Parkinson's - Physiotherapy Management and Interventions
Original Editor - Bhanu Ramaswamy as part of the APPDE Project
Top Contributors - Laura Ritchie, Kim Jackson, Wendy Walker, Mariam Hashem, Vidya Acharya, Ewa Jaraczewska, Rachael Lowe, Tony Lowe, Evan Thomas, Tarina van der Stockt, Lauren Lopez, Lenaertz Kiara, Admin, Stacy Schiurring, Oyemi Sillo, Naomi O'Reilly, WikiSysop, Simisola Ajeyalemi, Claire Knott and Lucinda hampton
Introduction[edit | edit source]
A person with Parkinson’s may be experiencing several symptoms at the same time; your history taking and physical assessment should elicit the main issue (s) to prioritise as part of the management strategy. Whilst physiotherapy concentrates on the physical manifestations of a disorder, don’t forget to pay attention to how their other symptoms impact on the person’s lifestyle.
Remember also that optimal outcome is achieved through the collaboration with others from a team of health and social care professionals with expertise in other domains of Parkinson’s, from volunteers, family and friends.
Aims of Physiotherapy[edit | edit source]
- Maintain and improve levels of function and independence, which will help to improve a person’s quality of life
- Use exercise and movement strategies to improve mobility
- Correct and improve abnormal movement patterns and posture, where possible
- Maximize muscle strength and joint flexibility
- Correct and improve posture and balance, and minimise risks of falls
- Maintain a good breathing pattern and effective cough
- Educate the person with Parkinson’s and their carer or family members
- Enhance the effects of drug therapy
Physiotherapy Intervention[edit | edit source]
The Review version of the European Physiotherapy Guideline divides physiotherapy intervention for Parkinson’s into exercise and movement strategy training.
Exercise[edit | edit source]
Exercise has been proven to maintain health and well-being in Parkinson’s and now importantly it is shown to play a big role in addressing secondary prevention (focusing on strength, endurance, flexibility, functional practice and balance). Exercise for neuroprotection focuses on endurance and uses motor learning principles approaches, such as mental imagery and dual task training. Neuroprotection training, to be effective, should be introduced in the early stages, but helps at all stages. It involves complex, powerful and intensive exercises.
Exercise undertaken in a group setting has the added value of providing a social connection to those becoming increasingly isolated as the condition progresses, or for those who are newly diagnosed, so they can see the benefits of maintaining exercise and activity. A group environment also permits time for people to ask questions and discuss their symptoms and own management strategies with one another.
Transition Care setting[1] improves the independence and functioning of the patients in order to delay their entry into residential aged care. provides time-limited, goal-oriented and therapy-focused packages of services to older people after a hospital stay which includes low-intensity therapy—such as physiotherapy and occupational therapy—social work and nursing support or personal care. A qualitative research study[2] suggests better outcomes in older patients (above 80yrs) with family participation to assist physiotherapy care in a Transition care setting.
| [3] |
Physical activity, in particular, aerobic exercise might slow down the motor skill degeneration and depression. Furthermore, it increases the quality of life of patients with Parkinson's.[4] A randomized controlled trial showed favorable outcomes with exercise and horticultural intervention programs for older adults with depression and memory problems[5].
Randomized controlled clinical trial protocol to evaluate the effect of inspiratory muscle training on lung functions in patients with mild-to-moderate Parkinson's suggests a better outcome.[6]
Quality of life may be increased when performing strength training against an external resistance (cycle ergometer, weight machines, therapeutic putty, elastic and, weight cuffs ...). This also improves physical parameters, such as balance, gait parameters, physical performance but the muscle strength does not improve necessarily. [7]
Executing a dual task, e.g. talking while walking, is commonly difficult in patients with Parkinson's. Training this with Motor-Cognitive Dual-Task training, improves dual-task ability and might improve gait, balance and cognition. [8]
A recent research study found out Progressive resistance training (PRT) to be effective in decreasing bradykinesia and improving functional performance in patients with mild-to-moderate Parkinson's Disease (PD)[9].
