Factors Affecting Wound Healing
Top Contributors - Stacy Schiurring and Jess Bell
Introduction[edit | edit source]
Disclaimer: This page discusses the use of sharp debridement of the wound bed. This is an advanced treatment technique which requires specialised training to be properly and safely performed. Please be aware of your profession's practice act. Traditionally, sharp excisional debridement into healthy viable tissue can only be performed by a medical doctor with advanced training, while other health professionals in some areas can perform sharp debridement of nonviable tissue with advanced training.
There are many factors to take into consideration when practising wound care. Some of these factors are within the control of the rehabilitation professional, and some are not. By gaining an understanding of these key factors, the rehabilitation professional will be able to adjust the wound care treatment plan to obtain the best possible healing outcome. There are three types of factors which can affect wound healing: (1) intrinsic, (2) extrinsic, and (3) iatrogenic.[1]
Understanding the influence of these factors can help shape and inform a wound care assessment, treatment plan, and prognosis. For example, it is unrealistic to expect a wound to heal in the same manner in a young healthy person as in an older person with multiple comorbidities. Providing patients with realistic expectations of the healing process improves goal setting and builds trust between patients can care providers.[1]
Intrinsic Factors[edit | edit source]
Intrinsic factors are those related to the person that cannot be changed, but may be managed.[1]
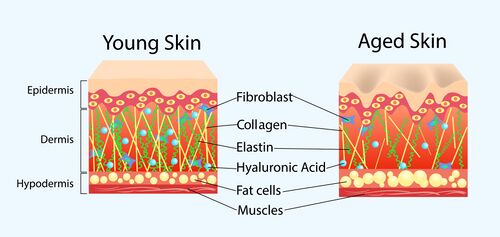
- Age. The epidermis becomes thinner with age and has a slower turnover. Collagen, elastin, and hyaluronic acid production also decreases as skin ages. This makes older skin more susceptible to tears and wounds. Human growth hormone plays a significant role in tissue healing and this decreases with age as well. Once older skin is wounded, it heals slower due to slower turnover of keratinocytes, reduced blood flow to the dermis, and a slowing of the complex healing cascade.[1]
- Genetics.
- In 2020, Tipton et al.[2] looked at the microbiomes of chronic wounds and found that people tend to be susceptible to infections by certain pathogens depending on their genotype. They also found that the variety of bacteria present is significantly related to wound healing. The more varied a wound microbiome, the faster that wound will close. While a person's microbiome is somewhat modifiable, much of the baseline is related to genotype and to the microbiome you are born with and seeded from during the birthing process.[1] [2]
- Skin elasticity and the ability to lay down collagen and fibrin is also genetically linked. This process can be seen in the body's ability to form scars, stretch marks, and wrinkles. Research in mice has found wound healing to be genetically controlled with a heritability rate of up to 86%. Other research in humans has found specific gene expression to be associated with the onset and progression of wound healing.[1][3]
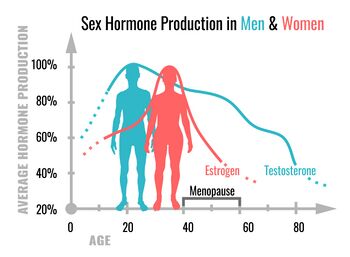
- Sex hormones. This is a complex topic. The research is mixed. Some research shows oestrogens speed healing and other research is in favour of androgens, depending on what phase the wound is in.[4] For most patients, this will not be of concern. However, it may need to be considered for patients taking synthetic hormones or going through an abrupt hormonal change, such as menopause.[1]
- Systemic diseases. Common medical conditions that may affect healing are (1) diabetes, (2) vascular diseases, (3) pulmonary diseases, (4) immunocompromised or autoimmune conditions, and (5) conditions that affect the autonomic nervous system. Both sympathetic and parasympathetic divisions play important roles in the wound healing phases.[1]
- Diabetes. Hyperglycaemia delays healing, therefore blood glucose levels need to be kept as close to the ideal range as possible. Ideally, blood glucose levels should be kept as close to the normal range as possible. However, even a reduction of blood glucose to 11.1 millimoles per litre, (200 milligrammes per decilitre) will have a beneficial effect on wound healing. Likewise, patients with an A1C of less than 7.1% have improved healing time. Providing this education to patients can help them to feel motivated in their progress toward more controlled blood glucose levels.[1]
