Primary-Progressive Multiple Sclerosis (PPMS) - A Case Study
Abstract[edit | edit source]
Purpose: This is a fictional case study designed to understand and explore an individual diagnosed with Primary Progressive Multiple Sclerosis (PPMS). Additionally, we investigated and applied a research-based treatment approach while integrating the role of technology in rehabilitation.
Case Presentation: The case study focuses on Michelle White, a 47year old female who is a work-from-home accountant who recently progressed from active PPMS without progression to active PPMS with progression. Her primary complaints were fatigue, difficulty with a normal gait, impaired balance, weakness, and decreased attention and memory.
Intervention: Mrs. White was prescribed activities and exercises that will maintain and improve her function as her PPMS continues to progress. These interventions were designed to target the patient's short and long-term goals, allowing her to regain and maintain function that has been deemed meaningful to the patient. Treatments prescribed included aerobic exercise, resistance training, balance training, fatigue management, education as well as referrals to target problems that are outside the scope of physiotherapy. Technology was utilized during the patient's rehabilitation in a multitude of ways.
Outcomes: At the 4-month reassessment, the patient was reassessed using the following outcome measures; Multiple Sclerosis Walking Scale, 6 Minute Walk, mini BESTest, Activities Balance Confidence Scale, 5 Times Sit to Stand Test, and the Modified Fatigue Impact Scale. After completing her physiotherapy sessions, her home exercise routine, and additional appointments with members of her inter-professional team, the patient was able to improve her abilities and confidence with ambulation, balance, and activities of daily living (ADLs).
Introduction[edit | edit source]
Multiple sclerosis (MS) is a neurological, autoimmune disease that affects the central nervous system.[2] Though the exact aetiology of MS is unknown, it occurs when the immune system attacks nerve fibers and the myelin sheath of neuronal axons, leading to inflammation and demyelination of the central nervous system.[3] As a result, it alters electrical signaling in the brain and leads to a variety of symptoms, such as difficulty with walking, blindness, paralysis, etc.[4] In Canada, over 90,000 people are living with MS, which equates to 1 in every 400 people.[5] Annually, 4,377 Canadians are diagnosed with MS, which equates to almost 12 people per day.[5]
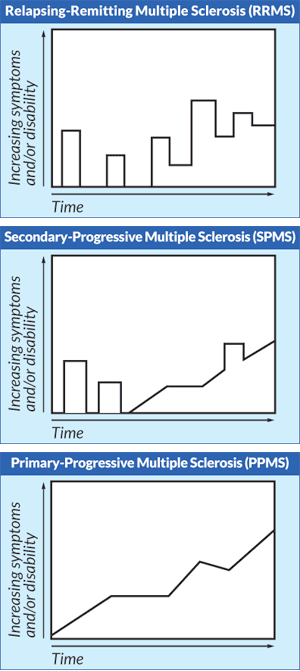
A thorough medical history in conjunction with a neurological examination and imaging are used to diagnose MS, and it is diagnosed once other potential reasons for symptoms are ruled out.[6] MS can be classified into four types of diagnoses: clinically isolated syndrome, relapsing remitting, secondary progressive and primary progressive.[7]
Primary progressive multiple sclerosis (PPMS) is characterised by a gradual deterioration in functional capacity due to neurological deficits, without the occurrence of early relapses (exacerbation or flare-ups). Furthermore, this type of MS can be categorized as active (confirmed via an occasional relapse and/or imaging) or inactive, as well as progressive (evident decrease in functional capacity) or non-progressive.[8] Globally, 10-15% of individuals diagnosed with MS present with PPMS[3].
This fictional case study will highlight the experience of Michelle White, a 47-year-old female who was diagnosed with PPMS. Michelle was referred to physiotherapy due to an acute exacerbation of PPMS, and her primary goals with rehabilitation are to improve her walking capacity and ability to perform ADLs. The purpose of this case study is to provide evidence-based information from the literature regarding symptoms, objective findings, and interventions for PPMS.
Client Characteristics [edit | edit source]
Michelle White is a 47-year-old female (DOB March 14th, 1975) who was diagnosed with PPMS 2 years ago. Since the onset of her symptoms, Mrs. White's status has changed from being in the active without progression PPMS stage (increasing accumulation of disability), to active (new MRI changes) with progression (increasing accumulation of disability). Mrs. White was diagnosed with clinical depression 1 year ago and has been managing hypertension for the last 5 years. Mrs. White is a work-from-home accountant and currently resides in a detached home in Mississauga, Ontario with her husband, 2 children, and a family dog. Mrs. White was referred to rehabilitation by her neurologist to reduce the risk of a relapse, as well as to help improve her mobility (walking with the use of a mobility aid and balance training) and function (activities of daily living).
