Anterior Interosseous Nerve Syndrome
Clinically Relevant Anatomy[edit | edit source]
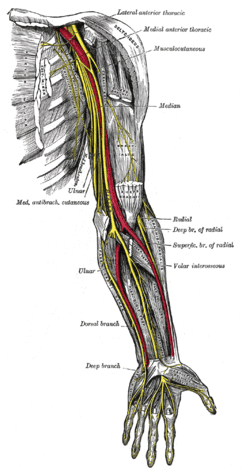
The anterior interosseous nerve (AIN) is the terminal motor branch of the median nerve. It branches from the median nerve in the proximal forearm just below to the elbow joint. It is about 5–8 cm distal to the lateral epicondyle and 4 cm distal to the medial epicondyle. It then passes between the two heads of the pronator teres muscle to run deep along the interosseous membrane along with anterior interosseous artery. and innervate following three muscles from proximal to distal, flexor pollicus longus (FPL), the index and long fingers of the flexor digitorum profundus (FDP), and the pronator quadratus (PQ). [1][2]
AIN syndrome is a pure motor neuropathy which is an isolated palsy of these three muscles. It manifests mostly as pain in the forearm accompanied frequently by a characteristic weakness of the index and thumb finger pincer movement. Many cases of AIN syndrome arise secondary to transient neuritis, although nerve compression and trauma are known etiologies as well. [1]
Parsonage and Turner first described the syndrome in 1948. Leslie Gordon Kiloh and Samuel Nevin defined it as an isolated lesion of the anterior interosseous nerve in 1952. It was known as Kiloh-Nevin syndrome.[1]
Mechanism of Injury / Pathological Process[edit | edit source]
Mechanism of injury can be grouped as either spontaneous or traumatic.
- Traumatic: Traumatic causes are forearm fractures such as supracondylar fractures, penetrating injuries and stab wounds, cast fixation, venipuncture, vial neuritis, and complication of open reduction and internal fixation of fractures.
- Spontaneous: Spontaneous causative factors are brachial plexus neuritis, compartment syndrome, and compression neuropathy. The most common site of AIN entrapment/compression is the tendinous edge of the deep head of the pronator teres muscle. Rheumatoid disease and gouty arthritis may be predisposing factors in anterior interosseous nerve entrapment.[1]
It is a rare disease which comprises only 1% of all upper extremity palsies.[1][2]
Clinical Presentation[edit | edit source]
AIN is a motor nerve so true AIN syndrome presentation will present with motor deficits only. There won't be any sensory complain. Poorly localized pain in the forearm and cubital fossa is usually the primary complaint along with difficulty bringing the distal phalanx of the thumb and index finger together. The patient may also complain of having difficulty forming a fist or the inability to button their shirts. [1][2]
On a physical examination, the patient will show weakness of the FLP and FDP to the index finger with a positive Pinch Grip test (Froment’s sign); rather than making the "OK" sign, the patient will clap the sheet between the index finger and an extended thumb. [1]
Sign of Benediction: When a patient is asked to make a fist, the patient will not be able to flex the 2nd and 3rd finger showing hand of benediction. It is different from Ulnar claw hand.
