Orthotics in Cerebral Palsy
Original Editor - Scott Buxton
Top Contributors - Kim Jackson, Asma Alshehri, Lucinda hampton, Naomi O'Reilly, Rucha Gadgil, Admin, Simisola Ajeyalemi, Scott Buxton, Amrita Patro, Samuel Winter, Jess Bell, Olajumoke Ogunleye, Carin Hunter and George PruddenIntroduction[edit | edit source]
An orthosis by definition, is "an externally applied device used to modify the structural and functional characteristics of the neuromuscular and skeletal system"[1].
Why are the interdisciplinary team members convinced to use the orthoses as part of the treatment plan?
Because of the comprehensive understanding of the Cerebral Palsy(CP) patients, concentrating on the function limitations has a great effect on the new range of improved designs of orthoses to improve the outcome for the benefit of the patient.
In 1994 during the consensus conference held in Duke University, ISPO (International Society for Prosthetics and Orthotics) identified the goals of the lower limb orthotic management of CP. The identified goals can also be applied in postural impairments of the trunk and upper limbs[2]. The identified goals were:
- To correct and/or prevent deformity
- To provide a base of support
- To facilitate training in skills
- To improve the efficiency of gait
It is important that the interdisciplinary team check the patient’s functional limitations according to the GMFCS in order to plan the treatment. The type and design of the orthosis is decided accordingly and can be changed periodically depending on the improvement of the patient condition.
Types of Orthotics[edit | edit source]
Under the International Standard terminology, orthoses are classified by an acronym describing the anatomical joints which they contain. For example, an ankle foot orthosis ('AFO') is applied to the foot and ankle, a thoracolumbosacral orthosis ('TLSO') affects the thoracic, lumbar and sacral regions of the spine. It is also useful to describe the function of the orthosis.
Types of orthoses which can be used for individuals with Cerebral Palsy are shown in the short video below then described in greater detail in the text that follows.
Orthotics described in this page:
Lower Limb
- Foot Orthoses
- Supramalleolar Orthosis
- Ankle foot Orthoses (Dynamic, solid, posterior leaf spring, ground reaction, hinged)
- Knee Orthoses (Immobilisers, plastic knee ankle orthoses)
- Hip abduction orthoses
Spinal Orthoses (Thoraco-Lumbar-Pelvic Brace)
Upper Limb (Resting Hand and Wrist Splint)
Lower Limb Orthotic Designs[edit | edit source]
Lower limb orthotics are a vital component of orthotic rehabilitation for individuals with various conditions, including cerebral palsy. These orthotic devices are specifically designed to support, align, and improve the function of the lower extremities. They play a crucial role in addressing a wide range of issues, such as foot deformities, gait abnormalities, muscle weakness, and joint instability. By providing external support and optimising biomechanics, lower limb orthotics aim to enhance mobility, promote efficient movement patterns, and improve overall quality of life for individuals with cerebral palsy.
Foot Orthoses (FO)[edit | edit source]
Foot orthotics do not prevent deformity. They provide a better contact of the sole of the foot with the ground. Foot orthoses are commonly prescribed to correct alignment issues and provide support for the foot.
Foot orthoses help improve foot stability, correct excessive pronation or supination, and promote optimal foot alignment. By providing support and redistributing pressures, foot orthoses enhance balance and reduce the risk of falls. They can also improve foot function during the stance phase of gait by optimising weight-bearing and promoting efficient movement patterns.
Supramalleolar Orthosis (SMO)[edit | edit source]
This orthosis extends to just above the malleoli and to the toes. Consider in mild dynamic equinus, varus and valgus instability. Supramalleolar orthoses are typically prescribed to address ankle and foot instability while allowing freedom of movement.
SMOs provide support to the ankle while allowing normal ankle motion. They enhance ankle stability and correct alignment issues, which can improve balance and prevent ankle sprains. SMOs primarily aid in the stance phase of gait by providing stability during weight-bearing activities.
University of California Biomechanics Laboratory Orthosis (UCBL): The medial side is higher than the lateral, holds the calcaneus more firmly, supports the longitudinal arch. Prescribed for hind and midfoot instability.
Ankle Foot Orthoses (AFO)[edit | edit source]
The AFO is the basic orthosis in CP and is a crucial piece of equipment for many children with spastic diplegia. The main function of the AFO is to maintain the foot in a plantigrade position. This provides a stable base of support that facilitates the function and also reduces tone in the stance phase of the gait.
