Toenail Issues in Older Persons
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton and Uchechukwu Chukwuemeka
Introduction[edit | edit source]
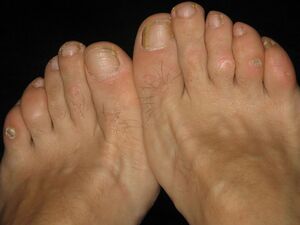
One of the hardest things to do regarding personal hygiene as we age is cutting toenails. With advancing age, morphology of the nail plate occurs with a reduction in growth rate as well as changes in colour and contour[1]. They tend to become a yellow-gray colour and can become opaque and a peculiar discolouration called "Neapolitan nail" occurs in ~20% of older people[2]. The nail can also become fissured, split or striated which can cause some alarm for some people. It is important to note that all become more common in those with osteoporosis[2].
Cutting Nails[edit | edit source]
Thirty one percent of older people are unable to cut their own toenails because the following[3]:
- Unable to reach their feet
- Lack finger dexterity to the point they are unable to use the clippers
- Get dizzy when bending
- Visual impairment
- Thick toenails
Fungal Infections[edit | edit source]
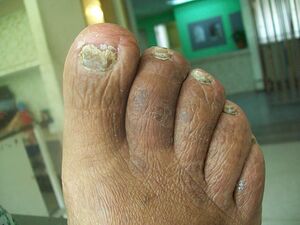
It is estimated that around a third of older people have fungal infections of the toenail, even higher in those with diabetes, CVD or obesity[4]
Onychomycosis is the most common nail infection (representing around 50% of all infections) and is common in the elderly[5]. Increased risk of onychomycosis is associated with multiple factors, including male sex, old age, smoking, underlying medical diseases (eg, peripheral arterial disease, diabetes, and immunodeficiency), and predisposing genetic factors[5].
Brittle Nails[edit | edit source]
Brittle nails (fragilitas unguium) affects around 20% of the population and in most places in the world, this is a conservative estimate in the elderly population. It clinically manifested with varying degrees of onychoschizia (localized hypertrophy of the nail plate) or onychorrhexis (subungual corn).
- Onychoschizia is usually caused by impairment of intercellular adhesion between the corneocytes that make up the nail plate. Exogenous factors (eg, repetitive cycles of wetting and drying, trauma, and fungal proteolytic products) and chemicals or cosmetics (eg, cuticle removers, nail enamel solvents, and nail hardeners) are among the underlying causes.
- Onychorrhexis frequently manifests as nail plate splitting or ridging, longitudinal thickening, or multiple splits leading to triangular fragments at the free edge. It is usually the result of nail matrix involvement leading to abnormalities in epithelial growth and keratinization. Among the various factors causing onychorrhexis are abnormalities of vascularization and oxygenation (such as anemia or arteriosclerosis), as well as systemic (metabolic, endocrine, etc) and dermatologic diseases (disorders of cornification and inflammatory diseases).
Ingrown Toenail[edit | edit source]
An ingrown toenail (Onychocryptosis) is a common discomfort that involves the nail curving down, into the surrounding skin as it grows. Most prevalent in the big toe. Ingrown toenails can be painful, display redness, swelling, and infection (yellow drainage). Ingrown toenails frequently resolve without medical treatment; however, chronic or complicated cases may require treatment by a physician[6].
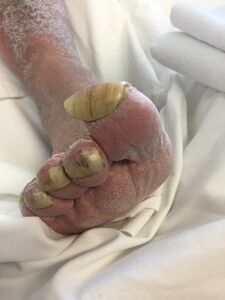
Rams Horn Nails[edit | edit source]
Ram’s horns nails, also called onychogryphosis, is a condition characterized by a thickening and lengthening of the fingernails or toenails to such a degree that they begin to resemble claws or a ram’s horn. Commonly caused by self-neglect coupled with a failure to cut the nails for an extended period of time. It is most often seen in the elderly community, as many older people don’t have the ability or wherewithal to practice good hygiene. Other cases of onychogryphosis are caused by trauma to the hands and feet, peripheral vascular disease, fungal infections, ichthyosis and syphilis. Sometimes onychogryphosis is congenital, meaning it is present at birth and therefore hereditary[7]. Left alone, it can lead to nails growing into the skin, causing pain, inflammation and infection. It also leaves the feet and hands a perfect place for different types of fungus to thrive.
Onychogryphosis is treated with avulsion of the nail plate (complete nail removal), by eg podiatrist with a local anaesthetic. Nail avulsion may lead to chronic ingrown toenails so it may be done in a surgical procedure that destroys the nail matrix (with phenol or a carbon dioxide laser) to prevent ingrown nails. The procedure is known as a partial or full matrixectomy (permanent nail removal).[7]
Owning individual nail clippers and files prevents cross contamination of infections along with regular washing and maintenance[8]. Toenail cutting services may be an alternative option to those unable to cut their own nails.
Toenail Care[edit | edit source]
Top tips include:
- Easier to cut after having a warm bath
- Straight cuts to the nails
- Filed sharp or rough edges
In the context of brittle nails it is important to consider the predominance of either onychoschizia or onychorrhexis and then correct these underlying issues. General therapeutic management may include nail hydration with daily 15-minute soaks using emollients rich in phospholipids[9]. Application of nail hardeners containing formaldehyde can be used to strengthen the nail plate[9]. However caution should be entertained when using these products, as they might cause brittleness, subungual hyperkeratosis, or onycholysis (ie, separation of the nail plate from the underlying nail bed). Mechanical nail plate protection and fracture filling can be accomplished using enamel; however, considerable dehydration might occur when it is removed afterward.
Overall it is not always the physiotherapists job to manage the nail conditions however, basic advice is always worth sharing with the patient. The main thing to be aware of is that elderly patients might complain of common nail changes and dystrophies that cause pain, affect daily activities, are of cosmetic concern. Awareness of these conditions is essential for onward referral to optimally manage the issues.
References[edit | edit source]
- ↑ Cohen PR, Scher RK. Geriatric nail disorders: diagnosis and treatment. J Am Acad Dermatol. 1992;26(4):521–31.
- ↑ 2.0 2.1 Abdullah L, Abbas O. Common nail changes and disorders in older people: Diagnosis and management. Canadian Family Physician. 2011;57(2):173-181.
- ↑ Soliman A, Brogan M. Foot assessment and care for older people. Nursing Times. 2014; 110(50): 12-15.
- ↑ Health in Aging. Foot Problems. [ONLINE] Accessed from http://www.healthinaging.org/aging-and-health-a-to-z/topic:foot-problems/ [23/03/2017]
- ↑ 5.0 5.1 Gupta AK, Ricci MJ. Diagnosing onychomycosis. Dermatol Clin. 2006;24(3):365–9.
- ↑ Foot and Anle Inst. 19 Problems with ageing feet. Available:https://www.footankleinstitute.com/blog/19-foot-problems-in-aging-feet/ (accessed 15.5.2022)
- ↑ 7.0 7.1 Foot files Rams horn nails Available:https://www.footfiles.com/subject/rams-horn-nails (accessed 15.5.2022)
- ↑ Woodrow P et al (2005) Foot care for non-diabetic older people. Nursing Older People; 17: 8, 31-32.
- ↑ 9.0 9.1 Van de Kerkhof PC, Pasch MC, Scher RK, Kerscher M, Gieler U, Haneke E, et al. Brittle nail syndrome: a pathogenesis-based approach with a proposed grading system. J Am Acad Dermatol. 2005;53(4):644–51.