Movement Strategy Training[edit | edit source]
Basal ganglia disorders cause deficits in the generation of internal (automatic) behavior. Strategies (physical or attentional cues and combined strategies) can help overcome some of the resultant problems, hence have become an increasingly utilised method of intervention for people with Parkinson’s.
Music-based movement therapy is a promising intervention that needs some further research. It is interesting since it combines cognitive movement strategies, cueing techniques, balance exercises and physical activity. The focus is on enjoying moving and not on the mobility limitation which might appeal more to the patients than standard exercises.[10]
We can see immediately the effects of external cueing and attention on improving step length, freezing and turning during walking tasks, and in activities of daily living. A Systematic Review and Meta-Analyses suggests better outcomes with short-term physiotherapy on the symptoms of freezing of gait in Parkison's patient. However, further randomized control trial studies are still needed[11]. Literature suggests that robot-assisted gait technology has better results in addressing the freezing of gait for Parkinson's patients. However, more research is needed in this field[12].
Depending on the cognitive state of the individual, they may be able to learn how to self-instruct in the use of an internal cue or strategy. If less able, the cue or strategy has to come from an external source e.g. a visual strip on the ground, the rhythmic beat of a metronome.
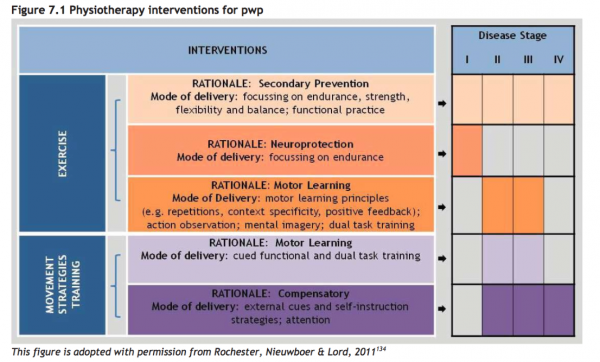
Depending on the stage of the condition, the rationale for intervention choices will differ:
This figure has been copied with permission of Rochester L, Nieuwboer A, Lord S [13].
As mentioned in the subsection on Physiotherapy for Parkinson’s: referral and assessment, during the earlier stages of diagnosis, greater emphasis is placed on education and self-management. The individual should be encouraged to continue being active and participate in physical exercise for as long as possible. Significant respiratory complications develop in many people as their Parkinson’s progresses, so attention should be paid to monitor and manage encroaching weakness of respiratory muscles and rigidity of the thoracic cage.
The European Guideline provides a section that describes the use of motor learning (pages 78 to 80), expectations if practiced and executed as a strategy to train improvements in movement. It takes the form of cued functional and dual task training, compensatory strategy training uses external cues, self-instruction and attention. Examples include:
- Visual cueing – a focus point to step over and initiate gait; strips of tape on the floor to initiate or continue walking through areas that cause slowing or freezing
- Auditory cueing – counting 1-2-3 to initiate walking; stepping to the beat of a metronome or specific music at a specified cadence to continue the rhythm of a walk
- Attention – Thinking about taking a big step; making a wider arc turn. This is applicable in case of correcting a bad habit- such as walking with stiff hip or hip hiking.
- Proprioceptive cueing – rocking from side to side ready to initiate a step; taking one step backwards as a cue ready to then walk forwards
A Systematic Review of thirty-five studies by Delgado-Alvarado M et al. emphasizes the benefit of non-pharmacological and nonsurgical treatments for freezing of gait symptoms. The study results suggest passive therapies (transcranial magnetic stimulation or transcranial direct current stimulation), active therapies (cognitive or physical training), and the transient effect therapies (using visual, auditory, or proprioceptive cues to shift the patient's habitual movements to a goal-directed one) help to overcome the freezing of gait episode[14].
Most people who are diagnosed with Parkinson’s are aged 50 or over, but 1 in 20 of those diagnosed are younger than this. Those with young onset of Parkinson’s are more likely to exhibit early dystonia and motor fluctuations and dyskinesias, caused by prolonged use of dopaminergic treatment.
