Chikungunya Fever
Original Editor - - Vanessa Rhule
Top Contributors - Vanessa Rhule, Lucinda hampton, Evan Thomas, Rishika Babburu, WikiSysop and Kim Jackson
Introduction[edit | edit source]
Chikungunya (CHIK-V) Fever:
- An arthropod-borne alphavirus that belongs to the family Togaviridae transmitted by Aedes mosquitoes.
- The virus is known for causing an acute febrile illness, rash, and arthralgia known as Chikungunya fever followed by potentially chronic and debilitating arthritic symptoms that may last for months or years.
- Historically, CHIKV was found mainly in Africa and Asia, initially isolated in the Makonde Plateau in Tanzania in 1952. The name Chikungunya is derived from a Makonde phrase meaning, "that which bends up."
- The worst outbreak reported occurred in the Reunion Island in 2005-2006 affecting nearly 35% of the population.
- Since 2005, cases of Chikungunya fever have spread mainly in tropical and sub-tropical regions finally reaching the Americas via the Caribbean island of St. Martin in 2013.
- Today, CHIKV is widespread worldwide and is a global public health concern[1].
Prevelance[edit | edit source]
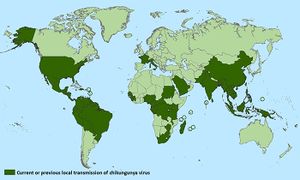
Chikungunya virus has been on the rise since 2013 affecting more than 100 countries and territories. As of October 2015, the picture below shows the distribution of chikunguyna virus transmission throughout the world.
In the United States prior to 2006, chikungunya virus was seldom identified in travelers coming to and from the United States. It was mainly identified from Asia, Africa, or the Indian Ocean. In late 2013, the first local transmission was identified in Caribbean countries and territories. In 2014, chikungunya virus was reported in Florida, Puerto Rico, and U.S. Virgin Islands. As of January 12, 2016 there was a total of 679 chikungunya virus cases with onset in 2015 reported to ArboNET from U.S. states or territories. Wyoming, South Dakota, New Mexico, Louisiana, and West Virginia are the only states that have not reported travel associated cases of the chikungunya virus.[2]
Global Issues[edit | edit source]
The global expansion of the virus demonstrates the effortlessness with which the virus can spread and infect the human population. This will in effect directly reduce productivity and place a burden on the economy on a global level given the long period of illness.
Preventative Measures
- Vector control through spraying and fogging of chemical insecticides as well as removal of breeding sites on a community level will reduce the rate of infection and transmission
- Large mass media coverage, campaigns and educational literature have been put in place with aims to increase awareness on the disease and promote the physical elimination of mosquito breeding sites
Aetiology[edit | edit source]
- The Aedes Aegypti and Aedes Albopictus mosquitos are the main vectors of the virus.
- The human being becomes the reservoir of infection and transmitted from human to human via the infected mosquito.
- These mosquitos bite mainly in the daytime and are also known to transmit the dengue virus [3]
Risk Factors [edit | edit source]
- There has been increased prevalence in densely populated, urbanized areas, since humans are the only reservoir of the virus.
- Poor living conditions and maintenance of peridomestic environment including pooling of water in water recipients or tyres and inappropriate waste disposal.These are all sources of Aedes mosquito species.[4]
- Migration and Travelling; the Center for Disease Control estimated approximately 9 million people travel between the United States and the Caribbean each year, increasing the risk of transmission [3]
Clinical Features [edit | edit source]
- The incubation period for Chikunguyna fever is noted to be between 3-7 days starting with fevers greater than 38.9°C which can last up to 2 weeks and are biphasic in nature
- Following the fever, majority of infected people develop severe polyarthralgias which are usually symmetric
- Pains are most commonly in the wrists, elbows, fingers, knees and ankles but are not limited to these.
- Pain and Joint swelling are often incapacitating and result in severe disabilities which can last for months.
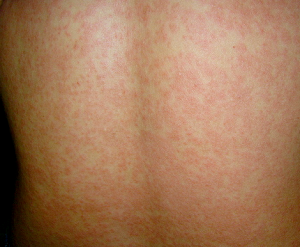
- The development of a maculopapular rash is often associated See image.
