Objective Vestibular Assessment
Top Contributors - Jess Bell, Kim Jackson, Rucha Gadgil and Robin Tacchetti
Introduction[edit | edit source]
As discussed here, the therapist needs to conduct a thorough subjective assessment of the vestibular patient in order to determine the nature and potential cause of his / her symptoms. The objective assessment must be equally thorough and include a range of tests, from oculomotor testing to dynamic visual acuity and gait / balance assessments. This page will discuss the key components of the objective assessment of the vestibular patient.
Objective Evaluation[edit | edit source]
Vision Screening[edit | edit source]
Oculomotor screen[edit | edit source]
When conducting any vision screening or testing, it is important to watch and ask the patient how must effort a task requires and the degree of symptoms provoked. The basic oculomotor screen during a vestibular assessment should include:[1]
- Fixation in primary and eccentric gaze
- Smooth pursuit or tracking
- Vestibulo-ocular reflex (VOR) cancellation
- Saccades
Oculomotor Testing[edit | edit source]
Spontaneous Nystagmus[edit | edit source]
Spontaneous nystagmus is tested in primary and eccentric gaze. It occurs due to the unopposed tonic neural activity of the intact side when there are lesions in the peripheral vestibular systems (acute) or central vestibular pathways.[1]
Primary gaze is tested as follows:[1]
- The patient looks forward and visually fixates on a target
- This position is held for 10 seconds and the therapist looks for any nystagmus
Eccentric gaze:[1]
The most common pathological type of nystagmus driven by the CNS is gaze evoked nystagmus (GEN). It is tested as follows:[1]
- The patient is asked to fixate on a position 30 degrees to each side, up and down (i.e. an eccentric position)
- Each position is held for 10 seconds and the therapist looks for nystagmus
- GEN is only present with eccentric gaze, not in primary gaze
It is important to differentiate between GEN and end point nystagmus. End point nystagmus occurs when gaze is held at the end of range. End point nystagmus is considered normal, so in order to test for GEN it is essential that the patient only holds his / her gaze 30 degrees off-centre.[1][2]
For a summary of the difference between peripheral and central nystagmus, please see Table 1.
| Findings | Peripheral | Central |
|---|---|---|
| Effect of fixation (room light) | Nystagmus is typically absent within 2 to 3 days in room light | Nystagmus either does not change or it increases |
| Direction of nystagmus | Usually mixed plane (horizontal and torsional) | Usually single plane (sustained down beating) |
| Effect of gaze | Nystagmus increases with gaze toward direction of quick phase | Nystagmus either does not change or it reverses direction |
Smooth Pursuit and VOR Cancellation[edit | edit source]
- Smooth pursuit movements are slow, tracking eye movements that maintain images of smaller moving targets (20 to 30 degrees per second) on the fovea[1][3]
- Centrally mediated reflex[1]
Smooth Pursuit Eye Movements[edit | edit source]
- Refixation saccades occur during target motion toward the side of the lesion
- There may be unilateral or bilateral refixation saccades[1]
VOR Cancellation[edit | edit source]
- Head and eyes move in unison with a target - suppressing the VOR
- Refixation saccades will occur during head movement toward the side of the lesion[1]
Smooth Pursuit Torsion Test[edit | edit source]
- The smooth pursuit neck torsion test measures smooth pursuit eye movement with the head / trunk in neutral and when the trunk and neck are rotated relative to a stationary head[5]
- Smooth pursuit neck torsion test is considered to be specific for detecting eye movement disturbances due to altered cervical sensory input[6][7]
- A decrease in velocity gain of smooth pursuit eye movements during the test is only seen in patients with neck pain[1]
Saccadic Eye Movements[edit | edit source]
Saccades are defined as: “fast conjugate eye movements that shift the eyes from one target to another, bringing an object of interest into focus on the fovea where visual acuity is highest”.[9]
Saccades are centrally mediated and there are volitional saccades and reflexive saccades.[10][11]
In order to test saccadic eye movements:[1]
- Instruct the patient to look from one target to the other as quickly as possible – vertical and horizontal
- During these fast changes in eye position, the therapist looks at the amplitude, velocity and accuracy of targeting
- Hypometric saccade = when the patient ‘undershoots’ the target
- Hypermetric saccade = when the patient ‘overshoots’ the target
One hypometric saccade is typically considered normal. Two or more hypometric or one or more hypermetric saccades is considered abnormal.[1]
Vestibulo-Ocular Reflex (VOR) Testing[edit | edit source]
The VOR is the primary mechanism for gaze stability during head movement. There are two tests of VOR function that can be done effectively in the clinic without an infrared camera system:[1]
- The head thrust test
- The dynamic visual acuity (DVA) test
The head shaking test can also be conducted, but it works better with an infrared camera system.[1]
Head Thrust Test[edit | edit source]