Examination Findings[edit | edit source]
Initial Assessment: May 3rd, 2022
Subjective Assessment[edit | edit source]
Chief Complaint: Mrs. White has concerns about taking her dog for daily walks in the summer. She is afraid of losing her balance and worried she won’t have enough energy to complete the walks. Mrs. White is also having trouble with the stairs in her house. She finds her legs weak and she is tired by the time she reaches the top of the stairs.
History of Present Illness:
- Medical diagnosis: PPMS active with progression
- Treatment to Date: No previous history of physiotherapy treatment.
- Current Symptoms:
Past Medical History:
- Diagnosed with active PPMS without progression 2 years ago
- Diagnosed with active PPMS with progression 2 weeks ago
- Co-morbidities:
- Depression[11] - diagnosed 1 year ago
- Prescribed medications
- Weekly visits to a psychiatrist to help with depressive symptoms
- Hypertension[11] - diagnosed 5 years ago
- Depression[11] - diagnosed 1 year ago
Medications:
- Oral Paroxetine - 20mg, once a day for depressive symptoms[9][12]
- Norvasc (Amlodipine) - 5mg, once per day for hypertension[12]
- Ocrevus - 600 mg intravenous infusion every six months[12]
Social History: Mrs.White lives in Mississauga in a house with 2 steps to get into the house as well as 12 steps to get to the second floor. She lives there with her husband, 2 children, and a family dog. She has been a work-from-home accountant for the last 15 years. Mrs.White enjoys working from home but has noticed in the last few months that she has trouble concentrating on her work and thinks her memory has gotten worse. Her family recently moved to Mississauga from Ottawa last year, and friends and distant family are still located in Ottawa. Mrs.White enjoys walking her dog daily, reading, and watching movies. However, she finds when she sits in the same position for a long period her pain and discomfort increase.
Family History: History of hypertension on maternal side.
Functional History: Mrs.White was previously able to ambulate for 45 minutes with her dog without the use of a gait aid. She was also less fearful of community ambulation. She previously enjoyed gentle weight-bearing resistance training at her local gym, often going twice a week for about 30-45 minutes. Mrs.White was also able to walk up a flight of stairs without fatigue. She had no problems with her daily activities such as grooming, cleaning, and cooking. However, she found carrying laundry up the stairs quite difficult but often received help from her husband or children.
Current Functional Status: Mrs.White has been cutting back on the length of her workouts at the gym as she now finds resistance training more painful and difficult due to balance impairments. Mrs.White has also become more fearful of community ambulation due to fear of falling, and currently only walks around the block. She walks the dog only twice a week due to her balance and stability deficits and will only go if her husband or one of her children accompanies her. Mrs.White is often fatigued and feels weak after walking up a flight of stairs and is unable to carry her laundry up the stairs anymore. She still manages her daily activities well but finds herself tired if she does a large cleaning of the house.
Patient Goals:
- Mrs.White would like to get back to walking her dog 3-4 days a week, independently.
- Mrs.White would also like to limit the progression of her symptoms.
- Mrs.White would like to improve her strength to be able to walk upstairs better.