- Venous insufficiency. A wound will not heal when persistent oedema is present. Oedema results in fibrinogen leaking out of capillaries into the dermis, which blocks oxygen and nutrients from being delivered to the tissues. This reduces blood flow and results in tissue hypoxia. Tissue hypoxia impairs tissue repair and increases susceptibility to infection by anaerobic microbes. It also inhibits fibroblast function and suppresses epithelial cells.[1]
- Arterial insufficiency. Blood flow to tissue needs to be optimised to facilitate wound closure. Insufficient perfusion reduces the delivery of the oxygen cells and nutrients necessary for healing.[1]
- Idiopathic pulmonary fibrosis. Pulmonary fibrosis reduces tissue oxygenation and negatively affects the tissue repair mechanisms via widespread epithelial injury.[1]
- Other chronic pulmonary diseases that affect tissue oxygenation can also impact healing.[1]
- Immunocompromised conditions. Such conditions prevent the necessary inflammatory response to initiate the healing cascade. This leads to an increased risk of infection, decreased phagocytosis, and decreased fibroblast activity.[1]
- Sensory and autonomic neuropathy. The neurotransmitters and neuropeptides produced by the cutaneous nerves are essential for all phases of repair. These substances are responsible for plasma extravasation, vasodilation, and neurogenic inflammation. Neuropathy limits the production of these substances.[1]
Extrinsic Factors[edit | edit source]
Extrinsic factors are things external to the wound that we can directly control.[1]
- Medications. It is important to perform a medication review and investigate any potential effects which could delay healing. Listed below is a non-exhaustive list of common medications which interfere with wound healing.[1]
- Steroids will delay all phases of wound healing. They can also contribute to elevated glucose levels with long-term use, recall how hyperglycaemia can delay healing as discussed above.[1]
- Anticoagulants inhibit the coagulation cascade and can result in tissue necrosis. This is especially common in fatty tissue.[1]
- Long-term non-steroidal anti-inflammatory drugs (NSAIDs) use delays wound healing by (1) suppressing the inflammatory response, (2) decreasing collagen synthesis, (3) reducing tensile strength and (4) increasing the risk of infection.[1]
- Chemotherapy drugs interfere with (1) cell proliferation, (2) prolong inflammation, (3) inhibit protein synthesis, and (4) decrease collagen synthesis. Chemotherapy-associated nausea and vomiting may also impair nutrition (see below for more details on nutrition).[1]
- Immunosuppressive or anti-rejection medications (1) impair fibroblast formation, (2) increase risk of infection and (3) decrease wound tensile strength. The gastrointestinal side effects of these medications can also impair nutrition (see below for more details on nutrition).[1]
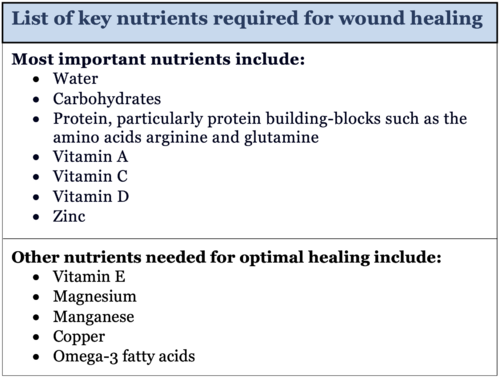
- Nutrition. The nutritional requirements for tissue healing are greater than the levels recommended for routine tissue maintenance or the recommended daily allowance (RDA).[5] [6][7] For example, additional water is needed to help with tissue repair depending on the size of the wound and the patient's overall health. It is estimated that a person's water requirements during wound healing are increased by approximately 20 to 30% above their normal requirements. Dietary adjustments will be made by dietitians or physicians while the patient is healing. Typically, the patient will be prescribed supplements at a dose that is above a nutrient's RDAs for two to 12 weeks while wound healing is initiated. This will then be reduced back to the RDA levels or the patient will be weaned off completely once healing is complete and a regular diet is established.[1]
- Stress and elevated cortisol levels. Stress results in (1) an increase in the incidence of opportunistic infection, (2) reduced expression of human growth hormone, and (3) delayed healing.[1]