These non-pharmalogical interventions are effective in increasing the Health-Related quality of life (HRQOL) according to Lee's meta-analysis. But since there is a big heterogenity between the interventions, more research is needed to take firm conclusions.[15]
To deliver a patient-centered treatment, it's important to provide your patients with information and education and allow time for patients to discuss their options and ask questions. Limited clinical time may be a challenge, however, good communication and sharing information are as important as delivering an intervention.
Complimentary Technology[edit | edit source]
Using virtual reality in rehabilitation has positive outcomes on balance, co-ordination and gait speed in Parkinson's patients[16]
Example of a man using visual cues to improve his walking.
| [17] |
The phenomena of using blue tints for dyskinesia
| [18] |
Using GaitAid
| [19] |
| [20] | [21] | [22] |
| [23] | [24] | [25] |
| [26] | [27] | [28] |
Related pages[edit | edit source]
- Parkinson's
- Parkinson's - Clinical Presentation
- Parkinson's - Anatomy, Pathology, Prognosis and Diagnosis
- Parkinson's - Physiotherapy Referral and Assessment
- Key Evidence and resources
References[edit | edit source]
- ↑ Transition Care Programme. Aging and aged care. Accessed from ☀https://agedcare.health.gov.au/programs-services/flexible-care/transition-care-programme on 4\12\19
- ↑ Lawler K, Taylor NF, Shields N. Family-assisted therapy empowered families of older people transitioning from hospital to the community: a qualitative study. Journal of physiotherapy. 2019 Jun 13.
- ↑ National Parkinson Foundation. Ask the Helpline: Why is Exercise Important for People with Parkinson's?. Available from: http://www.youtube.com/watch?v=e7dmw4Wuhzs [last accessed 24/09/16] (LoE)
- ↑ Wu, P.L., Lee, M., & Huang, T.T. Effectiveness of physical activity on patients with depression and Parkinson's: a systematic review. PloS one, 2017:12(7), eo181515.
- ↑ Makizako H, Tsutsumimoto K, Makino K, Nakakubo S, Liu-Ambrose T, Shimada H. Exercise and Horticultural Programs for Older Adults with Depressive Symptoms and Memory Problems: A Randomized Controlled Trial. Journal of Clinical Medicine. 2020 Jan;9(1):99.
- ↑ Montero Ferro A, P. Basso‐Vanelli R, Moreira Mello RL, Sanches Garcia‐Araujo A, Gonçalves Mendes R, Costa D, Gianlorenço AC. Effects of inspiratory muscle training on respiratory muscle strength, lung function, functional capacity and cardiac autonomic function in Parkinson's disease: Randomized controlled clinical trial protocol. Physiotherapy Research International. 2019 May 14:e1777.
- ↑ Ramazzina, I., Bernazzoli, B.,& Costantino, C. Systematic review on strength training in Parkinson's: an unsolved question. Clinical interventions in aging, 2017;12, 619.
- ↑ Fritz, N.E., Cheek, F.M., & Nichols-Larsen, d.S. Motor-cognitive dual-task training in neurologic disorders: a systematic review. Journal of neurologic physical therapy: JNPT, 2015;39(3), 142.
- ↑ de Moraes Filho AV, Chaves SN, Martins WR, Tolentino GP, Homem RD, de Farias GL, Fischer BL, Oliveira JA, Pereira SK, Vidal SE, Mota MR. Progressive Resistance Training Improves Bradykinesia, Motor Symptoms and Functional Performance in Patients with Parkinson’s Disease. Clinical Interventions in Aging. 2020;15:87.
- ↑ de Dreu, M. J., Van Der Wilk, A. S; d;, Poppe, E., Kwakkel, G., & van Wegen, E. E. Rehabilitation, exercise therapy and music in patients with Parkinson's: a meta-analysis of the effects of music-based movement therapy on walking ability, balance and quality of life. Parkinsonism & related disorders,2012; 18, S114-S119.