The head thrust test (HTT) is generally accepted as a useful clinical test for assessing the angular vestibulo-ocular reflex.[12] The test is performed as follows:[1][12]
- The patient is asked to focus on a target
- The therapist gently grasps the patient’s head and applies a small-amplitude, high-acceleration thrust
- It must be performed quickly
- The patient must not be able to predict on which side the thrust will be applied
- The therapist observes the patient’s eyes for corrective saccades once the head stops moving
- Refixation saccades indicate decreased VOR gain - i.e. a positive test
- The testing side is the side that the head is thrusted towards:[1]
- Positive head thrust on right side = right sided deficit
- Corrective saccades to right and left = bilateral deficit
Dynamic Visual Acuity[edit | edit source]
There are different ways to assess dynamic visual acuity (VOR), including the dynamic visual acuity (DVA) test. The DVA compares static visual acuity with dynamic visual acuity. A positive DVA test indicates the presence of oscillopsia or impaired gaze stability with head movement.[1]
Older Acuity Chart[edit | edit source]
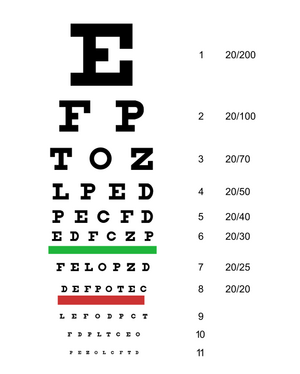
Utilises a 10 ft LogMar or Snellen chart (see Figure 1). There should be the same number of optotypes (i.e. letters) per line on the chart, but these charts do not have this feature.[1]
Current Acuity Chart[edit | edit source]
The current acuity chart does have the same number of optotypes on each line. A copy this chart can be found at i-see.org.
When using this chart, the patient’s distance from the chart can be varied. Each line on the acuity chart has a recommended distance.[1]
The test is conducted as follows:[1]
- Patient starts two feet away from the chart in a sitting position
- The patient’s head is tipped down into slight flexion
- The patient should wear glasses if required
- The patient reads the static visual acuity chart with his / her head still
- The following instruction is given:
- “Read the lowest line that is clear to you”
- The patient reads from left to right to the lowest line possible until she / he misses at least one optotype on a line
- The line above this (i.e. where no optotypes were missed) is the static visual acuity line
- Then, the therapist silently chooses a line that is 4 to 6 lines above the static line
- The therapist begins turning the patient’s head horizontally at 2 Hz or 120 bpm on a metronome
- The therapist tells the patient which line to start reading with the same instructions - using colours next to the lines can help to tell the patient where to start
- The patient continues to read down the chart from left to right until she / he misses at least one optotype on a line
- At this point, testing is stopped
- The line above the one where the patient began missing optotypes while the head was moving is the dynamic visual acuity line
To score the test, count the difference between the static and dynamic visual acuity lines (where there were no optotypes missed in each of these lines). If there is a three or more line difference, then the DVA is considered abnormal. This reflects a functional measurement of the VOR.[1]
Head Shaking Test[edit | edit source]
The head shaking test is designed to increase any nystagmus caused by an asymmetry of the peripheral vestibular system. The response may be stronger in side lying but is generally performed in sitting.[15] It works better when Frenzel or Infrared camera goggles are used to eliminate visual fixation.[1]
The test is performed as follows:[1]
- The therapist should observe the client’s eyes for nystagmus as a baseline
- The patient’s head is then quickly oscillated horizontally 20 times
- This test will potentially increase the resting nystagmus observed - a positive test is when there are at least three beats of nystagmus
- This test will NOT be positive in patients with a BVL because there is no asymmetry between the two sides
- The head shaking test can be attempted without an infrared camera system as long as at least 80 percent of the patient’s visual field is devoid of visual cues or reference points
- To achieve this, have the patient in sit looking at a blank wall or similar visual scene
- Oscillate the patient’s head quickly 20 times back and forth (eyes closed)
- Have the patient open his / her eyes - the therapist observes from the side to see if any nystagmus is present
Pressure Testing[edit | edit source]
Nystagmus or drift of the eyes can be assessed by applying pressure to the tragus (i.e. the prominence on the inner side of the external ear).[1]
- Tullio’s phenomenon – noise provokes vertigo / nystagmus[17]
- Hennebert sign – pressure testing provokes vertigo / nystagmus[18]
- This test may be positive in conditions such as perilymphatic fistula,[19] hypermobile stapes, and Meniere’s disease or hydrops[1]
Motion Sensitivity Testing[edit | edit source]
The motion sensitivity test (MST) measures motion-provoked dizziness during 16 quick head or body position changes.[20]
Sensory Conflict[edit | edit source]
- Certain head and body movements send abnormal vestibular signals to the brain, which conflict with normal signals from the intact visual and somatosensory systems