- Gouin et al.[8] compared the healing rate of a small punch biopsy wound on a group of dental students. They found that the participants healed an average of three days slower when they were under the stress of exams as compared to when they were on vacation break. This represented a 40% longer healing time for a small standardised wound in a young and otherwise healthy population.[8]
- Older persons with multiple comorbidities are already at risk for delayed healing, and stress further compounds that risk.[1]
- People who are stressed are more likely to engage in other habits that can delay wound healing, such as the (1) use of alcohol, tobacco or drugs, (2) less physical activity, (3) less sleep, (4) poor nutrition, and a (5) lack of medication compliance.[1]
- Sleep deprivation. Lack of quality sleep can lead to (1) increased cortisol production, (2) elevated rates of illness and infection, (3) delayed skin barrier recovery, (4) reduced growth hormone production, and (5) impaired healing potential. It is important to recall that sleep disturbances can be a common side effect of many medications and underlying health conditions.[9] Therefore, a thorough patient interview and medication review are indicated. Ideally, adults should get 8-9 hours of sleep per night.[1]
- Smoking. Smoking leads to (1) hypoxia, (2) tissue ischaemia, (3) blood vessel inflammation, and (4) interferes with every phase of wound healing. Smoking a single cigarette has been shown to reduce tissue oxygen concentrations, whereas pack-per-day smokers experience tissue hypoxia for a significant portion of each day. It is possible to reverse the damage caused by smoking:
- After 12 hours without smoking, the blood oxygen levels return to near normal levels.
- After 24 hours without smoking, nerves begin to recover.
- Smoking cessation has been shown to restore the tissue microenvironment and cellular functions within four weeks. For heavy smokers who are unable to quit, decreasing the number of cigarettes smoked may cause improvement in tissue healing ability.
- Smokers have also been shown to have significantly lower levels of plasma vitamin C compared to non-smokers. Therefore, diets that are higher in vitamin C or including vitamin C supplementation should be considered to mitigate blood vessel damage and then further promote healing.[1]
Please watch the following optional short video for a concise summary of how smoking affects wound healing.[10]
- Alcohol. Drinking alcohol (1) delays wound closure, (2) increases the risk of infection, (3) reduces angiogenesis, (4) impairs collagen production, (5) interferes with epithelialisation, and (6) induces tissue hypoxia. Wound healing can be affected after just a few exposures to alcohol drinking above the legal limit.[1]
- Infection.
- Bacterial infection. All skin surfaces, including open wounds, are colonised with bacteria. Some bacteria are harmless and are part of the skin's biome. They are necessary for wound healing. Chronic wounds will have more bacterial colonisation than acute wounds and tend to have more pathogenic bacteria. This does not create a problem as long as the body can manage the level of bacterial colonisation. The amount of bacteria present in the wound is categorised on a spectrum. Local infection delays wound healing by (1) reducing collagen production, (2) decreasing nutrients available for healing and (3) killing cells vital for the healing process.[1]. Please see special topic box at the end of this section for a 2022 update of this information.
- Fungal infection. These infections are particularly problematic for patients who are immunocompromised. They can occur more often with compression therapy dressings, which stay in place for up to seven days. Wound drainage and sweat create a moist environment within compression dressings that is ideal for fungal growth. This is especially true in hot and humid environments. Fungal infections are best managed through (1) topical antifungals, (2) more frequent dressing changes and (3) adequate absorption via dressing selection to manage wound drainage.[1]
- Biofilm. This is a topic of new and emerging research and is not yet fully understood. Bacteria have evolved a variety of strategies to ensure their survival, one of these is the development of polysaccharide encapsulation that shields them from destruction by the host's immune defenses.
- Biofilm adheres to the wound bed and is difficult to remove, making the wound resistant to healing.
