Neurophysiological Facilitation of Respiration (NPF)
Neurophysiological Facilitation of Respiration (NPF)[edit | edit source]
Neurophysiological Facilitation of Respiration is a treatment technique used for respiratory care of patients with unconscious or non-alert, and ventilated, and also with a neurological condition
NPF is the use of external proprioceptive and tactile stimuli that produce reflex respiratory movement responses and that increase the rate and depth of breathing
Techniques[edit | edit source]
There are six techniques used in the NPF
- Perioral pressure
- Intercoastal stretch
- Thoracic vertebral pressure
- Co-contraction of the abdominal muscles
- Applied manual pressure
- Anterior stretch-lifting of the posterior basal area (Basal Lift)
Perioral pressure[edit | edit source]
Method
The pressure is applied to the patient's top lip by the therapist's finger and maintained. The pressure is maintained for the length of time that the therapist wishes the patient to breathe in the activated pattern. (As a precautionary measure the use of surgical gloves is advised to avoid picking up a contaminant and/or carrying contaminants from one patient to another).[1]
Observation
- Increased epigastric excursions
- As the stimulus is maintained the epigastric excursions may increase so that movement is transmitted to the upper thorax and the patient appears to be deep breathing
- Swallowing
- Mouth closure
Mechanism
The primitive reflex response related to sucking
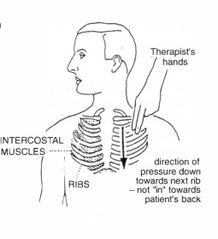
Intercoastal stretch[edit | edit source]
Method
Intercostal stretch is provided by applying pressure to the upper border of a rib in order to stretch the intercostal muscle in a downward(not inward) direction. The stretch position is then maintained while the patient continues to breathe in his/her usual manner. This procedure can be performed unilaterally or bilaterally on any rib.[1]
Observation
Increased movement of the area being stretched[1]
Mechanism
Intercostal stretch reflex[1]
Thoracic vertebral pressure[edit | edit source]
Method
- vertebral pressure high - manual pressure applied to thoracic vertebrae in the region T2 - T5[1]
- vertebral pressure low - manual pressure applied to thoracic vertebrae in the region T9 - T1[1]
Observation
vertebral pressure high
- Increased epigastric excursions
- Deep-breathing
vertebral pressure low
- Increased respiratory movements of the apical thorax
Mechanism
Dorsal-root-mediated intersegmental reflex
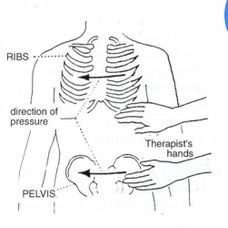
Co-contraction of the abdominal muscles[edit | edit source]
Method
Co -contraction of the abdominal muscles applied by the therapist placing one hand on the patient's lower ribs and one on the pelvis on the same side and pushing with moderate pressure so that force is applied at right angles to the patient.[1]
Observation
- Increased epigastric movements
- Increased muscle contraction (rectus abdominous)
- Decreased girth in obese
- Increased firmness to palpation
- Depression of umbilicus
Mechanism
Stretch receptors in abdominal muscles
Moderate manual pressure[edit | edit source]
Method
Mild pressure of the open hand(s) is maintained over the area in which expansion is desired[1]
Observation
Gradually increased excursion under the area of pressure
Mechanism
Cutaneous afferents
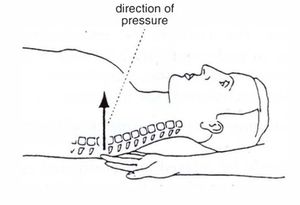
Anterior stretch-lifting of the posterior basal area (Basal Lift)[edit | edit source]
Method
Basal lift is applied by placing the hands under the posterior ribs of the supine patient and lifting gently upwards. The lift is maintained and provides a maintained stretch and pressure posteriorly and stretch anteriorly as well[1]
Observation
- Expansion posterior basal area
- Increased epigastric movements
Mechanism
Stretch receptors in intercostals. back muscles
Indication[edit | edit source]
- Neurologically impaired adult patients who are hypoventilating or have retained secretions (impaired tracheobronchial clearance, reduced lung volumes)[2]
- Used to alter respiratory pattern and relieve the symptoms of hyperventilation syndrome (control of breathing).[2]
- Unconscious and non-alert patients