Characteristics and Identification of Wound Types: Pressure Injuries and Non-healing Surgical Wounds
Top Contributors - Stacy Schiurring, Jess Bell and Kim Jackson
Introduction[edit | edit source]
This article provides information for rehabilitation professionals who are new to wound care or have been away from the practice and need a review of wound type identification. This article will not go into specifics on wound assessment or treatment.
The five most common types of chronic wounds include (1) arterial ulcers, (2) venous insufficiency ulcers or venous wounds, (3) neuropathic wounds, or diabetic foot ulcers, (4) pressure injuries, formerly known as pressure ulcers, and (5) non-healing surgical wounds.
The terms ulcer and wound will be used interchangeably throughout this article.[1]
Due to the large amount of information to be presented, this topic has been divided into three separate pages. This page will cover pressure injuries and non-healing surgical wounds. To learn more about arterial wounds and venous insufficiency ulcers, please see this article. To learn more about neuropathic wounds, please see this article.
Pressure Injuries[edit | edit source]
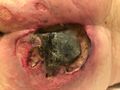
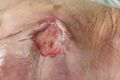
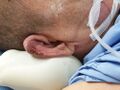
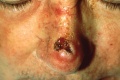
Pressure injuries (formally known as pressure ulcers, decubitus ulcers, or bedsores) develop in localised areas when soft tissues are compressed between a bony prominence and an external surface for a prolonged amount of time.[1][2] When the tissue is compressed, blood flow to the area stops or is decreased below a level that is necessary to sustain cell function. This lack of oxygen and nutrients results in cell death.[1] Deep tissue pressure injuries are areas of underlying soft tissue necrosis which present with persistent non-blanchable deep red or purple areas of intact or non-intact skin, or blood-filled blisters. Deep tissue pressure injuries are a serious form of pressure injury because they start in the underlying tissues and are not visible at the skin's surface until the wound is already quite advanced.[2]
- The term injury is more accurate term than ulcer because this condition does not always present as an open wound; damage can start in the deeper soft tissue layers.
- The term injury also helps focus on wound prevention rather than reactive treatment. Prevention is key to successful management for these wounds.[1]
Time to tissue breakdown[edit | edit source]
The amount of time required for cell death and tissue destruction is variable. It is dependent upon (1) tissue integrity, the (2) amount of pressure, and the (3) duration of pressure. For example, persons who are thin, have multiple comorbidities, and are bed bound may see effects sooner than persons of a different build, health status, and mobility level.[1]
General guidelines for tissue breakdown and recovery:[1] every individual is unique and requires a personalised care plan.
- Blanchable erythema occurs after approximately 30 minutes of unrelieved pressure. It requires one hour for tissue recovery once pressure is relieved.
- Tissue ischaemia occurs within two to six hours of unrelieved pressure and is seen as a deeper redness. It requires 36 hours for tissue recovery once pressure is relieved.
- Tissue necrosis occurs after six or more hours of unrelieved pressure. Once necrosis has occurred, recovery may not be possible.
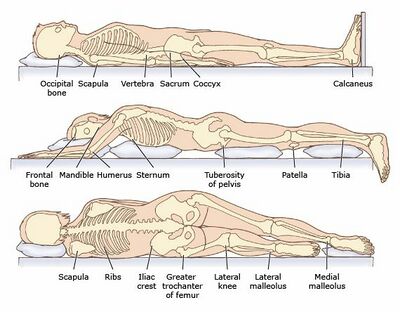
The most common sites of pressure injuries include the (1) sacrum, (2) ischial tuberosities, (3) greater trochanters, and (4) heels. But keep in mind that pressure injuries can occur on any part of the body where there is unrelieved pressure.[1]
Risk factors for pressure injuries[3][edit | edit source]