- Biofilm can be invisible to the naked eye (will make the wound surface appear shiny or slimy) or it can also resemble a thin layer of slough (yellow in colour) on the wound's surface.
- Mature biofilm can form in a matter of a few days - 90% of chronic wounds will have biofilms.
- Biofilm must be removed for wound healing. Regularly repeated sharp debridement is the preferred method to remove biofilm. Antimicrobial dressings are not an acceptable treatment method because they cannot penetrate the biofilm in order to kill the invading bacteria.[1]
Please watch this optional short video to learn more about the fascinating role the biofilm plays in delaying wound healing.[11]
- Obesity. Obesity is a known risk factor for multiple diseases. It also increases the risk of (1) wound infections, (2) haematomas, (3) surgical complications, (4) venous ulcers, and (5) pressure injuries.[1]
- These risks are likely due to (1) decreased tissue perfusion and ischaemia in adipose tissue, (2) increased tissue tension on wound edges, and (3) inadequate delivery of antibiotics.
- Adipocytes have been shown to secrete factors that interfere with normal inflammatory and immune responses.
- Other concerns which have the potential to affect wound healing in patients with obesity include increased risk of (1) pressure, (2) friction, (3) maceration, (4) limited mobility and or a sedentary lifestyle, and (5) oedema.[1]
Special Topic: The IWII Wound Infection Continuum (IWII-WIC) The IWII-WIC is an assessment tool which provides a framework for wound care professionals to understand the impact microorganisms have on (1) the host, (2) the wound and on (3) wound healing. The five stages in the IWII-WIC increase in severity as the microbial presence increases and begins to affect the host and wound functioning.[12]. The creation of the IWII-WIC included the elimination of the descriptive term critical colonisation for local infection.[13]
The IWII-WIC includes five conceptual stages:[12]
| Stages | Clinical Observations/Signs and Symptoms | Host Reactions | |
|---|---|---|---|
| 1
(least microbial burden) |
Contamination |
|
Host defences destroy microorganisms via phagocytosis |
| 2 | Colonisation |
|
|
| 3 | Local infection |
|
|
| 4 | Spreading infection
|
|
Spreading infection may involve deep tissue, muscle, fascia, organs or body cavities and result in more wide-spread signs and symptoms such as crepitus or lymphangitis |
| 5
(greatest microbial burden) |
Systemic infection |
|
|
Table adapted from the IWII-WIC 2022 update[12]
Iatrogenic Factors[edit | edit source]
Iatrogenic factors are related to how the wound is managed. The rehabilitation professional can have the biggest influence over this factor by modifying the treatment plan throughout the healing process after assessing the wound's response to interventions.[1]
- Dressing selection and management.[1]
- Compression is essential for venous wounds, and is indicated for oedema reduction in other wounds as well. Care must be taken to apply compression appropriately and monitor patient response regularly. Compression applied over an arterial wound or with an incorrect technique can reduce tissue perfusion and or create a tourniquet effect that damages both the wound and the peri-wound tissue.
- Dressing removal with poor technique can result in trauma to the healing wound tissues.
- Inappropriate dressing choices for a wound can cause tearing or maceration. Wounds require a moist environment for proper healing. Proper dressing selection is finding a balance between keeping the wound bed too moist or too dry. Proper dressing selection requires consideration of the drainage type and the amount and planned frequency of dressing changes. Repeated assessments must be performed to monitor the wound's response to the selected dressings.
- Too many dressing changes can also delay healing. When the wound bed is exposed to the outside environment during a dressing change, it can take up to 40 minutes for wound tissue to return to proper temperatures optional for healing. In addition, cellular mitosis is disrupted for up to three hours after a dressing change.
- Incorrect, unnecessary, or too frequent debridement. Excessive debridement is detrimental to healing because it causes a disruption of the wound bed. While maintenance debridement is often needed, attempts should be made to limit interruption to the healing process. This means when debridement is performed, care should be taken to remove as much necrotic tissue and biofilm as possible to allow for wound healing. This may require debridement by a medical doctor or surgeon who can debride deeper into viable tissue and a bleeding base.[1]
- Oedema management via positioning. Many chronic wounds are associated with oedema, particularly venous ulcers. Dependent positioning of an extremity will (1) increase oedema, (2) reduce the return of blood and lymphatic flow out of the extremity, and (3) increase pain.