AINS can be confounded by the Martin-Gruber anastomosis, present in up to 25% of the population: in these cases, the anterior interosseous nerve gives off branches to the ulnar nerve, creating atypical motor innervation patterns of the forearm and hand and thus effacing the typical clinical symptoms. [3]
Diagnostic Procedure[edit | edit source]
The utilization of electrodiagnostic studies, coupled with MRI, is poised to assist in the diagnosis of anterior interosseous nerve syndrome and help to specify the possible etiology. Sensory nerve conduction studies of the median nerve should be normal as there is no sensory innervation to the anterior interosseous nerve. Electromyography will show findings in the flexor pollicus longus, the radial portion of the flexor digitorum profundus, and the pronator quadratus. These will be helpful in differentiating neurologic amyotrophy from compression neuropathy.[1]
Magnetic Resonance Imaging ( MRI) is also a helpful evaluation procedure.[2]
Outcome Measures[edit | edit source]
It is very necessary to use outcome tools to see the prognosis and also to determine the goal of the patient following AIN syndrome. There are various outcomes addressing hand dexterity and also a simple manual muscle test (MMT) can be used as an outcome measure.[5]
Management / Intervention[edit | edit source]
An interprofessional approach to treatment is ideal. Traumatic AIN syndrome can be treated by treating the associated etiologies. Spontaneous anterior interosseous nerve syndrome's optimal treatment has not yet been established. Rather evidence recommends that surgical interventions be offered only to those patients who do not demonstrate any clinical improvement during the first few months or to those with confirmed cases of compression neuropathy. If the patient etiology is not confirmed then, for 3 months, the patient needs initially to be treated conservatively with rest, analgesia with anti-inflammatory medications, and physiotherapy for forearm flexor muscle stretching exercises, nerve gliding exercises and activity modification.[2] Upon follow up even after weeks of conservative treatment if the patient is not improving or deteriorating then surgical intervention consists of exploration, neurolysis, and decompression that may be needed.[1]
The study done by Kodama et al. 2019 had shown that patients who underwent surgical treatment within 8 months after symptom onset showed good recovery, with MMT whereas patients who underwent surgical treatment more than 12 months after onset showed poor recovery with MMT. Thus, conservative treatment for AIN syndrome should be continued when patients show signs of recovery within 6 months after symptom onset and surgical treatment may be performed within 8 months from the onset of symptoms when the patients show no recovery signs for 6 months.[5]
The prognosis is usually good, and most cases don't require surgical treatment. If conservative therapy fails beyond three months, surgery might be offered in select cases.[1]
Physiotherapy management[edit | edit source]
Based on the cause of AIN syndrome, physiotherapy management varies. In spontaneous AIN syndrome, physiotherapy intervention plays a vital role as the exact cause for the palsy is unknown. Since it is motor neuropathy, the goals of physiotherapy intervention are:
- to maintain muscle integrity.
- to decrease the over sensitivity of nerve.
- to prevent contractures.
- to increase strength of respective muscles.
So to achieve those goals following intervention can be given but it should be individualized and follow up assessment every month is a must.
- Nerve mobilization exercises of upper extremity.
- Stretching exercise of forearm
- Electrical stimulation- TENS (Transcutaneous Electrical Stimulation) or NMES (Neuromuscular Electrical Stimulation)
- Soft tissue mobilization of forearm musculature.
- Strengthening exercises of hand and wrist.
A case report published on 2016 has used cryo massage, neural mobilization, transcutaneous electrical nerve stimulation (TENS), and the strain-counter strain (SCS) technique four times a week for two weeks in the patient who has had AIN syndrome due to active trigger point in the middle of the anterior forearm. In this study, strain- counter strain is defined as an indirect myofascial technique that is used to treat somatic dysfunctions of the neuro-musculoskeletal system. After these intervention, the patient has shown an improved pinch grip strength of eight pounds, an inactive trigger point confirmed through palpation, and improved handwriting.[6]
Differential Diagnosis[edit | edit source]
Anterior interosseous nerve entrapment or compression injury is rare and remains a challenging clinical diagnosis. Some of the differential diagnoses are: stenosing tenosynovitis, flexor tendon adherence or adhesion, flexor tendon rupture, and brachial neuritis. [1]
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 Akhondi H, Varacallo M. Anterior interosseous syndrome. InStatPearls [Internet] 2019 Jun 4. StatPearls Publishing.
- ↑ 2.0 2.1 2.2 2.3 2.4 Aljawder A, Faqi MK, Mohamed A, Alkhalifa F. Anterior interosseous nerve syndrome diagnosis and intraoperative findings: A case report. International Journal of Surgery Case Reports. 2016 Jan 1;21:44-7.
- ↑ Radiopaedia. Anterior interosseous nerve syndrome. Available from: https://radiopaedia.org/articles/anterior-interosseous-nerve-syndrome-1 (last accessed: 6/26/2020)
- ↑ Anterior Interosseous Nerve - Everything You Need To Know - Dr. Nabil Ebraheim. Available from:https://www.youtube.com/watch?v=R15I0JzYIDc. Last accessed: [6/26/2020]
- ↑ 5.0 5.1 Kodama N, Ando K, Takemura Y, Imai S. Treatment of spontaneous anterior interosseous nerve palsy. Journal of Neurosurgery. 2019 Mar 8;132(4):1243-8.
- ↑ Goyal M, Goyal K, Narkeesh K, Samuel AJ, Sharma S, Chatterjee S. The strain–Counter strain technique in the management of anterior interosseous nerve syndrome: A case report. Journal of Taibah University Medical Sciences. 2017 Feb 1;12(1):70-4.