AFOs improve ankle stability, correct foot alignment, and facilitate a more functional gait pattern. For individuals with foot drop, AFOs help prevent the foot from dragging during the swing phase of gait. They provide ankle support during the stance phase, improving balance and preventing ankle sprains. AFOs can also correct equinus deformity (toe walking) and promote a smoother, more energy-efficient gait. There are various types of the AFO.
Dynamic AFO (DAFO)[edit | edit source]
Dynamic AFOs are commonly prescribed for individuals with weak or spastic muscles, who require assistance with foot clearance during the swing phase.
Dynamic AFOs incorporate a hinge mechanism that allows controlled movement during specific phases of gait. They assist with foot clearance during swing phase by providing dorsiflexion assistance, helping individuals clear their toes and prevent tripping.
Solid AFO [edit | edit source]
Solid AFOs are prescribed to provide maximum stability and control for individuals with significant muscle weakness or joint instability.
The solid or rigid AFO allows no ankle motion, it covers the back of the leg completely and extends from just below the fibular head to metatarsal heads. The solid AFO enables heel strike in the stance phase and toe clearance in the swing phase. It can improve knee stability in ambulatory children. It also provides control of varus/ valgus deformity.
Benefits and Function: Solid AFOs offer rigid support to stabilise the ankle and foot. They correct alignment issues, improve balance, and provide substantial control during weight-bearing activities. Solid AFOs can improve stability during stance phase, preventing ankle collapse and offering a secure base of support for walking.
Solid AFOs provides ankle stability in the standing frame in non-ambulatory children.
Posterior Leaf Spring AFO (PLSO)[edit | edit source]
A Posterior Leaf Spring AFO is a rigid AFO trimmed behind the malleoli’s to provide flexibility at the ankle and allows passive ankle dorsiflexion during the stance phase. A PLSO provides smoother knee-ankle motion during walking while preventing excessive ankle dorsiflexion Varus-valgus control is also poor because it is repeatedly deformed during weight bearing. A PLSO is an ideal choice in mild spastic equinus. Do not use it with patients who have crouch gait and pes valgus.
Posterior leaf spring AFOs help facilitate toe clearance during the swing phase by providing a gentle plantarflexion moment at the ankle. They assist with foot clearance, allowing for a smoother, more natural gait pattern. By addressing foot drop, these AFOs contribute to improved balance and reduced tripping risk.
Ground Reaction AFO (GRAFO)[edit | edit source]
This AFO is made with a solid ankle, the upper portion wraps around the anterior part of the tibia proximally with a solid front over the tibia. The rigid front provide strong ground reaction support for patients with weak triceps surae. The foot plate extends to the toes. The ankle may be set in slight plantar flexion of (2-3 degrees) if more corrective force at the knee is necessary. Use the GRAFO in patients with quadriceps weakness or crouch gait. It is an excellent brace for patients with weak triceps surae following hamstring lengthening. Children with static or dynamic knee flexion contractures (more than 15 degrees) do not get benefit out of it and do not tolerate the GRAFO.
Ground reaction AFOs are prescribed for individuals with weak lower leg muscles, instability, or excessive knee flexion during stance. Ground reaction AFOs use a design that applies forces to the lower limb during walking, specifically at the ankle and knee joints. They provide stability, enhance knee extension during stance, and prevent excessive knee flexion or collapse. These AFOs improve overall balance, enhance stability during weight-bearing, and promote a more efficient gait pattern.
Anti-Recurvatum AFO[edit | edit source]
This special AFO is molded in slight dorsiflexion or has the heel built up slightly to push the tibia forward to prevent hyperextension during stance phase. Anti recurvatum AFOs are prescribed for individuals with hyperextension of the knee during stance phase.
Anti recurvatum AFOs limit knee hyperextension by providing a posterior stop. They improve knee stability, prevent excessive backward bending of the knee, and enhance weight-bearing distribution. These AFOs promote a more controlled and balanced gait by limiting knee hyperextension during the stance phase.