- Leg elevation should be higher than the heart and combined with calf pump exercises. If the patient is unable to tolerate or achieve this position, attempt to elevate the distal leg to the level of the hip.
- The only wounds that should be kept dependent are wounds where tissue perfusion is compromised, such as arterial ulcers. In this case, gravity can help to improve blood flow to the wound.[1]
- Topical antiseptics and antibiotic ointments.
- Cytotoxic antiseptics have a wide spectrum of action on bacteria. However, they also cause eradication of beneficial bacteria and damage to the healing cells.
- Common examples used in wound care include (1) betadine (povidone-iodine), (2) Dakin's solution (sodium hypochlorite), (3) chlorhexidine, (4) hydrogen peroxide, (5) Burow's solution (aluminium acetate), and (6)silver nitrate.[1]
- Topical antibiotics have a more narrow spectrum of action and are less cytotoxic than antiseptics. They are typically less destructive to healing cells, but can still be detrimental when used inappropriately. Research in both human and animal models has demonstrated that broad-spectrum topical antibiotics slow skin healing.
- Common topical antibiotics used in wound care include (1) bacitracin, (2) mafenide acetate, (3) mupirocin, (4) neomycin, (5) Neosporin, (6) Polysporin, and (7) silver sulfadiazine.
- In addition to delayed wound healing, some of these products can be harmful to the kidney and liver and should be avoided in those with pre-existing kidney or liver impairment.
- When indicated, these products are effective if used correctly. However, they should be chosen with careful consideration and used for the shortest amount of time necessary to achieve the desired outcome and minimise detrimental effects.[1]
- Cytotoxic antiseptics have a wide spectrum of action on bacteria. However, they also cause eradication of beneficial bacteria and damage to the healing cells.
- Local trauma.[1]
- External pressure applied over tissues will collapse capillaries which results in reduced blood flow and tissue oxygenation.
- Friction and shear forces from footwear and dressings can cause tissue damage which can lead to wound formation and also impair current wound healing. This includes bumping, rubbing, scratching, excessive movement, or other disruption of the wound.
- These local traumas can occur through wound cleansing, dressing changes, loose compression dressings, footwear, or patient positioning.
Factors that can Optimise Wound Healing[edit | edit source]
Five key factors that can optimise wound healing are:[1]
- Address underlying disease processes. This can include: (1) blood pressure, (2) blood glucose levels, (3) tissue perfusion, (4) oedema management, (5) reinforce medication compliance, (6) offloading, and (7) pressure relief. The rehabilitation professional can provide education on how these factors can affect wound healing. When appropriate, reinforce treatment plans established by other healthcare providers and refer the patient to other members of the healthcare team as needed.
- Promote nutrition. The rehabilitation professional can (1) refer to a dietitian or nutritionist, (2) reinforce compliance with the prescribed diet, (3) emphasise the importance of hydration for tissue healing, (4) educate on the benefits of nutrition for healing.
- Exercise and physical activity. Physical activity (1) increases circulation and tissue perfusion, (2) reduces oedema, (3) improves overall health, and can (4) reduce the negative impact of systemic disease.[14]
- Peer support and mindfulness. We know that beliefs and attitudes can contribute to chronic health conditions and this includes chronic wounds. This may mean that the patient puts the onus on the healthcare provider to heal them rather than taking responsibility for the control that they have over their healing process. Alternatively, the patient may feel powerless or feel unsure about how to go about making the recommended changes. Therefore, patients who have been dealing with wounds for a long time and/or have seen multiple healthcare providers may feel hopeless.
- Peer support groups can be helpful in increasing patient adherence to a treatment programme.
- Examples include (1) walking or exercise groups, (2) nutrition groups, (3) support for health challenges and setbacks, (4) breath-work and breathing exercise groups.