Objective Assessment[edit | edit source]
- Upper extremity (UE) - Within normal limit (WNL)
- Lower extremity (LE) - Table 1
| Joint | Movement | Active ROM - LEFT | Passive ROM - LEFT | Active ROM - RIGHT | Passive ROM -RIGHT |
| Hip | Flexion | 100 | 105 | 90 | 100 |
| Hip | Extension | 10 | 15 | 10 | 15 |
| Hip | Adduction | 20 | 30 | 20 | 30 |
| Hip | Abduction | 40 | 45 | 40 | 45 |
| Hip | External Rotation | 30 | 40 | 30 | 40 |
| Hip | Internal Rotation | 30 | 40 | 30 | 40 |
| Knee | Flexion | 125 | 130 | 115 | 125 |
| Knee | Extension | 0 | -5 | -5 | -5 |
| Ankle | Plantar flexion | 40 | 45 | 35 | 45 |
| Ankle | Dorsiflexion | 10 | 15 | 5 | 10 |
| Ankle | Inversion | 15 | 20 | 10 | 15 |
| Ankle | Eversion | 5 | 10 | 5 | 10 |
Spasticity
- UE - WNL
- LE - Table 2
| Muscle Group | Left Limb | Right Limb |
| Hip Flexors | 0 | 0 |
| Hip Extensors | 0 | 0 |
| Hip Adductors | 0 | 0 |
| Hip Abductors | 0 | 0 |
| Knee Flexors | 1 | 1 |
| Knee Extensors | 1 | 1 |
| Ankle Plantar Flexors | 1+ | 2 |
| Ankle Dorsiflexors | 1 | 1+ |
Strength
5 Times Sit to Stand Test: 7.3 seconds[14]
Manual Muscle Testing (MMT)
- UE - WNL
- LE - Table 3
| Muscle Group | Left Limb | Right Limb |
| Hip Flexors | 4+ | 4+ |
| Hip Extensors | 4 | 4 |
| Hip Adductors | 4 | 4 |
| Hip Abductors | 4 | 3+ |
| Hip External Rotators | 4 | 3+ |
| Hip Internal Rotators | 4 | 3+ |
| Knee Flexors | 4 | 4- |
| Knee Extensors | 4 | 4- |
| Ankle Plantar Flexors | 4 | 4 |
| Ankle Dorsiflexors | 4- | 3+ |
| Ankle Inverters | 4- | 4- |
Neurological
- Dermatomes - WNL
- Myotomes - WNL
- Reflexes
- Sensation testing - decreased pinprick sensation to dorsal feet bilaterally[15]
- Proprioception - contralateral joint matching task - reduced proprioception found in the ankle joint[15]
Gait
- 3D Motion Analysis - Gait Deviations:
- Assessment Measures
- 6 Minute Walk Test: 348m[17]
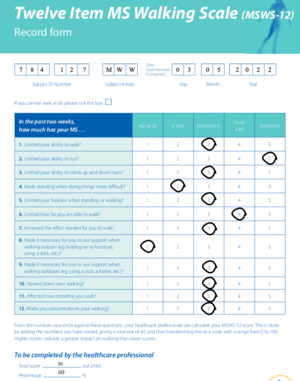
- Multiple Sclerosis Walking Scale – 12 (MSWS-12): 36/60 (60%)[18]
- See Figure 1
Balance
Assessments:
- Mini BESTest: 11/28[19]
- See Figure 2
- Activities Balance Confidence Scale (ABC): 69%[20]
- See Figure 3
Fatigue
- Modified Fatigue Impact Scale (MFIS): 50/84[21]
- See Figure 4
Clinical Impression[edit | edit source]
Patient Profile
Mrs. White is a 47-year-old female with PPMS that has been experiencing declining function since her disease progressed to active progression. Currently, Mrs. White is presenting to outpatient rehabilitation with significantly impaired mobility and balance due to lower extremity weakness and spasticity, reduced sensation of the feet, gait deviations, and fatigue. Additionally, Mrs. White is also experiencing urgency incontinence and cognitive deficits that are also impacting her quality of life.
Problems list
- Body structure function
- Reduced balance due to decreased proprioception and weakness in lower extremities.
- Impaired memory due to disease progression.
- Impaired sensation due to irreversible destruction of the myelin sheath and axons of nerves.[22]
- Mild drop foot gait with poor heel strike due to weak dorsiflexors.
- Increased muscle tone/spasticity around ankle and knee joints due to demyelinated nerves in the brain and spinal cord.[23]
- Weak hip abductors, hip external and internal rotators, knee extensors and flexors, and ankle dorsiflexors due to demyelinated peripheral nerves.
- Activity
- Difficulty climbing stairs due to fatigue and SOB.
- Urgency incontinence due to weakened sphincter muscles.
- Reduced attention span due to fatigue and cognitive deficits.
- Reduced walking endurance due to gait deviations and fatigue.
- Participation
- Unable to walk her dog due to impaired mobility and fatigue.
- Avoids resistance training due to pain and lack of stability.
- Difficulty concentrating at work due to impaired memory and attention deficits.
- Personal factors
- Patient is fearful of falling.
- Reduced productivity at work due to pain during prolonged positioning.
- Easily fatigued.
- Diagnosed with depression 1 year ago.
- Environmental
- The patient's home has 2 steps to enter, and 12 steps to reach the second floor.
