Prader-Willi Syndrome
Original Editor - Rucha Gadgil
Top Contributors - Rucha Gadgil, Naomi O'Reilly, Candace Goh, Amanda Ager and Khloud Shreif
What Is Prader-Willi Syndrome?[edit | edit source]
Prader-Willi syndrome (PWS) is a rare genetic disorder caused by the abnormal functioning of specific genes on chromosome 15. The condition is named after Swiss physicians Andrea Prader and Heinrich Willi and Alexis Labhart who described it in detail in 1950s[1]. It is also called as Prader-Labhart-Willi, or Prader-Willi-Fanconi Syndrome.
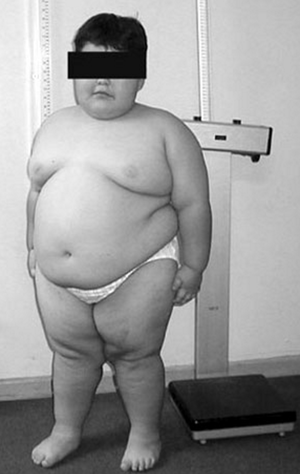
It is characterized by small hands and feet, abnormal growth and body composition (small stature, early onset childhood obesity), hypotonia (weak muscles) at birth, hypogonadism, insatiable hunger, extreme obesity, and intellectual disability.
Prevalence[edit | edit source]
PWS affects an estimated 1 in 15,000 - 30,000 people[2]. The prevalence rates differ among studies across countries, mainly due to using different methods for case identification. There is no strong evidence for increased risk in specific countries or gene pools. Both sexes are affected equally[2].
Etiology and Pathological Process[edit | edit source]
People normally inherit one copy of chromosome from each parent except those with sex characteristics. Some of these genes activate only on the copy inherited from a person's father (the paternal copy). This is called as genomic imprinting.
PWS is caused due to abnormality in the expression of genes on Chromosome 15 specifically on the long arm of chromosome 15q11-q13. This abnormality can be caused due to[3]:
- Deletion of the genes on the paternal copy (70-80%)
- The genes on the maternal copy are turned off (inactive) (20-25%)
- Has two copies of chromosome 15 inherited from the mother instead of one copy from each parent (maternal uniparental disomy) (1%)
- Chromosomal rearrangement called a translocation (<1%)
- By a mutation or other defect (Imprinting center defects) (1%)
Prader-Willi syndrome is the first human disorder attributed to genomic imprinting.
The PW genes identified are[4]:
- SNRPN and NDN necdin genes,
- clusters of snoRNAs: SNORD64, SNORD107, SNORD108 and two copies of SNORD109
There are significant advances in understanding and characterizing the genetic changes associated with PWS that have taken place, though, the exact mechanism by which lack of functional genetic material causes PWS is not understood. Researchers are still studying the normal role of the genetic sequences in the PWS region and how their loss affects multiple other systems in the body.
The genetic changes associated with this disorder present as random events when reproductive cells are forming or in early embryonic development. Hereditary and familial transmission is very rarely seen.
Clinical Features[edit | edit source]
The Clinical Features vary according to the age and individual. The signs and symptoms change over time from childhood to adulthood. The clinical features aid in diagnosis of the PWS. They are categorized into major, minor and supportive findings[5]:
In Infants:
Signs and symptoms that may be present include:
Major Findings:
- Poor muscle tone: poor muscle tone (hypotonia)
- Developmental Delay[6]
- Distinct facial features: almond-shaped eyes, a narrowing of the head at the temples, a turned-down mouth and a thin upper lip.
- Poor sucking reflex: feeding difficulty causing failure to thrive.
- Underdeveloped genitals: Males may have a small penis and scrotum or cryptorchidism. In females, the clitoris and labia may be small.
- Obesity: PWS is the most common cause of genetic obesity, with a prevalence between one in 20,000 and one in 30,000 births.[7]
Minor Findings:
- Generally poor responsiveness: A baby appears unusually tired, responds poorly to stimulation or have a weak cry.
Early childhood to adulthood
Features of Prader-Willi Syndrome appearing during early childhood remain throughout life, requiring careful management. These features include:
Major Findings:
- Excessive appetite and overeating (hyperphagia): a constant craving for food, resulting in rapid weight gain, starting around age 2 years. Behaviors, such as hoarding food, eating frozen food or garbage is also noted.
- Hypogonadism: sex organs (testes in men and ovaries in women) produce little or no sex hormones causing incomplete or delayed puberty, and in nearly all cases, infertility. Without treatment, women may not start menstruating until their 30s or may never menstruate, and men may not have much facial hair and their voices may never fully deepen.