- Immobility. Soft tissues have a limited tolerance of pressure over time before damage will occur. That may be a low pressure over a long period of time or a high pressure over a short period of time. When sensory systems are intact, the need to reposition for pressure relief is automatic. However, if there is a lack of mobility or a loss of sensation, a patient may not receive sensory feedback for a position change or may be unable to change position independently.[1]
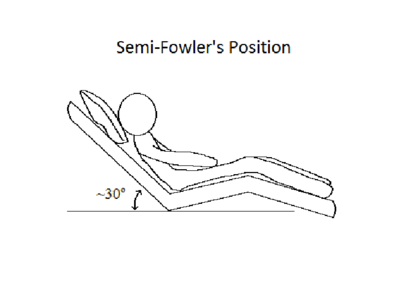
- Shear. Shear is a mechanical force that has internal effects on the skin in a direction parallel to the body’s surface. Shearing forces occur between internal body structures and the skin. Typically the shearing force and the body move in opposite directions. These forces influence deeper tissues via a “bottom-up” mechanism of tissue injury.[4] Shear forces distort both superficial and deep tissues which can result in damage to the capillaries, reducing blood flow and oxygenation to the tissues. The most common position that increases shear force is the semi-fowler's position.[1]
- Friction. Friction is a mechanical force exerted over the skin when it is dragged across a surface. Damage created by friction alone typically results in superficial abrasions with a vulnerability to pressure injuries.[1][4] Friction forces have the greatest effect on the superficial layers of skin from a “top-down” mechanism of tissue injury.[4] This can also wear away the epidermis which results in a reduced tolerance to the shear forces that occur deeper within the tissue.[1]
- Moisture or excess fluid on the skin. Moisture sources can include (1) exudate, (2) sweat, or (3) incontinence. Excessive moisture trapped against the skin causes maceration (prolonged exposure of intact skin to moisture, skin appear soggy, feels soft, and or appears more white than usual) and reduces the skin's tolerance to shear and friction forces.[1]
- Malnutrition. This can reduce healing in current wounds and increase the risk of further tissue breakdown. Individuals with a body mass index (BMI) of less than 18.5 or who are of cachectic build are at higher risk for pressure injury formation because they have more pronounced bony prominences and the tissues are subjected to higher pressures from external sources.[1]
- Age. Older persons are at greater risk due to (1) decreased healing capacity, (2) reduced skin integrity, (3) increased likelihood of mobility issues, and increased likelihood of (4) multiple comorbidities. 70% of pressure injuries occur in those that are over the age of 70.[1]
- Significant or severe systemic disease or multiple comorbidities. Diagnoses which increase the likelihood of pressure injury development include (1) diabetes, (2) previous or other current pressure injuries, patients who experience (3) longer ICU admissions, (4) hypotension.[1]
Scales for pressure injury prediction:
These scales look at different risk factors for pressure ulcers, and then attempt to predict the risk. Studies have not clearly shown one to be more valid than others, and have found that they are relatively weak predictors of pressure injury formation. However they can be used to highlight risk factors, and when combined with clinical judgment, can aide in determining appropriate prevention measures.[1]
Pressure injury management[edit | edit source]
The three most important factors in pressure injury management:
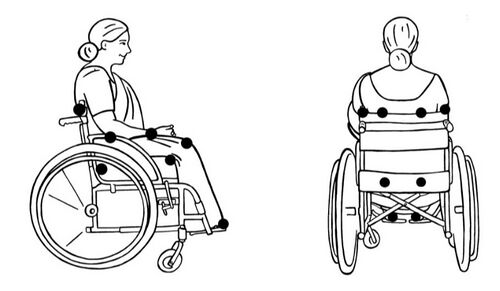
- Offloading. Healing of pressure injuries and wounds cannot begin until the source of pressure is eliminated. These wounds need to be completely offloaded in order to heal. Sufficient offloading requires a thorough assessment of (1) the wound, the (2) patient's mobility, and any (3) other factors that may affect that offloading plan. Strategies should be implemented on all surfaces that the patient uses throughout the day: bed, wheelchair, bedside chair, couch, recliner, et cetera. Offloading may be accomplished through (1) surface overlays, (2) cushions, (3) positioning, or (4) mobilisation, and often require a combination of all the above.
