompanied by a reduction in that pain.
This clinical reasoning process employs the "If, then" sequence of thought, where the hypothesis is used to explain why a problem exists and then to justify the treatment choice. If common musculoskeletal pain syndromes and the movement deviations associated with those syndromes are identified, then verbal cues can be identified to alter the movement deviations.[1][3][4]
Identify a series of sequential techniques such as alternate movements, postures, alignments, and/or adaptive equipment that reduces or alleviates the symptoms within the treatment session.[1]
This step employs the symptom modification procedure. This is a useful contemporary approach by physiotherapists to target the reduction of symptoms and the improvement of function by identifying movements that provoke symptoms and then modifying that movement.[5] The reduction of symptoms is the key factor in identifying the correct movement modifier. For example, spinal pain encountered during a sit-to-stand movement may be reduced by minimising lumbar flexion and increasing flexion at the hip accompanied by abdominal bracing. In this case, mediolateral shear was decreased.[6] In a different case, a movement accompanied by increased mediolateral shear, indicating a different biomechanical change, may be the one that reduces the symptoms.[6] The correct movement strategy is the one that modifies the symptoms in the desired manner.
The use of 2D slow motion video analysis may allow the clinician to identify the atypical movement associated with symptom provocation and bring the nature of this movement to the awareness of the patient. This is the point at which the clinician should develop a working hypothesis to explain why the movement problem exists and then begin determining the movement modifier that leads to symptom reduction.[1]
This step involves generating a working hypothesis or a series of working hypotheses that may justify the potential intervention that will decrease or eliminate the symptoms.[1]
The working hypothesis should be tested, and movement re-examined to assess the effect on the symptoms. The intervention may be verbal cues to correct the deviant movement. Determine if there is any change, if the symptoms are alleviated, decreased, or increased, or if there is any unintended consequence. For example, the patient may exhibit a limp which is corrected via verbal cues, but this results in increased hip pain. The intervention should be modified at this point, perhaps with use of an assistive device, or with strengthening of the gluteal muscles, so that the movement deviation may be eliminated along with reduction of the pain.[1]
Potential Side Effects: It is helpful to have prepared the patient ahead of time for the potential of side effects. This can increase the patient's level of engagement, help the clinician be prepared to mitigate the side effects if and when they manifest and facilitate timely adjustments of the intervention.
- Is there a cognitive overload for the patient? If so, the patient potentially just needs to practise the movement.[1]
- Is there an increase in energy expenditure? The ramifications of this may be positive from a conditioning perspective, or perhaps in terms of weight loss for a patient who has a high body mass index. If this side effect is a negative one, appropriate adjustments to the intervention may be determined.[1]
- Is there an increase in muscle fatigue and soreness? The clinician must decide if this is at an acceptable level or indeed harmful to the patient.[1]
- Be aware of the potential "nocebo" effect, where the patient's "negative beliefs, anticipations, or experiences related to the treatment"[7] results in a negative outcome being associated with that intervention. Despite this potential, proactively preparing the patient for potential side effects can increase the patient's level of engagement with the provider and help facilitate timely adjustments of the interventions.[1]
Advantages of Symptom Modification Procedure for the Client[edit | edit source]
- Provides within session reduction and/or elimination of symptoms
- Provides some autonomy or control of the problem, enhanced self-confidence
- Increases the level of self-awareness which by itself is often therapeutic
- Facilitates individualisation of intervention
- Facilitates earlier return to desired activity
- Facilitates desensitisation therapy when dealing with a high level of fear avoidance behaviour
- Can decrease the number of healthcare visits and costs[1]
Advantages of Symptom Modification Procedure for the Clinician[edit | edit source]
- Improves communication when client can see immediate benefits
- Facilitates the all-important level of patient engagement
- Assists in determining whether treatment should continue or whether referral to a different kind of healthcare provider is needed
- Can provide a systematic clinical reasoning process to facilitate proper diagnosis
- Can provide a systematic clinical process to facilitate reliability testing[1]
Shortcomings of Symptom Modification Procedure[edit | edit source]
Be aware that "poking the bear" does not work for everyone. A change in movement performance is not the same as learned behaviour; the patient will still need practice and training. The clinician should also recognise that the rationale for the reduction of symptoms with the altered movement may not be known. It could be due to a change in the biomechanics, altered motor control, or even the placebo effect. While it is easy to assume that control of the symptoms indicates a successful intervention, looking further into the cause of the impairment and further appropriate steps to intervene for a long-term, sustained result may be beneficial. Finally, consider that the inability to provoke or modify the symptoms by altering the movement may indicate the need for referral to a more appropriate healthcare provider.[1]
Telehealth[edit | edit source]
The integration of 2D slow motion video analysis with telehealth services is possible without prohibitive effort once a clinician has initiated use of this technology in the clinic.[1] Healthcare provided through telehealth can be an effective strategy for monitoring conditions and communicating with patients.[8][9]
- Capture a recording of the telehealth visit.
- Review the recording to conduct the movement analysis, using video editing apps or software as appropriate.
- At the second telehealth visit, share the analysis with the client using the 'share screen' function or using the edited slow-motion video files via a secure platform.