Interventions[edit | edit source]
Patient-Centered Treatment Goals
Short Term Goals:
- Mrs.White will achieve a minimum of a 4/5 MMT score for all lower extremity muscle groups within 4 weeks.
- Improvement in Activities Balance Confidence Scale score from 69% to 86% within 2 weeks. [24]
- Be able to ambulate up and down 12 stairs with a single-point cane independently within 2 weeks.
Long Term Goals:
- Mrs.White will be able to lower her score on the MFIS by 10-20 points within 6 weeks.
- Mrs.White will be able to maintain or improve her lower extremity MMT scores at the current baseline within 6 months.
- Mrs.White will have the functional capacity to walk her dog independently 3 times a week for 20 minutes each within 6 weeks.
Strength Training:
- Functional exercises are prioritized, mainly targeting large muscle groups. [25]
- Examples of functional exercises: [25]
- Farmers Carry
- Sit to Stand
- 1/2 Squat
- Step ups and step downs
- Heel walking & Toe walking
- Strengthening muscles of the lower extremity will help with improving gait as well as counteract spasticity present in ankles and knees.[16]
- Mrs. White is encouraged to pick one exercise from each of the following muscle groups and complete 5-10 exercises in a training session, for 8-15 reps and 1-2 sets, 2-3 times per week:[26]
- Dorsiflexors: Toe raises, resisted dorsiflexion
- Plantarflexors: Seated heel raises, standing heel raises
- Knee Flexors: Hamstring curls, RDLs
- Knee Extensors: resisted knee extension, mini squat
- Hip Abductors: side-lying hip abduction
- The patient should be reaching slight fatigue within the outlined rep range. If the patient is able to reach 12 reps with ease, resistance can be added.
Gait Training:
- Prescribe and fit the patient to a single-point cane to improve stability while maintaining as much mobility as possible.
- Gait training may include:
- FES can be incorporated to help improve gait patterns in the early stages by facilitating dorsiflexion through activation of the tibialis anterior to improve drop foot gait. [28]
- Continue with gait training until Mrs. White is proficiently using her single-point cane for ambulation. This intervention may need to be adapted as Mrs. White's disease progresses.
- Aerobic exercise will improve the patient's aerobic capacity and improve her ability to walk for longer periods of time without fatigue. [29][25]
- Should be performed 2-3 times per week working up to around 10-30 minutes of moderate-intensity exercise (11-13 RPE on a 20-point scale).[26]
- Methods of aerobic training include:
- Treadmill training, swimming, walking, arm bike[16]
- From all options listed above, the patient's goals align most with walking therefore walking will be prioritized.
- Treadmill training, swimming, walking, arm bike[16]
- Be mindful of the patient's level of fatigue throughout training.[16]
Flexibility Training
- Mrs. White will be encouraged to partake in flexibility training daily, completing 2-3 sets of each stretch, and holding the stretch for 30-60 seconds.[26]
- Mrs. White's flexibility training will have a strong emphasis on the lower extremity to target the increased tone and spasticity that is currently presenting in the lower limbs.
- Examples of exercises that will be prescribed include:
- Plantar flexor stretch
- Hamstring stretches
- Hip Flexor stretches
- Quadriceps Stretch
- Ankle Rolls
- Gastrocnemius and Soleus Stretch
Balance/Neuromotor Training:
- In-clinic exercises, as well as the prescribed home exercise plan, should total 20-60 mins of training and be completed 3-6 times per week.[26] Specific intensity and duration will be determined for each individual task.[26] As the patient gets more comfortable, balance exercises can be performed outside of the clinical setting. Examples include: [30]
- Reaching, nudging and leaning in seated progressing to standing as well as to eyes closed as tolerated
- Standing eyes open, progressing to eyes closed and widening base of support as needed [30]
- Ankle sways [30]
- Marching in place[30]
- Adding cognitive task to any or all of the above to increase intensity and difficulty for the patient[16]
- Mrs.White was educated on and encouraged to find a program or class in Tai Chi, Yoga, or Pilates to help maintain balance abilities. [16]
- Reducing fatigue can be addressed with the 4P's: Pacing, Planning, Prioritizing, and Positioning.[16]
- Any exercise can be broken up throughout the day to manage fatigue further.[16]
- Educate Mrs. White to take breaks as required.