Hinged AFO[edit | edit source]
Hinged AFOs are prescribed for individuals with complex foot and ankle problems, such as severe ankle instability or significant muscle weakness.. They have a mechanical ankle joint usually preventing plantar flexion, but allowing relatively full dorsiflexion during the stance phase of gait. They provide a more normal gait because they permit dorsiflexion in stance phase of the gait, thus making it easier to walk on uneven surfaces and stairs. This is the best AFO for most ambulatory patients. Adjust the plantar flexion stop in (3- 7 degrees) dorsiflexion to control knee hyperextension in stance in children with genu recurvatum. The hinged AFO is contraindicated in children who do not have passive dorsiflexion of the ankle because it may force the midfoot joints into dorsiflexion and cause midfoot break deformity. Knee flexion contractures and triceps weakness are other contraindications where a hinged AFO may increase crouch gait. The AFO may be fitted with a hinge that allows 10 degrees passive dorsiflexion while preventing plantar flexion. This creates a more natural gait.
Hinged AFOs offer adjustability and customizability to address specific foot and ankle issues. They provide stability, correct alignment, and enhance foot and ankle control. Hinged AFOs improve balance, reduce the risk of falls, and facilitate a more functional gait pattern by supporting and aligning the lower limb throughout the gait cycle.
Knee Orthoses[edit | edit source]
Knee orthoses are used as resting splints in the early postoperative period and during therapeutic ambulation. There are two types of knee orthoses, the knee immobilizer and the plastic knee-ankle foot orthosis (KAFO). The use of such splints protects the knee joint, prevents deformity recurrence after multilevel lengthening and enables a safer start to weight bearing and ambulation after surgery.
Knee Immobilisers[edit | edit source]
Knee immobilisers are made of soft elastic material and hold only the knee joint in extension, leaving the ankle joint free. Consider using them in the early postoperative period after hamstring surgery and rectus tendon transfers.
Plastic KAFOs[edit | edit source]
Plastic resting KAFOs extend from below the hips to the toes and stabilise the ankle joint as well as the knee. They are more rigid and provide better support to the ankle and the knee in the early postoperative phase. Knee-ankle-foot orthoses with metal uprights and hinged joints (KAFOs) were developed and used extensively in the 1950s and 60s for children with poliomyelitis[4]. Though KAFOs are still used for ambulation in poliomyelitis and myelomeningocele where there is a need to lock the knee joint, they are not useful for the child with CP because they disturb the gait pattern by locking the knee in extension in the swing phase. Donning the KAFO on and off takes a lot of time and they are difficult to wear. For these reasons, KAFOs for functional ambulation have disappeared from use in children with CP. Instead, anti recurvatum AFOs or GRAFOs for knee problems in ambulatory children have proved useful.
Use the plastic KAFO at night and in the early postoperative period after multi-level surgery to protect the extremity while allowing early mobilisation.
Hip Abduction Orthoses[edit | edit source]
Consider using hip abduction orthoses in children with hip adductor tightness to protect hip range of motion and prevent the development of subluxation. One clear indication for hip abduction orthoses is the early period after adductor lengthening.
Spinal Orthotics[edit | edit source]
There are various types of braces used for spinal deformity. This braces are not prescribed in order to stop the progression of scoliosis but to provide better sitting balance. As most children with scoliosis need spinal surgery to establish and maintain sitting balance in the long run. A thoraco-lumbo-sacral brace helps the child to sit better during the growth spurt period when spinal deformity becomes apparent, progresses fast and the child out grows custom molded seating devices quickly. Children who are not candidates for surgery for different reasons may use spinal braces instead of seating devices for better sitting.
Upper Limb Orthotics[edit | edit source]
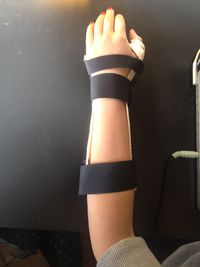
The indications of bracing in the shoulder and elbow are very limited. An example of a resting splint is a thermoplastic resting wrist and hand splint which keeps the wrist in 10-20 degrees extension, the metacarpal phalangeal joint(MPJ) in 60 degrees flexion and the interphalangeal joint (IPJ) in extension ( see figure on R). This type of splint is used at night and during periods of inactivity with the hope of preventing deformity. An example of a functional splint is an opponents splint, which can be used in everyday activities. Hand orthoses may inhibit the active use of the extremity and effect sensation of the hand in a negative way. Use them only in the therapy setting or at school and take them off during other times in the day.
These are the most known type of orthoses used in one stage of the Cerebral Palsy Treatment Plan, bearing in mind with Cerebral Palsy a periodical orthosis assessment has to be done in order to decide if there is a need for changing the design or type.