- Additionally, the individual may experience cervical lymphadenopathy, headaches, fatigue, nausea, vomiting, conjunctivitis and myalgia.[5]
- In the acute stage of infection, blood tests may reveal abnormalities such as leukopenia, thrombocytopenia, hypocalcemia and moderate increase in liver function test results
- Asymptomatic cases have also been reported[6]
Musculoskeletal Implications [edit | edit source]
- In the chronic phase of the infection, individuals may experience musculoskeletal symptoms for several weeks to months
- Joint manifestations such as joint effusions, hygromas, bursitis and axial pain can be identified in areas with previously occurring injuries
- Carpal Tunnel syndrome and Raynaud phenomenon in chronic phase have been noted [7]
- Carpal or Cubital Tunnel syndromes are often a result of hypertrophic tenosynovitis of the anterior wrist [7]
Other Complications[8][edit | edit source]
- Cardiac complications were also reported in a number persons infected with the chikunguyna virus resulting in cases of myocarditis and cardiomyopathy. In many cases, these conditions have been noted to resolve spontaneously
- Chikungunya fever is rarely fatal however there are cases of death has been reported resulting from severe complications or by a weakened immune system
Diagnosis[edit | edit source]
- Chikungunya virus infection should be considered in patients with acute onset of fever and polyarthralgia
- Testing of the serum or plasma detects the virus, viral nucleic acid or virus-specific immunoglobulin and neutralizing antibodies[3]
Treatment [edit | edit source]
There is no specific antiviral therapy for CHIK-V however treatment is usually centered on symptom reduction.
Includes:
- Non-steroidal Anti-Inflammatory drugs (NSAIDs) to relieve pain and fever
- Rest
- Increased fluid in-take
- Paracetamol
Persistent joint pains may benefit from NSAIDs, Corticosteroids and Physical therapy.However, Aspirin should be avoided because of the increased risk of bleeding[3]
- Snake venom proteins have been shown to exhibit antiviral action against a variety of viruses, including arboviruses, which are of public health concern. Phospholipase A2CB (PLA2CB), a protein isolated from Crotalus durissus terrificus venom, has previously been demonstrated to have anti-inflammatory, antiparasitic, antibacterial, and antiviral properties. Snake venom proteins have been shown to exhibit antiviral action against a variety of viruses, including arboviruses, which are of public health concern. .Using Chickungunya Virus(CHIKV)-nanoluc, a marker virus containing a nanoluciferase reporter, a study was conducted on the numerous impacts of PLA2CB on the CHIKV replicative cycle in BHK-21 cells. PLA2CB has a substantial anti-CHIKV activity, according to the findings, with a selectivity index of 128.
- PLA2CB therapy effectively protected cells from CHIKV infection by lowering the adsorption and post-attachment stages of virus entry. Furthermore, PLA2CB showed a small but considerable activity in the CHIKV replicative cycle's post-entry stages. PLA2CB may interact with CHIKV glycoproteins, primarily E1, via hydrophobic contacts, according to molecular docking calculations. Infrared spectroscopy tests also revealed PLA2CB and CHIKV glycoprotein interactions, correlating with evidence from in silico analysis.[9]
Physical Therapy management[edit | edit source]
The main role of the physiotherapist is to provide supportive care.
- Disability level is assessed using a standard disability index and plan of care is based on the patient's presentation.
- Joint pain from CHIKV is said to respond to mild exercise. Stretches, passive and active exercises will also assist in the prevention or reduction of contractures and deformities
Prognosis[edit | edit source]
Despite a low case fatality ratio (CFR), Chikungunya fever is highlighted by a substantial post-chikungunya chronic polyarthralgia, defined as joint pains lasting longer than 6 weeks.
- A study published in 2018, composed of Aruba CHIKV cases, reported that 26% of all serology-confirmed infected patients presented with post-chikungunya polyarthritis.
- Another study published in 2018, from 2014 French Guiana, reported post-CHIKV rheumatic or musculoskeletal pain at 3 and 6 months of 40% and 31.3% respectively of all RT-PCR proven cases[1].
Differential Diagnosis[edit | edit source]
Chikungunya virus can present similarly to other illnesses because of its signs and symptoms of fever, joint pain, headache, rash, and nausea/vomiting.
