Persistent Genital Arousal Disorder (PGAD)
Introduction[edit | edit source]
Persistent genital arousal disorder (PGAD), restless genital syndrome (ReGS), or genitopelvic dysesthesia (GD) is a rare disorder defined as a persistent, unpleasant, distressing sensation of unwanted, uncontrollable genital arousal, that happens in the absence of any arousal or sexual stimulus, does not resolve by orgasm or masturbation, may last for hours or days, and usually has a negative impact on individual's life. Symptoms may be triggered by sexual cues or non-sexual cues, or it may be idiopathic. Persistent genital arousal disorder (PGAD) was described for the first time in 2001 by Sandra Leiblum and Sharon Nathan[1]. It is related mainly to women but it was presented in men also[2].
Mechanism of Injury / Pathological Process[edit | edit source]
As it was described for the first time 20 years ago and it is difficult to know its prevalence there are limited studies about PGAD that are individual case studies till now there are not RCT or SR studies about PGAD on how to diagnose, assess, or treat.
There are different hypotheses for causes of PGAD that may be multifactorial; vascular factors, central and peripheral nervous system factors, pharmacological factors, psychosocial factors,' dietary, or even idiopathetic factors.
Pharmacological factors, it was reported in a few case report studies that drugs that contain serotonergic such as antidepressant medication (SSRIs /SNRIs) may induce or worsen PGAD symptoms [3]even at initiation or withdrawal of drug, however, there were cases in which there was a fundamental improvement of PGAD symptoms anticonvulsant or SNRI[4].
Nervous system factors, nerve roots compression at the level of cauda equina (roots of genitalia) this compression may be because of Tarlov cysts that cause cauda equina syndrome. In a study on an online support group for patients with PGAD(18) their MRI was collected, (12/18) there were Tarlov cysts[5]. Compression of the dorsal nerve of clitoris is another possible factor for PGAD[6].
Psychosocial factors, assessment of psychological factors of the patient is important for diagnoses of PGAD[7], maybe it is not the main factor but it may play a role in the development or maintenance of symptoms[1], history with sexual abuse is another possible cause.
Other factors; childbirth, falling, vehicle accidents, or sacroiliac joint dysfunction. In 2022, Zhang reported a case with PGAD symptoms after many visits to neurosurgeons, neurologists, gynecologists, and psychologists there was no symptoms relief, and with a physical exam there was SIJ dysfunction, and here symptoms were released after physical therapy sessions to restore joint alignment[8].
Clinical Presentation[edit | edit source]
- Uncontrollable genital arousal dos not affected by orgasm or masturbation.
- Symptoms may persist for hours or days in absence of sexual desire or objective stimulus.
- Pain or discomfort in the genitalia
- Tingling around the clitoris.
- Genital engorgement.
- Lubrication or discharges
- Throbbing response[10].
Diagnostic Procedures[edit | edit source]
Pelvic MRI in cases with suspected pudendal nerve entrapment.
Lumbosacral MRI for exclusion of cauda equina syndrome[11].
Management / Interventions[edit | edit source]
There is no guideline for PGAD/ GD and all we have to depend on case studies, the intervention for PGAD treatment needs the collaboration of a multidisciplinary team for diagnosis and treatment[12].
Pharmacological intervention[edit | edit source]
There was an improvement in PGAD symptoms with the intervention of antidepressant and anticonvulsant[4] and there was a successful treatment for female patients with leuprolide[13] that were case studies.
Neurolysis of dorsal nerve to clitoris[edit | edit source]
In cases with nerve compression, there was complete relief of symptoms after surgery and bilateral neurolysis had better outcomes than unilateral. The dorsal nerve to the clitoris is compressed mainly at the exit of the canal of Alcock and the site of compression can be detected during physical examination it will be tender and painful with palpation[14].
Physical Therapy[edit | edit source]
- Relaxation exercise and diaphragmatic breathing help to relax pelvic floor muscles[15], manual therapy and soft tissue mobilization[16].
- Electrotherapy for pain management (TENS, nerve neuromodulation)
- Advice for lifestyle modification, to participate in general body conditioning exercise program, yoga, advice for bowel and bladder habits, and stress management[15].
A case report study in 2010 demonstrated a 27 years old female 27 weeks pregnant, presented with PGAD symptoms she was evaluated and assessed to identify the underlying cause, during pelvic floor physical therapy examination there were multiple trigger points in obtrurator internus and hypertonicity of pelvic floor muscles. The patient has undergone for obtrurator internus soft tissue mobilization for about 15 minutes, and there was a completely relieve in symptoms 14 weeks later to this session[16].