- ↑ Cosentino C, Baccini M, Putzolu M, Ristori D, Avanzino L, Pelosin E. Effectiveness of Physiotherapy on Freezing of Gait in Parkinson's Disease: A Systematic Review and Meta‐Analyses. Movement Disorders. 2019 Dec 4.
- ↑ Alwardat M, Etoom M. Effectiveness of robot-assisted gait training on freezing of gait in people with Parkinson disease: evidence from a literature review. Journal of exercise rehabilitation. 2019 Apr;15(2):187.
- ↑ Rochester L, Nieuwboer A, Lord S. Physiotherapy for Parkinson’s disease: Defining evidence within a framework for intervention. Neurodegen Dis Man 2011; 1: 57 - 65
- ↑ Delgado‐Alvarado M, Marano M, Santurtún A, Urtiaga‐Gallano A, Tordesillas‐Gutierrez D, Infante J. Nonpharmacological, Nonsurgical Treatments for Freezing of Gait in Parkinson's Disease: A Systematic Review. Movement Disorders. 2019 Nov 26.
- ↑ Lee, J., Choi, M., & Yoo, Y. A Meta-analysis of nonpharmacological Interventions for People With Parkinson's. Clinical nursing research, 2017;26(5), 608-631.
- ↑ Triegaardt J, Han TS, Sada C, Sharma S, Sharma P. The role of virtual reality on outcomes in rehabilitation of Parkinson’s disease: meta-analysis and systematic review in 1031 participants. Neurological Sciences. 2019 Dec 6:1-8.
- ↑ Oxford Computer Consultants. Virtual Reality Glasses for people with Parkinson's (Paper Cues). Available from: http://www.youtube.com/watch?v=yKSJQ_f9cjM [last accessed 24/09/16] (LoE:5)
- ↑ RevZonenet. Dyskinesia and Blue Lenses - RevZone. Available from: http://www.youtube.com/watch?v=h3y13erwfxw [last accessed 24/09/16] (LoE:5)
- ↑ Amir Baram. Parkinson's Freezing improves walking with the GaitAid. Available from: http://www.youtube.com/watch?v=6XoHBqw8GnI [last accessed 24/09/16] (LoE:5)
- ↑ TouroInfirmary. LSVT Big & Loud Parkinson's Therapy at Touro Neuro Rehab Center. Available from: http://www.youtube.com/watch?v=9fUQ6jptaBY [last accessed 29/09/16]
- ↑ Advance Rehab Centre. LSVT Big. Available from: http://www.youtube.com/watch?v=3jPEtanYmI0 [last accessed 29/09/16]
- ↑ UStepWalker. The U-Step 2 Walker, a Parkinson's Therapy Aid. Available from: http://www.youtube.com/watch?v=mirtZhHJSB4 [last accessed 29/09/16]
- ↑ Parkinson's Dance: People with Parkinson's can;t do that..can they? Available from: http://www.youtube.com/watch?v=pL_LZgAEsnM [last accessed 29/09/16]
- ↑ SusieG5678. Dancing Feet Help Defeat Parkinson's. Available from: http://www.youtube.com/watch?v=koaA1T0MynM [last accessed 29/09/16]
- ↑ Tom Anthony. Dancing helps Parkinson's Patients. Available from: http://www.youtube.com/watch?v=UEAaWPHDRbk [last accessed 29/09/16]
- ↑ 205beers. Exercise program for Parkinson disease. Available from: http://www.youtube.com/watch?v=YEiupqJDugA [last accessed 29/09/16]
- ↑ captainpat. Parkinson's - Vigorous Exercise. Neil Sligar June 2011. Available from: http://www.youtube.com/watch?v=R_-nRQmO8ko [last accessed 29/09/16]
- ↑ Polestar Pilates. Polestar Pilates for Parkinson's Patients. Available from: http://www.youtube.com/watch?v=yWBn0Ozt2fU [last accessed 29/09/16]