Care of Orthosis[edit | edit source]
It is important that the orthosis is in good working order and shows minimal signs of wear and tear. Check that components are in good condition and if hinged check they are functioning and locking if needed. Check the fit also and teach client in hygiene and care aspects of orthosis. See video below.
Orthotic Prescription[edit | edit source]
Lower Limb Orthoses for Ambulatory Children (GMFCS I, II and III)[edit | edit source]
Ambulatory children diagnosed with cerebral palsy, categorised under GMFCS levels I, II, and III, exhibit various degrees independent walking. Their mobility can be notably enhanced through the tailored application of lower limb orthotics. The strategic use of these devices not only optimises gait mechanics but also offers vital support for maintaining balance and minimising energy expenditure during ambulation. Ultimately, these measures serve to boost the child's functional abilities.[6]
Key concerns typically addressed by orthotics in ambulatory children within GMFCS levels I, II, and III include:
- Correct Alignment: Some children may experience lower limb alignment deviations, such as excessive foot pronation or supination, knee valgus or varus, or hip internal rotation during walking. Corrective orthotics are specifically designed to counter these deviations, fostering better alignment and promoting an optimal walking posture.[7] By improving alignment, orthotic devices enhance stability and reduce the risk of falls. This increased stability not only boosts the child's confidence whilst walking but also encourages more independent exploration of their environment.[8]
- Support Weak Muscles:Muscle weakness is a recurrent issue among children with cerebral palsy, potentially affecting their overall mobility and stability when walking.Orthotics provide the necessary support to compensate for this weakness, aiding in balance and movement control.[9]
- Improving Balance and Coordination: Maintaining balance and coordinating movements can pose significant challenges for children with cerebral palsy. Orthotics play a pivotal role in helping these children navigate their environments safely and confidently.[10]
- Improving Energy Efficiency: Orthotic devices can also help optimise energy use during walking, crucial for preventing fatigue and improving endurance. By mitigating excessive movements and compensatory patterns, orthotics can contribute to more energy-efficient gait.[11] By minimising unnecessary muscle effort and compensatory patterns, lower limb orthotics enhance the energy efficiency of the child's gait. This enables the child to walk for longer periods and participate in physical activities with less fatigue.[12]
Orthotics also contribute to a smoother, more natural gait. By rectifying alignment issues and addressing muscle imbalances, these devices assist with improving foot clearance during the swing phase of the gait cycle, facilitating better overall mobility.[13]
Through these benefits, orthotic interventions have emerged as an invaluable tool in the rehabilitation and support of children living with cerebral palsy, empowering them to lead a more independent and active life.[14]
Lower Limb Orthoses for Non-Ambulatory Children (Pre-standing and GMFCS IV and V)[edit | edit source]
Orthotic devices for children with cerebral palsy classified as pre-standing and within GMFCS levels IV and V are tailored to address specific functional needs, including alignment, stability during weight-bearing activities, and prevention of contractures and deformities.[7] These devices enhance comfort, optimise postural control, and support functional capabilities.[8]
- Hip Instabiliity: Hip instability is a common issue among children with cerebral palsy classified under GMFCS levels IV and V. To manage this, orthotic devices are used to enhance hip stability, provide support, and prevent the development of contractures or deformities.[ref] Orthoses can improve alignment, limit pain, reduce risk of hip dislocation, and optimise function and comfort. By doing so, they contribute to a better quality of life for these children.[ref]
- Ankle Foot Orthoses: Ankle Foot Orthoses (AFOs) are often recommended for children with cerebral palsy classified under GMFCS levels IV and V. They aid in foot positioning, improve stability, and prevent contractures.[9] AFOs can contribute to better alignment and stability, reduce muscle imbalances, and optimise gait. They can be specifically tailored to meet individual functional needs, promoting better mobility and comfort. [15]
- Spinal Orthoses:Children with cerebral palsy categorised under GMFCS levels IV and V can benefit from spinal orthoses, especially when experiencing spinal deformities or complications such as scoliosis. Spinal orthoses are used to improve spinal alignment and stability, and slow the progression of spinal deformities.[16] Spinal orthoses can improve alignment, provide support, and enhance comfort, thereby improving quality of life for children with cerebral palsy in these GMFCS categories.[17]
Orthotic Management[edit | edit source]
Lower Limb Transverse Plane and Coronal Plane Deformities[edit | edit source]
The identification of the primary cause of lower limb transverse and coronal plane deformities is imperative to selecting appropriate orthotic interventions.[6] A systematic review by Hudson et al. (2020) highlighted that orthoses can have a positive impact on gait parameters and can improve gross motor function, especially in children with spastic CP.[18] Evidence also suggests that orthotic management, as part of a comprehensive therapeutic intervention, can potentially decrease the progression of these deformities.[19]
Leg Length Discrepancies[edit | edit source]
Leg Length Discrepancies (LLDs) are frequently observed in children diagnosed with hemiplegia, owing to conditions such as Developmental Dysplasia of the Hip (DDH) and the uneven pressure exerted on limbs causing a decrease in bone growth. Resultantly, this can lead to pelvic obliquity and functional constraints like the reduced ability for contralateral hip adduction and ipsilateral hip abduction. An effective strategy to rectify this is the implementation of a shoe raise which can help realign the pelvis and improve functional capacity1.