- Endocrinological Imbalance: Underproduction of growth hormone causing short adult height, low muscle mass and high body fat. Other endocrine problems include: 1) underproduction of thyroid hormone (hypothyroidism). 2) central adrenal insufficiency, which prevents the body from responding appropriately during stress or infections.
- Cognitive impairment: Mild to moderate intellectual disability, such as issues with thinking, reasoning and problem-solving.
- Delayed motor development: delayed motor, cognitive, and language development. The average intelligence quotient of older individuals is in the upper range of mild mental retardation. Learning disabilities may also be present.
Minor Findings:
- Speech problems: Speech is often delayed with poor articulation of words
- Behavioral problems: stubborn, angry, controlling or manipulative with frequent temper tantrums They may also develop obsessive-compulsive or repetitive behaviors, or both a well as anxiety and skin picking.
- Sleep disorders: disruptions of the normal sleep cycle, sleep apnea, excessive daytime sleepiness
- small hands and feet, short stature.
Supportive Findings:
- Scoliosis,
- Reduced saliva flow
- Vision problems: Near-sightedness
- Problems regulating body temperature,
- A high pain tolerance,
- Hypopigmentation: hair, eyes and skin are pale.
- Osteoporosis
- Early Adrenarche
Diagnosis[edit | edit source]
The diagnosis of PWS is mainly via Genetic Testing and Counselling and supported by Clinical Diagnostic Criteria.
Methods of Genetic testing and counselling:
- DNA methylation[8]: only technique which can both confirm and reject the diagnosis of PWS. Gold Standard.
- High resolution chromosomal analysis (HRCA)[9]: along with the fluorescence in situ hybridization (FISH) to detect deletions and translocation of chromosome 15
- methylation-specific multiplex ligation PCR amplification[10]
Consensus clinical diagnostic criteria have been published and modified to trigger diagnostic testing[5][11]. The Major, minor and supportive features have been reported above. The Scoring is done as:
- In children 3 years of age and younger, only five points are required for diagnosis; four must come from the major group.
- A total score of eight is necessary for the diagnosis in the 3 year to adulthood group with major criteria items comprising five or more points of the total score
Differential Diagnosis[edit | edit source]
PWS has to be differentially diagnosed with[12]:
- Craniopharyngioma: DNA methylation will help in differentiating
- Congenital myotonic dystrophy type 1
- Spinal muscular atrophy: Molecular genetic testing, EMG/NCV, and/or muscle biopsy required to differentiate these conditions.
- Angelman syndrome
- Fragile X syndrome
- WAC-related intellectual disability
- Albright hereditary osteodystrophy
- Alstrom Syndrome
- Cohen Syndrome
DNA methylation technique helps to differentially diagnose PWS from the above conditions.
Physiotherapy Management and Treatment[edit | edit source]
Currently there is no cure for PWS and treatment focuses on mainly symptom management and prevention of complications. PWS patients need continuous support from geneticists, endocrinologists, nutritionists, pulmonologists, neurologists, along with including physical, occupational, and speech therapists. Their treatment is a multidisciplinary and long-term approach. Early diagnosis and intervention are critical[13].
Main points to focus on when dealing with PWS are[14]:
- Nutrition and dietary control
- Endocrinological Aspects
- Psychological Support
- Physical, occupational and speech therapy
- Regular medical check-up for diabetes, obesity, blood pressure and vision issues.
Physiotherapy management in such cases is mainly focused on managing impairments and preventing complications along with ensuring the individual's functional growth and development.
Major areas targeted by Physiotherapy include[15]:
- Physical Therapy from 0-5 years of age:
- Parent Education: educate about importance of movement and guide them in activities to promote play skills and strength.
- Facilitating developmental milestones (such as sitting, crawling, standing and walking at the right time)
- Improving Muscle Tone
- Play Therapy[16]
- Physical Therapy from 6-17 years of age:
- Strengthening Programme
- Prevention of Scoliosis and Osteoporosis
- Gait training with balance and co-ordination training
- Aerobic Fitness programme
- Obesity Management
- Physical Therapy from 18+
- Aerobic fitness programme[17]
- Obesity Management
Physiotherapy Management in case of PWS has to go hand in hand with the occupational therapy and behavioural therapy to ensure long-term and lasting effects.
Physical Activity & PWS[7][edit | edit source]
- Promoting physical activity (PA) is an integral aim in the management of PWS.
- The benefits are improved physical function such as muscle strength, walking distance, and coordination.
- Supervised training programs are beneficial for children and adults with PWS. Guidance and support should be provided to families to facilitate their implementation in real-life settings.
Resources[edit | edit source]
Several resources are available for further information about PWS. A few of them are listed below:
- Guidelines for management of PWS by American Academy of Pediatrics.