- Sensory conflict is believed to produce the symptoms associated with motion-induced dizziness
- Provocative positions form the basis for treatment[1]
Motion sensitivity testing has been found to be a valid and reliable instrument for monitoring dizziness provoked by motion.[20] A score of 0-10 indicates mild symptoms; 11-30 indicates moderate symptoms and greater than 30 indicates severe symptoms.[1]
Balance and Gait Assessment[edit | edit source]
The central nervous system integrates sensory inputs from the visual, vestibular and somatosensory systems to achieve postural control. There are three postural control strategies:[1]
- Ankle strategy
- Hip strategy
- Stepping strategy
Static Balance Tests[edit | edit source]
The following tests can be used to assess static balance. It is important to note, however, that vestibular patients may have normal results in these tests.[1]
- Romberg test - the patient stands with his / her feet together and arms crossed. The patient is asked to maintain this position with eyes open and then eyes closed. It is usually stopped at around 30 seconds.[1]
- Sharpened Romberg - this test is similar to the Romberg, but this version is performed in tandem standing with eyes open and closed. [1]
- Single leg stance - eyes open and closed
- Modified clinical test of sensory interaction and balance (m-CTSIB):[21]
- The patient stands on foam with eyes open in order to alter somatosensory input
- The patient then stands on foam with his / her eyes closed - this alters the somatosensory and visual input, so that vestibular input is primarily utilised
Gait Assessment[edit | edit source]
The gait assessment involves the evaluation of dynamic postural control mechanisms in a variety of situations. The therapist should observe for the presence of gait deviations, including:[1]
- Veering to the right or left
- Widened base of support
- Decreased gait speed or arm swing
- Shortened step length
- Decreased ability to perform multiple tasks when walking
Basic Gait Assessment[edit | edit source]
Initial assessment:[1]
- Walk at normal speed
- Walk at an increased pace
- Walk while changing pace
- Walk with horizontal / vertical head turns
- Walk and turn rapidly
- Walk tandem forwards, backwards
- Watch for ‘en bloc’ or slow turns
Gait Deviation Assessment[edit | edit source]
- Take two pieces of tape 20 feet long (6m) and 1 foot wide
- The therapist instructs patients to walk between the pieces of tape - they should not allow their feet to touch the tape
- A score of ‘1’ is given each time one of a patient’s foot touches the tape
- This can be used as a home training exercise as well
- The width of the tape can be varied[1]
Singleton Test[edit | edit source]
Patients with UVL often have more difficulty turning quickly toward their affected side. The singleton test can be a useful test to localise the side involved. This test is performed as follows:[1]
- The patient is asked to walk normally and, on command, have them turn quickly 180 degrees, stop and place their feet together and then close their eyes
- Complete these steps on both the right and left sides
A patient may have increased postural instability when turning to the side with impaired vestibular function.[1]
Dynamic Gait Index[edit | edit source]
The dynamic gait index (DGI) can be used to quantify gait dysfunction in people with vestibular deficits.[22]
This measure includes eight dynamic gait tasks. It takes less than ten minutes to perform and uses minimal equipment (e.g. shoebox, two cones, stairs).[1]
- Patients are scored as having normal gait or a minimal, moderate or severe gait dysfunction
- Scores of 19 or less are predictive of falls in older community living adults[23]
Functional Gait Assessment[edit | edit source]
- The functional gait assessment (FGA) is adapted from the DGI:
- The FGA includes higher level gait tasks than the DGI which is beneficial as the DGI has been found to have a ceiling effect for individuals with vestibular dysfunction[25]
- Like the DGI, it utilises a 20 feet (6 m) runway, 1 foot wide
- It includes ten test conditions or tasks with a maximum score of 30, which indicates normal performance[1][25]
Summary[edit | edit source]
- There are a number of objective tests that should be included in the objective assessment of the vestibular patient
- From this assessment, you will be able to determine the optimal treatment approach
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 1.20 1.21 1.22 1.23 1.24 1.25 1.26 1.27 1.28 1.29 1.30 1.31 1.32 1.33 1.34 1.35 1.36 1.37 1.38 1.39 Tonks B. Vestibular Assessment Course. Plus , 2021.
- ↑ Serra A, Leigh RJ. Diagnostic value of nystagmus: spontaneous and induced ocular oscillations. J Neurol Neurosurg Psychiatry. 2002;73(6):615-8.
- ↑ Purves D, Augustine GJ, Fitzpatrick D, et al., editors. Neuroscience. 2nd edition. Sunderland (MA): Sinauer Associates; 2001. Types of Eye Movements and Their Functions. Available from: https://www.ncbi.nlm.nih.gov/books/NBK10991/
- ↑ Physical Therapy Nation. VOR Cancellation Test. Available from: https://www.youtube.com/watch?v=ExOs7HSHv-c [last accessed 5/7/2021]
- ↑ Tjell C, Rosenhall U. Smooth pursuit neck torsion test: a specific test for cervical dizziness. Am J Otol. 1998;19(1):76-81.