- Mrs. White will be educated on good times to exercise throughout the day, avoiding peak temperatures.[26] Exercise in temperature-controlled environments to avoid spikes in symptom onset will also be recommended.[26]
- Additionally, cooling techniques will be taught for when Mrs.White's temperature control is reduced. [26]
- Recommended that Mrs. White achieve 150 mins of lifestyle physical activity per week.[26]These activities can be selected by Mrs. White. Options include:
- Mrs.White is educated on the use of a single-point cane with a 2-point step-to gait pattern, progressing to a step-through pattern as she gets comfortable and her balance and stability improve.
- Mrs.White is informed that exercise is important and movement is always encouraged. [16]
- As the disease may progress, exercise is modified to ensure that the patient is doing as much as they can be based on their new functional status.[16]
- Mrs.White should seek Physiotherapy even when her symptoms are stable to follow up with functional status and make any changes to the treatment plan as necessary.
Referrals:
- Mrs.White will be referred to a Pelvic Floor Physiotherapist to help treat her urgency incontinence.
- Mrs.White will be referred to a Neurologist to work on improving her memory and attention.
- Mrs.White will be referred to a Psychiatrist to control her depression if she is not currently seeing one.
- Mrs.White will be referred to a Pharmacist to look over medications.
Outcome[edit | edit source]
After Mrs.White's initial assessment on May 3, 2022 she was reassessed on September 4th, 2022, about 4 months later. She was reassessed using the Multiple Sclerosis Walking Scale, 6 Minute Walk, mini BESTest, Activities Balance Confidence Scale, Modified Fatigue Impact Scale, and 5 times sit to stand. Table #4 below shows the change in each test. Mrs.White's improvement in the Multiple Sclerosis Walking and her 6-minute walk test demonstrates improved ability to walk indicated by increased pace, distance, and decreased effort needed to walk. Mrs.White's improved mini BESTest, Activities Balance Confidence scale, and 5 minutes Sit to Stand demonstrate the positive impact of the interventions on her dynamic balance, functional mobility, and confidence in balance. While completing these tests, Mrs. White experienced less overall fatigue. Mrs. White was able to improve her strength for the major LE muscles indicated by higher scores on MMT. Her ROM for LE did not change
| Outcome Measure | Initial Assessment: May 3rd, 2022 | Reassessment: September 4th, 2022 |
| Multiple Sclerosis Walking Scale | 36/60 or 60% | 28/60 or 47% |
| 6 Minute Walk | 348m | 387m |
| Mini BESTest | 11/28 | 16/28 |
| Activities Balance Confidence Scale | 69% | 76% |
| 5 times sit-to-stand test | 7.3 seconds | 6.9 seconds |
| Modified Fatigue Impact Scale | 50/84 | 39/84 |
After the 16-week intervention, we are pleased with the progress Mrs.White has made and she will continue treatment as needed or every 6 months. Mrs.White will continue with her home exercise program and understands she is able to contact the clinic if she has any questions or concerns. No further referrals are needed at this time.
Mrs.White has completed her initial assessment with a pelvic floor physiotherapist and will be continued to seek treatment for her urgency incontinence. Mrs.White will continue to have follow-up appointments with other members of her inter-professional care team including her neurologist and general practitioner to follow the progression of her PPMS as well as her psychiatrist to help support her depression.
Discussion[edit | edit source]
Mrs.White is a 47year old female work-from-home accountant who was diagnosed with PPMS 2 years ago. Mrs.White was referred to physiotherapy because her status recently changed from active PPMS without progression to active PPMS with progression. As a result of the progressive demyelination and recently reduced activity level, Mrs.White had been experiencing challenges with normal gait, balance, fatigue, attention, and memory. These symptoms have been affecting Mrs.White's ability to complete ADLs, work efficiently and participate in physical activity. Mrs.White's goals were to limit the progression of her symptoms, walk her dog 4 days a week and improve her strength to help with ambulation of stairs.
In her physiotherapy assessment, Mrs.White demonstrated reduced strength and flexibility of her lower extremities, with her right being worse than her left. Her neurological testing was within normal limits with the exception of reduced sensation to her dorsal feet bilaterally and reduced proprioception of the ankle joint bilaterally. Furthermore, Mrs.White displayed moderate balance impairments, fatigue, and gait deviations.
During her physiotherapy intervention, exercise was directed mostly at gait training, aerobic capacity and lower extremity exercise to target the patient's goals and limitations as best as possible. Functional and isolated resistance training exercises were performed to target both functional activities in order to improve ADL participation as well as improve the patient's widespread lower extremity weakness. Mrs.White was educated about monitoring and reducing the amount of fatigue that she experiences. Balance training was incorporated to improve the patient's stability as well as increase her confidence in her stability. Gait training was incorporated as well in order to improve the patient's function and participation.