Differential Diagnosis[edit | edit source]
Hypersexuality, unlike PGAD it is associated with a desire to have sex and was defined as the desire and urge to engage in sexual activity.
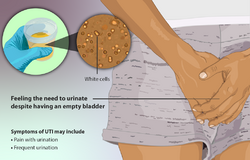
Urinary tract infection if there were symptoms like burning and itching.
Vulvodynia[17], persistent vulvar pain that is usually unexplained and may be caused by irritation to peripheral nerves around the vulva.
Penoscrotodynia[17], related to men and is similar to vulvodynia in women, is a skin-burning sensation in the genital area.
References[edit | edit source]
- ↑ 1.0 1.1 Jackowich RA, Pukall CF. Persistent genital arousal disorder: a biopsychosocial framework. Current Sexual Health Reports. 2020 Sep;12:127-35.
- ↑ Stevenson BJ, Köhler TS. First reported case of isolated persistent genital arousal disorder in a male. Case Reports in Urology. 2015 Feb 12;2015.
- ↑ Leiblum SR, Goldmeier D. Persistent genital arousal disorder in women: case reports of association with anti-depressant usage and withdrawal. Journal of Sex & Marital Therapy. 2008 Feb 21;34(2):150-9.
- ↑ 4.0 4.1 Kruger TH, Schippert C, Meyer B. The pharmacotherapy of persistent genital arousal disorder. Current Sexual Health Reports. 2020 Mar;12:34-9.
- ↑ Komisaruk BR, Lee HJ. Prevalence of sacral spinal (Tarlov) cysts in persistent genital arousal disorder. The Journal of Sexual Medicine. 2012 Aug;9(8):2047-56.
- ↑ Klifto KM, Dellon AL. Persistent genital arousal disorder: a review of pertinent peripheral nerves. Sexual Medicine Reviews. 2020 Apr 1;8(2):265-73. BibTeXEndNoteRefManRefWorks
- ↑ · Aswath M, Pandit LV, Kashyap K, Ramnath R. Persistent genital arousal disorder. Indian journal of psychological medicine. 2016 Jul;38(4):341-3.
- ↑ Zhang Y, Su L, Ge H, Wang Q. Persistent genital arousal disorder/genito-pelvic dysesthesia caused by sacroiliac joint dysfunction. Sexual Medicine. 2022 Oct 1;10(5):100544.
- ↑ Pelvic Rehabilitation Medicine. Persistent Genital Arousal Disorder PGAD | Causes, Symptoms, and Treatments | Pelvic Rehabilitation. Available from: http://www.youtube.com/watch?v=8hIAUeajssA [last accessed 30/3/2023]
- ↑ Deka K, Dua N, Kakoty M, Ahmed R. Persistent genital arousal disorder: Successful treatment with leuprolide (antiandrogen). Indian journal of psychiatry. 2015 Jul 1;57(3):326-8.
- ↑ Oaklander AL, Sharma S, Kessler K, Price BH. Persistent genital arousal disorder: a special sense neuropathy. Pain Reports. 2020 Jan;5(1).
- ↑ Martín-Vivar M, Villena-Moya A, Mestre-Bach G, Hurtado-Murillo F, Chiclana-Actis C. Treatments for Persistent Genital Arousal Disorder in Women: A Scoping Review. The Journal of Sexual Medicine. 2022 Jun;19(6):961-74.
- ↑ Deka K, Dua N, Kakoty M, Ahmed R. Persistent genital arousal disorder: Successful treatment with leuprolide (antiandrogen). Indian journal of psychiatry. 2015 Jul 1;57(3):326-8.
- ↑ Klifto K, Dellon AL. Persistent genital arousal disorder: Treatment by neurolysis of dorsal branch of the pudendal nerve. Microsurgery. 2020 Feb;40(2):160-6.
- ↑ 15.0 15.1 Jackowich RA, Mooney KM, Hecht E, Pukall CF. Online Pelvic Floor Group Education Program for Women With Persistent Genital Arousal Disorder/Genito-Pelvic Dysesthesia: Descriptive Feasibility Study. JMIR Formative Research. 2021 Jan 11;5(1):e22450.
- ↑ 16.0 16.1 Rosenbaum TY. Physical therapy treatment of persistent genital arousal disorder during pregnancy: A case report. The Journal of Sexual Medicine. 2010 Mar 1;7(3):1306-10.
- ↑ 17.0 17.1 Markos AR, Dinsmore W. Persistent genital arousal and restless genitalia: sexual dysfunction or subtype of vulvodynia?. International Journal of STD & Aids. 2013 Nov;24(11):852-8.