- ↑ Daly L, Giffard P, Thomas L, Treleaven J. Validity of clinical measures of smooth pursuit eye movement control in patients with idiopathic neck pain. Musculoskelet Sci Pract. 2018;33:18-23.
- ↑ Majcen Rosker Z, Vodicar M, Kristjansson E. Inter-visit reliability of smooth pursuit neck torsion test in patients with chronic neck pain and healthy individuals. Diagnostics (Basel). 2021;11(5):752.
- ↑ The Physio Channel. Smooth Pursuit Neck Torsion Test. Available from: https://www.youtube.com/watch?v=YwQvcgY0A_k [last accessed 5/7/2021]
- ↑ Termsarasab P, Thammongkolchai T, Rucker JC, Frucht SJ. The diagnostic value of saccades in movement disorder patients: a practical guide and review. J Clin Mov Disord. 2015;2:14.
- ↑ Patel SS, Jankovic J, Hood AJ, Jeter CB, Sereno AB. Reflexive and volitional saccades: biomarkers of Huntington disease severity and progression. J Neurol Sci. 2012;313(1-2):35-41.
- ↑ McDowell JE, Dyckman KA, Austin BP, Clementz BA. Neurophysiology and neuroanatomy of reflexive and volitional saccades: evidence from studies of humans. Brain Cogn. 2008;68(3):255-70.
- ↑ 12.0 12.1 Schubert MC, Tusa RJ, Grine LE, Herdman SJ. Optimizing the sensitivity of the head thrust test for identifying vestibular hypofunction. Phys Ther. 2004;84(2):151-8.
- ↑ Physical Therapy Nation. Head Thrust Test. Available from: https://www.youtube.com/watch?v=KYI7eHhwhwk [last accessed 5/7/2021]
- ↑ Physical Therapy Nation. Dynamic Visual Acuity Test. Available from: https://www.youtube.com/watch?v=AfghWx3IInE [last accessed 5/7/2021]
- ↑ Cohen HS. A review on screening tests for vestibular disorders. Journal of Neurophysiology. 2019 Jul 1;122(1):81-92.
- ↑ Vestibular Today. Head Shake Test (Vestibular Examination). Available from: https://www.youtube.com/watch?v=glSJGnTMeHE [last accessed 5/7/2021]
- ↑ Lehmkuhl B, Andaloro C. Tullio Phenomenon. [Updated 2020 Dec 11]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK513229 /
- ↑ Castellucci A, Botti C, Bettini M, Fernandez IJ, Malara P, Martellucci S et al. Case report: could Hennebert's Sign be evoked despite global vestibular impairment on video head impulse test? Considerations upon pathomechanisms underlying pressure-induced nystagmus due to labyrinthine fistula. Front Neurol. 2021;12:634782.
- ↑ Casale M, Errante Y, Sabatino L, Incammisa A, Salvinelli F, Quattrocchi CC. Perilimphatic fistula test: a video clip demonstration. Eur Rev Med Pharmacol Sci. 2014;18(23):3549-50.
- ↑ 20.0 20.1 Akin FW, Davenport MJ. Validity and reliability of the Motion Sensitivity Test. J Rehabil Res Dev. 2003;40(5):415-21.
- ↑ Antoniadou E, Kalivioti X, Stolakis K, Koloniari A, Megas P, Tyllianakis M et al. Reliability and validity of the mCTSIB dynamic platform test to assess balance in a population of older women living in the community. J Musculoskelet Neuronal Interact. 2020;20(2):185-93.
- ↑ Dye DC, Eakman AM, Bolton KM. Assessing the validity of the dynamic gait index in a balance disorders clinic: an application of Rasch analysis. Phys Ther. 2013;93(6):809-18.
- ↑ Wrisley DM, Kumar NA. Functional gait assessment: concurrent, discriminative, and predictive validity in community-dwelling older adults. Phys Ther. 2010;90(5):761-73.
- ↑ BoysTownHospital. Vestibular Tests - DGI Tests. Available from: https://www.youtube.com/watch?v=ZtoPoTlENlo [last accessed 5/7/2021]
- ↑ 25.0 25.1 Wrisley DM, Marchetti GF, Kuharsky DK, Whitney SL. Reliability, internal consistency, and validity of data obtained with the functional gait assessment. Phys Ther. 2004;84(10):906-18.
- ↑ Mission Gait. Functional Gait Assessment - Setup and Instruction. Available from: https://www.youtube.com/watch?v=kqQ_nigCJkQ [last accessed 5/7/2021]