During the 4 month re-assessment, Mrs.White improved her ability to ambulate. She was able to walk further and longer while becoming less fatigued and having more confidence. Mrs.White's balance and strength also improved over the 16-week period. Her progress demonstrated improved scores on the following tests; Multiple Sclerosis Walking Scale, 6 Minute Walk, mini BESTest, Activities Balance Confidence Scale, 5 Times Sit to Stand Test, and the Modified Fatigue Impact Scale.
Individuals with MS can present with a variety of symptoms and impairments, despite this fact, there are many aspects of this current case study that can be applied to the MS population. Firstly, it is important to have a multi-disciplinary team unique to each patient based on the symptoms they are experiencing. In this case, we included a neurologist, a psychiatrist, a pelvic floor physiotherapist, and a pharmacist. Additionally, if available, technology can be used to enhance assessment and treatment. In this case, we used 3D gait analysis to gather detailed information about gait deviations. In regards to treatment, functional electrical stimulation and robot gait training was used to help correct and strengthen the patient's gait pattern. Finally, the current case study demonstrates the importance of physical activity and exercise for patients with MS. Some of the benefits include reduced fatigue, improved mood, increased physical fitness, reduction of depressive symptoms, reduced pain, and improved balance.[31]
References[edit | edit source]
- ↑ Types of Multiple Sclerosis. Multiple Sclerosis Association of America. Available from: https://mymsaa.org/ms-information/overview/types/ (accessed May10 2022)
- ↑ What is multiple sclerosis (MS)?: The Johns Hopkins Multiple Sclerosis Center. 2015. Available from: https://www.hopkinsmedicine.org/neurology_neurosurgery/centers_clinics/multiple_sclerosis/conditions/ (accessed May10 2022)
- ↑ 3.0 3.1 Tafti D, Ehsan M, Xixis KL. Multiple Sclerosis. Treasure Island (FL): StatPearls Publishing; 2022 Available from: https://www.ncbi.nlm.nih.gov/books/NBK499849/ ([accessed May10 2022)
- ↑ What is MS? National Multiple Sclerosis Society. Available from: https://www.nationalmssociety.org/What-is-MS (accessed May10 2022)
- ↑ 5.0 5.1 Latest MS Research News: Prevalence and incidence of MS in Canada and around the world - MS Society of Canada. MS Society. 2020. Available from: https://mssociety.ca/research-news/article/prevalence-and-incidence-of-ms-in-canada-and-around-the-world (accessed May10 2022).
- ↑ Diagnosis - MS Society of Canada. MS Society. Available from: https://mssociety.ca/about-ms/diagnosing-ms (accessed May10 2022).
- ↑ Types of MS. National Multiple Sclerosis Society. Available from: https://www.nationalmssociety.org/What-is-MS/Types-of-MS (accessed May10 2022).
- ↑ Primary progressive MS (PPMS). National Multiple Sclerosis Society. Available from: https://www.nationalmssociety.org/What-is-MS/Types-of-MS/Primary-progressive-MS (accessed May10 2022).
- ↑ 9.0 9.1 9.2 9.3 9.4 Tsang BK, Macdonell R. Multiple sclerosis: diagnosis, management and prognosis. Australian family physician. 2011 Dec;40(12):948-55.
- ↑ 10.0 10.1 10.2 10.3 10.4 10.5 10.6 10.7 Miller DH, Leary SM. Primary-progressive multiple sclerosis. The Lancet Neurology. 2007 Oct 1;6(10):903-12.
- ↑ 11.0 11.1 Magyari M, Sorensen PS. Comorbidity in multiple sclerosis. Frontiers in Neurology. 2020 Aug 21;11:851.
- ↑ 12.0 12.1 12.2 Medications. MS Society of Canada. (n.d). Available from https://mssociety.ca/managing-ms/treatments/medications (accessed May10 2022).
- ↑ Harb A, Kishner S. Modified Ashworth scale. InStatPearls. 2021. StatPearls Publishing.
- ↑ Five times SIT to stand test. Shirley Ryan AbilityLab. (2013). Available from: https://www.sralab.org/rehabilitation-measures/five-times-sit-stand-test#non-specific-patient-population (accessed May10 2022).
