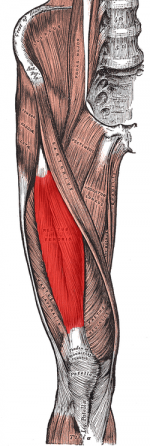
Ely's Test
Original Editor - Sam Verhelpen
Top Contributors - Sheik Abdul Khadir, Admin, Sam Verhelpen, Naomi O'Reilly, Kim Jackson, Laura Ritchie, Evan Thomas, Venus Pagare, WikiSysop, Wanda van Niekerk, 127.0.0.1, Tony Lowe, Daphne Jackson and Kai A. Sigel
Purpose[edit | edit source]
Ely’s test or Duncan-Ely test is used to assess rectus femoris spasticity or tightness.[1]
Technique[edit | edit source]
The patient lies prone in a relaxed state. The therapist is standing next to the patient, at the side of the leg that will be tested. One hand should be on the lower back, the other holding the leg at the heel. Passively flex the knee in a rapid fashion. The heel should touch the buttocks. Test both sides for comparison. The test is positive when the heel cannot touch the buttocks, the hip of the tested side rises up from the table, the patient feels pain or tingling in the back or legs.
Evidence[edit | edit source]
Studies show Ely’s test has a sensitivity ranging from 56% to 59% and the specificity ranging from 64% to 85%.[1]
Critical Review[edit | edit source]
Though the Duncan-Ely test is commonly performed clinically, the importance of a positive Duncan-Ely test for rectus femoris spasticity is uncertain. Perry et al[2] showed that the Duncan-Ely test is not a specific indicator of rectus tightness or spasticity since it elicits electromyographic (EMG) responses in both the rectus femoris and the iliacus in many subjects with CP. Chambers et al[3] reported that the Ely test has no predictive value for abnormal rectus femoris EMG activity.
References[edit | edit source]
- ↑ 1.0 1.1 Marks M C, Alexander J, Sutherland D H, Chambers H G. (2003) Clinical utility of the Duncan-Ely test for rectus femoris dysfunction during the swing phase of gait. Developmental Medicine & Child Neurology 2003, 45: 763–768
- ↑ Perry J, Hoffer MM, Antonelli D, et al. Electromyography before and after surgery for hip deformity in children with cerebral palsy. A comparison of clinical and electromyographic findings. J Bone Joint Surg [Am]. 1976;58:201–208.
- ↑ Chambers H, Lauer A, Kaufman K, et al. Prediction of outcome after rectus femoris surgery in cerebral palsy: the role of cocontraction of thefckLRrectus femoris and vastus lateralis. J Pediatr Orthop. 1998;18:703–711.