- Telehealth platforms typically require a signed Business Associate Agreement (BAA) to ensure the vendor is responsible for data breaches in order to be compliant with privacy regulations in the United States. See the resources below for a link to Telemedicine Platform Reviews. Use of a public-facing video communication platform without a BAA and without adequate privacy encryption mechanisms is typically not sufficient to meet confidentiality standards.[10]
There are instances where a therapist might ask a telehealth client to record their movement deviation, so that the therapist can review it later.[1] As Damien Howell notes, selfie videos can improve the quality of a telehealth consultation.[11]
"A barrier to typical telehealth visits is being able to adequately observe patients’ functional movements of walking, jumping, lifting, and moving. If the patient can share a selfie video of their symptomatic functional activities the quality of the telehealth visit can improve." -- Damien Howell[11]
Steps for the healthcare practitioner to utilise the patient’s selfie video:[11]
- Request the client to collect and share selfie real-world video data.
- Provide clients with directions on how to collect useful selfie video data. Investigate the use of a selfie stick tripod, 360 camera. Have a significant other capture video recording of movement.
- Provide a secure hyperlink for clients to upload selfie video data.
- Invest in video editing software and learn how to use functions of video editing software to analyze movements and digital storage of client data.
In his blog, Damien Howell offers the following tips to improve the quality and standardise the process of capturing selfie videos to facilitate the motion analysis process.[12]
- Lighting: When recording outside, avoid early morning and dusk. Arrange the light source from the sun, light from a window, indoor lights, or a selfie light ring behind the camera. When capturing a video recording outside, have a shady area available nearby to review the recording.
- Camera position - orientation: Consider on which type of computer screen the motion analysis will occur when choosing whether to orient the smartphone in portrait vs landscape. When playing back a video on a computer screen or TV monitor, the screen is wider than taller, so capturing video recording in the landscape is better. Using the “grid” option on the camera helps improve the orientation of the camera relative to the subject and the environment to improve the quality of the video recording. This option is found under the camera settings “more” function. It is best to hold the camera at the height of the centre of action. For most activities, the camera should be at the height of the “belt line”. A selfie stick with a tripod can hold the camera steady at the height of the belt line.
- Frames/second - slow-motion capture: Consider movement speed when choosing a camera mode of slow motion versus regular speed recording. For normal walking speed, capturing the video at the camera’s default setting of 24 to 30 frames/second provides acceptable quality. The camera's default frames/sec setting takes less storage space and less lighting. Recording at a camera setting of slow motion or higher frame rate takes more storage space and needs more illumination lighting.
- Staging: Choose clothing to be able to visualise key bony landmarks. Avoid wearing unicolour clothing or the “ninja effect”.[12]
For more information on recording selfie videos for telehealth, please see Damien Howell's blog posts:
- Using a selfie video for motion analysis
- How to improve the quality of a selfie video to facilitate motion analysis
Resources[edit | edit source]
- Damien Howell Physical Therapy Blog
- Hypothesis-Oriented Algorithm for Clinicians II (HOAC II)
- Shoulder Symptom Modification Procedure
- Telemedicine Platform Reviews
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 Damien Howell. Integrating 2D Video Analysis with Symptom Modification Procedure, Intervention and Telehealth. Plus Course. 2021.
- ↑ Rothstein JM, Echternach JL, Riddle DL. The hypothesis-oriented algorithm for Clinicians II (HOAC II): A guide for patient management. Physical Therapy. 2003;83(5):455–70.
- ↑ Zimmermann WO, Bakker EWP. Reducing vertical ground reaction forces: The relative importance of three gait retraining cues. Clinical Biomechanics. 2019;69:16–20.
- ↑ Futrell EE, Gross KD, Reisman D, Mullineaux DR, Davis IS. Transition to forefoot strike reduces load rates more effectively than altered cadence. Journal of Sport and Health Science. 2020;9(3):248–57.
- ↑ Lehman GJ. The role and value of symptom-modification approaches in Musculoskeletal practice. Journal of Orthopaedic & Sports Physical Therapy. 2018;48(6):430–5.
- ↑ 6.0 6.1 Ikeda DM, McGill SM. Can altering motions, postures, and loads provide immediate low back pain relief. Spine. 2012;37(23).
- ↑ Wartolowska K. The nocebo effect as a source of bias in the assessment of treatment effects. F1000Research. 2019;8:5.
- ↑ Omboni S, Ballatore T, Rizzi F, Tomassini F, Panzeri E, Campolo L. Telehealth at scale can improve chronic disease management in the community during a pandemic: An experience at the time of COVID-19. PLOS ONE 2021;16(9):e0258015.
- ↑ Mcelroy JA, Day TM, Becevic M. The Influence of Telehealth for Better Health Across Communities. Preventing Chronic Disease 2020;17.
- ↑ Assistant Secretary for Public Affairs (ASPA). Telehealth: Delivering care safely during covid-19 [Internet]. HHS.gov. 2021 [cited 2022Jan17]. Available from: https://www.hhs.gov/coronavirus/telehealth/index.html
- ↑ 11.0 11.1 11.2 Damien Howell Physical Therapy. Using a selfie video for motion analysis. Available from: https://damienhowellpt.com/using-a-selfie-video-for-motion-analysis/ (last accessed 1 November 2023).
- ↑ 12.0 12.1 Damien Howell Physical Therapy. How to improve the quality of a selfie video to facilitate motion analysis. Available from: https://damienhowellpt.com/how-to-improve-the-quality-of-a-selfie-video-to-facilitate-motion-analysis/ (last accessed 1 November 2023).