- Mindfulness. Research has found that mindful stress-reduction techniques, relaxation, and guided imagery have been associated with improved wound healing.
- Examples include (1) positive self-talk about the healing ability of the body, (2) fostering belief in the potential for healing, (3) mindfulness exercises that address tissue oxygenation, nutrition, tissue repair, body resiliency, or (4) turning the focus inward to body repair rather than outward to life stresses. Guided imagery can also be used to talk the patient through (1) the phases of tissue healing, (2) breathwork, (3) directing healing breath and healing cells towards the wound, or (4) positive affirmations. These exercises can be in spoken, written, or audio form. Many patients utilise a combination of these methods.
- Peer support groups can be helpful in increasing patient adherence to a treatment programme.
- Education. Patient education specific to the patient's wound and the underlying condition is key yet this is often overlooked as part of the plan of care. Patient understanding of the plan of care and specific recommendations can greatly improve adherence to a treatment plan and improve compliance of interventions that promote healing.
- Patient education should be an interdisciplinary effort and be provided at all levels of the care team.
- It helps with intrinsic versus extrinsic locus-of-control; the patient knows what factors are changeable, what factors can be modified, and what factors are completely within their control.
- Education assists the patient in goal setting and prioritising.
- Patient education can be provided as needed. Rehabilitation professionals are ideal for this role as they often spend more time with the patient and can provide education in smaller and better-retained amounts.
Resources[edit | edit source]
Optional Additional Reading:
- Intrinsic Factors:
- Demling RH. The role of anabolic hormones for wound healing in catabolic states. J Burns Wounds. 2005 Jan 17;4:e2.
- Engeland CG, Sabzehei B, Marucha PT. Sex hormones and mucosal wound healing. Brain, behaviour, and immunity. 2009 Jul 1;23(5):629-35.
- Tipton CD, Wolcott RD, Sanford NE, Miller C, Pathak G, Silzer TK, Sun J, Fleming D, Rumbaugh KP, Little TD, Phillips N. Patient genetics is linked to chronic wound microbiome composition and healing. PLoS pathogens. 2020 Jun 18;16(6):e1008511.
- Zhu HJ, Fan M, Gao M. Identification of potential hub genes associated with skin wound healing based on time course bioinformatic analyses. BMC Surg. 2021;21:303.
- Extrinsic Factors:
- Aberg KM, Radek KA, Choi EH, Kim DK, Demerjian M, Hupe M, Kerbleski J, Gallo RL, Ganz T, Mauro T, Feingold KR, Elias PM. Psychological stress downregulates epidermal antimicrobial peptide expression and increases severity of cutaneous infections in mice. J Clin Invest. 2007Nov;117(11): 3339-49.
- Attinger C, Wolcott R. Clinically addressing biofilm in chronic wounds. Adv Wound Care. 2012 Jun;1(3):127-132.
- Besedovsky L, Lange T, Born J. Sleep and immune function. Pflugers Arch. 2012 Jan;463(1):121-37.
- Clinton A, Carter T. Chronic wound biofilms: Pathogenesis and potential therapies. Laboratory Medicine. 2015;46(4):277-284.
- Garbarino S, Lanteri P, Bragazzi NL, Magnavita N, Scoditti E. Role of sleep deprivation in immune-related disease risk and outcomes. Communications biology. 2021 Nov 18;4(1):1-7.
- Gouin JP, Kiecolt-Glaser JK. The impact of psychological stress on wound healing: methods and mechanisms. Immunology and Allergy Clinics. 2011 Feb 1;31(1):81-93.
- Heitzer T, Just H, Mu¨nzel, T. Antioxidant vitamin C improves endothelial dysfunction in chronic smokers. Circulation. 1996;94:6-9.
- Jung MK, Callaci JJ, Lauing KL, Otis JS, Radek KA, Jones MK, Kovacs EJ. Alcohol exposure and mechanisms of tissue injury and repair. Alcohol Clin Exp Res. 2011 Mar;35(3):392-9.
- McDaniel JC, Belury M, Ahijevych K, et al. Omega-3 fatty acids effect on wound healing. Wound Repair Regen. 2008;16(3):337–45.