Management of Torsional Deformities[edit | edit source]
Observations of gait patterns in children exhibiting torsional deformities often reveal an 'in-toeing' or 'scissor' gait. In such cases, a comprehensive evaluation of the lower limb's rotational profile is of paramount importance. This assessment allows the orthotist to distinguish between muscular or bony origins of the torsional deformity. Femoral and tibial rotational deformities along with any fixed muscle contracture are primarily surgical issues and are not usually managed with orthotics2.
Tuning of Ankle Foot Orthosis and Footwear (AFO-FC) Combination[edit | edit source]
Proper tuning of the AFO-FC is critical in maximising its positive impact on gait mechanics, particularly for children with CP. This fine-tuning process involves making detailed adjustments to the orthosis design to optimise its function during walking activities1.
The Role of Ground Reaction Force (GRF)[edit | edit source]
Effective gait requires precise muscular control to properly align the GRF with respect to the ankle, knee, and hip joints during the stance phase. For a child with CP, managing GRF can be challenging due to their compromised neuromuscular condition. That's where AFOs come into play, as they are designed to assist in controlling lower limb movements, thereby positively influencing gait kinetics and kinematics.
A common misconception is that achieving optimal knee extension during the stance phase requires a 90° positioning of the talo-cural joint. However, the key lies in maintaining an appropriate Shank to Vertical Angle (SVA), defined as the angle between the tibial shank and the vertical plane in the sagittal plane2.
In typically developed children and those with CP, the optimum SVA angle during mid-stance ranges between 7° to 15° of inclination, with an ideal target of 10° to 12°. Achieving this SVA permits the vertical progression of the pelvis and trunk, ensuring optimal alignment of the GRF with respect to the ankle, knee, and hip joints.
In the process, the parameters that are commonly adjusted include the heel's height, type and design, and the design and location of the rocker at the metatarsal heads. The design of the AFO and the type and stiffness of the material used for its construction all impact its effect on the child's gait3.
The goal of the tuning process is to ensure the AFO provides the necessary control at the foot and ankle during the stance phase. This helps resist undesirable dorsiflexion, often referred to as 'buckling', and allows for the GRF to be maintained in a desired position with respect to the knee and hip joints.
Moreover, heel height adjustments of as little as 3mm can cause angular changes in the SVA of up to 2°. Hence, minor adjustments can have a significant effect on gait characteristics4.
Although it is recommended that AFO-FC tuning becomes routine in clinical practice, time constraints and access to a gait laboratory for video vector gait analysis often pose challenges. However, the benefits of tuning, which include optimised biomechanical alignment and an enhanced gait, make it a worthwhile part of treatment plans for children with CP.
Benefits of using those orthoses for a child with CP[edit | edit source]
When an orthotic device is a successfully part of treatment, then it should help children establishing normal conditions of joint motion and muscle function as much as possible.
Orthotics can help remedy this situation by one or more of the following effects
- Providing a stable base of movement
- Improving the gait pattern
- Reducing the impact of spasticity on upper and lower limbs
- Creating a better environment in which a child can perform the exercises advised to him/her
- Reducing excessive energy used to move
- Reducing the potential of fall risk
- Controlling muscular imbalance
- Also, the child will have a stable bases for movement, where they would develop higher level of functioning including joints ROM, muscle strength, fitness and endurance, balance and control over spastic movement.[20]
References.[edit | edit source]
- ↑ Gale Encyclopedia of Medicine. Copyright 2008 The Gale Group, Inc.