- Dengue- Dengue is also a mosquito contracted illness when symptoms arise quickly (4-7 days) just like chikungunya virus. Dengue and chikungunya virus are often misdiagnosed. These two illness have similar sign and symptoms but typically dengue fever will present with enlarged lymph nodes, severe eye pain, mild bleeding of the nose and gums, and easily bruising which chikungunya does not. Also chikungunya virus the pain is more intense and specific in the joints than dengue.
- Zika Virus
- West Nile Virus- West Nile Virus is another mosquito transmitted disease just like chikungunya virus. Most people infected will not show any symptoms however the 20-30% who do will have a similar presentation. This includes headache, body ache, joint pain, vomiting, diarrhea, or rash. Additional laboratory testing can be completed to detect the WNV-specific IgM antibodies.
- Alphavirus infections (Mayaro Fever, Ross River, Barmah Forest, and Sindbis viruses)- These infections all have distinguishing symptoms of joint pain along with a rash. Also, these viruses and transmitted through mosquitoes. It is very important to look at all the signs and symptoms as well as duration.
- Malaria
- Group A Streptococcus- Group A Streptococcus is spread through contact of infected droplets from a person's cough or sneeze. This group includes necrotizing fasciitis, strep throat, and scarlet fever. Each of these have some similar symptoms to chikungunya virus but some are specific to each illness and the transmission is also different.
- Rubella- Rubella can be similar to chikungunya virus in the symptoms of rash and fever. Rubella symptoms only typically last 2-3 days where chikungunya virus is just a few days longer. Also the transmission of the diseases are different.
- Measles- One way to prevent getting measles is to get vaccinated especially if traveling around the world as it still common in many countries. Some symptoms that do not align with chikungunya is runny nose, watery eyes, and a cough.
- Enteroviruses- The group of enteroviruses can include the diseases epidemic pleurodynia, hand-foot-and mouth disease, herpangina, poliomyelitis, aseptic meningitis, and myopericarditis.
- Septic Arthritis
- Rheumatologic conditions- There are more than 100 different rheumatologic conditions each which are unique in their own presentation. Some common conditions include: osteoarthritis, rheumatoid arthritis, lupus, ankylosing spondylitis, and sjogren’s syndrome. It is common to have joint pain, joint swelling, and possibly a fever with these conditions just like chikungunya virus.
- Leptospirosis
References[edit | edit source]
- ↑ 1.0 1.1 Staples JE, Breiman RF, Powers AM. Chikungunya fever: an epidemiological review of a re-emerging infectious disease. Clinical infectious diseases. 2009 Sep 15;49(6):942-8.Available from:https://www.statpearls.com/articlelibrary/viewarticle/81/
- ↑ Centers for Disease Control and Prevention. Chikungunya Virus [Internet]. Atlanta, Georgia: Centers for Disease Control and Prevention. 2015 Aug 3 [updated 2015 Nov 15; cited 2016 April 1]. Available from: http://www.cdc.gov/chikungunya/
- ↑ 3.0 3.1 3.2 3.3 Cdc.gov. Chikungunya outbreak progresses in Caribbean, Central and South America| CDC Online Newsroom | CDC [Internet]. 2015 [cited 20 June 2015]. Available from: http://www.cdc.gov/media/releases/2014/p1106-chikungunya-outbreak.html
- ↑ Sissoko D, Moendandze A, Malvy D, Giry C, Ezzedine K, Solet J et al. Seroprevalence and Risk Factors of Chikungunya Virus Infection in Mayotte, Indian Ocean, 2005-2006: A Population-Based Survey. PLoS ONE. 2008;3(8):e3066.
- ↑ Rhule V. Chikungunya. Presentation presented at; 2015; Utica, New York and Kingston,Jamaica.
- ↑ Staples J, Breiman R, Powers A. Chikungunya Fever: An Epidemiological Review of a Re‐Emerging Infectious Disease. Clinical Infectious Diseases. 2009;49(6):942-948.
- ↑ 7.0 7.1 Parola P, Simon F, Oliver M. Tenosynovitis and Vascular Disorders Associated with Chikungunya Virus-Related Rheumatism. Clinical Infectious Diseases. 2007;45(6):801-802.
- ↑ Obeyesekere I, Hermon Y. Myocarditis and cardiomyopathy after arbovirus infections (dengue and chikungunya fever). Heart. 1972;34(8):821-827.
- ↑ https://www.nature.com/articles/s41598-021-88039-4