- NHS UK guidelines.
- Mayo Clinic Guidelines.
- PWS in brief: The video below has been created by Osmosis.
References[edit | edit source]
- ↑ Prader A, Labhart A, Willi H. Ein syndrom von adipositas kleinwudis, kryptorchismus und oligophrenic nach myatonicartigem zustard im neugeborenenalter. Schweiz Med Wochenschr.1956; 86: 1260-1261.
- ↑ 2.0 2.1 Cassidy SB, Driscoll DJ. Prader-Willi syndrome. Eur J Hum Genet. 2009;17(1):3-13. doi: 10.1038/ejhg.2008.165
- ↑ Genetics Home Reference. Prader-Willi Syndrome.https://ghr.nlm.nih.gov/condition/prader-willi-syndrome
- ↑ de los Santos T, Schweizer J, Rees CA, Francke U. Small evolutionarily conserved RNA, resembling C/D box small nucleolar RNA, is transcribed from PWCR1, a novel imprinted gene in the Prader-Willi deletion region, which Is highly expressed in brain. Am J Hum Genet. 2000;67(5):1067-1082. doi:10.1086/303106
- ↑ 5.0 5.1 Holm VA, Cassidy SB, Butler MG, et al. Prader-Willi syndrome: consensus diagnostic criteria. Pediatrics. 1993;91(2):398-402.https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6714046/
- ↑ Eiholzer U, Meinhardt U, Rousson V, Petrovic N, Schlumpf M. Developmental profiles in young children with Prader–Labhart–Willi syndrome:effects of weight and therapy with growth hormone or coenzyme Q10. Am J Med Genet. 2008; 146: 873-880.
- ↑ 7.0 7.1 Bellicha A, Coupaye M, Mosbah H, Tauber M, Oppert JM, Poitou C. Physical Activity in Patients with Prader-Willi Syndrome—A Systematic Review of Observational and Interventional Studies. Journal of Clinical Medicine. 2021 Jan;10(11):2528.
- ↑ Glenn CC, Saitoh S, Jong MT, Filbrandt MM, Surti U, Driscoll DJ, Nicholl RD. Gene structure, DNA methylation and imprinted expression of the human SNRPN gene. Am J Hum Genet.1996;58(2):335–346. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1914536/
- ↑ Butler MG. High resolution chromosome analysis and fluorescence in situ hybridization in patient referred for Prader-Willi or Angelman syndrome. Am J Med Genet. 1995; 56(4):420–422. doi: 10.1002/ajmg.1320560414.
- ↑ Procter M, Chou LS, Tang W, Jama M, Mao R. Molecular diagnosis of Prader-Willi and Angelman syndroems by methylation specific melting analysis and methylation-specfic multiplex ligation-dependent probe amplification. Clin Chem. 2006;52(7):1276–1283. doi: 10.1373/clinchem.2006.067603.
- ↑ Gunay-Aygun M, Schwartz S, O'Riordan MA, Cassidy SB. The changing purpose of Prader-Willi syndrome clinical diagnostic criteria and proposed revised criteria. Pediatrics. 2001;108:E92.
- ↑ Driscoll DJ, Miller JL, Schwartz S, et al. "Prader-Willi Syndrome". . GeneReviews® U.S. National Library of Medicine, 1998 Oct 6. (Accessed 19 Sept 2020) Available from: https://www.ncbi.nlm.nih.gov/books/NBK1330/#
- ↑ Eiholzer U. A comprehensive team approach to the management of patient with Prader-Willi syndrome. J Pediatr Endocrinol Metab 2004; 17: 1153-1175.
- ↑ Elena G, Bruna C, Benedetta M, Stefania DC, Giuseppe C. Prader-willi syndrome: clinical aspects. J Obes. 2012;2012:473941. doi:10.1155/2012/473941
- ↑ Health Supervision for Children With Prader-Willi Syndrome The Committee on Genetics Pediatrics Jan 2011, 127 (1) 195-204; DOI: 10.1542/peds.2010-2820
- ↑ Rubin DA, Wilson KS, Wiersma LD, Weiss JW, Rose DJ. Rationale and design of active play @ home: a parent-led physical activity program for children with and without disability. BMC Pediatr. 2014 Feb ;14:41. doi: 10.1186/1471-2431-14-41.
- ↑ Silverthorn KH, Hornak JE. Beneficial effects of execise on aerobic capacity and body composition in adults with Prader-Willi syndrome. Am J Ment Retard. 1993; 97: 654-658.
- ↑ Osmosis. Prader-willi syndrome - causes, symptoms, diagnosis, treatment, pathology. Available from:https://www.youtube.com/watch?v=nYvm4Rsh7t8&ab_channel=Osmosis