- ↑ Report of a Consensus Conference on Lower Limb orthotic Management in Cerebral Palsy. International Society for Prosthetics and orthotics. 1994. https://www.ispoint.org/resource/resmgr/4_EXCHANGE/Conference_on_the_Lower_Limb.pdf
- ↑ Dr A. Elnahhas ORTHOTIC PRESCRIPTION FOR CEREBRAL PALSY Available from: https://www.youtube.com/watch?v=VxRfpd9srRk&app=desktop (last accessed 6.11.2019)
- ↑ Hachisuka K, Makino K, Wada F, Saeki S, Yashimoto N. Oxygen consumption, oxygen cost and physiological cost index in polio survivors: A comparison of walking without orthosis, with an ordinary or a carbon-fibre reinforced plastic knee-ankle-foot orthosis. J Rehabil Med 2007; 39: 646–650
- ↑ nhsggs NHSGGC - Orthotics Patient Information: Orthosis care and repair Available from: https://www.youtube.com/watch?v=GA_tnK-Oe-g (last accessed 6.11.2019)
- ↑ 6.0 6.1 Rodda J, Graham HK. Classification of gait patterns in spastic hemiplegia and spastic diplegia: a basis for a management algorithm. European journal of neurology. 2001 Nov;8:98-108.
- ↑ 7.0 7.1 Morris C. A review of the efficacy of lower-limb orthoses used for cerebral palsy. Developmental medicine and child neurology. 2002 Mar;44(3):205-11.
- ↑ 8.0 8.1 Rethlefsen S, Kay R, Dennis S, Forstein M, Tolo V. The effects of fixed and articulated ankle-foot orthoses on gait patterns in subjects with cerebral palsy. Journal of Pediatric Orthopaedics. 1999 Jul 1;19(4):470-4.
- ↑ 9.0 9.1 Buckon CE, Thomas SS, Jakobson-Huston S, Moor M, Sussman M, Aiona M. Comparison of three ankle–foot orthosis configurations for children with spastic diplegia. Developmental medicine and child neurology. 2004 Sep;46(9):590-8.
- ↑ Lam WK, Leong JC, Li YH, Hu Y, Lu WW. Biomechanical and electromyographic evaluation of ankle foot orthosis and dynamic ankle foot orthosis in spastic cerebral palsy. Gait & posture. 2005 Nov 1;22(3):189-97.
- ↑ Brehm MA, Harlaar J, Schwartz M. Effect of ankle-foot orthoses on walking efficiency and gait in children with cerebral palsy. Journal of rehabilitation medicine. 2008 Jul 1;40(7):529-34.
- ↑ Radtka SA, Skinner SR, Dixon DM, Johanson ME. A comparison of gait with solid, dynamic, and no ankle-foot orthoses in children with spastic cerebral palsy. Physical therapy. 1997 Apr 1;77(4):395-409.
- ↑ Rose GE, Lightbody KA, Ferguson RG, Walsh JC, Robb JE. Natural history of flexed knee gait in diplegic cerebral palsy evaluated by gait analysis in children who have not had surgery. Gait & posture. 2010 Mar 1;31(3):351-4.
- ↑ Kerkum YL, Buizer AI, Van Den Noort JC, Becher JG, Harlaar J, Brehm MA. The effects of varying ankle foot orthosis stiffness on gait in children with spastic cerebral palsy who walk with excessive knee flexion. PloS one. 2015 Nov 23;10(11):e0142878.
- ↑ Rodda JM, Graham HK, Carson L, Galea MP, Wolfe R. Sagittal gait patterns in spastic diplegia. The Journal of bone and joint surgery. British volume. 2004 Mar;86(2):251-8.
- ↑ Progression of scoliosis after skeletal maturity in institutionalized adults who have cerebral palsy.
- ↑ Miller A, Temple T, Miller F. Impact of orthoses on the rate of scoliosis progression in children with cerebral palsy. Journal of Pediatric Orthopaedics. 1996 May 1;16(3):332-5.
- ↑ Hudson D, Michalowski H, Miller F. Lower Extremity Orthoses for Children and Youth with Cerebral Palsy. Cerebral Palsy. 2020:2999-3021.
- ↑ Hägglund G, Lauge-Pedersen H, Wagner P. Characteristics of children with hip displacement in cerebral palsy. BMC musculoskeletal disorders. 2007 Dec;8:1-6.
- ↑ Orthotic Devices. www.cerebralpalsy.org/information/mobility/orthotics (accessed 11 Dec 2016)