- Meesters A, den Bosch-Meevissen YMCI, Weijzen CAH, Buurman WA, Losen M, Schepers J, Thissen MRTM, Alberts HJEM, Schalkwijk CG, Peters ML. The effect of Mindfulness-Based Stress Reduction on wound healing: A preliminary study. J Behav Med. 2018 Jun;41(3):385-397.
- Szabo G, Mandrekar P. A recent perspective on alcohol, immunity, and host defense. Alcohol Clin Exp Res. 2009 Feb;33(2):220-32.
- Thorpe J. The importance of water: In modern wound care. Wounds UK. 2010;5:115-118.
- Iatrogenic Factors:
- Keylock KT, Vieira VJ, Wallig MA, et al. Exercise accelerates cutaneous wound healing and decreases wound inflammation in aged mice. Am J Physiol Regul Integr Comp Physiol. 2008;294(1):R179–84
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 1.20 1.21 1.22 1.23 1.24 1.25 1.26 1.27 1.28 1.29 1.30 1.31 1.32 1.33 1.34 1.35 1.36 1.37 1.38 1.39 1.40 1.41 Palmer, D. Physiotherapy Wound Care Programme. Factors Affecting Wound Healing. Plus. 2022.
- ↑ 2.0 2.1 Tipton CD, Wolcott RD, Sanford NE, Miller C, Pathak G, Silzer TK, Sun J, Fleming D, Rumbaugh KP, Little TD, Phillips N. Patient genetics is linked to chronic wound microbiome composition and healing. PLoS pathogens. 2020 Jun 18;16(6):e1008511.
- ↑ Zhu HJ, Fan M, Gao W. Identification of potential hub genes associated with skin wound healing based on time course bioinformatic analyses. BMC surgery. 2021 Dec;21(1):1-3.
- ↑ Engeland CG, Sabzehei B, Marucha PT. Sex hormones and mucosal wound healing. Brain, behaviour, and immunity. 2009 Jul 1;23(5):629-35.
- ↑ Polcz ME, Barbul A. The role of vitamin A in wound healing. Nutrition in Clinical Practice. 2019 Oct;34(5):695-700.
- ↑ T. H. Chan School of Public Health, Harvard University. The nutrition source: Vitamin D. Published May 2020. Accessed October 25, 2021.
- ↑ McDaniel JC, Belury M, Ahijevych K, et al. Omega-3 fatty acids effect on wound healing. Wound Repair Regen. 2008;16(3):337–45.
- ↑ 8.0 8.1 Gouin JP, Kiecolt-Glaser JK. The impact of psychological stress on wound healing: methods and mechanisms. Immunology and Allergy Clinics. 2011 Feb 1;31(1):81-93.
- ↑ Garbarino S, Lanteri P, Bragazzi NL, Magnavita N, Scoditti E. Role of sleep deprivation in immune-related disease risk and outcomes. Communications biology. 2021 Nov 18;4(1):1-7.
- ↑ JYouTube. Why Smoking Makes It Harder to Heal | SciShow. Available from: https://www.youtube.com/watch?v=qQUy15nNbFQ [last accessed 04/10/2022]
- ↑ YouTube. Biofilm is an enemy worth targeting | Rechtsdepesche International. Available from: https://www.youtube.com/watch?v=H8KeFIsTFi8 [last accessed 04/10/2022]
- ↑ 12.0 12.1 12.2 Wounds International. Wound Infection In Clinical Practice: Principles of best practice. Available from: https://www.woundsinternational.com/resources/details/wound-infection-in-clinical-practice-principles-of-best-practice (accessed 26/11/2022).
- ↑ Haesler E, et al. Clinical indicators of wound infection and biofilm: reaching international consensus. J Wound Care, 2019; 28 (Sup 3b).
- ↑ Keylock KT, Vieira VJ, Wallig MA, et al. Exercise accelerates cutaneous wound healing and decreases wound inflammation in aged mice. Am J Physiol Regul Integr Comp Physiol. 2008;294(1):R179–84