- Adequate hydration and nutrition. Proper nutrition is essential for both healing damaged tissue and maintaining the health of undamaged tissue. Malnutrition leads to low protein and vitamin stores, which is going to impact wound healing. It also leads to weight loss, and then that exacerbates the bony prominences and further increases the risk of pressure injury. Protein or amino acids supplements may be beneficial to promote healing in those who are malnourished. These patients should receive a thorough nutritional assessment by a dietitian and a customised nutrition plan.[1][5]
- Prevention. Pressure injury prevention is key to avoiding complications, improving quality of life, and reducing treatment cost. It is estimated that the cost of pressure injury prevention is two to three times less than the cost to treat them. A prevention plan is going to look different for every patient, depending their (1) health status, (2) skin assessment, (3) mobility ability, and (4) education.[1]
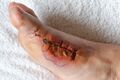
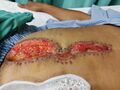
Non-Healing Surgical Wounds[edit | edit source]
Non-healing surgical wounds occur when a surgical incision does not heal as expected.[1]
- The prevalence of this wound type varies by (1) surgery type, (2) surgical location on the body, (3) local surgical practices, (4) general population health, and the (5) rehabilitation professional's practice setting.[1]
Factors that will increase the risk of a surgical wound not healing[edit | edit source]
- Infection. This is typically seen within 30 days post-surgery or within 90 days of a prosthetic device implantation
- Weakened immune system
- Steroid use
- Multiple comorbidities. Often seen with diabetes
- Smoking. Abstinence from smoking for as little as four weeks will significantly improve incisional healing
- Poor nutrition and hydration
- Older age
- Being overweight or obese
- Surgical special considerations. Surgeries lasting over two hours, emergency surgeries, abdominal surgery, or inadequate perfusion to the wound site for whatever reason
Signs of a non-healing surgical wound[edit | edit source]
- Fever
- Excessive drainage from the wound, especially purulent drainage (pus)
- Increased temperature at the wound site
- Foul odour
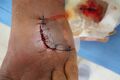
- Dehiscence (opening of the wound edges at the surgical incision). This most often occurs early in the healing process, three to 10 days post-surgery. Dehiscence is more c ommonly seen in abdominal, pelvic, or vascular surgeries. It is more commonly seen in those patients with increased age and or higher BMI.[6][7]
Management of non-healing surgical wounds[edit | edit source]
The three most important factors for management of non-healing surgical wounds:
- Compliance with post-operative orders. This includes: dressing changes, weight bearing, tension on the skin or sutures, or possibly lifting restrictions. Collaboration with the surgeon is recommended.
- Nutrition. The body requires more protein, vitamins, and minerals than usual when attempting to heal tissue. Limit sugary, processed, and inflammatory foods. Increase water, plants, and protein and then:
- General protein requirements are 1.2 to 2 grams of protein per kilogram of body weight
- General water requirements are 30 to 40 millilitres per kilogram of body weight per day
- Education. This can include (1) home management, (2) any restrictions or activity limitation, (3) activity of daily living training, (4) wound care procedures and dressing application, and (5) infection prevention.
Resources[edit | edit source]
Clinical resources:
- Waterlow Scale PDF
- The National Pressure Injury Advisory Panel: pressure injury prevention guideline
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 Palmer, D. Characteristics and Identification of Wound Types. Physiotherapy Wound Care Programme. Plus. 2022.
- ↑ 2.0 2.1 Wound Source. Pressure Injuries, Deep Tissue Pressure Injury (DTPI). Available from: https://www.woundsource.com/patientcondition/pressure-injuries-deep-tissue-pressure-injury-dtpi (accessed 21/09/2022).
- ↑ Chung M-L, Widdel M, Kirchhoff J, Sellin J, Jelali M, Geiser F, Mucke M, Conrad R. Risk factors of pressure injuries in adult patients: A narrative synthesis. Int J Environ Res Public Health. 2022;19(2):761.
- ↑ 4.0 4.1 4.2 Broderick VV, Cowan LJ. Pressure Injury Related to Friction and Shearing Forces in Older Adults. Journal of Dermatology and Skin Science. 2021 Jul 12;3(2).
- ↑ Munoz N, Posthauer ME. Nutrition strategies for pressure injury management: Implementing the 2019 International Clinical Practice Guideline. Nutrition in Clinical Practice. 2022 Jun;37(3):567-82.
- ↑ Shanmugam VK, Fernandez SJ, Evans KK, McNish S, Banerjee AN, Couch KS, Mete M, Shara N. Postoperative wound dehiscence: predictors and associations. Wound Repair and Regeneration. 2015 Mar;23(2):184-90.
- ↑ Rosen RD, Manna B. Wound Dehiscence. In: Treasure Island (FL): StatPearls Publishing; [Updated 2021 May 9]. available at https://www.ncbi.nlm.nih.gov/books/NBK551712/