Peripheral Arterial Disease: Revascularization
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton
Introduction[edit | edit source]
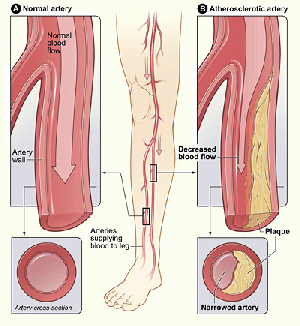
The prevalence of peripheral arterial disease (PAD) is increasing worldwide, with recent global estimates exceeding 200 million people. Advanced PAD leads to a decline in ambulatory function and diminished quality of life. In its most severe form, critical limb ischemia, rest pain, and tissue necrosis are associated with high rates of limb loss, morbidity, and mortality. Revascularization of the limb plays a central role in the management of symptomatic PAD. when lifestyle changes and medicines do not work. With advances during the last 20 years, there has been an ongoing evolution of revascularization options. These include:
- Ecdarterectomy: direct removal of obstructive plaque.
- Endovascular surgery: Angioplasty/Stenting When lifestyle changes and medicines do not work, then the doctor may go on to conduit Angioplasty to widen the blocked artery and ensure more blood flow. The surgeon may place a stent, or small mesh tube, in there to keep it open.
- Surgery (Bypass with vein or graft): Bypass surgery can also be performed to give blood a different path around the blocked artery.
- Hybrid: bypass and angioplasty or stenting.[1]
Revasculisation[edit | edit source]
Patient-specific factors are critical in selecting the most efficacious and durable outcome, with particular importance placed on comorbid conditions, estimated life expectancy, functional status, pattern of disease, and availability of conduit.[2]
Endarterectomy[edit | edit source]
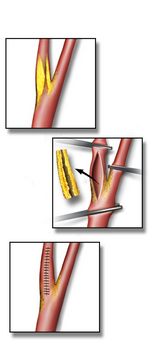
Endarterectomy is the direct removal of obstructive plaque from an arterial segment and it is best applied for focal lesions in large caliber vessels, particularly at bifurcations (eg, carotid, aortoiliac, common femoral arteries)
- Advantages: autogenous nature without need for conduit.
- Limitations: relate to adequate securing of the end points, thrombogenicity of the resulting surface in low flow environments, and the subsequent healing response of the artery (intimal hyperplasia), which may lead to recurrent stenosis[2].
Image: CarotidEndarterectomy
Angioplasty and Stenting[edit | edit source]
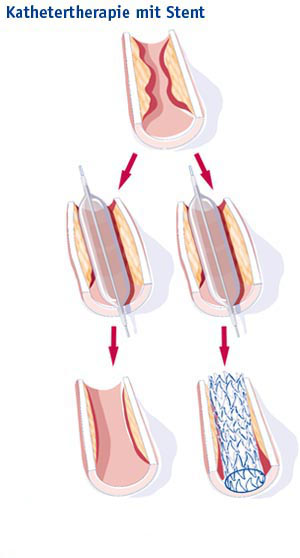
- Angioplasty is a procedure to open narrowed or blocked blood vessels. Angioplasty uses a medical "balloon" to widen blocked arteries. The balloon presses against the inside wall of the artery to open the space and improve blood flow. A metal stent is often placed across the artery wall to keep the artery from narrowing again[3].
- A stent is a small tube that keeps the artery open. Stents are made of either metal or plastic. Stent grafts are larger stents used for larger arteries. They may be made of a specialized fabric. Stents can also be coated with medication to help keep a blocked artery from closing[4].
Image: PAD therapy with stenting
Bypass[edit | edit source]
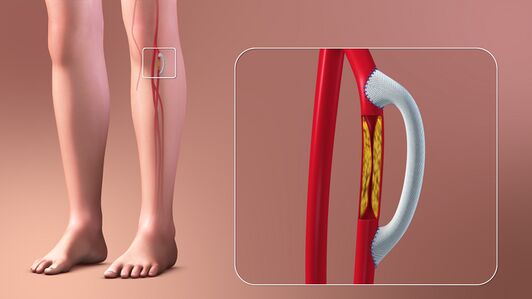
Surgical bypass is a versatile and flexible tool allowing for revascularization across a broad range of disease patterns, from the aorta down to the foot.
Image: 3D Medical Animation still shot depicting the Vascular Bypass Grafting in legs
- The large caliber arteries and the high-flow environment of aortoiliac reconstructions favor prosthetic grafts for reconstruction. Both Dacron and PTFE have excellent long-term results. Modern fabrication practices with either collagen or gelatin-impregnated Dacron or PTFE have resulted in synthetic materials that have minimal blood loss through the graft, excellent long-term structural integrity, and ability to incorporate into native tissues.
- In contrast, small caliber conduits typically required for infrainguinal bypass (≤6 mm) face a more demanding hemodynamic environment for patency. The ideal bypass conduit is an arterial autograft. For infrainguinal reconstructions, autologous vein is well established as the optimal conduit. The quality of the vein is the single greatest determinant of long-term outcomes of lower extremity bypass.
The limitations of prosthetic conduits in these environments relate to the potential for infection (an infrequent, although highly morbid complication), anastomotic pseudoaneurysms, and thrombosis.
Hybrid Approach[edit | edit source]
As endovascular interventions evolve, vascular surgeons are increasingly using hybrid approaches, a combination of catheter-based and open techniques to achieve limb revascularization with less invasiveness. eg open common femoral endarterectomy with concomitant angioplasty and stenting of aortoiliac disease.[2]
Physiotherapy[edit | edit source]
Supervised exercise programs have been recommended as first-line therapy for treatment of claudication and still as important post surgery.
Exercise therapy involves walking until reaching pain tolerance, stopping for a brief rest, and walking again as soon as the pain resolves. These walking sessions should last 30 to 45 minutes, 3 to 4 times per week for at least 12 weeks[5]
Recent evidence demonstrates benefits of exercise training even among those patients with PAD who do not have claudication.
Goals:
- Reduce limb symptoms
- Improve exercise capacity and prevent or lessen physical disability
- Decrease the occurrence of cardiovascular events[6].
See also physiotherapy section peripheral arterial disease (PAD)
References[edit | edit source]
- ↑ Lybrate Revascularization In PAD - All You Should Know! Available: https://www.lybrate.com/topic/revascularization-in-pad-all-you-should-know/93e1546a8a9f5584604a0052ed01d8ac (accessed 28.9.2021)
- ↑ 2.0 2.1 2.2 Vartanian SM, Conte MS. Surgical intervention for peripheral arterial disease. Circulation research. 2015 Apr 24;116(9):1614-28.Available:https://www.ahajournals.org/doi/full/10.1161/circresaha.116.303504 (accessed 28.9.2021)
- ↑ medlineplus Angioplasty and stent placement - peripheral arteries Available: https://medlineplus.gov/ency/article/007393.htm (accessed 29.9.2021)
- ↑ Healthline Stents Available: https://www.healthline.com/health/stent (accessed29.9.2021)
- ↑ Zemaitis MR, Boll JM, Dreyer MA. Peripheral arterial disease. StatPearls [Internet]. 2020 Jul 6.Available :https://www.ncbi.nlm.nih.gov/books/NBK430745/(accessed 29.9.2021)
- ↑ Hamburg NM, Balady GJ. Exercise rehabilitation in peripheral artery disease: functional impact and mechanisms of benefits. Circulation. 2011 Jan 4;123(1):87-97.Available:https://www.ahajournals.org/doi/full/10.1161/circulationaha.109.881888 (accessed 28.9.2021)