- ↑ 15.0 15.1 Miehm JD, Buonaccorsi J, Lim J, Sato S, Rajala C, Averill J, et al. Sensorimotor function in progressive multiple sclerosis. Multiple Sclerosis Journal–Experimental, Translational and Clinical. 2020 Jul;6(3):2055217320934835.
- ↑ 16.00 16.01 16.02 16.03 16.04 16.05 16.06 16.07 16.08 16.09 16.10 16.11 16.12 A RESOURCE FOR HEALTHCARE PROFESSIONALS: Physical Therapy in Multiple Sclerosis. National Multiple Sclerosis Society. 2018. Available from: https://www.nationalmssociety.org/NationalMSSociety/media/MSNationalFiles/Brochures/Clinical_Bulletin_Physical-Therapy-in-MS-Rehabilitation.pdfb (accessed May10 2022).
- ↑ Wetzel JL, Fry DK, Pfalzer LA. Six-minute walk test for persons with mild or moderate disability from multiple sclerosis: performance and explanatory factors. Physiotherapy Canada. 2011 Apr;63(2):166-80.
- ↑ Twelve item ms walking scale (MSWS-12). Shirley Ryan AbilityLab. (n.d). Available from: https://www.sralab.org/sites/default/files/2017-07/msws-eng.pdf (accessed May5 2022).
- ↑ Mini-bestest: Balance Evaluation Systems Test. Oregon health. (n.d). Available from: https://www.sralab.org/sites/default/files/2017-06/MiniBEST_revised_final_3_8_13.pdf (accessed May 9 2022).
- ↑ Nilsagård Y, Carling A, Forsberg A. Activities-specific balance confidence in people with multiple sclerosis. Multiple sclerosis international. 2012 Aug 7;2012: 613925.
- ↑ Modified fatigue impact scale (MFIS). Shirley Ryan Abilitylab. (n.d). Available from: https://www.sralab.org/sites/default/files/2017-06/mfis.pdf (accessed May 9 2022)
- ↑ Multiple sclerosis. NORD (National Organization for Rare Disorders). 2020. Available from: https://rarediseases.org/rare-diseases/multiple-sclerosis/ (accessed May 9 2022)
- ↑ Spasticity (stiffness). MSAA. 2022. Available from: https://mymsaa.org/ms-information/symptoms/spasticity/ (accessed May 9 2022)
- ↑ Raad J, Moore J, Hamby J, Rivadelo RL, Straube D. A brief review of the Activities-Specific Balance Confidence Scale in older adults. Archives of Physical Medicine and Rehabilitation. 2013 Jul 1;94(7):1426-7.
- ↑ 25.0 25.1 25.2 Feinstein A, Freeman J, Lo AC. Treatment of progressive multiple sclerosis: what works, what does not, and what is needed. The Lancet Neurology. 2015 Feb 1;14(2):194-207.
- ↑ 26.00 26.01 26.02 26.03 26.04 26.05 26.06 26.07 26.08 26.09 26.10 26.11 26.12 26.13 26.14 Kalb R, Brown TR, Coote S, Costello K, Dalgas U, Garmon E, et al. Exercise and lifestyle physical activity recommendations for people with multiple sclerosis throughout the disease course. Multiple Sclerosis Journal. 2020 Oct;26(12):1459-69.
- ↑ 27.0 27.1 Lo AC, Triche EW. Improving gait in multiple sclerosis using robot-assisted, body weight supported treadmill training. Neurorehabilitation and neural repair. 2008 Nov;22(6):661-71.
- ↑ Campbell E, Coulter EH, Mattison PG, Miller L, McFadyen A, Paul L. Physiotherapy rehabilitation for people with progressive multiple sclerosis: a systematic review. Archives of physical medicine and rehabilitation. 2016 Jan 1;97(1):141-51.
- ↑ Beer S, Khan F, Kesselring J. Rehabilitation interventions in multiple sclerosis: an overview. Journal of neurology. 2012 Sep;259(9):1994-2008.
- ↑ 30.0 30.1 30.2 30.3 Jackson K, Mulcare JA, Donahoe-Fillmore B, Fritz HI, Rodgers MM. Home balance training intervention for people with multiple sclerosis. International Journal of MS Care. 2007;9(3):111-7.
- ↑ Motl RW, Sandroff BM. Benefits of exercise training in multiple sclerosis. Current neurology and neuroscience reports. 2015 Sep;15(9):1-9.










